‘The goal of recovery is not to become normal. The goal is to embrace the human vocation of becoming more deeply, more fully human’ (Reference DeeganDeegan, 1996).
To ask if someone will recover is the most obvious and basic question when confronted with any severe health problem, and helping people recover is the most fundamental goal for any service or practitioner. However, it has long been assumed that people with severe mental illness do not recover, leading to low expectations which have been seen to erode hope and collude with chronicity (Reference Harrison and MasonHarrison & Mason, 1993). Advances in psychiatric practice usually involve an improvement of existing treatments or new methods of service delivery. Occasionally a new way of thinking about mental health problems arises, a new clinical philosophy, which enables old problems to be thought about in new ways – the rediscovery of ‘recovery’ is just that.
When the Department of Health reissued a summary of the National Health Service (NHS) Plan and the National Service Framework for Adult Mental Health as The Journey to Recovery (Department of Health, 2001b ), it cleverly coupled the full weight of the modernisation agenda and strategic review with the liveliest and most optimistic philosophy emerging from the user movement. Increasingly, talk of ‘recovery’ can be found in the pages of a wide range of professional journals, the lay press and even MENSA Magazine. This interest has arisen largely from service-user and non-statutory groups, supported by the National Institute for Mental Health in England (NIMHE), which has established a Fellowship for Recovery and a Positive Practice Award (for details search http://www.nimhe.org.uk). As psychiatrists continue to debate their roles and responsibilities, they need to understand that service users are also moving to redefine these roles and are developing a model in which people can recover without the help of doctors, and sometimes even despite them. Superficially, this may look like the latest reincarnation of anti-psychiatry, but is actually the opposite: a potentially unifying and collaborative goal – recovery.
Milestones on the road to recovery
Claims that the present recovery movement constitutes a new paradigm (Reference Allott, Loganathan, Fulford, Lurie, McCubbin and DallaireAllott et al, 2003) are probably exaggerated, as it perhaps represents a rediscovery of practices initiated more than 200 years ago. For it was a critical appraisal of psychiatric practice that inspired the Tukes at York to establish a clinical philosophy and therapeutic practice based on kindness, compassion, respect and hope of recovery (Reference TukeTuke, 1813). It is noteworthy that visitors to the College pass a plaque of William Tuke as they enter the lobby.
Reference AnthonyAnthony (1993) has described how interest in ‘recovery’ evolved from both the physical disability movement and deinstitutionalisation within psychiatry, to emerge as a guiding vision for mental health services in the USA during the 1990s. Major reviews were prepared as background when the US surgeon general set recovery at the centre of mental health policy (Reference Ralph, Lambert and KidderRalph et al, 2002); and since 1998 (Reference O'HaganO'Hagan, 2001) New Zealand mental health services have been based on a recovery-centred ‘Blueprint’, which has led them to become a wellspring of ideas and guidance on recovery-based practice. The UK developments in recovery have been traced to anti-discriminatory and disability legislation, the growth of consumerism (Reference Allott, Loganathan, Fulford, Lurie, McCubbin and DallaireAllott et al, 2003) and broad initiatives in support of the Department of Health's Expert Patients Programme (Department of Health, 2001a ).
In the UK, as in the USA, mental health professionals have contributed to the moving and instructive personal accounts of the experience of recovery from severe mental illness (e.g. Reference NorthNorth, 1988; Reference JamisonJamison, 1995; Reference FisherFisher, 2001; Reference May, McGorry and GleesonMay, 2004), and there is a process at work analogous to ‘coming out’ in combating stigma. When the current President of the Royal College of Psychiatrists Mike Shooter sought election with the usual brief curriculum vitae detailing his qualifications for the job, unusually this included his personal experience of depression. In conferring upon him this highest office, the Members and Fellows of the College appear to have placed a very different value on this disclosure from that of the past, acknowledging the value of personal experience alongside professional skills and training (Reference CraneCrane, 2003). Increasing convergence between a user-led perspective and NHS policy is also reflected in the clinical guidelines for schizophrenia recently published by the National Institute for Clinical Excellence (NICE; 2002), which contain striking parallels with what US service users have identified as the most important recovery-oriented practices (Ohio Department of Mental Health, 2003) (Box 1).
Box 1 Comparison of the highest-ranking recovery-oriented practices from the Ohio outcomes initiative and the National Institute for Clinical Excellence's clinical guidelines for schizophrenia
| Ohio | Encourage my independent thinking |
| NICE | Discuss preferences, record advance directives (p. 39) |
| Ohio | Treat me in a way that helps my recovery process |
| NICE | Offer help in an atmosphere of hope and optimism (1.1.1) |
| Ohio | Treat me as an equal in planning my services |
| NICE | Foster a collaborative working relationship (1.1.5) |
| Ohio | Give me the freedom to make my own mistakes |
| NICE | Service-user preferences are central (1.4.5) |
| Ohio | Treat me like they believe I can shape my own future |
| NICE | Patients have the right to be fully informed and share in decision-making (p. 50) |
| Ohio | Listen to me and believe what I say |
| NICE | Encourage patients to write their own account of their illness in their notes (1.3.3); record your treatment preferences (p. 39) |
| Ohio | Look at and recognise my abilities |
| NICE | Include assessment of occupational status and potential (1.4.6) |
| Ohio | Work with me to find the resources or services I need |
| NICE | Comprehensive care coordination (p. 46) |
| Ohio | Be available to talk to me when I need to talk to someone |
| NICE | Professionals who work with you should be engaging and kind, in constructive partnership (p. 38) |
| Ohio | Teach me about the medications I am taking |
| NICE | Give patients clear and intelligible information, full discussion, choice (1.4.5) |
What is meant by ‘recovery’?
Definition and redefinition
The term ‘recovery’ appears to have a simple and self-evident meaning, but within the recovery literature it has been variously used to mean an approach, a model, a philosophy, a paradigm, a movement, a vision and, sceptically, a myth (Reference WhitwellWhitwell, 1999). Two main perspectives have generated very different kinds of data. The first focuses on the familiar dimensions of clinical and social recovery, measured objectively through outcome studies and expressed as approximations to cure. The second focuses on the personal and existential dimensions of recovery, taking the form of subjective and self-evaluated accounts of how an individual has learned to accommodate to an illness. These accounts have become the founding stories of the recovery movement (e.g. Reference ChamberlinChamberlin, 1978; Reference LovejoyLovejoy, 1984; Reference DeeganDeegan, 1988, Reference Deegan1996; Reference LeeteLeete, 1989; Reference UnzickerUnzicker, 1989; Reference ClayClay, 1994; Reference ColemanColeman, 1999; Reference RidgewayRidgeway, 2000), and anthologies of these personal stories have been used by governments and professions as a means of combating stigma and reasserting a focus on personal perspectives (Reference LeibrichLeibrich, 1999; Reference Lapsley, Waimarie and BlackLapsley et al, 2002; Reference Ramsay, Page and GoodmanRamsay et al, 2002). For example, Daniel Fisher, as a psychiatrist and co-director of the National Empowerment Centre in the USA, illustrates the power of the personal account through his challenge in the Washington Post, which begins:
‘I have recovered from schizophrenia. If that statement surprises you – if you think schizophrenia is a lifelong brain disease that cannot be escaped – you have been misled by a cultural misapprehension that needlessly imprisons millions under the label of mental illnesses’ (Reference FisherFisher, 2001).
The practitioner of evidence-based medicine will also be aware of the dangers of adopting a general theory and expectation based on a single case history.
Reference AnthonyAnthony (1993) is credited with the most widely accepted contemporary definition of recovery. He argues that the person with a mental illness can recover even when the illness is not cured, and that the process of recovery can proceed in the presence of continuing symptoms and disabilities. From this viewpoint ‘wellness’ and ‘illness’ may be considered as independent variables. Thus, recovery involves:
‘a deeply personal, unique process of changing one's attitudes, values, feelings, goals, skills and roles. It is a way of living a satisfying, hopeful, and contributing life even with limitations caused by the illness. Recovery involves the development of new meaning and purpose in one's life as one grows beyond the catastrophic effects of mental illness’.
Recovery and cure: the significance of long-term outcome studies
Many authors cite Harding et al's pioneering long-term studies in support of a more optimistic attitude and higher expectations for recovery; in these studies half to two-thirds of patients with severe mental illness, including ‘some very chronic cases’, significantly improved or recovered (Reference Harding, Brooks and AsolagaHarding et al, 1987). The criteria for recovery are impressive: no current medication, working, relating well to family and friends, integrated into community, and behaving in such a way that no one could detect that the individual had ever been hospitalised for any kind of psychiatric problem. However, the applicability of these findings to other clinical settings has been challenged on the grounds of selection bias and the unusual comprehensiveness of the patients’ treatment. An inherent difficulty in interpreting long-term outcome studies is that the ‘outcomes’ can say as much about the sampling of patients admitted to these studies as about the illnesses studied (Reference Harrison and MasonHarrison & Mason, 1993). Reference WarnerWarner's (1994) review of 85 studies over the past 100 years led him to observe that ‘few topics in psychiatry have been researched as frequently, and over as long a period of time, as has recovery from schizophrenia,’ but despite this volume of work, ‘a clear picture of long-term outcome has not emerged’. He attributes this to the limited validity of schizophrenia as a diagnostic entity.
The International Study of Schizophrenia (Reference Harrison, Hopper and CraigHarrison et al, 2001), which is probably the most substantial long-term follow-up study to date, included 1633 participants from 14 culturally diverse areas, studied at 15 years and 25 years after diagnosis. The results were in line with previous studies. Global outcomes at 15 years and 25 years were favourable for over half of all people followed up. There was evidence of a ‘late recovery’ effect, which supported the case for therapeutic optimism and suggested that these findings should ‘join others in relieving patients, carers and clinicians of the chronicity paradigm which dominated thinking throughout much of the 20th century’.
While underlining the need to carefully operationalise the concept of recovery, Harrison et al also comment that studies such as their own, which rely heavily on the absence of symptoms, social disabilities and resource utilisation as outcome indicators, ‘should not be equated with recovery of the level of functioning achieved before onset of illness, and even less with the recovery of lost potential’, and furthermore that ‘recovering a meaningful and fulfilling life within the limitations of the disorder’ is an important judgement that their data do not allow them to make.
It would appear that until these parameters are more adequately accounted for and the core concepts carefully operationalised, estimation of recovery will not be greatly helped by outcome research.
Recovery and the medical model
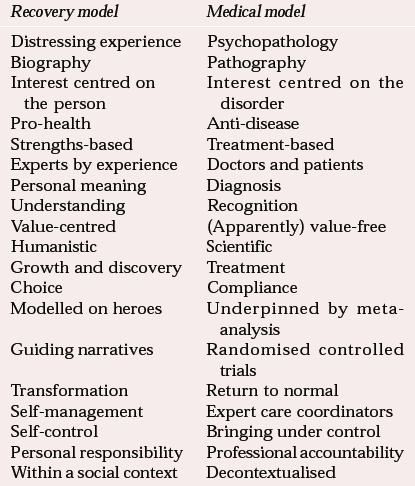
It is a largely non-medical assertion that medical practice is governed by something called ‘the medical model’, and the largely non-medical recovery literature yields a strong and clear view that psychiatric thought and practice are almost entirely hostage to it. It is often depicted as narrowly focused on disease, treatment and biological reductionism, underwritten by evidence-based medicine, and this is contrasted with the broader, person-centred focus of recovery models (Reference Ralph, Lambert and KidderRalph et al, 2002), which assert the validity of an evidence base largely composed of personal narrative, and the views of ‘experts by experience’. At present, these two perspectives, their values and language, stand in significant tension with one another (Table 1).
Table 1 Differences in concepts, language and values between the recovery and the medical models
| Recovery model | Medical model |
|---|---|
| Distressing experience | Psychopathology |
| Biography | Pathography |
| Interest centred on the person | Interest centred on the disorder |
| Pro-health | Anti-disease |
| Strengths-based | Treatment-based |
| Experts by experience | Doctors and patients |
| Personal meaning | Diagnosis |
| Understanding | Recognition |
| Value-centred | (Apparently) value-free |
| Humanistic | Scientific |
| Growth and discovery | Treatment |
| Choice | Compliance |
| Modelled on heroes | Underpinned by meta-analysis |
| Guiding narratives | Randomised controlled trials |
| Transformation | Return to normal |
| Self-management | Expert care coordinators |
| Self-control | Bringing under control |
| Personal responsibility | Professional accountability |
| Within a social context | Decontextualised |
Thus, the recovery literature often characterises psychiatrists as risk averse and wedded to a prescribing, relapse-prevention and maintenance model of care (‘warehousing’), which fosters dependence. Critics further emphasise that time, much time, can pass without benefit. Reference DeeganDeegan (1988) has poignantly recollected that she stood,
‘drugged and stiff in the hallways of a mental hospital while my classmates went off to college. We experienced time as a betrayer. Time did not heal us’.
The process of recovery
In contrast with emphasising the struggle for cure, Reference DeeganDeegan (1988) defines recovery as ‘a process, a way of life, an attitude, and a way of approaching the day's challenges’. The recovery literature (Reference Ralph, Lambert and KidderRalph et al, 2002; Reference Allott, Loganathan, Fulford, Lurie, McCubbin and DallaireAllot et al, 2003) similarly describes being ‘in recovery’ as a process that involves gaining or regaining many aspects of life that are usually taken for granted and may have been lost or severely compromised by mental illness. Most authors consider that the pivot of recovery is the individual's active and responsible engagement with his or her distress and difficulties. This may involve many steps and stages, and inevitable uncertainty, so that recovery becomes ‘an uncharted, unpredictable, and personal journey’ (Reference SheehanSheehan, 2002).
Recovery is often described as having a defining moment or turning-point (Reference Allott, Loganathan, Fulford, Lurie, McCubbin and DallaireAllott et al, 2003), sometimes a low turning-point (Reference Rakfeldt and StraussRakfeldt & Strauss, 1989), before which the individual felt stuck, perhaps denying the illness because of anxiety or unresolved grief for loss of health and future. It is sometimes claimed that recovery is often further delayed by a state of learned helplessness encouraged by the low expectations of mental health professionals, especially when they remove the individual's responsibility. However, even in circumstances that begin with compulsory admission, there is the possibility of progressive handing back of power and control to the patient, so that choice and self-direction are supported at the earliest opportunity.
The experience of turning towards recovery may come out of the blue, but is more often described as arising from talking to others, particularly to other service users rather than professionals. It is experienced as regaining a sense of self, of taking control and responsibility, often combining optimism for the future with acceptance of the past. Service users describe a wide range of transitions at work in the recovery process. Finding meaning in and for psychotic experiences can be empowering, as can the emphasis on spirituality that is common in patients’ accounts (Reference Faulkner and LayzellFaulkner & Layzell, 2000; Reference LeibrichLeibrich, 2001).
From within the user movement, Reference ColemanColeman (1999) has emphasised that recovery depends far more on self-help and collaboration than on being treated:
‘Recovery is not a gift from doctors but the responsibility of us all … We must become confident in our own abilities to change our lives; we must give up being reliant on others doing everything for us. We need to start doing these things for ourselves. We must have the confidence to give up being ill so that we can start becoming recovered.’
And although this risks formulating recovery as ‘simply’ an act of faith, it is apparent that it will be difficult to realise recovery without faith and hope in the possibility.
Measurement of recovery
Reference Liberman and KopelowiczLiberman & Kopelowicz (2002), after a decade of witnessing the promotion of recovery in the USA, insist on the need to
‘go beyond the hype, vague “vision” and glittering generalities … and move into the realm of empirically supported validation of an operationally defined concept of recovery.’
They suggest dimensions that could be used to derive such an operational definition (Box 2).
Box 2 Dimensions for operationalising recovery from schizophrenia (Reference Liberman and KopelowiczLiberman & Kopelowicz, 2002. Reproduced with permission from Taylor & Francis Ltd)
-
1 Remission of both positive and negative psychotic symptoms and signs
-
2 Working or studying in normative employment or educational settings
-
3 Independent living without supervision of money, self-care and medication
-
4 Social activities with peers
-
5 Cordial family relations and contacts
-
6 Recreational activity in normative settings (i.e. not in psychosocial clubhouses or day treatment programmes)
-
7 Resilience and capacity for problem-solving when faced with stressors or challenges in everyday life
-
8 Subjective satisfaction with life
-
9 Self-esteem and stable self-identity
-
10 Participation as a citizen in voting, self-advocacy, neighbourliness and other civic arenas
It appears that, despite a century or more of measuring the results of interventions, the measurement of recovery is at an early stage. The need to gather and strengthen the evidence base for recovery suggests a major area for collaboration between service users and providers. For service users, narratives of recovery, whether written or spoken, offer relief from alienation, validation of unusual experience and, when experiences are told in groups, a social context in which coping strategies can be exchanged. For psychiatrists, meta-analyses of randomised controlled trials, although important, provide little guidance on what might make a difference to an individual patient entering the service. There remains a need to develop research methods that integrate the relevance of subjective accounts with the rigour of reproducible objective measures: ‘the challenge is to make the important measurable, not the measurable important’ (attributed to former US Secretary of State Robert McNamara). Reference Ralph, Kidder and PhillipsRalph et al(2000) have produced a compendium of recovery and recovery-related instruments, all of which remain in development. In the current UK national trial of outcomes measures, the NIMHE (Users and Carers) Experts by Experience Group is recommending that the Ohio Department of Mental Health's (2003) Mental Health Recovery and Consumer Outcomes Initiative be selected as a recovery outcomes tool (Reference Allott, Loganathan, Fulford, Lurie, McCubbin and DallaireP. Allott, personal communication, 2003).
Steps towards recovery-oriented psychiatric practice
A shift of professional role from authority to coach
Recovery might not be in the gift of doctors, but the skills, knowledge, authority and commitment of psychiatrists can have a significant influence on the promotion and implementation of recovery-based approaches. A change in the role of the psychiatrist is required, from someone who is perceived as a remote expert or authority to someone who behaves more like a coach or personal trainer, offering professional skills and knowledge, while learning from and valuing the patient, who is an ‘expert by experience’. There are striking stories of how effective this can be when ‘seeing a psychiatrist’ is experienced by patients as having alongside an trained and committed person, who believes in them and their future (Reference Ramsay, Page and GoodmanRamsay et al, 2002).
Focusing on the core significance of hope and optimism
Being met with hope and optimism, especially at the initial contact, is of central significance in many people's accounts of recovery, and ‘offering help, treatment and care in an atmosphere of hope and optimism’ is the first and overarching principle in the NICE clinical guidelines (National Institute for Clinical Excellence, 2002: 1.1.1.1). This has implications for staff selection and training to enable them to foster hope-inspiring relationships (Box 3) and exhibit recovery competencies (see Box 5).
Box 3 Dimensions of hope-inspiring relationships (from Reference Repper and PerkinsRepper & Perkins, 2003)
-
1 Valuing people as human beings
-
2 Acceptance and understanding
-
3 Believing in the person's abilities and potential
-
4 Attending to people's priorities and interests
-
5 Accepting failures and setbacks as part of the recovery process
-
6 Accepting that the future is uncertain
-
7 Finding ways of sustaining our own hope and guarding against despair
-
8 Accepting that we must learn and benefit from experience
Box 5 New Zealand guidelines on recovery competencies for mental health workers (adapted from Reference O'HaganO'Hagan, 2001, with permission)
A competent mental health worker:
-
1 understands recovery principles and experiences in the national and international contexts
-
2 recognises and supports the personal resourcefulness of people with mental illness
-
3 understands and accommodates the diverse views on mental illness, treatments, services and recovery
-
4 has the self-awareness and skills to communicate respectfully and develop good relationships with service users
-
5 understands and actively protects service users’ rights
-
6 understands discrimination and social exclusion, its impact on service users and how to reduce it
-
7 acknowledges different cultures and knows how to provide a service in partnership with them
-
8 has comprehensive knowledge of community services and resources and actively supports service users in accessing them
-
9 has knowledge of the service-user movement and is able to support its participation in services
-
10 has knowledge of family perspectives and is able to support the family's participation in services.
Timing responses: what helps when?
Reference McGorryMcGorry (1992) describes the need to carefully match explanations of illness to the patient's readiness to accept them. He advises us ‘to avoid adding insight to injury’, for denial of illness, especially early on, may have a self-protective function (Reference DeeganDeegan, 1988). Furthermore, although a ‘sealing-over’ recovery style predicts poor engagement, the common shift from ‘integration’ to ‘sealing over’ in the first 6 months is associated with symptomatic improvement (Reference Tait, Birchwood and TrowerTait et al, 2003). If symptoms carry significant meanings for individuals, then their presence and absence are both significant, and the process of recovery may be accompanied by complex losses and powerful realisations (Reference RobertsRoberts, 2000; Box 4). Insufficient attention has been given to the dynamics of resistance in considering recovery, but all of this contributes to a growing view that working with psychotic symptoms may be more helpful than attempting to demonstrate their falseness.
Box 4 ‘The end of empire’
And so I walked, beside the canal, plans and policies talked out so far only silence remained, enemies everywhere, none greater than those closest, news from the frontier forgotten as soon as it is told, spies lost in their own ciphers. In this way an empire crumbles, aimlessly, along the canal, a walk, the swans that can at least fly this place, a chill wind blowing from the Alps. Soon, all this will be desolation, The banks broken, the ducks caught for starving troops. Alone, I walked, aimless, with the strange lethargy of total defeat, and memories of other days stirring the silence with fanfares.
Graeme Hobbs (undated), ‘written after 3 years of schizophrenia and a few days before I recovered my sanity’ (reproduced with permission from Reference HobbsHobbs, 1998; emphasis added)
Medication and medicating: more than compliance
Many service users have considerable problems with the need to take medication. It is often not just the drugs themselves, and their unwanted effects, but the whole implication of taking something for a ‘broken brain’, and the atmosphere of persuasion or compulsion that often surrounds them. Many patients associate being well with giving up medication, even when there are adverse, and sometimes repetitive, consequences.
There is therefore much to be gained in working for a negotiating stance, in which risks can be taken within safe parameters and lessons learned from experience. Individuals then have an opportunity to value the use of their (own) medication as a tool in pursuit of their recovery. As described in the NICE guidelines (National Institute for Clincial Excellence, 2002: 1.4.5 & p. 48), such negotiation and choice should be based on a well-informed and thoughtful search for the most effective medication in the lowest dose and include recognition that, for some, the experience of taking medication can be worse than the disorder. It also needs to be acknowledged that it is possible for some to recover and stay well without medication, but there is no reliable way of knowing who will remain well, and stopping medication is probably the most common cause of relapse.
Working with risk: a shift from risk avoidance to risk-sharing
Deegan's rallying call that ‘professionals must embrace the concept of the dignity of risk, and the right to failure if they are to be supportive of us’ (Reference DeeganDeegan, 1996) seems completely at odds with the risk-averse climate in which we live and work, where, for instance, patients often have to be medically ‘vetted’ before an occupational therapist can take them for a cycle ride. And yet risk is inevitable, and healthy. We begin to take risks with our first few steps in life, and without risk there is no progress or development.
For psychiatrists, stopping a patient's medication can represent the risks that epitomise the tensions involved in implementing a recovery model. Failing to distinguishing between a temporary exacerbation of symptoms due to medication reduction and a genuine relapse carries the possibility of reinforcing the belief that medication needs to be lifelong. Reference May, McGorry and GleesonMay (2004) describes his experience of medication as intolerable, especially as, for him, the ‘psychic indifference’ towards psychotic symptoms carried over into every aspect of life. He went into hiding from family and services for weeks and experienced what he describes as a withdrawal syndrome that was quite different in quality from previous episodes of psychosis and that resolved spontaneously. He subsequently took a psychology degree and trained as a clinical psychologist. He has remained medication-free ever since and has become a highly respected witness and advocate for recovery. A single story cannot support ‘non-compliance’ as a route to recovery, but if an individual is determined to stop medication, a recovery-oriented approach should aim to negotiate a phased reduction, during which contact and relationship is maintained, reducing the risk of relapse through awareness of early signs and enabling both patient and prescriber to learn from the experience.
What would a recovery-based service look like?
Reference AnthonyAnthony (1993, Reference Anthony2000) has emphasised that effective service development must be based on what people in recovery have found to be helpful or valuable. It has been repeatedly observed that this is significantly different from what is currently found in standard psychiatric textbooks (Reference Faulkner and LayzellFaulkner & Layzell, 2000; Reference Baker and StrongBaker & Strong, 2001; Mental Health Foundation, 2002), although some services are beginning to train staff in ‘recovery competencies’ (Box 5).
Promoting self-management
Empowerment is seen as a core dynamic in promoting recovery (Reference Repper and PerkinsRepper & Perkins, 2003). There is increasing awareness of the value of detailed self-management strategies that help individuals to take control of their experience and their lives. The Wellness Recovery Action Plan (WRAP; Reference CopelandCopeland, 2002) is one of the most popular and well-established recovery tools. It begins by helping individuals to equip themselves with ‘personal wellness tools’. This involves identifying actions, thoughts and behaviours that, from personal experience, are associated with staying well and reducing symptoms. These tools are then incorporated into a written plan, which includes daily maintenance, triggers and how to avoid them, warning signs and how to respond to them, and a crisis plan.
Hospital should be a ‘springy safety net’
Although Reference May, McGorry and GleesonMay (2004) acknowledges that hospital was a useful safety net for him and his family, he speaks for many when he writes ‘my main complaint was the lack of springiness in the net to allow me to get back on the tightrope’. Service users want rapid access to help in a crisis, but once the crisis has resolved they do not necessarily want to be caught up in long-term involvement and monitoring, however much health care professionals may regard that as prudent. They would also like to be able to renew contact with their service as soon as problems arise, without having to wait for complex referral processes to be instigated. This points towards redesigning some aspects of the care programme approach to include a more user-oriented recovery plan.
The expert patient
There is a progressive move throughout the NHS to value patients as ‘experts in their own experience’ (Department of Health, 2001a ). There is a complex need to reconcile the emergent role of ‘expert by experience’ with the role of health care professional, to balance the preservation of patient autonomy with the professional's duty of care for some of the most vulnerable people in society. There is inevitable difficulty in this, but also considerable opportunity in finding safe and respectful ways of opening this dialogue. A recovery-based service centres staff training on the lived experience of service users. Such training sessions typically cover the history of recovery and its social context, the language used by clinicians, the importance of complementary therapies and the use of the WRAP. During training sessions, mental health workers often reveal their own experience of mental illness (C. Willey, Clinical Nurse Manager, Black Country NHS Trust, personal communication, 2003). Learning benefits include focusing on life rather than illness, changes in the use of language and greater emphasis on what patients value most: safe and satisfactory accommodation, sufficient money, supportive relationships, work and meaningful activity.
Valuing ethnicity and diversity
The North American recovery literature has been criticised for an excessively individualistic approach which sidelines ethnicity and its social consequences for users, ‘projects traditional American values onto disabled people, such as rugged individualism, competition, personal achievement and self-sufficiency’ and fails to appreciate that, for some service users, independent living can be a lonely experience in a single room in a rooming house (Reference DeeganDeegan, 1988). This contrasts with the New Zealand perspective, particularly in the context of Maori people (Reference Fenton and Te KoutuaFenton & Te Koutua, 2000; Reference O'HaganO'Hagan, 2001; Reference Lapsley, Waimarie and BlackLapsley et al, 2002), which has illustrated the importance of valuing a person's cultural origins and personal meanings as reference points around which to support their citizenship and combat stigma. Recovery is then based on ‘knowing who you are, and where you come from, and re-integrating yourself with your own people in your own way’ (Reference Lapsley, Waimarie and BlackLapsley et al, 2002), a sentiment that carries universal relevance and appeal. There is also a great need to recognise the significance of celebrating the small achievements of ordinary living (Reference LeibrichLeibrich, 1999), rather than risk being eclipsed by culture-bound heroic ideals.
Making recovery worth it: what is there to recover for?
Traditional medical approaches attempt to relieve adverse experiences with little consideration given to what happens next. Reference Butterworth and DeanButterworth & Dean (2000) describe how a survey of mental health service users in the Bristol area found that less than half of the participants were engaged in any form of occupational activity. This led to the creation, in 1997, of a Work Development Team, which has since become a ‘Beacon site’. The team has helped over 200 people in returning to full-time employment, and it included a job retention service which has helped over 50 people to remain in their jobs and 19 to explore other career paths before successfully returning to the labour market (R. Butterworth, personal communication, 2003). Work and employment have such a major role in recovery, bringing financial, social, existential and spiritual benefits, that there is a clear case for drawing occupational therapists back from generic roles in community teams. Mental health services could also put their own house in order by developing supported employment schemes within trusts (Reference Repper and PerkinsRepper & Perkins, 2003).
Difficulties over diagnosis and steps towards a common language
The development of a professional language and identity can be seen as part of a ‘tribal’ induction that sets us apart, and membership of the group follows a formal exhibition of proficiency to its elders. However, mental health workers have recently been advised to develop their specialist knowledge and language in such a way that it can easily be shared with the service users to whom it refers (National Institute for Clinical Excellence, 2002: 1.1.7). The Department of Health's (2003) guidance on copying letters to patients will oblige psychiatrists, in common with all doctors, to write in a way that patients can readily and usefully understand.
Diagnoses are a recurrent concern. They are perceived by some as ‘life sentences’, inducting a person into expectations of life saturated with problems, with all the associated pessimism and stigma. Diagnoses can be experienced as overwhelming, eclipsing personal identity, so that, for example, people with mental illnesses become ‘schizophrenics’. Reference Davidson and StraussDavidson & Strauss (1992) found that a key correlate of favourable long-term outcome in schizophrenia was that individuals were able to differentiate themselves from their diagnosis and that they had a sense of an intact, healthy self, separate from their illness experience: a ‘me’ separate from an ‘it’. It is noteworthy that Leibrich's anthology of personal recovery stories, in which people write about their unique lives and personal illness experiences (Reference LeibrichLeibrich, 1999), was commissioned by the New Zealand Government as part of its national anti-stigma campaign. The exchange of meanings and stories by people with severe illness can itself significantly influence their experience, and it is central to the message of the recovery literature that redefining oneself as being ‘in recovery’ has consequences very different from those of being defined by others as ‘chronically ill’ (see also Reference KleinmanKleinman, 1988).
Diagnostic caution is commendable when considering severe mental illnesses, but it carries the risk of diagnostic dithering or avoidance, which may risk an unhealthy collusion with a patient or relatives, provoking divisions within a family and becoming a barrier to desperately needed treatment and support. Practitioners need a sophisticated understanding of what diagnosis is, and is not, and should make sure that they are at least as aware as their patients of the continuing debate over the diagnosis of schizophrenia (Reference van Os and McKennavan Os & McKenna, 2003).
Medical notes are often taken, for example by the courts, as an objective and accurate record of what has happened and why, although they are clearly a medical interpretation of events. In an interesting and provocative development, we are now required to support individuals in writing their own account of their illness in their notes (National Institute for Clinical Excellence, 2002: 1.3.3). There is the explicit aim of helping patients to understand what has happened to them and to give an account of it in their own words. There should no longer be a single account of the illness experience, refracted through a medical perspective. Current guidance promotes the preservation of a diversity of viewpoints within the official record.
Looking ahead
As a professional group, our journey into recovery is unlikely to be smooth or easy. As in many movements for change, some proponents readily take up an antagonistic or even hostile position. Some have likened collaboration between service users and NHS planners to ‘supping with the devil’ (Reference JacksonJackson, 2003); others have likened professional involvement in recovery to colonisation or worry about a professional take-over. There are also those who have little hesitation in using ‘straw man’ arguments to support their views. They set up a caricature of a psychiatrist, apparently inspired by the medical model in his inept and abusive practices, and then knock this down to demonstrate the superiority of their own views and values. In some ways this works well as a rhetorical device, providing demarcation and a banner beneath which enthusiasts and radicals can gather. But it does not serve the cause of promoting recovery, for reality is more complex, and few practitioners will identify with these distorted images or feel the need to repent in a manner that these dramas invite. There is more likelihood of perpetuating splits, rather than gathering support for change. It is also simply unnecessary, since the recovery movement, unlike some other user movements, is not fundamentally based on opposition or grievance and is not anti-psychiatry. It centres on an outward, pro-recovery approach, offering a broad, inclusive, humanistic philosophy that could unite professionals, service users and others in the collaborative project of working for better lives for those who experience severe mental health problems (Box 6 lists some relevant organisations).
Box 6 Contacts and resources for the recovery movement

| Department of Health's Expert Patient Programme | http://www.ohn.gov.uk/ohn/people/expert.htm |
| http://www.lmca.org.uk/docs/expert.htm | |
| Long-term Medical Conditions Alliance (LMCA) | http://www.lmca.org.uk |
| Manic Depression Fellowship's self-help resources | http://www.mdf.org.uk |
| Mary Ellen Copeland's mental health recovery self-help strategies (including WRAP) | http://www.mentalhealthrecovery.com |
| National Empowerment Center (USA) | http://www.power2u.org |
| New Zealand Mental Health Commission | http://www.mhc.govt.nz |
| NIHME UK's mental health and recovery site (in development) | http://www.mentalhealthrecovery.org.uk |
| Ohio Department of Mental Health's guiding principles of the recovery model and outcomes | http://www.mh.state.oh.us/initiatives/outcomes/outcomes.html |
| Rethink's self-management project | http://www.rethink.org/recovery/self-management/index.htm |
| Survivors Network (UK) | http://www.healthy-life-styles.com |
At present many psychiatrists are sceptical of the movement. Doctors tend to be conservative and are not easy converts, and society depends on that wary scepticism and need for evidence, according us trust for our caution and dependability. However, the disadvantage of these same characteristics is an endemic resistance to change, making us slow to embrace the Government's aspiration to ‘shift the balance of power’ such that ‘front line staff and patients have the opportunity to think and work differently to solve old problems in new ways’ (Department of Health, 2001c ). However, if this ‘modernisation’ is genuinely underpinned by a ‘culture of mutual respect across all levels of the services’ and by the promised additional resources, then these changes may find resonance not only in the recovery movement, but also in the profession's own need and wish to change. For psychiatry in general, and general psychiatry in particular, are in difficulty – we have our need of recovery also.
The recovery emphasis offers a potentially invigorating vision for all involved. However, there is also justifiable suspicion that current services will superficially rebrand themselves to appear more modern, changing their names and headed paper, but without fully embracing the implications. It might be useful to emphasise that redefinition also carries a substantial responsibility to rethink, redesign and reorient. A forthcoming College Council Report redefining psychiatric rehabilitation for the 21st century poses just such a challenge for practitioners and their services (Royal College of Psychiatrists, 2004).
Some service users have felt threatened by a robustly expressed recovery model, feeling that they cannot recover and that to attempt further change is only to invite failure. Others have concluded that their lives have been so blighted that there is nothing to return to; they have come to terms with the severity and persistence of their difficulties and built a lifestyle around them. Some professionals are worried that redefining recovery as open to all, even in the presence of ‘chronic illness’, risks generating false hope and colluding with denial, and represents a misuse of language. There are also anxieties concerning what will happen to current services. One of us (P.W.) was surprised that, at a carefully constructed consultation with service users, explicitly convened to discuss how to develop a recovery-based service, users immediately voiced concerns and fears that day services, i.e. provision for those in continuing need of support, would be cut.
At present, professionals and patients both have misgivings and misunderstandings concerning what is meant by recovery. However, those leading the recovery movement are clear that it is neither about an unrealistic hope of magical transformation, nor about the impossible prospect of returning to whatever preceded illness. Instead, it is an open-ended and cautiously optimistic process of sketching out a path forward and developing hope for a more satisfactory life alongside whatever remains of the illness. A great deal remains to be learned concerning what prevents, and what promotes and sustains, recovery. There is even more uncertainty about why some recover and others do not. But despite all these tensions, there is much common ground between the aspirations of professionals and service users. Furthermore, living with these simple but central questions, and continuing to seek satisfactory answers, goes to the heart of psychiatric theory and practice. Setting recovery at the centre of our work may carry considerable hope for service users and staff alike.
Multiple choice questions
-
1 The modern concept of recovery is applicable:
-
a only to patients for whom cure is realistic
-
b only to patients who are considered to have a good clinical prognosis
-
c only to patients in their first episode
-
d to all patients presenting with severe mental health problems
-
e only to patients with self-limiting problems or adjustment disorders.
-
-
2 The following are recognised as helping patients to recover:
-
a having the example and companionship of others
-
b creative risk-taking
-
c someone who carries a sense of belief and confidence in their future
-
d vigorous challenging of the falseness of delusional beliefs and hallucinatory experiences
-
e being well looked after and relieved of the burden of personal responsibility.
-
-
3 Recovery is inhibited or arrested by:
-
a the individual's fear of change
-
b the organisation's fear of change in the social context
-
c lack of a vision for recovery in helping agencies
-
d involving service-user advocates
-
e unmonitored medication.
-
-
4 For the patient, transitions involved in the recovery process include:
-
a moving away from self-perception primarily as a mental patient
-
b getting back to normal
-
c moving towards discovering a positive self-image
-
d moving towards feeling able to take control of important aspects of his or her own life
-
e being cured.
-
-
5 It is important that recovery plans for individual patients are:
-
a standardised
-
b individualised
-
c evidence based
-
d standardised and evidence based
-
e individualised and evidence based.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | T | a | F |
| b | F | b | T | b | T | b | F | b | T |
| c | F | c | T | c | T | c | T | c | T |
| d | T | d | F | d | F | d | T | d | T |
| e | F | e | F | e | T | e | F | e | T |






eLetters
No eLetters have been published for this article.