In 1996, APT published an article with much the same title and by the same author. The article, which I wrote during 1995, examined the key issues concerning psychiatric nursing (Reference GournayGournay, 1996). The article began by describing the rationale for returning the focus of nursing to serious mental illness, citing the problems associated with the interventions of community psychiatric nurses (CPNs),Footnote 1 during the 1980s and early 1990s, working with people with common mental disorders in primary care. I argued that, in order to be effective, nurses needed to acquire clinical skills in the management of people with schizophrenia and other serious and enduring illnesses. In particular, I argued that, unless nurses received appropriate training in these clinical skills, merely shifting the focus of their work from institutions to the community, and the patient focus from those with common mental disorders to those with schizophrenia, would prove inadequate. I also advanced the argument that the problems of people with dual diagnosis, i.e. substance misuse and serious mental illness, needed particular attention. I drew attention to the neglected nursing roles of physical healthcare and medication management, and set out a range of areas in which education and training could be improved. The training priorities included the expansion of the Thorn Programme for training nurses in psychosocial interventions, and the continuing need to train a relatively smaller number of nurses in cognitive–behavioural therapy for common mental disorders. I concluded the article by arguing for a strengthening of evidence-based approaches to nurse education and suggesting the development of research in psychiatric nursing within the context of multidisciplinary investigations using randomised controlled trials and economic analyses.
In the 9 years that have passed since that article was written we have seen major changes in the National Health Service and in mental health policy. In this revisitation article I examine what has actually happened, in this intervening period, to the topics described above, and consider other topics that have since become important.
Serious mental illness
In 1990, a quinquennial review of community psychiatric nursing (Reference WhiteWhite, 1990) showed that 27% of the patients on CPN case-loads had a principal diagnosis of schizophrenia and a quarter of CPNs in the UK had no people with schizophrenia on their case-loads. Although there have been no further comprehensive surveys of community psychiatric nursing, it is clear that the vast majority of psychiatric nurses now work with people with schizophrenia within the context of the community mental health teams and the assertive outreach and crisis resolution services. Thus, the pendulum has indeed swung in the direction that was desired by so many community psychiatrists, and some nurses, in the early 1990s. However, there is now some concern that this shift has caused problems for people with common mental disorders.
As is noted below, there have been very substantial changes in the training provided to CPNs, with an emphasis on psychosocial interventions in serious mental illness (Box 1). However, there is very little training available to them in managing conditions such as obsessive–compulsive disorder, post-traumatic stress disorder, severe panic disorder and agoraphobia, and so on. It is now clear that the focus of CPNs on people with serious mental illness has consumed the CPN workforce entirely. Even so, there is a shortage of CPNs to provide skilled nursing care for people with serious and enduring mental illness. The reality is that several thousand more CPNs are needed to provide a reasonable standard of care for patients on community case-loads. Even if the money to do this were immediately available, it would not solve the problem. It takes several years to train a nurse and several years more to train them to a level where they may carry out effective community roles. Thus, it would be many years before the workforce would be sizeable enough to meet the needs of services. Furthermore, there are currently enormous difficulties in recruiting and retaining nurses in many parts of the UK and the problem is compounded by the well-acknowledged demographic time bomb, wherein disproportionate numbers of CPNs will retire over the next few years. Pay, conditions of service and the problem of house prices further exacerbate the problem. Given all of the difficulties in meeting the needs of people with serious and enduring mental illness, there seems little prospect that CPNs will have a significant role in the care of people with common mental disorders.
Box 1 Important roles of nurses in serious mental illness
-
• Family interventions
-
• Physical healthcare
-
• Medication management
-
• Working with dual diagnosis patients
-
• Cognitive–behavioural therapy for delusions and hallucinations
Contemporary nursing services and nursing roles
As noted above, the nature of community psychiatric nursing has changed considerably in the past decade or so, and the CPN may differ little in function from their case manager colleagues from other professions in the community teams. Certainly, the professional distinctions between nurses, social workers and occupational therapists have blurred somewhat, and the overlap of roles and the sharing of case management tasks seems to be to the advantage of patients.
By contrast, nurses in in-patient services continue in a custodial role. However, the nature of this role has changed. In-patient care has become one of the most difficult (and undervalued) areas of psychiatry. In my 1996 article, dual diagnosis was highlighted as an increasing problem, and there is little doubt that it still provides one of the single largest challenges in services. A number of recent studies (e.g. Reference Wright, Gournay and GlorneyWright et al, 2002) demonstrate the rising prevalence of this problem, particularly in inner cities. It is likely that, on the average acute ward, there are more people with a dual diagnosis than without. This, of course, has brought additional problems, and dual diagnosis is arguably a significant factor in the increasing levels of violence one sees in in-patient services. In turn, the in-patient population is increasingly likely to be sectioned under the Mental Health Act and to be non-compliant (non-concordant) with treatment. Thus, nurses in in-patient services have a more difficult job than in the asylum days.
The difficulties of the in-patient environment lead to problems of recruitment and retention to which no one really has a solution. The background work to the National Institute for Clinical Excellence (NICE) guidance on the short-term management of violent behaviour in psychiatric in-patient settings (National Institute for Clinical Excellence, 2005) emphasises the problem by citing the very high rates of injury to staff and patients during restraint episodes, and identifies a wide range of problems concerning the use of seclusion and training in control and restraint.
Neglected nursing roles
My 1996 article identified two areas as being particularly important: the physical health of people with serious mental illness and the managment of medication.
Physical health
The first, physical health in serious mental illness, remains a problem. However, my department at the Institute of Psychiatry has recently begun to develop modules of training for nurses working in both in-patient and community settings to deal with a very wide range of physical health issues that are of particular relevance for those with mental illness. This training includes health education and takes account of the difficulties of delivering interventions to people who may have cognitive deficits or very poor levels of motivation. The training emphasises the need to target areas such as cardiovascular and respiratory disease and sexual health and also recognises that this population may need active help to access an appropriate range of health services. There is no doubt that all those involved in nurse education must make major efforts to continue training initiatives, so that the physical health needs of those with serious and enduring mental illnesses are adequately met.
The management of medication
Medication management (Box 2) is an area in which there has been significant success. At the time of writing the 1996 article, I had begun developing educational materials for nurses on this topic. By 2004, a medication management training package for nurses had been subject to a randomised trial (Reference Gray, Wykes and EdmondsGray et al, 2004). The programme allocated 1 day a week for 10 weeks to teaching nurses to improve compliance in the manner described by Reference Kemp, Kirov and EverittKemp et al(1998). The training also included measures to improve nurses’ skills in using standardised instruments to assess mental state and the side-effects of medication and also to deal with patients’ beliefs and feelings about treatments. Nurses were provided with a range of other skills necessary to improve compliance. These skills centred on using a non-confrontational approach, based on the principles of motivational interviewing, and emphasised listening to the reasons why patients had difficulty complying and then negotiating compromise solutions.
Box 2 Components of medication management training for nurses
-
• Knowledge of psychopharmacology
-
• Mental state assessments
-
• Assessment of medication side effects
-
• Motivational interviewing skills
-
• Strategies to improve adherence
The trial demonstrated not only that nurses trained in these methods improved their skills and knowledge but, most importantly, that their intervention led to very significant changes in patient psychopathology, with a 17 point difference on the Positive and Negative Syndrome Scale (PANSS) score between the treatment and the control group.
This training package has now been disseminated to more than 1000 nurses across the UK, following another Institute of Psychiatry initiative to train trainers in all regions to deliver the training programme locally. At the time of writing, the package has also been disseminated across the states of Australia and there are similar training programmes planned for other European countries. The Reference Gray, Wykes and EdmondsGray et al(2004) study is now being replicated with funding from the Medical Research Council.
Nurse prescribing
Although this training innovation should lead to major improvements in patients’ compliance with drug regimens, nurse prescribing is arguably a more important development. The arguments for nurse prescribing are set out in detail in Reference Gournay and GrayGournay & Gray (2001). Nurse prescribing is now a reality and, although psychiatric nurses are somewhat behind their general nursing counterparts in obtaining prescriptive authority, training programmes in prescribing are being set up at a number of universities across England. Within a few years it is envisaged that thousands of psychiatric nurses will be carrying out a range of prescribing tasks up to and including prescribing new psychiatric drugs independently (albeit under the overall supervision of a consultant psychiatrist). The principal advantage of nurse prescribing is that it will free up the psychiatrist to deal with the complex and difficult cases, leaving the routine to experienced nurses. To ensure that this development is both safe and effective, we need to ensure that the training and supervision of nurses are adequate and that the necessary resources are released to continue funding the initiative appropriately. Furthermore, providing nurses with prescriptive authority is clearly an important topic for evaluation and there is an obvious need to assess clinical and economic outcomes of nurse prescribing.
The nurse cognitive–behavioural therapist
The 1996 article argued for the further development of training programmes for nurses in cognitive–behavioural therapy. Regrettably, this expansion has not come to fruition, and although there are a few hundred such qualified nurses, cognitive–behavioural therapy for people with common mental disorders is scarce, to say the least, outside of specialist centres. There has been a modest increase in the number of clinical psychology training places, but the expansion of the cognitive–behavioural therapy workforce has been completely overwhelmed by a widening of the evidence base for the efficacy of this approach. This has been emphasised even further by the NICE guidance on schizophrenia, which recommends the provision of cognitive–behavioural therapy to deal with hallucinations and delusions (National Institute for Clinical Excellence, 2002). It seems obvious that nurses are in an ideal position to become the agents for the delivery of cognitive–behavioural therapy. However, they will need a more intensive training than that currently offered on psychosocial intervention programmes (see below). Realistically, such intensive training will not be available for some time to come, as training providers are still dealing with the backlog caused by the absence of appropriate basic training for CPNs over a number of years.
Education and training
The 1996 article set out the background to the Thorn Nurse Initiative (Reference Gournay and BirleyGournay & Birley, 1998), which at that time had delivered training to a few dozen CPNs. The Thorn Programme has now been replicated in many universities across the UK, and similar training programmes in psychosocial intervention have been developed at various educational levels, up to and including master’s degree, by other universities and the Sainsbury Centre for Mental Health. We now have thousands of mental health professionals trained in psychosocial interventions, and most community mental health teams include several workers who have received basic training in assertive community treatment methods, basic cognitive–behavioural therapy techniques for dealing with hallucinations and delusions, and family interventions.
The Thorn Programme opened its doors to other professionals several years ago and now nurses occupy about two-thirds of course places. However, while all this is very welcome, the limitations of such training need to be emphasised. What these programmes have done is to provide mental health professionals with basic skills across a number of areas. There is still a need, as with cognitive–behavioural therapy, to equip more professionals with more advanced skills in family interventions for those with schizophrenia and their carers, and also to develop specialist programmes for other groups, including those with personality disorders and the increasing community population who have fallen foul of the criminal justice system.
Undergraduate nurse education
In 1995 I highlighted some of the shortcomings of undergraduate nurse education, including the problems of teachers being located in universities rather than in clinical centres. Many departments of nursing in universities were then characterised by a preponderance of anti-psychiatric philosophy in many programmes, and lack of important information in training courses regarding the biological aspects of mental illness and psychopharmacology. There has been progress in some of these areas, although clinically focused training is probably an ideal rather than a reality.
The 1996 article also identified the problems of nurses who had been trained in large institutions and needed an updating in their skills. There have been several recent initiatives, including efforts by the National Institute for Mental Health (England) to improve the skills of nurses working in in-patient settings, and these are to be welcomed. However, there are now some ominous signs that, following the moves to make nursing an all-graduate profession, psychiatric and, indeed, learning disabilities nursing may disappear in their present form. For many years it has been possible to train and register as a psychiatric, rather than a general or learning disabilities nurse. However, there are moves afoot to set up generic training, so that one has to qualify as a generic registered nurse before moving on to training in psychiatric nursing as a post-qualifying specialty. In my opinion, this would compromise a number of the aforementioned initiatives. However, in the wider circles of nursing, the debate continues and it may yet be several years before any resolution, one way or the other, is achieved.
Other areas
High secure hospitals
Two areas that were not discussed in any detail in my 1996 article have now become prominent in psychiatric nursing. The first is the issue of the expansion of forensic services. Nursing in the high secure hospitals has been beset by problems over the years and these have, of course, been raised in the two notorious reports into care and treatment at Ashworth Hospital (Department of Health, 1992, 1999). One positive effect of these scandals has been the investment in nursing in these institutions. Nevertheless, it must be said that this work is extremely demanding, with nurses (and indeed other staff) trying to balance the needs of the patient against public safety. In turn, attempting to provide therapeutic interventions within a custodial environment presents enormous challenges.
Although there are very welcome initiatives aimed at transferring many of the female patients to less intimidating environments, forensic services as a whole continue to expand. Indeed, because of the shortage of beds, forensic populations frequently overspill into local mental health services and the mixed custodial/care role of nurses is now much more mainstream than a decade ago. This is reflected in the new NICE guidelines (National Institute for Clinical Excellence, 2005) that set out guidance and methods to improve security (such as closed-circuit television) and place an understandable emphasis on searching, restraint, seclusion and the use of rapid tranquillisation. While this guidance will be very useful, it none the less emphasises the changing nature of psychiatric care.
Prisons
Yet another area of expansion of mental health services is prison healthcare. From 2005, prison healthcare becomes the responsibility of the NHS and prisoners should expect the same standard of mental healthcare as patients in local services. At the time of writing, there are no fewer than 60 prisons with in-reach programmes, i.e. nurses, doctors and other health professionals, employed by local services, are spending part or all of their working day delivering mental healthcare and treatment to prisoners in our overcrowded jails. Nurses, and indeed other professionals, may now be party to what Len Stein, the pioneer of assertive community treatment, once called ‘transinstitutionalisation’, as the care and treatment of mentally ill individuals passes gradually from hospital to prison. The role of the psychiatric nurse in this respect has undergone a fundamental shift.
Care or custody?
In addition to the increase in care for people with mental illness who have contact with the criminal justice system, there are now growing numbers of people with personality disorders being cared for within our services. The Government’s Dangerous and Severe Personality Disorder Initiative is now being piloted in two high secure hospitals (Rampton and Broadmoor) and in two prisons. There are significant numbers of nurses caring for these patients/prisoners, and they are in a very uneasy position as both custodians and treatment agents. Nurses (and their colleagues in psychiatry), may be wondering exactly what their role is, as the patient populations differ considerably from people with identifiable psychiatric illnesses. At present, some nurses are unhappy about the prospect of this more custodial role and are understandably asking whether this is part of a remit for a profession with primary focus on caring for those who are unable to care for themselves because of illness. As in the rest of psychiatry, there are uneasy questions to be asked regarding the age-old topics of mad versus bad and custodian versus carer.
Conclusions
In summary, the years since my original article have seen many changes in mental healthcare, which have, to a greater or lesser extent, been mirrored within psychiatric nursing. There is no doubt that the skills of psychiatric nurses have improved in many respects; in other areas, such as physical healthcare, there has been little change. Furthermore, the young (or indeed older) person entering the nursing profession will generally have a higher standard of education than in previous generations and the psychiatric nurses who qualify over the next few years will do so with an honours degree. Perhaps this fact identifies the most important shift yet to come. It seems extremely likely that the caring tasks undertaken by psychiatric nurses in years gone by, which included helping people with schizophrenia in their activities of daily living, attending to the incontinence of elderly mentally ill patients and simply looking after those who cannot care for themselves, may no longer be the province of the nurse – these essential tasks may be delegated to other, less-well paid, individuals who are now increasingly populating our workforces.
MCQs
-
1 Psychiatric nursing is expanding into:
-
a primary care
-
b CBT for common mental disorders
-
c forensic areas
-
d general hospitals.
-
-
2 In 1990, the proportion of people with schizophrenia on CPN case-loads was:
-
a 87%
-
b 67%
-
c 47%
-
d 27%.
-
-
3 One of the most important neglected nursing roles is:
-
a public education
-
b GP liaison
-
c physical healthcare
-
d community team management.
-
-
4 Nurses working within the Dangerous and Severe Personality Disorder Initiative are now located in:
-
a one prison and one high secure hospital setting
-
b two prisons and two high secure hospital settings
-
c three prisons and three high secure hospital settings
-
d four prisons and four high secure hospital settings.
-
-
5 NICE guidance to be published early in 2005 of relevance to psychiatric nursing focuses on:
-
a schizophrenia
-
b depression
-
c disturbed/violent behaviour
-
d computer-assisted treatments.
-
MCQ answers
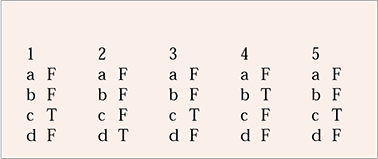
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | F | a | F |
| b | F | b | F | b | F | b | T | b | F |
| c | T | c | F | c | T | c | F | c | T |
| d | F | d | T | d | F | d | F | d | F |





eLetters
No eLetters have been published for this article.