Depersonalisation is defined in DSM–IV as an
‘alteration in the perception or experience of the self so that one feels detached from and as if one is an outside observer of one’s mental processes or body’ (American Psychiatric Association, 1994: pp. 488–490).
In ICD–10, depersonalisation is explicitly linked with the related phenomenon of derealisation, in the diagnostic category depersonalisation–derealisation syndrome,
‘in which the sufferer complains that his or her mental activity, body, and/or surroundings are changed in their quality, so as to be unreal, remote, or automatized’ (World Health Organization, 1992: p. 171).
Although this definition encompasses both depersonalisation and derealisation, the diagnostic criteria require ‘either or both’ phenomena to be present, so the condition can be diagnosed on the basis of depersonalisation or derealisation alone.
Box 1 gives a summary of ICD–10 and DSM–IV diagnostic criteria for depersonalisation disorder.
Box 1 Diagnostic criteria for depersonalisation disorder, adapted from ICD–10 and DSM–IV
ICD–10
Either or both of (a) and (b), plus (c) and (d):
-
a Depersonalisation symptoms
-
b Derealisation symptoms
-
c Acceptance that this is a subjective change not imposed by any outside agency
-
d Clear sensorium
DSM–IV
-
a Feeling detached from one’s mental processes or body
-
b Intact reality testing
-
c Clinically significant distress and/or functional impairment
-
d Symptoms do not occur exclusively as part of another disorder or due to direct physiological effects of a substance
Our article is intended mainly as a discussion of the primary disorder, but it may also be applicable to the assessment and treatment of patients in whom depersonalisation has become chronic and pervasive in the context of another disorder.
Nosology
Both ICD–10 and DSM–IV betray uncertainty as to the nosological status of depersonalisation: in the former, it is included under the vague heading of ‘other neurotic disorders’, whereas in the latter it is listed under dissociative disorders, an equally problematic classification, as the hallmark of true dissociation is a lack of subjective awareness of change. By contrast, sufferers from depersonalisation are all too aware of a disturbing change in their experience of themselves and/or their surroundings – indeed, in the primary disorder, this awareness of change is the very essence of the presenting complaint. Other ways in which depersonalisation differs from dissociative disorders are explored at length in Reference Hunter, Phillips and ChalderHunter et al(2003).
Epidemiology
Depersonalisation may occur as a transient phenomenon in healthy individuals, particularly in the context of fatigue, during or after intoxication with alcohol and/or drugs, or in situations involving serious danger (Reference Noyes and KlettiNoyes & Kletti, 1977). It may also occur as a chronic, disabling and clinically significant phenomenon, either as a primary disorder or secondarily in a range of neuropsychiatric settings (e.g. major depressive disorder, schizophrenia, temporal lobe epilepsy). Until recently, there was a prevailing consensus that
‘the number of individuals who experience this disorder in a pure or isolated form is small. More commonly, depersonalization-derealization phenomena occur in the context of depressive illnesses, phobic disorder, and obsessive-compulsive disorder’ (World Health Organization, 1992: p. 172).
However, epidemiological reviews (Reference Bebbington, Marsden and BrewinBebbington et al, 1997; Reference Hunter, Sierra and DavidHunter et al, 2004) conclude that clinically significant depersonalisation may affect 1–2% of the general population, with a gender ratio of about 1:1. In psychiatric populations, depersonalisation is encountered with surprising frequency: one survey (Reference Brauer, Harrow and TuckerBrauer et al, 1970) found that it occurred in 80% of a sample of psychiatric in-patients, and was chronic and disabling in a fifth of this group. Other work (Reference StewartStewart, 1964; Reference Simeon, Gross and GuralnikSimeon et al, 1997) suggests that depersonalisation might be the third most common psychiatric symptom after anxiety and low mood.
Although such studies do not always distinguish between primary and secondary depersonalisation, it does seem likely that the primary disorder is considerably more common than previously thought. Reflecting this, two major case series have recently been published (Reference Baker, Hunter and LawrenceBaker et al, 2003; Reference Simeon, Knutelska and NelsonSimeon et al, 2003b ), comprising 204 and 117 cases respectively.
Phenomenology
Although empirical studies of depersonalisation are a recent development, there are some rich phenomenological descriptions in older literature (e.g Reference SchilderSchilder, 1928; Reference Mayer-GrossMayer-Gross, 1935; Reference Shorvon, Hill and BurkittShorvon et al, 1946; Reference AcknerAckner, 1954), and these remain invaluable to any present-day clinician attempting to understand the condition. Reference Mayer-GrossMayer-Gross (1935) includes an array of patient self-reports, which are strikingly similar to descriptions given by patients attending the Maudsley depersonalisation clinic (Reference Phillips, Sierra and HunterPhillips et al, 2001a ; Reference Baker, Hunter and LawrenceBaker et al, 2003). A systematic comparison of historical and current cases (Reference Sierra and BerriosSierra & Berrios, 2001) confirms that the disorder shows a reliable phenomenological consistency.
Self-reports emphasise the strange and disturbing quality of the depersonalisation experience: some patients report feeling ‘like a robot’, ‘different from everyone else’ and ‘separate from myself’ (this last should be understood metaphorically rather than taken to imply autoscopic experience). Others describe feeling ‘half-asleep’ or ‘as if my head is full of cotton wool’, with associated difficulties in concentration. External reality may also be strangely altered: it may appear somehow artificial – as if ‘painted, not natural’, or ‘two-dimensional’ or ‘as if everyone is acting out a role on a stage, and I’m just a spectator’. Even though the world does not necessarily look unreal, it is nevertheless experienced as ‘less interesting and less alive than formerly’. A reduction in, or complete absence of, bodily feelings is often described (‘as if I were a phantom body’, ‘my hands seem not to belong to me’), as are reduced intensity in the experience of thirst, hunger and physical pain. Another frequent theme is a reduction or loss of emotional responses: ‘my emotions are gone, nothing affects me’, ‘I am unable to have any emotions, everything is detached from me’. This loss of emotional reactivity may be particularly disturbing for the patient and those around them, and can have serious adverse effects on intimate relationships.
Clinical features and assessment
A thorough clinical assessment should include a full psychiatric and general medical history and mental state examination. Neurological examination may be appropriate if the history is suggestive of epilepsy or other organic disease (Reference Lambert, Sierra and PhillipsLambert et al, 2002). In the history and mental state examination, particular attention should be paid to the following areas.
Nature of symptoms
As outlined above, depersonalisation may involve various types of alteration in subjective experience, and its phenomenology is often more complex than might be guessed from the descriptions in ICD–10 and DSM–IV. This should be borne in mind when assessing patients with this condition, and it can be useful to subdivide one’s assessment into four symptom categories (Box 2): depersonalisation, derealisation, desomatisation and de-affectualisation. Symptoms in any of these four domains should alert the clinician to the possibility of depersonalisation.
Box 2 Division of symptoms of depersonalisation disorder into four major domains

| Depersonalisation | Disturbing sense of being ‘separate from oneself’, observing oneself as if from outside, feeling like a robot or automaton |
| Derealisation | Threatening sense of unfamiliarity or unreality in the environment, perceptual anomalies may be present, other people may feel like actors in a play |
| Desomatisation | Diminution, loss or alteration of bodily sensations, sense of disembodiment; there may be a raised pain threshold |
One striking feature of the de-affectualisation is that it is not usually accompanied by an objectively blunted affect such as that seen in schizophrenia (Reference AcknerAckner, 1954; Reference TorchTorch, 1978; Reference Sierra and BerriosSierra & Berrios, 1998). This preservation of normal affect can help differentiate the condition from major depression. Rating scales can be helpful for checking symptoms and tracking changes over time – the Cambridge Depersonalisation Scale (Reference Sierra and BerriosSierra & Berrios, 2000) is particularly useful (this is a ‘trait’ scale, but there is also a modified ‘state’ version).
Onset and pattern of symptoms
In the largest case series to date (Reference Baker, Hunter and LawrenceBaker et al, 2003), mean age at onset was 22.8 years, although 30% reported age at onset below 16 years. The typical history is that symptoms are initially episodic, with episodes becoming longer and more severe until depersonalisation is pervasive and unremitting. Within this, however, there may still be some fluctuation in the intensity of symptoms, even if they are never entirely absent. Some patients are able to identify factors that produce a transient change in their condition – artificial light and crowds are often described as exacerbating the symptoms, whereas physical exercise and alcohol may provide some temporary relief. A small number of patients develop alcohol dependence as a result, although this seems to be uncommon (Reference Baker, Hunter and LawrenceBaker et al, 2003). Sometimes symptoms are apparently precipitated by a period of psychological stress: examples from our clinical experience include caring for a terminally ill relative and protracted relationship break-ups. Although precipitants are not always identifiable, a search for a precipitating event (or, more commonly, series of events) should always form part of the assessment. Some patients attribute the onset of symptoms to an episode of illicit drug use, particularly cannabis, but the subsequent course and nature of their condition does not appear to differ markedly from cases not involving drug use (Reference Medford, Baker and HunterMedford et al, 2003). A history of brief stereotypical episodes of depersonalisation accompanied by cognitive and/or behavioural disturbance is suggestive of temporal lobe epilepsy and should be investigated appropriately.
Duration of symptoms
Often, patients have symptoms for many years before consulting a psychiatrist or other doctor. In the case series reported by Reference Baker, Hunter and LawrenceBaker et al(2003), mean duration of symptoms was over 12 years at the time of first contact with a specialist depersonalisation clinic. To some extent this reflects the fact that the condition is poorly understood, and clinicians should be sensitive to the possibility that patients may have had frustrating experiences with healthcare professionals and may have received inaccurate and unhelpful information in the past.
Other associated features
Patients not infrequently describe a tendency to philosophical rumination, e.g. ‘If I’m not really me, then who am I?’, ‘How can things be real but seem not real?’ Such thoughts tend to be circular and fruitless, and may also become repetitive and intrusive. They may be accompanied by obsessional self-monitoring and self-observation, which may become chronic and refractory (Reference Shorvon, Hill and BurkittShorvon et al, 1946; Reference SchilderSchilder, 1950). The clinical impression in such cases is that these tendencies often exacerbate the condition, by heightening the sense of unreality and existential unease, and thus contributing to the perpetuation of symptoms. Reference TorchTorch (1978) provides a particularly useful discussion of the relationship between obsessional tendencies and depersonalisation, highlighting the relevance of the pre-morbid personality and illuminating the difficulties encountered in treating such cases.
Alterations in perception may also be described, such as a reduction (or, more rarely, an increase) in the vividness of colours or the impression that visual perceptions are oddly flat and two-dimensional. Other perceptual anomalies and hypo- or hyperacuity may also occur (Reference Baker, Hunter and LawrenceBaker et al, 2003).
When loss of bodily sensation is a prominent feature, patients may seek relief through self-injurious behaviour such as cutting themselves, although this is far more common when depersonalisation occurs in the context of a wider disturbance of personality.
Presence or absence of other psychopathology
In particular, features of depression, anxiety and panic disorders, and obsessive–compulsive disorder (OCD) should be sought. A recent survey of 109 patients with OCD found that about 6% satisfied criteria for comorbid depersonalisation disorder (Reference Lochner, Seedat and HemmingsLochner et al, 2004). Furthermore, as described above, patients with chronic depersonalisation often exhibit marked obsessional tendencies even if they fall short of satisfying criteria for a diagnosis of OCD.
It is also important to explore depersonalisation-related phenomena to satisfy oneself that these are not, in fact, psychotic experiences. Patients with depersonalisation will frequently use the descriptor ‘as if’ when attempting to explain their experiences – ‘as if I were an automaton’, ‘as if I did not really exist’, ‘as if the world is not real’. These experiences are hard to capture in words, so it is not surprising that patients rely heavily on similes or metaphors when attempting to communicate them. However, if the clinician is not sufficiently alive to the fact that these are indeed similes or metaphors and that insight is preserved, a psychotic disorder may be erroneously diagnosed. We have seen a number of cases where patients with primary depersonalisation had been previously misdiagnosed with schizophrenia and started on antipsychotic medications, which had invariably worsened their symptoms. In general, establishing the presence or absence of other symptoms should enable the distinction between primary and secondary depersonalisation, although if depersonalisation and related phenomena are the sole or predominant complaint, it may be reasonable to treat the case as one of primary depersonalisation even when there is a history of other symptoms. For example, many patients with depersonalisation (43% in Reference Baker, Hunter and LawrenceBaker et al, 2003) describe a previous history of anxiety or panic attacks, and in some cases there may be a clear temporal relationship between these symptoms and symptoms of depersonalisation. However, in other individuals, there may be no such apparent relationship, and in either case it may be that symptoms of anxiety or panic have long since disappeared by the time the patient seeks help regarding depersonalisation. In this situation, a diagnosis of primary depersonalisation provides the best descriptor of the current problems. In some patients, symptoms of depersonalisation and anxiety occur together, apparently feeding each other – the strangeness and sense of isolation occasioned by depersonalisation fuels the anxiety and the depersonalisation then intensifies as a defence against this anxiety. The relationship between depersonalisation and anxiety is discussed further in the section on psychological treatments below.
Aetiological considerations
Reference Mayer-GrossMayer-Gross (1935) conceived of depersonalisation as a ‘pre-formed response of the brain’ – meaning that he believed it to be a normal response to threat which could become fixed and maladaptive in some individuals. Seventy years later, this remains an attractive idea. Healthy individuals exposed to life-threatening danger almost always report at least some features of depersonalisation (Reference Noyes and KlettiNoyes & Kletti, 1977), supporting the idea that it is a normal part of the response to overwhelming threat. It may be that in susceptible individuals this response is more readily triggered and that, once established, depersonalisation becomes fixed and pervasive. Both psychological (Reference SedmanSedman, 1970) and biological (Reference Sierra and BerriosSierra & Berrios, 1998) models suggest that, in depersonalisation, normal emotional responses are ‘shut down’, leading to de-affectualisation with associated loss of emotional tone in the experience of oneself (depersonalisation, desomatisation) and one’s surroundings (derealisation). Once established, the unpleasant and unfamiliar feelings and experiences that comprise the depersonalisation symptom complex may in turn generate further anxiety, and so on in a vicious cycle. This may be the basis of the relationship between depersonalisation and anxiety seen in some patients, as mentioned above, and it forms the cornerstone of a recent cognitive–behavioural conceptualisation (Reference Hunter, Phillips and ChalderHunter et al, 2003).
Neurological factors
Recent functional neuroimaging (Reference Phillips, Medford and SeniorPhillips et al, 2001b ) and psychophysiological (Reference Sierra, Senior and DaltonSierra et al, 2002) studies have found objective evidence of an abnormal response to emotional stimuli, consistent with patients’ reports of loss of emotional reactivity. The neural substrate for the ‘shutting down’ of emotional responses is hypothesised (Reference Sierra and BerriosSierra & Berrios, 1998) to be a combination of prefrontal regions inhibiting limbic areas (particularly the amygdala) and reciprocal actions of the right dorsolateral prefrontal cortex and anterior cingulate cortex (Reference Phillips, Medford and SeniorPhillips et al, 2001b ). The anterior cingulate cortex is thought to play an important role in the regulation of normal emotional responses (Reference DrevetsDrevets, 2000). In the functional magnetic resonance imaging study by Reference Phillips, Medford and SeniorPhillips et al (2001b ), an area of the right dorsolateral prefrontal cortex was activated in patients with depersonalisation when they viewed aversive scenes; during the same experimental task, ‘normal’ controls did not show such activation, but they did show activation in the anterior cingulate cortex. Other work has suggested that it is the anterior cingulate cortex that may have a direct role in depersonalisation: a positron emission tomography study in which tetrahydrocannabinol (THC) was administered to healthy volunteers found a significant positive correlation between anterior cingulate activation and the degree of THC-induced depersonalisation (Reference Mathew, Wilson and ChiuMathew et al, 1999). Thus, there is converging evidence that, in depersonalisation, prefrontal cortical areas act to inhibit the neural circuits that normally form the substrate of emotional experience, but precise details of the underlying functional neuroanatomy await clarification.
Psychoanalytical models
Psychoanalytical theorists have presented various models for understanding the genesis and maintenance of depersonalisation. These vary widely, but a common theme is the idea of depersonalisation as a defence against, or result of, psychic conflicts that threaten the integrity of the self. These ideas are briefly reviewed by Reference AcknerAckner (1954). Freud described his own experience of an isolated episode of depersonalisation in a letter to Romain Rolland, his forensic self-scrutiny giving rise to some interesting observations, whether or not one finds his psychoanalytical exegesis of the experience convincing (Reference FreudFreud, 1941). Reference TorchTorch (1987) gives the most complete contemporary psychoanalytical account, emphasising the role of overly demanding parents and consequent feelings of inadequacy, leading to obsessive self-scrutiny. The general applicability of this model is questionable, but a number of patients whom we have seen have displayed family dynamics similar to those described by Torch, and this may be an area where further study is warranted. A study examining childhood experiences of adults with depersonalisation found an association between emotional abuse in childhood and subsequent symptoms of depersonalisation (Reference Simeon, Guralnik and SchmeidlerSimeon et al, 2001b ).
Endocrinology
Endocrine studies of patients with depersonalisation have found a striking negative correlation between severity of depersonalisation and urinary norepinephrine (Reference Simeon, Guralnik and KnutelskaSimeon et al, 2003a ). However, there are conflicting data on the relationship between depersonalisation and cortisol levels, with two studies (Reference Morozova, Gamper and DubininaMorozova et al, 2000; Reference Stanton, David and CleareStanton et al, 2001) reporting low salivary cortisol, but another (Reference Simeon, Guralnik and KnutelskaSimeon et al, 2001a ) finding raised plasma cortisol.
Treatment
Recognising and diagnosing the condition may in itself have therapeutic benefits. Many patients express the sense that their problems are baffling and perhaps even unique – a recurring theme among patients attending our specialist depersonalisation clinic is the relief of discovering, first, that their problem is recognised and described by psychiatry and, second, that they are not the only individuals to suffer from the condition. For this reason alone, patients may benefit from referral to a specialist clinic. But we also hope that dissemination of information on depersonalisation through articles such as this will enable general psychiatrists to feel more confident about diagnosing and treating the condition. With regard to specific treatment interventions, both pharmacological and psychological approaches may be of value. We consider these separately here, although in practice it is often appropriate to combine them.
Pharmacological approaches
There is no recognised drug treatment for depersonalisation, and at the time of writing no drugs are licensed for its treatment in the UK. However, there is some evidence to support the use of selective serotonin reuptake inhibitor (SSRI) antidepressants, and more recently the combination of lamotrigine and an SSRI has shown promise. The evidence is reviewed briefly here, but it should be stressed that it is composed entirely of small studies and isolated case reports, and that large randomised controlled trials have not been performed.
SSRIs
Various lines of evidence hint at serotonergic dysfunction in depersonalisation. Reference Simeon, Hollander and SteinSimeon et al(1995) found that the partial serotonin agonist metachlorophenylpiperazine induced depersonalisation in healthy volunteers, and there are case reports of depersonalisation being apparently precipitated by initiation (Reference Black and WojcieszekBlack & Wojcieszek, 1991) and discontinuation (Reference Hollander, Hwang and MullenHollander et al, 1993) of an SSRI, the drugs involved being fluoxetine and clomipramine respectively. (Although clomipramine is classed as a tricyclic, its mode of action is far more akin to that of the SSRIs than to other tricyclics.) There are isolated case reports (Reference Ratliff and KerskiRatliff & Kerski, 1995; Reference Strohle, Kumpfel and SonntagStrohle et al, 2000) describing good response to SSRIs, the latter in a patient with depersonalisation in the context of multiple sclerosis. A small study by Reference Hollander, Liebowitz and DeCariaHollander et al(1990) found some evidence of therapeutic benefit for SSRIs, although the patients in this study were a heterogeneous group with high levels of psychiatric comorbidity. Reference Simeon, Stein and HollanderSimeon et al(1998) studied the effects of clomipramine in seven patients with primary depersonalisation, but found significant benefits in only two cases. A large randomised placebo-controlled trial of fluoxetine showed little specific antidepersonalisation effect (Reference Simeon, Guralnik and SchmeidlerSimeon et al 2004).
Lamotrigine
Our own clinical experience has been that many patients referred to our clinic have been on an SSRI for prolonged periods with little or no impact on their symptoms, and this has led us to investigate other potential pharmacotherapies, in particular the anticonvulsant lamotrigine. Lamotrigine acts at the presynaptic membrane to reduce the release of glutamate, and it has been shown to reverse depersonalisation-related phenomena induced by the N-methyl-d-aspartate (NMDA) receptor antagonist ketamine in healthy individuals (Reference Anand, Charney and OrenAnand et al, 2000). In the absence of large-scale randomised controlled trials, and in the presence of conflicting published data (see below), the efficacy of lamotrigine (whether as monotherapy or in conjunction with an SSRI) is not yet firmly established, but it is often our first-line treatment for the condition.
An initial study of lamotrigine monotherapy in four patients with primary depersonalisation found substantial benefits in all cases (Reference Sierra, Phillips and LambertSierra et al, 2001), but a subsequent placebo-controlled cross-over study of nine patients found no significant benefits from the drug (Reference Sierra, Phillips and IvinSierra et al, 2003). Nevertheless, our clinical experience suggests that lamotrigine does benefit some patients with primary depersonalisation, although this effect may be more reliable when the drug is given in conjunction with an SSRI (further details available from the authors on request).
Lamotrigine should be initiated at a starting dose of 25 mg/day, with the dose gradually increased at fortnightly intervals. Patients should be monitored for haematological and dermatological side-effects (refer to British National Formulary guidelines for more details; British Medical Association & Royal Pharmaceutical Society of Great Britain, 2004). Stevens–Johnson syndrome is a rare but potentially serious adverse effect. Blood levels of lamotrigine should also be monitored, particularly if the drug is used in combination with sertraline, as there is a report of two individuals with epilepsy in whom sertraline apparently produced marked changes in lamotrigine levels (Reference Kaufman and GernerKaufman & Gerner, 1998), although it would appear that such interactions are rare.
When lamotrigine cannot be tolerated or is ineffective, clonazepam may be useful, although the usual caveats regarding prescription of benzodiazepines apply. Although literature on the use of clonazepam in depersonalisation is scarce, one study found that it reduced levels of caffeine-induced derealisation in a single individual (Reference Stein and UhdeStein & Uhde, 1989). A role for anxiolytic drugs is also suggested by the data of Reference NullerNuller (1982), and a recent case report describes an individual with primary depersonalisation successfully treated with a combination of clonazepam and citalopram (Reference SachdevSachdev, 2002). As Sachdev notes, the same combination has apparently been found effective by a number of contributors to an internet bulletin board for people with depersonalisation.
Reference Nuller, Morozova and KushnirNuller et al(2001) found a significant transient beneficial effect of naloxone infusion on symptoms of depersonalisation in 10 of 14 patients studied. This intriguing result suggests a possible role of the endogenous opioid system in the pathogenesis of depersonalisation, and the possibility that anti-opioid drugs may have therapeutic value. To date, this hypothesis has not been explored further in the literature, despite the impressive results from this pilot study. However, one open-label study has found evidence of a role for the opioid receptor antagonist naltrexone in treating dissociative symptoms in the context of borderline personality disorder (Reference Bohus, Landwehrmeyer and StiglmayrBohus et al, 1999), and it may be of note that the selective kappa opioid receptor agonist enadoline has been found to induce depersonalisation, although this was only one of numerous reported physical and psychological effects (Reference Walsh, Strain and AbreuWalsh et al, 2001).
Psychological approaches
As with pharmacotherapy, there is no recognised psychological treatment for depersonalisation. There are isolated case reports describing successful treatment using psychoanalytical therapy (Reference TorchTorch, 1987), behavioural therapy (Reference Sookman and SolyomSookman & Solyom, 1978) and directive therapy (Reference BlueBlue, 1979), although in the latter two reports the patients described have high levels of comorbid psychopathology and may not be cases of primary depersonalisation.
More recently, a cognitive–behavioural model of depersonalisation has been proposed (Reference Hunter, Phillips and ChalderHunter et al, 2003). It is based on the idea, touched on earlier in this article, that anxiety and depersonalisation are intimately related, and that depersonalisation is best conceptualised as related to anxiety disorders rather than to dissociative conditions.
The model suggests that there are various ways in which depersonalisation may initially arise, related to some external psychological stressor and/or as a consequence of a change in mental state (e.g. low mood, anxiety, drug use). Crucially, in those in whom depersonalisation becomes chronic and pathological, the appearance of depersonalisation features is interpreted as highly threatening (‘catastrophic attribution’), leading to a range of cognitions and behaviours that can serve to perpetuate and intensify the symptoms. This leads to a number of practical suggestions for treatment, aimed at psychoeducation, the reduction of avoidant ‘safety behaviours’ (such as avoiding social situations) and excessive self-observation (e.g. looking in the mirror to see if one has changed), and challenging the ‘catastrophic’ attributional style (e.g. ideas such as ‘My brain is not working’). This model forms the basis for the cognitive–behavioural therapy (CBT) approach used in our clinic, which is undertaken by a clinical psychologist trained in CBT, usually in combination with pharmacotherapy initiated and monitored by a psychiatrist.
Relaxation techniques such as progressive muscular relaxation do not appear to be of benefit in depersonalisation. Indeed, it has been noted that patients with depersonalisation may actually experience an increase in symptoms after using progressive muscular relaxation (Reference FewtrellFewtrell, 1984). However, techniques aimed at refocusing attention away from introspection and self-observation may yet prove to be of benefit, and to this end the use of biofeedback methods may be a worthwhile avenue for future study.
MCQs
-
1 The following are true regarding depersonalisation disorder:
-
a onset is usually over the age of 30
-
b patients typically exhibit nihilistic delusions
-
c perceptual anomalies may be present
-
d it may be apparently precipitated by drug use
-
e placebo-controlled trials have demonstrated a role for SSRIs.
-
-
2 In depersonalisation disorder, the following are typical symptoms:
-
a difficulty in concentrating
-
b loss of emotional reactivity
-
c compulsive overeating
-
d anxiety
-
e autoscopy.
-
-
3 The following have been described in association with depersonalisation disorder:
-
a reduced amygdala response to aversive images
-
b raised plasma cortisol levels
-
c raised salivary cortisol levels
-
d a correlation with emotional abuse in childhood
-
e history of panic attacks.
-
-
4 Regarding treatment for depersonalisation disorder:
-
a there are well-established treatment guidelines
-
b olanzapine is usually helpful in reducing symptoms
-
c fluoxetine has recently been shown to be effective in depersonalisation
-
d CBT may have a role
-
e clonazepam is useful in some patients.
-
-
5 Regarding the use of lamotrigine in depersonalisation disorder:
-
a randomised controlled trials have confirmed its efficacy
-
b Stevens–Johnson syndrome is a recognised adverse effect
-
c haematological and biochemical indices should be monitored
-
d lamotrigine may be more effective when given with an SSRI
-
e lamotrigine may interact adversely with sertraline.
-
MCQ answers
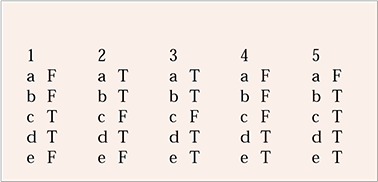
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | F | a | F |
| b | F | b | T | b | T | b | F | b | T |
| c | T | c | F | c | F | c | F | c | T |
| d | T | d | T | d | T | d | T | d | T |
| e | F | e | F | e | T | e | T | e | T |





eLetters
No eLetters have been published for this article.