There is considerable concern about the access of people from Black and minority ethnic groups to appropriate healthcare (Reference Dyson, Smaje, Culley and DysonDyson & Smaje, 2001). This may reflect real or perceived barriers to services because of disadvantage related to minority status. Several approaches have been proposed to address this problem, one of which has been to increase cultural diversity training for all clinical staff, including psychiatrists. It is the issues surrounding such training that we discuss in this article.
Defining concepts
Culture
Culture is not a value-free concept and it is defined in many ways, as are other widely used terms such as ethnicity and race (Reference BradbyBradby, 2003). One cannot dispute that the concept of culture, cultural identity or belonging to a cultural group involves a degree of active engagement by individuals and is a dynamic process. It is problematic to assign cultural categories externally and based only on certain characteristics. It must be recognised that individuals make sense of themselves in relation to the cultural groups with which they themselves identify or are externally identified in various ways. Membership of such groups is not always voluntary. How much an individual chooses to identify with a group to which he or she is assigned varies from person to person. Concepts of culture and understanding cultural groups imply understanding of the hierarchies and rules of conduct of those groups.
The concept of identity is closely related to the idea of culture. Identities can be formed through the cultures and subcultures to which people belong or in which they participate. Reference Frosh, Bullock and TrombleyFrosh (1999: p. 413) described the view that identity draws from culture but is not simply formed by it. Given that the focus of our article is cultural diversity in the context of delivering psychiatric services, the definition of culture that we use is consistent with that adopted by the Association of American Medical Colleges (AAMC):
‘Culture is defined by each person in relationship to the group or groups with whom he or she identifies. An individual’s cultural identity may be based on heritage as well as individual circumstances and personal choice. Cultural identity may be affected by such factors as race, ethnicity, age, language, country of origin, acculturation, sexual orientation, gender, socioeconomic status, religious/spiritual beliefs, physical abilities, occupation, among others. These factors may impact behaviours such as communication styles, diet preferences, health beliefs, family roles, lifestyle, rituals and decision-making processes. All of these beliefs and practices, in turn can influence how patients and heath care professionals perceive health and illness and how they interact with one another’ (Task Force on Spirituality, Cultural Issues, and End of Life Care, 1999: p. 25).
This is a patient-centred definition that can be applied to clinical situations. It suggests that individuals draw on a range of resources and, through the interplay of external and internal meanings, construct a sense of identity and unique culture. Patients will themselves define which aspect of their cultural belonging is relevant at any particular time. This may change in different clinical contexts and at different stages of an individual’s life, and may also depend on the clinical presentation itself. This is not to underplay the complexity of the term, but to use it in a way that it is suitable in the context of healthcare delivery. The academic debate about the meaning of culture is less relevant here than the interplay between culture and identity, which involves the individual’s perception. The latter is more relevant in clinical contexts.
Diversity
Although various definitions of culture are offered, less has been written about diversity. One might think that diversity should be a more straightforward term. However, again the word is used imprecisely. In some cases, it means diversity of ethnicity, which is often called ‘multiculturalism’ (e.g. Reference Culhane-Pera, Reif and EgliCulhane-Pera et al, 1997; Reference Loudon, Ross and GillLoudon et al, 2001). There is also a perspective that diversity covers the range of groups within society and thus includes groups identified by characteristics other than ethnicity, such as sexual orientation. In other cases, it covers a much broader range of difference, relating to individual characteristics beyond ethnicity. Policies relating to equality within institutions suggest that diversity and acceptance refer to the diversity of individuals (Gallant 2000 Ltd, 2003).
In this article, diversity includes not only race, ethnicity and gender but also ability/disability, education, class and many other differences.
Cultural competence
In the North American medical system, many educational programmes have endeavoured to teach ‘cultural competence’ as a way of understanding culture. A widely used definition of this states:
‘The model called “cultural competence” … involves systems, agencies and practitioners with the capacity to respond to the unique needs of populations whose cultures are different than that which might be called “dominant” or “mainstream” American. The word culture is used because it implies the integrated pattern of human behaviour that includes communications, actions, customs, beliefs, values and institutions of a racial, ethnic, religious or social group. The word competence is used because it implies having the capacity to function in a particular way: the capacity to function within the context of culturally integrated patterns of human behaviour as defined by the group. While this publication focuses on ethnic minorities of colour, the terminology and thinking behind this model applies to each person – everyone has or is part of a culture’ (Reference Cross, Bazron and DennisCross et al, 1989: p. 3).
Although this definition does not emphasise working towards services that are sensitive to an individual patient’s needs, it does highlight the needs of groups, which may or may not be as homogeneous as is implied.
Cultural competence is a widely used term and it has many other meanings (Reference HenryHenry J. Kaiser Family Foundation, 2003).
Race and ethnicity
There is similar inconsistency in definitions of race and ethnicity (Reference BradbyBradby, 2003). For example, in the USA ‘race’ is still perceived more as a biological characteristic, whereas in the UK there is greater acceptance that it is a social construct (Reference Dogra and KarnikDogra & Karnik, 2004).
How does diversity relate to healthcare delivery?
Although many psychiatrists readily accept that diversity influences use of healthcare services and health outcomes, there is evidence that some regard psychosocial factors as too ‘touchy–feely’ (Reference ToynbeeToynbee, 2002; Reference RivettRivett, 2003). However, there is evidence to suggest that the patients of clinicians who respect different patient perspectives have improved healthcare outcomes, feeling better understood, respected and valued as partners in their own care (Reference Secker and HardingSecker & Harding, 2002).
Reference Levinson, Roter and MulloolyLevinson et al (1997) offered several reasons to justify the teaching of cultural diversity to medical students. They argued that dealing effectively with diversity should improve doctor–patient communication. This can be generalised to postgraduate contexts: if diversity training does make a difference to healthcare outcomes, training should be undertaken throughout a doctor’s career. Evidence shows that good communication skills diminish the risk of malpractice: the doctor is better able to identify the patient’s problems, which reduces misdiagnoses and misunderstandings. Appreciation of cultural diversity should also increase patients’ adherence to treatment regimens and improve outcomes, including patient satisfaction.
DiversityRx is an American clearing house of information on ways to meet the language and cultural needs of minorities, immigrants, refugees and other diverse populations seeking healthcare. In an overview of cultural competence in medical training and practice, they reported that lack of awareness about cultural differences makes it difficult for both providers and patients to achieve the best, most appropriate care. Figure 1 shows some of the problems that may arise where clinicians are culturally incompetent or unaware (DiversityRx, 2001a ).

Fig. 1 Possible repercussions of healthcare providers’ lack of awareness of cultural differences (DiversityRx, 2001a).
The National Institute for Mental Health in England (NIMHE) (2003) has highlighted the possibility that people from Black and minority ethnic groups experience inadequate healthcare provision. Reference WilliamsWilliams (1997) argued that, when culture is overlooked, incorrect and even harmful decisions may be made. Furthermore, the healthcare provider’s ability to engage individuals and families and build on strengths may be limited. DiversityRx (2001b ) stated that providers may need to ask themselves how they react when confronted with a new situation that does not fit their expectations and whether it provokes feelings of anxiety and discomfort. They also suggested that clinicians consider what is going on within themselves and within their patients. They should ask themselves whether they have useful strategies for clarifying puzzling situations and improving their own and their patients’ understanding.
Tirado & Thom found no statistically significant impact of training on physicians’ cultural competence, on healthcare processes or outcomes of care (M. Tirado, personal communication, 2004). However, they did find that culturally competent physicians had a positive impact on the care of patients with hypertension and/or diabetes.
Diversity training for psychiatrists
Until recently there has been no framework within which training in diversity has been formally considered for psychiatrists or other healthcare professionals. There has been a tendency to assume that diversity, especially diversity related to ethnicity, inherently leads patients to have different beliefs about mental health and that this should be the focus of exploration (e.g. Reference Bhui and BhugraBhui & Bhugra, 2004). Although this may be valuable, it may not reveal the whole picture. Variability within groups is either not recognised or minimised.
First moves towards a national training programme were published in Inside Outside (National Institute for Mental Health in England, 2003: p. 31), which advocated mandatory training in cultural competencies for all professional staff working in mental health. In the same year, an inquiry into the death of a Black man, David ‘Rocky’ Bennett, in a psychiatric hospital (Department of Health, 2003) recommended that training the 40 000-strong existing mental health workforce in cultural competence should become a priority. In 2004, the NIMHE and the Sainsbury Centre for Mental Health published a document laying down the most important areas in which all staff in mental health services should be trained (‘the ten essential shared capabilities’; Reference HopeHope, 2004). One of these is respecting diversity, which is decribed as :
‘working in partnership with service users, carers, families and colleagues to provide care and interventions that not only make a positive difference but also do so in ways that respect and value diversity including age, race, culture, disability, gender, spirituality and sexuality’ (Reference HopeHope, 2004: p. 3).
Hope makes specific mention of the discrimination known to exist in many services, pointing out that issues of race and culture require particular attention. Among other things, respect for diversity requires practitioners to understand and acknowledge diversity and to understand the impact of discrimination and prejudice on mental health and mental health services (Reference HopeHope, 2004: p. 14). Although these are commendable recommendations and evidence-based practice is touched upon, little more is said on the value of such education.
With a clarity often lacking in other documents, the Sainsbury Centre for Mental Health (2002) reviewed the relationship between mental health services and African and Caribbean communities. In a discussion of the usage of terms and their potential impact on training, the review pointed to the effect of the confusion that exists in healthcare arenas regarding ‘cultural diversity’, in particular definitions that rely on group-based distinctions. It noted that political rather than educational agendas have often influenced educational programmes. The centrality of issues of ‘race’ and ‘culture’ for mental health services should not be underestimated but nor should they be used to reinforce stereotypical views about minority ethnic communities. In some circumstances, the report noted, it is evident that the term ‘culture’ is used in a similar way to ‘race’, to denote immutable and fixed physical attributes and/or behaviours. Elsewhere, the term seems to denote a set of shared beliefs or a system of kinship. In the context of mental health this approach is problematic, as an individual’s culture needs to be understood for that individual, rather than extrapolated from given generalities. The review felt that this is particularly important, as many ‘cultural awareness’ courses define or predict the characteristics of certain ethnic groups, along with standard responses by professional workers, by means of overarching generalisations.
Current training and issues raised
When considering the need for an evidence-based approach to medical education, it is clear that evaluation of new programmes needs attention. Many programmes are available, as an internet search will reveal. However, very few claiming to teach cultural diversity have been subject to evaluation beyond subjective student feedback. The exceptions are studies with undergraduates by Reference Mao, Bullock and HarwayMao et al(1988), Reference CopemanCopeman (1989), Reference Rubenstein, Bonnie and O'ConnorRubenstein et al(1992), and Reference DograDogra (2001) and with postgraduates by Reference Culhane-Pera, Reif and EgliCulhane-Pera et al(1997) and Reference Majumdar, Keystone and CuttressMajumdar et al(1999). All used pre- and post-teaching questionnaires and reported some degree of ‘positive’ change in student perspectives, but there was little follow-up. Only one of these studies was conducted in the UK (Reference DograDogra, 2001). This might suggest that, although medical organisations claim to run programmes on cultural diversity, there is little follow-up to ensure that these make any difference. Furthermore, the content of programmes is often variable. Some focus on knowledge acquisition (e.g. Reference Deloney, Graham and ErwinDeloney et al, 2000), some on skills (e.g. Reference Majumdar, Keystone and CuttressMajumdar et al, 1999) and some on attitudes (e.g. Reference Sifri, Glaser and WittSifri et al, 2001). Many attempt to address all three aspects, although their focus varies (e.g. Reference Culhane-Pera, Reif and EgliCulhane-Pera et al, 1997; Reference DograDogra, 2001). There is evidence (Reference Dogra, Conning and GillDogra et al, 2005) that, although many UK medical schools now address this issue at undergraduate level, teaching is fragmented and there is a great deal of uncertainty as to what diversity education actually is.
Some study results
Reference Webb and SergisonWebb & Sergison (2003) reported that child healthcare professionals found their race awareness training useful. In a follow-up study, staff commented on how they thought their own behaviour had changed. For example, some used more culturally appropriate pictures in wards and stopped using minors as interpreters. However, there were no objective measures of change.
A systematic review of five interventions to improve cultural competence in healthcare systems that included cultural competency training for healthcare providers was undertaken by Reference Anderson, Scrimshaw and FulliloveAnderson et al(2003). They judged that only one study had a fair quality of execution and therefore concluded that the evidence was insufficient.
The findings of Tirado & Thom (M. Tirado, personal communication, 2004) suggest that cultural competency is important in healthcare but as yet we have not clarified how physicians can be effectively trained to become culturally competent and how policy relating to this issue can best be framed for medical organisations.
Political correctness
In a report mentioned earlier, the Sainsbury Centre for Mental Health (2002) commented on staff concerns that issues of race and culture cannot be freely discussed, implicitly blaming ‘political correctness’. The report acknowledges that attempts to address racism and sexism have at times focused on the ridiculous. ‘Political correctness’ can also be viewed as a tool used by the American political right to discredit the whole process of tackling disparities. Any initiative against racism or sexism is likely to be met with the charge of political correctness by those opposed to changes, and it is necessary to achieve a rational balance between outlandish prohibitions on behaviour or language (e.g. black coffee) and reasonable criticism of racism.
The findings of the Sainsbury Centre’s report have been borne out in our own discussions with colleagues about their training experiences. Training is often enforced so that organisations can claim they are complying with legislation, but there is a feeling that there is little commitment to actually changing practice or systems.
Changing how we think
Several issues need consideration if there is a serious intention to review whether or not training in diversity influences healthcare outcomes and how psychiatrists can be trained to provide care appropriate to a patient’s culture. In the remainder of this section we consider just some of these.
How patients are viewed
First, we need to ask whether information about specific groups is helpful or not. Reference KellyKelly (2003) highlighted studies that have shown higher prevalence of particular disorders in particular groups, but there is no evidence to show that having such information influences healthcare outcomes for better or worse. Indeed, the information may do more to reinforce stereotypes than challenge practitioners to question their own biases in decision-making processes. While public healthcare may be about services to groups of the population, clinical care is about service provision to individuals. We must consider how we tailor public services to individuals’ needs. This seems to be a fundamental and yet unresolved issue.
If we consider diversity among patients and use the Association of American Medical College’s definition (Task Force on Spirituality, Cultural Issues, and End of Life Care, 1999), the focus is on individuals not groups. Ethnicity is only one component of how someone might choose to define him- or herself. We need to consider for whose benefit we provide general information about groups with which patients may or may not identify themselves. Individuals should be able to choose how they define themselves, rather than have services define them on the basis of their skin colour or any other characteristic. Publications such as Addressing Black and Minority Ethnic Health in London (Department of Health, 1999) imply that the needs of individuals are primarily based on their skin colour. In general, Black people and people from minority ethnic groups are treated as a single homogeneous population. This approach makes assumptions that the experiences of all such individuals are the same and that their skin colour overrides other facets of their individuality. Talking about groups of people reduces patients to lists by which their needs are decided, as opposed to asking them as individuals what their views are. Managing diverse patients should mean trying to improve access and services for all potential users, not just for those from specific groups. It should also be recognised that equitable care does not mean the same care, as individual needs will be different.
Educational models for teaching cultural diversity
There is criticism that education and training in cultural diversity have largely been driven by government policy and not educational needs or an evidence base (Reference DograDogra, 2004b ). Nevertheless, the concept of cultural competence discussed earlier has provided an important background to developments in the UK. It might be argued that there are two different models for teaching cultural competence. One is based on a notion of expertise and the other on a notion of sensibility (Reference DograDogra, 2004a ).
Cultural expertise
An expert may be described as having special skill at a task or knowledge in a subject, so that expertise is the skill or knowledge that the expert possesses (Reference ThompsonThompson, 1995). The notion that, through gaining knowledge about ‘other’ cultures, someone can develop ‘cultural expertise’ has given rise to educational programmes trying to impart cultural competence, to create ‘cultural experts’.
Cultural sensibility
‘Cultural sensibility’ should not be confused with the more common term ‘cultural sensitivity’. In general usage, sensibility (openness to emotional impressions, susceptibility and sensitiveness; Reference ThompsonThompson, 1995) relates to a person’s moral, emotional or aesthetic ideas or standards. Thus, cultural sensibility is interactional: if one is open to outside experience, one might reflect and change because of that experience. This is not necessarily the case with cultural sensitivity, which is more the quality or degree of being aware of cultural issues and is closer in meaning to cultural expertise. In cultural sensibility, there is no notion of acquiring expertise about others; rather, there is a recognition that we need to be aware of our own perspectives and how they affect our ability to view the perspectives of others with an open mind.
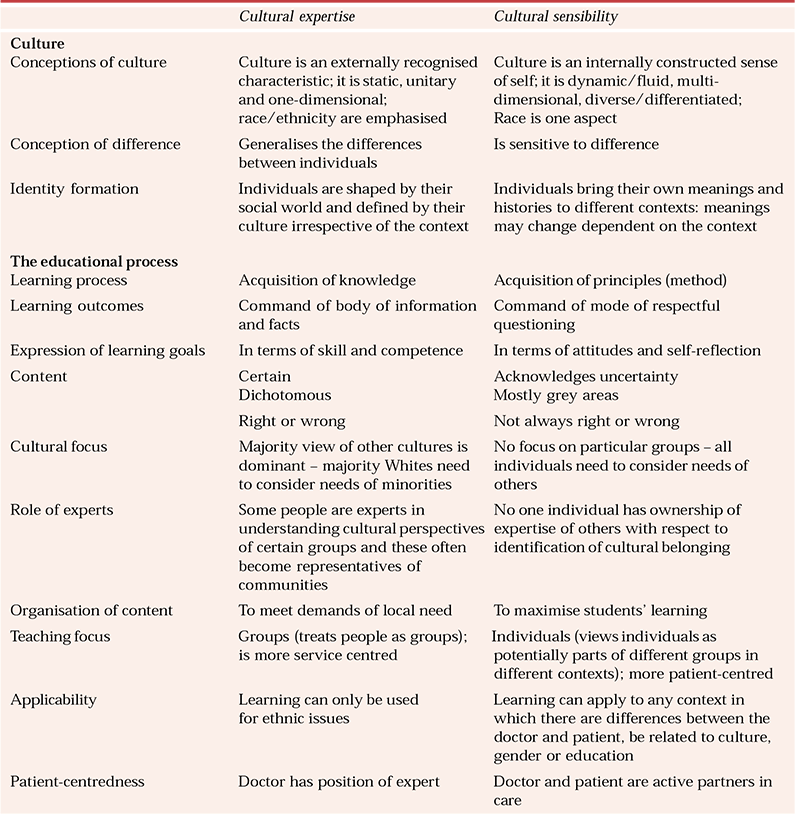
Table 1 shows how the two models view culture and some aspects of the educational process involved in a teaching model based on a notion of cultural sensibility (Reference DograDogra, 2004a ).
Table 1 Conceptions of culture and the educational process (Reference DograDogra, 2004a )
| Cultural expertise | Cultural sensibility | |
|---|---|---|
| Culture | ||
| Conceptions of culture | Culture is an externally recognised characteristic; it is static, unitary and one-dimensional; race/ethnicity are emphasised | Culture is an internally constructed sense of self; it is dynamic/fluid, multi-dimensional, diverse/differentiated; Race is one aspect |
| Conception of difference | Generalises the differences between individuals | Is sensitive to difference |
| Identity formation | Individuals are shaped by their social world and defined by their culture irrespective of the context | Individuals bring their own meanings and histories to different contexts: meanings may change dependent on the context |
| The educational process | ||
| Learning process | Acquisition of knowledge | Acquisition of principles (method) |
| Learning outcomes | Command of body of information and facts | Command of mode of respectful questioning |
| Expression of learning goals | In terms of skill and competence | In terms of attitudes and self-reflection |
| Content | Certain Dichotomous |
Acknowledges uncertainty Mostly grey areas |
| Right or wrong | Not always right or wrong | |
| Cultural focus | Majority view of other cultures is dominant – majority Whites need to consider needs of minorities | No focus on particular groups – all individuals need to consider needs of others |
| Role of experts | Some people are experts in understanding cultural perspectives of certain groups and these often become representatives of communities | No one individual has ownership of expertise of others with respect to identification of cultural belonging |
| Organisation of content | To meet demands of local need | To maximise students’ learning |
| Teaching focus | Groups (treats people as groups); is more service centred | Individuals (views individuals as potentially parts of different groups in different contexts); more patient-centred |
| Applicability | Learning can only be used for ethnic issues | Learning can apply to any context in which there are differences between the doctor and patient, be related to culture, gender or education |
| Patient-centredness | Doctor has position of expert | Doctor and patient are active partners in care |
In both teaching and clincial practice too much emphasis on practical issues such as language and use of interpreters may mean that practitioners avoid dealing with difficult personal issues such as questioning their own vulnerabilities, fears, ignorance or prejudices. Very few organisations or individuals set out to plan lower-quality services but we need to think about why some patients still fail to receive the care that they need or value.
Service models
Service models influence the training that is delivered and help to establish who is held responsible for delivering equitable services to all. Some organisations delegate this responsibility to a named individual such as a diversity officer, which appears to absolve everyone else of the need to feel responsible. Legally in the UK it is everyone’s responsibility.
In response to a debate about specific services for minority ethnic groups (Reference Bhui and SashidharanBhui & Sashidharan, 2003), Reference Whitley, Kirmayer and JarvisWhitley et al (2004) raised the issue that the diversity of Canadian society is not captured by the broad ethno-racial categories commonly used in the UK and USA; thus, specialised clinics for each minority group are not feasible in Canada. Provision of ethnic-specific services in that country is not pursued for practical rather than philosophical reasons.
Reference Robertson, Sathyamoorthy and FordRobertson et al (2000) found that most of the Black services users they interviewed in a UK study did not want an ethnically specific service, but one that all users could access and benefit from. In another UK study, Reference Secker and HardingSecker & Harding (2002) reported that service users valued the ability of staff to engage with them and see the world from their perspective and that this was not dependent on ethnic matching.
Reference BhuiBhui (2004) has suggested that the integrationist solution has failed to ensure that generic mental health services are culturally capable or appropriate. However, until there is greater debate about this, training will flounder as there is no consensus on what it is trying to achieve. There is also a danger in assuming that individuals who share the same ethnicity have the same views on issues relating to mental health.
Policies regarding training in cultural diversity
As already mentioned, there is strong evidence that political imperatives rather than educational need or purpose have driven diversity training thus far (Reference DograDogra, 2004b ).
It is now essential that policy has an educational priority and that training programmes are developed on a sound evidence base, undergo effective evaluation and have clearly measurable outcomes. (A current educational fashion is ‘reflective learning’, but there is often little thought given to how this might be measured.) Some of the issues relating to policies regarding diversity training are highlighted in Box 1.
Box 1 Policies relating to diversity training
-
• Training needs to be educationally led using an evidence base where possible
-
• Policies should be transparent and clear regarding their philosophical stance
-
• Diversity has to be an integral part of all aspects of service delivery and diversity training should improve care for all patients
-
• Policy must be implemented in a meaningful way that improves outcomes
-
• There is an urgent need to develop outcome measures that can demonstrate that diversity training affects outcomes in mental health
Educational bodies may need to take the lead in directing policies in the healthcare sector.
In 2001 the Royal College of Psychiatrists held a 2-day workshop to discuss the training required to produce culturally capable psychiatrists. An article arising from this workshop, describing the knowledge skills and attitudes of a well-trained and culturally competent psychiatrist, has been published by Parimala Moodley, then chair of the College’s Transcultural Special Interest Group (Reference MoodleyMoodley, 2002). Transcultural psychiatry is now included in the revised curriculum for basic specialist training and the MRCPsych examination (Royal College of Psychiatrists, 2001: p. 71).
The Sainsbury Centre for Mental Health is attempting to establish an evidence base for diversity training, and it is to be hoped that this will inform future policy. There is also a need to direct teaching away from a superficial checklist approach to medical training and to ensure that it delivers healthcare professionals who are able to meet the needs of individual patients and their families. Policies might also be more explicit in indicating that the concept of equality applies to everyone and not just to certain minority groups. This does not, of course, minimise the need to address the issue of racial equality, which has already been highlighted as a priority.
How can practitioners make a difference?
There is no doubt that organisations need to take responsibility for ensuring they put systems in place that urgently address diversity. However, individual practitioners need to take personal responsibility for their delivery of care. Box 2 highlights some questions that practitioners might ask themselves in order to reflect on their practice. We are not suggesting that current practitioners are not thinking about their patients; rather we are reminding everyone that external pressures and our own vulnerabilities affect the care we deliver.
Box 2 Reflecting on your practice
-
• Think about how you view culture and sense of identity given the frameworks presented
-
• Justify your position in the context of your professional role
-
• Reflect on your own practice and evaluate how your own views influence the choices you offer your patients
-
• How often are you genuinely interested in asking individual patients what they might need?
-
• How often do you assume that the needs of patients are already known on the basis of their diagnosis, ethnicity, gender or any other factor?
-
• What three things could you do to change your own practice?
Conclusions
There is a need to investigate the steps to be taken to raise the credibility of cultural diversity as a subject within the profession as a whole and to demonstrate the value of diversity training. This is an area in which the links between undergraduate and postgraduate education could be explored to improve the continuity of medical education. Although there appears to be some consistency between educational models, it is not possible to state which model effectively provides the desired outcomes. Implementing and comparing the outcomes of different models of delivering cultural diversity teaching may also help provide the educational clarity that is needed. Different models might meet different learning objectives and it would be helpful for teachers to know this when they are devising educational programmes. Effective instruments for evaluating the outcomes of cultural diversity teaching are urgently needed. It might be possible to derive them from research in other areas, although measuring changes in attitudes and ways of thinking is fraught with difficulties. However, this should not mean that the problem is avoided.
It is now time to implement and evaluate different educational approaches, so that cultural diversity teaching develops rigour and an evidence base. Unless this is done, it will continue to be a path laid with good intentions but one that ultimately fails to educate healthcare providers to meet patients’ individual needs irrespective of their background or sense of identity.
MCQs
-
1 Culture:
-
a is a clearly defined term
-
b has many different definitions
-
c is interchangeable with ethnicity
-
d and identity are linked
-
e is often externally attributed.
-
-
2 Diversity factors:
-
a have been shown to influence healthcare outcomes
-
b are widely accepted as relevant when considering healthcare provision
-
c relate only to race and ethnicity
-
d may be more relevant in some contexts than others
-
e vary from individual to individual.
-
-
3 In the context of clinical care, diversity factors:
-
a may affect doctor–patient communication
-
b are relevant only when the doctor and patient are of differing ethnicities
-
c may not be explored because of time pressures
-
d may challenge doctors about their own prejudices
-
e may be relevant in compliance.
-
-
4 Training in diversity has:
-
a been shown to be effective in changing practice
-
b developed within clear educational frameworks
-
c focused largely on predicting the characteristics of ethnic groups
-
d often had unclear learning outcomes
-
e become a recent priority.
-
-
5 In considering diversity training there is a need to:
-
a consider how patients are viewed
-
b establish clearer educational models
-
c establish whether different service models need different types of training
-
d evaluate training more effectively
-
e encourage practitioners to reflect on their own practice.
-
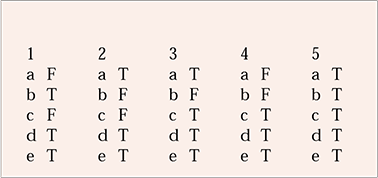
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | F | a | T |
| b | T | b | F | b | F | b | F | b | T |
| c | F | c | F | c | T | c | T | c | T |
| d | T | d | T | d | T | d | T | d | T |
| e | T | e | T | e | T | e | T | e | T |







eLetters
No eLetters have been published for this article.