‘… coffee sets the blood in motion and stimulates the muscles; it accelerates the digestive processes, chases away sleep, and gives us the capacity to engage a little longer in the exercise of our intellects.’
Honoré de Balzac (paraphrasing Brillat-Savarin)
Traité des Excitants Modernes(1838), (translated from the French by Robert Onopa)
Caffeine is the most widely used psychoactive drug in the world. It is found in more than 60 known species of plants, and dietary sources include coffee, tea, cocoa beverages, chocolate and soft drinks. Coffee was consumed in Arabia in the 13th century and was introduced into Europe in the early 17th century. Tea was probably drunk in China before the birth of Christ and was brought to Europe in the 16th century. Most dietary caffeine is still consumed as tea and coffee, and the latter accounts for 55% of per capita intake in the UK (Reference Scott, Chakraborty and MarksScott et al, 1989). Despite (or perhaps because of) its ubiquity, caffeine is rarely thought of as a problematic drug. Doctors do not often ask patients about its use and enquiry into caffeine consumption is not usually included in psychiatric assessment.
On average, a cup of brewed coffee contains 100 mg of caffeine, compared with 75 mg for instant coffee and 50 mg for tea (Food Standards Agency, 2001); a can of Coca Cola contains 30 mg. Increasingly, stimulant drinks such as Red Bull (80 mg of caffeine per can) are being marketed to the public, and sales have increased dramatically since they first became available in 1987 (Reference FinneganFinnegan, 2003). Pharmaceutical caffeine may be bought over the counter (for example as ProPlus tablets) and is also contained in numerous proprietary analgesics, cold and ’flu remedies, diet pills and diuretics; Anadin Extra, for example, contains 90 mg of caffeine per dose. In the UK, mean caffeine consumption is estimated at 359 mg/day (Reference Scott, Chakraborty and MarksScott et al, 1989).
Effects and diagnostic classification
The primary effect of caffeine is to relieve fatigue and enhance mental performance. Excessive ingestion leads to a state of intoxication known as caffeinism, which is characterised by restlessness, agitation, excitement, rambling thought and speech, and insomnia. These symptoms clearly overlap with those of many psychiatric disorders. The potential harmful effects of caffeine have long been recognised. As long ago as 1900, the Journal of the American Medical Association reported a conference on ‘Coffee as a beverage: its deleterious effects on the nervous system’, at which a contributor complained that ‘most physicians had given the subject little if any attention’. Another contributor asserted that coffee could cause a variety of symptoms, including depression, irritability, insomnia, tremulousness, loss of appetite and ‘frequent eructations of gas’ (JAMA, 2001).
Four caffeine-related syndromes are recognised in DSM–IV (American Psychiatric Association, 1994): caffeine intoxication; caffeine-induced anxiety disorder; caffeine-induced sleep disorder; and caffeine-related disorder not otherwise specified. Caffeine withdrawal is included in the Appendix to DSM–IV under ‘Criteria sets and axes provided for further study’. The ICD–10 (World Health Organization, 1992) is less specific. It recognises ‘Mental and behavioural disorders due to use of other stimulants, including caffeine’ (F15), which are then sub-classified in the same way as other substance use disorders (acute intoxication, harmful use, dependence syndrome, withdrawal state, etc.). However, there is no specific guidance on diagnosing problems due to caffeine misuse, and the diagnostic criteria are the same as for other substance use disorders. The prevalence of the various caffeine-related syndromes is uncertain.
Despite this formal recognition, caffeine generally receives little attention from psychiatrists. For example, the New Oxford Textbook of Psychiatry (Reference Gelder, Lopez-Ibor and AndreasenGelder et al, 2003) does not discuss caffeine misuse, although caffeine is mentioned briefly as a cause of insomnia. Consequently, psychiatrists rarely enquire about caffeine intake when assessing patients. This may lead to a failure to identify caffeine-related problems and offer appropriate interventions.
This article describes the clinical effects of caffeine consumption in a variety of psychiatric disorders and offers some guidance on assessing and managing caffeine-related problems.
Biochemistry and pharmacology of caffeine
Caffeine is a methylxanthine (1,3,7-trimethylxanthine). The effects of this group of chemicals include stimulation of the central nervous system (CNS), diuresis, stimulation of cardiac muscle and relaxation of smooth muscle. Caffeine initially stimulates the CNS at the level of the cerebral cortex and medulla and only later stimulates the spinal cord (at higher doses). Its effects begin within 1 h and last for 3–4 h (Reference Baker and TheologusBaker & Theologus, 1972). Caffeine is rapidly absorbed from the gastrointestinal tract and then metabolised by demethylation and oxidation in the liver. There is some individual variation in the rate of metabolism; the half-life is reduced in smokers but increased in pregnancy and in women taking oral contraceptives (Reference FinneganFinnegan, 2003).
Biochemically, the main action of caffeine is anatagonism of adenosine A1 and A2 receptors. Higher doses cause inhibition of phosphodiesterases, blockade of γ-aminobutyric acid type A (GABAA) receptors and release of intracellular calcium (Reference Daly and FredholmDaly & Fredholm, 1998; Reference FinneganFinnegan, 2003). Neuropsychiatric effects are mediated largely by blockade of A1 and A2A receptors in the CNS. Adenosine A1 receptors are present in almost all brain areas, but particularly in the hippocampus, cerebral cortex, cerebellar cortex and thalamus.
There are important connections between adenosine receptors and the dopaminergic system, which may be relevant to the effects of caffeine in psychosis (see below, in the subsection ‘Schizophrenia’). Adenosine A2A receptors are concentrated in the dopamine-rich regions of the brain and are thought to have considerable links with dopaminergic receptors (Reference Ferre, Fuxe and von EulerFerre et al, 1992; Reference Lorist and TopsLorist & Tops, 2003). Moreover, there is evidence that the stimulatory effects of caffeine require intact dopaminergic neurotransmission (Reference Ferre, Fuxe and von EulerFerre et al, 1992). These stimulatory effects appear to result primarily from blockade of A2A receptors, which stimulate inhibitory GABAergic neurons in pathways to the dopaminergic reward system of the striatum (Reference Daly and FredholmDaly & Fredholm, 1998). Blockade of adenosine receptors also reverses the inhibition of adrenaline release in the sympathetic nervous system and results in sympathetic stimulation (Reference KrugerKruger, 1996).
Elsewhere in the body, caffeine causes relaxation of smooth muscle (especially bronchial smooth muscle) and stimulation of cardiac muscle; these effects resemble those of β-adrenoceptor stimulation. The stimulatory effect on the heart can result in tachycardia at high doses.
Psychological effects
The psychological effects of caffeine are biphasic. Low doses produce stimulation, which is often perceived as desirable, whereas high doses can cause the unpleasant effects of caffeinism (Reference Daly and FredholmDaly & Fredholm, 1998). Caffeine increases alertness, reduces fatigue and can elevate mood (Leinart & Huber, 1966; Reference Rogers and DernoncourtRogers & Dernoncourt, 1997; Reference SmithSmith, 2002). Normal consumption improves performance on tasks that require alertness, such as simulated driving tasks (Reference SmithSmith, 2002). The effect on more complex cognitive tasks is less clear, although there is evidence to suggest that high consumption is associated with better performance, especially in older people (Reference SmithSmith, 2002).
Adverse effects
Caffeine has a number of adverse effects on the gastrointestinal tract. It relaxes the lower oesophageal sphincter and can predispose to gastro-oesophageal reflux disease. It also causes gastric hypersecretion, which is associated with susceptibility to ulceration. It increases the rate of gastric emptying and the acidic gastric contents therefore pass more rapidly into the duodenum; this can lead to inflammation of the duodenal mucosa (Reference Boekema, Samson and van Berge HenegouwenBoekema et al, 1999).
The diuretic action of caffeine is well known. The public is often advised to abstain from consuming caffeine in situations where dehydration may be significant, such as long-haul flights. A recent review (Reference Maughan and GriffinMaughan & Griffin, 2003) concluded that single doses of caffeine such as those found in commonly consumed beverages have little or no diuretic action, although large doses (>250 mg) do.
Caffeine may precipitate sinus tachycardia but does not increase the risk of cardiac arrhythmias, except perhaps at very high dose (Reference Katan and SchoutenKatan & Schouten, 2005). It can trigger migraine in susceptible individuals (Reference Goadsby, Warrell, Cox and FirthGoadsby, 2003). Excessive use of caffeine-containing analgesics has been linked to analgesic nephropathy (Reference De Broe, D'Haese, Elseviers, Warrell, Cox and FirthDe Broe et al, 2003). Caffeine may also be harmful in pregnancy; intakes above 300 mg/day may be associated with low birth weight and miscarriage (Food Standards Agency, 2001; Reference Parazzini, Chiaffarino and ChatenoudParazzini et al, 2005). The UK Food Standards Agency has recommended that pregnant women should limit their intake to less than this amount, which is equivalent to four average-sized cups or three average-sized mugs of instant coffee or six average-sized cups of tea (Food Standards Agency, 2001).
Dependence and withdrawal
Caffeine acts as a reinforcing agent in both humans and animals (Griffiths & Munford, 1995), although its effect is less powerful than that of stimulants such as cocaine and amphetamine (Reference Daly and FredholmDaly & Fredholm, 1998). The reinforcing effect is thought to be due to both pleasurable stimulatory effects and unpleasant withdrawal symptoms (Reference Daly and FredholmDaly & Fredholm, 1998). Caffeine differs from classical drugs of misuse in causing dopamine release in the prefrontal cortex rather than the nucleus accumbens, which is the principal area involved in reward and addiction (Reference NehligNehlig, 1999).
Withdrawal symptoms have been reported in both humans and animals (Reference Schuh and GriffithsSchuh & Griffiths, 1997; Reference Griffiths and WoodsonGriffiths & Woodson, 1998). Well-recognised symptoms include headache, irritability, sleeplessness, confusion, nausea, anxiety, restlessness and tremor, palpitations and raised blood pressure (Reference FinneganFinnegan, 2003). They typically start slowly, are at their worst at 1–2 days, and recede within a few days. They are rapidly relieved by intake of caffeine, suggesting that they are genuine withdrawal symptoms. Tolerance has been reported to the effects of caffeine on the respiratory and cardiovascular systems, but there is little tolerance to its effect on sleep or mood (Reference Daly and FredholmDaly & Fredholm, 1998).
Data on the prevalence of withdrawal symptoms are inconsistent, with a range of 11% or less to 100% (Reference Dews, O'Brien and BergmanDews et al, 2002). One study found that 7.5% of the population may experience adverse effects following either caffeine consumption or withdrawal (Reference Scott, Chakraborty and MarksScott et al, 1989). In another study (Reference Dews, Curtis and HanfordDews et al, 1999), 11% of caffeine consumers reported withdrawal symptoms. Among regular caffeine users, only 0.9% of males and 5.5% of females reported withdrawal symptoms significant enough to interfere with normal activities. Withdrawal symptoms appear to be more common in teenagers: in one sample, 77.8% reported withdrawal symptoms and 41.7% tolerance (Reference Bernstein, Carroll and ThurasBernstein et al, 2002).
Overall, clinically significant withdrawal symptoms seem to be relatively uncommon in the general population (Reference Dews, Curtis and HanfordDews et al, 1999). It has been suggested that there is a definable caffeine dependence syndrome, on the basis that some adults meet the DSM–IV criteria for substance dependence (Reference Strain, Mumford and SilvermanStrain et al, 1994). However, many studies of caffeine withdrawal have methodological limitations (Reference SmithSmith, 2002) and the status of caffeine as a drug of dependence remains controversial.
Caffeine and psychiatric disorder
Consumption of caffeine may be higher in psychiatric patients than in the population as a whole (Reference Greden, Fontaine and LubetskyGreden et al, 1978; Galliano, cited in Reference Scott, Chakraborty and MarksScott et al, 1989). Caffeine use has been linked with specific disorders such as anxiety disorders, sleep disorders and eating disorders, and there is a possible association with schizophrenia. Surprisingly, there are no published reports linking caffeine use with mania or hypomania.
Anxiety disorders
The resemblance between the symptoms of excessive caffeine ingestion and those of anxiety is obvious and they may both have a basis in overactivity of the sympathetic nervous system. It has been argued that the symptoms of caffeinism are indistinguishable from those of anxiety (Reference GredenGreden, 1974). However, caffeinism is normally associated with a daily intake of 1000–1500 mg, and the relevance of Greden’s observation to lower doses is uncertain (Reference SmithSmith, 2002). There is a substantial literature documenting the anxiogenic effects of caffeine in both experimental and realistic situations (e.g. Reference ChaitChait, 1992; Reference Brice and SmithBrice & Smith, 2002; Reference Botella and ParraBotella & Parra, 2003). The stimulation of anxiety in response to caffeine may be due to increased levels of lactate in the brain (Reference Tancer, Stein and UhdeTancer et al, 1991, Reference Tancer, Stein and Uhde1994). The role of adenosine in mediating caffeine-induced anxiety is supported by the finding that there is an association between different anxiety levels after caffeine administration and polymorphisms on the A2A receptor gene (Reference Alsene, Deckert and SandAlsene et al, 2003).
Clinically, caffeine may be involved in the precipitation, exacerbation or maintenance of anxiety disorders (Reference KrugerKruger, 1996). Sensitivity to caffeine is increased in people with panic disorder and social phobia, and administration of caffeine can provoke panic attacks in these individuals (Reference Charney, Heninger and JatlowCharney et al, 1985; Reference Tancer, Stein and UhdeTancer et al, 1991, Reference Tancer, Stein and Uhde1994). There are clinical reports of anxiety symptoms improving on caffeine withdrawal or limitation (Reference GredenGreden, 1974; Reference Bruce and LaderBruce & Lader, 1989), and people suffering panic attacks may benefit from a reduction in their intake (Reference Charney, Heninger and JatlowCharney et al, 1985).
Sleep disorders
It is well-known that caffeine produces insomnia. It reduces slow-wave sleep in the early part of the sleep cycle and can reduce rapid eye movement (REM) sleep later in the cycle (Reference Nicholson and StoneNicholson & Stone, 1980). Caffeine increases episodes of wakefulness (Reference Brezinova, Oswald and LoudonBrezinova et al, 1975), and high doses in the late evening can increase the time taken to fall asleep (Reference SmithSmith, 2002). In elderly people, the use of medication containing caffeine is associated with an increased risk of difficulty in falling asleep (Reference Brown, Salive and PahorBrown et al, 1995).
Eating disorders
Clinical experience suggests that people with eating disorders such as bulimia nervosa and anorexia nervosa often consume large quantities of drinks containing caffeine, in the belief that caffeine increases metabolic rate and suppresses appetite. In people with anorexia nervosa, who are already at high risk of cardiac arrhthymias, the stimulant effect of caffeine on the heart may be dangerous. Excessive caffeine ingestion may also contribute to osteoporosis, which has a high prevalence in anorexia nervosa (Reference DealDeal, 1997).
Surprisingly, caffeine consumption in people with eating disorders has received little attention in the literature. There is only one published study, carried out in the USA, that focuses on caffeine intake in this population (Reference Krahn, Hasse and RayKrahn et al, 1991). This study of individuals with anorexia nervosa, bulimia nervosa and eating disorder not otherwise specified found that 14.6% had a high caffeine intake (over 750 mg/day), 39.2% had a moderate intake (250–750 mg/day) and 46.3% had a low intake (<250 mg/day). High and moderate intakes were associated with an increased frequency of binge eating, compared with low intake. Those in the high-intake group were also more likely to misuse laxatives and diet pills and have higher levels of anxiety. High and moderate intake were associated with high scores on the Michigan Alcohol Screening Test. We are currently conducting a study of caffeine use in British people with eating disorders.
Schizophrenia
It has already been noted that there are connections between adenosine A2A receptors and the dopaminergic system in the brain. As adenosine inhibits dopaminergic neurotransmission, blockade of A2A receptors by caffeine may increase dopaminergic activity and exacerbate psychotic symptoms (Reference Ferre, Fuxe and von EulerFerre et al, 1992). Clinically, the symptoms of caffeine intoxication can mimic those of psychosis (Reference KrugerKruger, 1996) or be confused with the side-effects of medication (Reference Hughes, McHugh and HoltzmanHughes et al, 1998). Cessation of caffeine causes fatigue and drowsiness, which can be confused with the side-effects of psychotropic drugs (Reference Hughes, McHugh and HoltzmanHughes et al, 1998).
There is also evidence that people with schizophrenia have higher than average intakes of caffeine, although the literature is inconsistent. There are a number of case reports of high caffeine intake among in-patients with schizophrenia (Reference Benson and DavidBenson & David, 1986; Reference Zaslove, Russell and RossZaslove et al, 1991). Studies published in the 1970s give conflicting results, one finding that 71% of in-patients used more than 500 mg of caffeine per day (Reference WinsteadWinstead, 1976) and the other that only 17% used more than this amount (Reference FurlongFurlong, 1975). A more recent study found that the mean daily caffeine intake of 26 in-patients was 503 mg, with 38% using more than 555 mg (Reference Mayo, Falkowski and JonesMayo et al, 1993).
Several theories have been advanced as to why people with schizophrenia might have high intakes of caffeine (Reference Hughes, McHugh and HoltzmanHughes et al, 1998). These include using caffeine to relieve boredom and apathy and to offset the sedating effects of antipsychotic medication. Many psychotropic drugs produce a dry mouth, which might increase the intake of caffeinated drinks. About 80% of people with schizophrenia smoke (Reference Lohr and FlynnLohr & Flynn, 1992) and these individuals may use more caffeine to make up for the increased elimination of caffeine due to heavy smoking (Reference Swanson, Lee and HoppSwanson et al, 1994).
There have been a number of case reports of delusions and hallucinations after large intakes of caffeine by people both with (Reference MikkelsenMikkelsen, 1978; Reference Zaslove, Russell and RossZaslove et al, 1991) and without psychosis (Reference McManamy and SchubeMcManamy & Schube, 1936; Reference Rush, Sullivan and GriffithsRush et al, 1995). One study of 78 people with schizophrenia found that caffeine intake was correlated with positive symptoms but not with negative symptoms (Reference Goff, Henderson and AmicoGoff et al, 1992). Another, small study found only a slight correlation between caffeine intake and severity of psychosis (Reference Hamera, Schneider and DevineyHamera et al, 1995).
Three studies have attempted to determine the effect of caffeine on psychotic symptoms in in-patients by comparing the effect of caffeinated and decaffeinated beverages. All used the Brief Psychiatric Rating Scale (BPRS; self-reported) and the Nurses Observation Scale for Inpatient Evaluation (NOSIE; nurse rated). The first found that scores on the anxiety and hostility sub-scales of the BPRS and irritability scores on the NOSIE were higher when caffeine was being consumed (Reference De Freitas and SchwartzDe Freitas & Schwartz, 1979). The second found that scores for hostility, hallucinations and unusual thought content on the BPRS and for irritability and psychosis on the NOSIE were correlated with caffeine intake (Reference Koczapski, Paredes and KoganKoczapski et al, 1989). However, these changes were small and statistically questionable. The third study found no relationship on either scale between caffeine intake and anxiety, depression or total scores (Reference Mayo, Falkowski and JonesMayo et al, 1993).
In an experimental study, caffeine was administered intravenously to 13 patients with schizophrenia who had been caffeine free for 6 weeks (Reference Lucas, Pickar and KelsoeLucas et al, 1990). The dose used (10 mg/kg of body weight) was the equivalent of drinking seven cups of brewed coffee in a row. Caffeine increased both the total score and the unusual thoughts sub-scale score on the BPRS. Conversely, caffeine decreased withdrawal/retardation. Interestingly, this large dose did not increase anxiety scores. The results of this study are consistent with those of the clinical studies described above, but they need to be interpreted with caution because of the large dose and the lack of a control group of people without schizophrenia (Reference Hughes, McHugh and HoltzmanHughes et al, 1998).
Interaction with antipsychotics
Caffeine has been shown to react in vitro with antipsychotics to form an insoluble precipitate (Reference HirschHirsch, 1979), which could lead to decreased absorption (Reference KrugerKruger, 1996). Evidence also suggests that it may compete with clozapine for metabolism by the cytochrome P450 (CYP) 1A2 isoenzyme and could potentiate the side-effects of clozapine (Reference Odom-White and de LeonOdom-White & de Leon, 1996). This has not been tested experimentally, although a published case report suggests that caffeine can increase clozapine levels sufficiently to produce clinically significant side-effects (Reference Odom-White and de LeonOdom-White & de Leon, 1996). The literature also includes a case report of an individual with schizophrenia who experienced an acute exacerbation of psychotic symptoms when clozapine was combined with caffeinated drinks (Reference Vainer and ChouinardVainer & Chouinard, 1994).
Substance misuse
Caffeine appears to prime reward-relevant dopaminergic circuits implicated in cocaine misuse, and has been found to reinstate extinguished cocaine-taking behaviour in rats (Reference Worley, Valadez and SchenkWorley et al, 1994). It may also influence the intake or actions of alcohol and benzodiazepines (Reference Daly and FredholmDaly & Fredholm, 1998). There is evidence that patients who are addicted to other drugs use more caffeine than general psychiatric patients (Reference Hays, Farabee and MillerHays et al, 1998). Caffeine consumption is often found to be higher in smokers than in non-smokers (Istvan & Matarazzo, 1984; Reference Scott, Chakraborty and MarksScott et al, 1989). This may reflect the increased elimination of caffeine due to heavy smoking, as mentioned above, or a general need for stimulation. On the other hand, one small study found that caffeine use was lower in patients undergoing alcohol detoxification than in the general population (Reference Pristach, Smith and WhitneyPristach et al, 1983).
Children
Caffeine intake is lower in children than in adults, with a mean daily intake of 14–22 mg for children between 1 and 9 years of age in the USA (Reference Knight, Knight and MitchellKnight et al, 2004). Intake is likely to be higher in older children and adolescents, with the majority coming from soft drinks (Reference Valek, Laslavic and LaslavicValek et al, 2004). Excessive consumption of caffeine by children and adolescents has been identified as a cause of headache, which usually resolves on withdrawal (Reference Hering-Hanit and GadothHering-Hanit & Gadoth, 2003). Caffeine is also associated with sleep disturbance, with shorter nocturnal sleep duration, increased wake time after sleep onset and increased daytime sleep (Reference Pollak and BrightPollak & Bright, 2003). It is unclear whether caffeine plays a significant role in behavioural disturbance in children.
Psychiatric in-patients
Among adult psychiatric patients in the USA, a significant number have been found to use large amounts of caffeine (750 mg or more per day); such individuals have higher levels of both anxiety and depression than those who consume less (Reference Greden, Fontaine and LubetskyGreden et al, 1978). Stimulation of the sympathetic nervous system by caffeine puts the body in ‘fight or flight’ mode. In psychiatric in-patients, who can neither fight nor flee, sympathetic arousal will produce excitement and anxiety, which may result in behavioural disturbance (Reference KrugerKruger, 1996).
In a study of long-stay psychiatric in-patients, switching to decaffeinated coffee for 3 weeks led to an improvement in anxiety, irritability and hostility, which was reversed when caffeine was reintroduced; reintroduction of caffeine also caused an increase in psychotic features (Reference De Freitas and SchwartzDe Freitas & Schwartz, 1979).
In institutionalised adults with learning disability, caffeine challenge following a period of abstinence resulted in an increase in disturbed behaviour (Reference SearleSearle, 1994). It has been reported in a naturalistic study that higher doses of phenothiazines are prescribed to in-patients supplied with caffeinated coffee than to those given decaffeinated (Reference Shisslak, Bleutler and ScheiberShisslak et al, 1985). However, a double-blind crossover study found no correlation between caffeine consumption and anxiety, depression or behaviour in long-stay patients with schizophrenia (Reference Mayo, Falkowski and JonesMayo et al, 1993). Caffeine may antagonise the effect of benzodiazepines such as lorazepam and diazepam (Reference File, Bond and ListerFile et al, 1982; Reference Roache and GriffithsRoache & Griffiths, 1987; Reference Kaplan, Tai and GreenblattKaplan et al, 1990; Reference KrugerKruger, 1996); it has been suggested that patients may use caffeine to reverse the effects of sedatives, so creating a vicious cycle (Reference De Freitas and SchwartzDe Freitas & Schwartz, 1979).
Assessment and treatment of caffeine-related problems
In summary, although there is little evidence that caffeine produces clinically significant dependence, it may play a contributory role in a variety of psychiatric disorders. Assessment of caffeine intake should therefore form part of routine psychiatric assessment. This is particularly important in people with anxiety and sleep disorders, eating disorders and substance misuse. Assessment can easily be incorporated into the assessment of alcohol and drug use. In people who misuse drugs or have an eating disorder, it is appropriate to ask about use of over-the-counter products that contain caffeine. Intake should be quantified roughly in terms of the number of cups/mugs of tea or coffee and cans of carbonated drinks consumed in an average day. This can be converted into daily caffeine intake (Box 1). Intake may be classified as low (<250 mg/day), moderate (250–750 mg/day) or high (>750 mg/day).
Box 1 Caffeine content of drinks and chocolate

| • Average cup of instant coffee | 75 mg |
| • Average mug of instant coffee | 100 mg |
| • Average cup of brewed coffee | 100 mg |
| • Average cup of tea | 50 mg |
| • Regular can of cola drink | up to 40 mg |
| • Regular can of energy drink | up to 80 mg |
| • Plain 50 g bar of chocolate | up to 50 mg |
| • Milk 50 g bar of chocolate | up to 25 mg |
| (Data from Food Standards Agency, 2001, with permission) | |
Psychiatrists should always enquire about use of caffeine before prescribing hypnotics. Other situations where caffeine intake may be relevant include poor response to hypnotics, recurrent headaches and palpitations (Reference GredenGreden, 1974). General practitioners, who see large numbers of patients with anxiety and sleep disorders, should also be made aware of the importance of caffeine and encouraged to ask about its use. Those who consume large amounts of caffeine should be given information about is effects and encouraged to reduce their intake.
If overuse of caffeine is established, gradual reduction in intake or gradual substitution with caffeine-free alternatives is probably preferable to abrupt cessation. Decaffeinated coffee and tea are now readily available. Although there have been concerns about potential carcinogenic effects when beverages are decaffeinated chemically, processes that use water and carbon dioxide seem to be safe. Caffeine-free cola is also becoming more available. Those responsible for in-patient psychiatric units should be aware of the potential role of excessive caffeine consumption in exacerbating sleep problems and behavioural disturbance and should encourage patients to reduce their consumption. Decaffeinated beverages should be provided on psychiatric wards.
Box 2 gives useful website addresses for further information on caffeine.
Box 2 Useful web addresses
For the general public
http://www.eatwell.gov.uk/healthydiet/nutritionessentials/drinks/waterandsoftdrinks
For professionals
Health effects:
http://www.jr2.ox.ac.uk/bandolier/band58/b58-4.html
Psychiatric effects:
http://www.emedicine.com/med/topic3115.htm
MCQs
-
1 The effects of caffeine typically last for:
-
a 1–2 h
-
b 3–4 h
-
c 5–6 h
-
d 7–8 h
-
e 9–10 h.
-
-
2 Stimulatory effects of caffeine appear to be due to blockade of:
-
a adenosine A1 receptors
-
b β-adrenoceptors
-
c noradrenaline receptors
-
d dopaminergic receptors
-
e adenosine A2 receptors.
-
-
3 Caffeine has been shown to form an insoluble precipitate with:
-
a antidepressants
-
b benzodiazepines
-
c antipsychotics
-
d mood stabilisers
-
e pain killers.
-
-
4 Caffeinism is associated with doses of:
-
a 100–500 mg
-
b 500–1000 mg
-
c 1000–1500 mg
-
d 1500–2000 mg
-
e 2000–2500 mg.
-
-
5 Caffeine can potentiate the side-effects of:
-
a carbamazepine
-
b clozapine
-
c olanzapine
-
d chlorpromazine
-
e risperidone.
-
MCQ answers
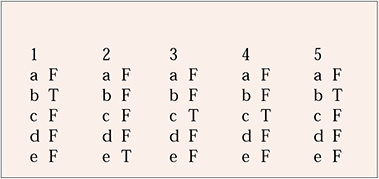
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | F | a | F |
| b | T | b | F | b | F | b | F | b | T |
| c | F | c | F | c | T | c | T | c | F |
| d | F | d | F | d | F | d | F | d | F |
| e | F | e | T | e | F | e | F | e | F |





eLetters
No eLetters have been published for this article.