In 2001, 16% of England’s population was over 65 years of age, and this proportion is forecast to rise to 21% by 2026 (Reference EwingFalaschetti et al, 2002). In 1988, 13% of men aged 65 and over drank more than the weekly guideline of 21 units; the figure had increased to 17% in 2000. The number of women drinking over the recommended guideline (14 units per week) increased from 4% in 1988 to 7% in 2000 (Reference O'Connell, Chin and CunninghamOffice for National Statistics, 2001).
Alcohol use disorders among older people are often described as a hidden problem, which may be due to a number of factors. First, many elderly people do not disclose information about their drinking because they are ashamed. Many are isolated, with minimal social contact or networks, thereby making the problem more difficult to detect. It has also been suggested that older people may significantly under-report their drinking (Reference Miller and RollnickNaik & Jones, 1994). Second, people in the helping professions seem reluctant to ask an older person about drinking, either because it makes them feel awkward or because of the stereotypical image of alcohol use disorders as a problem affecting mostly younger people (Reference Curtis, Geller and StokesDeblinger, 2000). Third, alcohol problems often present in a large number of non-specific ways such as accidents, depression, insomnia, confused states and self-neglect, many of which are linked to the ageing process. Finally, as Reference Koenig, Blazer and BirrenKrach (1998) pointed out, Western societies hold several misconceptions about alcohol use by elderly people, for example that alcoholism is not a significant problem in the elderly population, that it is easy to detect among elderly people and that the amount an elderly person drinks in a single sitting is a good indicator of alcohol misuse.
Patterns of alcohol use
Alcohol use disorder may be described as being of early or late onset. Elderly people who fall into the early-onset category have had a lifelong pattern of problem drinking and have probably been alcoholics for most of their lives (Reference McInnes and PowellMenninger, 2002). American studies suggest that this category comprises two-thirds of elderly alcoholics (Reference Grant, Adams and ReedGulino & Kadin, 1986; Reference Atkinson, Tolson and TurnerAtkinson et al, 1990). Typically, there is a family history of alcoholism and these individuals had drinking problems in their early 20s or 30s. They are more likely to have psychiatric illness, cirrhosis and organic brain syndromes (Reference McInnes and PowellMenninger, 2002).
About one-third of elderly alcoholics fall into the late-onset category (Reference Adams and WaskelAdams & Waskel, 1991), first developing drinking problems at 40–50 years of age. They tend to be highly educated and a stressful life event frequently precipitates or exacerbates their drinking. Reference Brandt, Butters and RyanBrennan & Moos (1996) reported that, in contrast to early-onset problem drinkers, those in the late-onset category typically have fewer physical and mental health problems. This group is more receptive to treatment and more likely to recover spontaneously from alcoholism (Reference McInnes and PowellMenninger, 2002). A longitudinal study of the prognosis for older alcoholics found an overall stable remission of 21% in late-life drinking at 4 years, with late-onset alcoholics almost twice as likely as those with early-onset alcoholism to have stable remission with treatment (Reference Schonfeld, Dupree and Dickson-EuhrmannSchutte et al, 1994).
Key factors associated with heavy drinking
Reference Cook, Winokur and GarveyCooper et al’s (1999) review and statistical analysis of data from the 1992 and 1994 General Household Surveys and the 1993 and 1994 Health Surveys for England looking at health-related behaviour in older people revealed the following.
Gender
Men are more than twice as likely as women to exceed sensible guidelines for weekly drinking. In terms of excessive drinking, 2% of men aged 70–74 drank over 50 units per week, whereas less than 1% of women over 70 drank 35 units or more per week. Older women were more likely to abstain than men in all age bands between 55 and 85 years.
Socio-economic group
For both genders higher levels of drinking were most prevalent among the higher social classes and the most affluent.
Living arrangements and partnerships
Among older men, those who were married were least likely to drink heavily. Next came single (never-married) men. Widowed or divorced men were most likely to engage in health-damaging behaviour such as smoking or excessive drinking. In contrast, among older women those married had the highest levels of alcohol consumption. Other studies have commented on the following factors.
Social exclusion
A survey of older homeless people in London conducted about 15 years ago showed that around 30% were aged 50 and above, and of these a significant proportion had a drink problem (Reference Hurt, Finlayson and MorseKelling (1991), cited in Ward, 1997).
Ethnic and religious origins
Drinking patterns vary considerably across ethnic groups. A study carried out in England by Reference Cermak, Blow and HillCochrane & Bal (1990) found that, in general, African–Caribbean, Muslim and Hindu women reported drinking less than their White counterparts. Among Asian Muslims, Sikhs and Hindus, older men had more alcohol problems than younger men.
Genetic factors
There is substantial evidence that genetic factors are important in the development of alcohol problems. Some studies have suggested that, among men, genetics might play a greater part in early- than in late-onset alcohol misuse (Reference Atkinson, Tolson and TurnerAtkinson et al, 1990). Studies of older people in the USA have provided strong evidence that drinking behaviour throughout the lifespan is greatly influenced by genetic factors (Reference Atkinson and AtkinsonAtkinson, 1984; Reference Gulino and KadinHeller & McClearn, 1995).
Causes and triggers of problem drinking
Reference Brennan and MoosBrennan et al(1999) have commented on the complex two-way relationship between stressors and drinking behaviour, and a report by Alcohol Concern (2002) lists a number of factors that commonly lead to heavy drinking. These include bereavement – the death of a partner, family member or friend; mental stress; physical ill health; loneliness and isolation; and loss – including loss of occupation, function, skills or income. In elderly people the ageing process itself can be a causative factor (Box 1).
Box 1 Life changes associated with alcohol misuse in elderly people
Emotional and social problems
-
• Bereavement
-
• Loss of friends and social status
-
• Loss of occupation
-
• Impaired ability to function
-
• Family conflict
-
• Reduced self-esteem
Medical problems
-
• Physical disabilities
-
• Chronic pain
-
• Insomnia
-
• Sensory deficits
-
• Reduced mobility
-
• Cognitive impairment
Practical problems
-
• Impaired self-care
-
• Reduced coping skills
-
• Altered financial circumstances
-
• Dislocation from previous accommodation
Alcohol-related health problems
Alcohol use disorders in elderly people can cause a wide range of physical, psychological and social problems. Excessive drinking puts older people at increased risk of coronary heart disease, hypertension and stroke (Reference DeblingerDepartment of Health, 1995). Alcohol adds to the risk accidents and has been identified as one of the three main reasons for falls, which are a significant cause of mortality and ill health in older people (Wright & Whyley, 1994). Alcohol misuse can exacerbate insomnia and increase the likelihood of incontinence and gastrointestinal problems (Reference Speer and BatesTabloski & Maranjian Church, 1999). The incidence of osteoporosis is increased and its progression hastened in those who misuse alcohol. Alcohol may excerbate Parkinson’s disease in older people, and delirium tremens is associated with higher mortality rates in this age-group (Reference Falaschetti, Malbut, Primatesta, Prior and PrimatestaFeuerlein & Reiser, 1986). Heavy drinking is implicated in a whole set of problems relating to self-neglect, including poor nutrition, poor hygiene and hypothermia (Reference WillenbringWoodhouse et al, 1987). Older heavy drinkers are at greater risk of developing serious liver problems, including cirrhosis, and have increased incidence of cancer of the liver, oesophagus, nasopharynx and colon (Reference Schutte, Brennan and MoosSmith, 1995).
Of particular concern is the likelihood that older drinkers will be mixing alcohol and prescribed drugs. Around 8 out of 10 people aged 65 and over regularly take prescribed medicine, and polypharmacy is reasonably common: about one-third of men and women in private households are taking four or more prescribed medicines a day (Reference EwingFalaschetti et al, 2002). Alcohol is contraindicated for use with many of the drugs taken by older people. Thus, there is greater possibility of interactions with prescribed medication (Reference DunlopDunne, 1994).
Comorbidity
Considerably less is known about the comorbidity of alcohol misuse and psychiatric illness in late life. However, a few studies have shown that dual diagnosis with alcohol use disorders is important among elderly people (Reference Babor, de La Fuenta and SaundersBlazer & Williams, 1980; Reference Feuerlein and ReiserFinlayson et al, 1988; Reference Reid and AndersonSaunders et al, 1991; Reference Blow and BarryBlow et al, 1992). In their study of substance misuse, Reference SmithSpeer & Bates (1992) found that older people were more likely to have the triple diagnosis of alcoholism, depression and personality disorder, whereas younger people were more likely to have the single diagnosis of schizophrenia.
Comorbid depressive symptoms are not only common in late life, but are important in both the course and prognosis of psychiatric disorders. Estimates of the incidence of primary mood disorders in older alcohol misusers vary from 12% to 30% or more (Reference Feuerlein and ReiserFinlayson et al, 1988; Reference KellingKoenig & Blazer, 1996). Depression in older alcoholics has a more complicated clinical course, and older alcoholics with depression have an increased risk of suicide and more social dysfunction than non-depressed alcoholics; moreover, they are more likely to seek treatment for their problems (Reference Conwell, Schneider, Reynolds and LebowitzCook et al, 1991; Reference Cochrane and BalConwell, 1994). A history of alcohol use disorders is an indicator of a poorer response to treatment of late-life depression. It has been reported that a history of alcohol misuse predicted a more severe and chronic course for late-life depression (Reference Conwell, Schneider, Reynolds and LebowitzCook et al, 1991). The very high risk of suicide in this patient group should always be borne in mind.
More rarely, other psychiatric disorders such as schizophrenia may coexist with alcohol problems and complicate the treatment of both.
Dementias
It has been reported that there is increased occurrence of all types of dementia except Alzheimer’s disease in elderly people with alcohol use disorders (Reference Tabloski and Maranjian ChurchThomas & Rockwood, 2001). The reasons for this have yet to be fully elucidated, as the relationship between alcohol use and dementias such as Alzheimer’s disease is very complex. Also, it can be difficult to differentiate Alzheimer’s disease from alcohol-related dementia.
Although rates of alcohol-related dementia in late life differ depending on the diagnostic criteria used and the nature of the population studied, there is consensus that alcohol contributes to the acquisition of cognitive deficits in late life. Among participants over the age of 55 in the Epidemiologic Catchment Area study in the USA, the prevalence of alcohol use disorders was 1.5 times greater among people with mild and severe cognitive impairment than those with no impairment (Reference Folstein, Folstein and McHughGeorge et al, 1991).
Sensible drinking
Experts in the field have consistently maintained sensible drinking limits to be 21 units per week for men and 14 units per week for women. However, in England there is no specific separate recommendation for older people, and the publicised sensible drinking limits do not mention the fact that older people are more vulnerable to alcohol, as will be discussed below.
In the USA, the Reference Naik and JonesNational Institute on Alcohol Abuse and Alcoholism (1995) recommends that people over 65 years of age should consume no more than 1 standard drink per day, 7 standard drinks per week and no more than 2 drinks at any one time. This is a much clearer message that should help people to make a more informed decision about their drinking and assist carers in assessing whether an older person has a problem.
A report on UK adults’ drinking behaviour and knowledge about alcohol in 2000 showed that older people are one of the least well-informed groups when asked about alcohol units – highlighting the need for a targeted awareness campaign (Reference KrachLader & Meltzer, 2001).
Assessment and screening
Identification of alcohol problems among elderly people is difficult (Box 2). A number of studies in Australia and the USA have found that clinicians recognise alcoholism in only one-third of older hospitalised patients (Reference Cooper, Arber and FeeCurtis et al, 1989; Reference Mann, Lehert and MorganMcInnes & Powell, 1994). A number of factors impede the identification of alcohol misuse in elderly people and these are listed in Box 3. Another factor may be that health professionals working with elderly people have a mistaken perception about their prognosis, believing, for example, that elderly problem drinkers are too old to change the habit (Reference Watson, Arfken and BirgeWillenbring, 1990).
Box 2 Signs and symptoms of alcohol misuse in elderly people
-
• Anxiety
-
• Depression
-
• Blackouts
-
• Disorientation
-
• Falls, bruises
-
• Elder abuse
-
• Incontinence
-
• Increased tolerance to alcohol
-
• Memory loss
-
• New difficulties in decision-making
-
• Poor hygiene
-
• Poor nutrition
-
• Idiopathic seizures
-
• Sleep problems
-
• Unusual response to medication
Box 3 Barriers to identification of alcohol misuse in elderly people
-
• Societal myths
-
• Health practitioners’ awareness and attitudes
-
• Denial by the person
-
• Similarities between the symptoms of alcoholism and those of other conditions
-
• Unreliability of self-reports
-
• Screening instruments that are not designed to be used with elderly people
Elderly people should be routinely screened for alcohol misuse. Screening questions can be incorporated into assessments about health, nutrition and recreation. Basic screening questions about the amount and frequency of alcohol consumption such as ‘On average, how many days a week do you drink?’ or ‘How many drinks do you have on a typical day?’ may be a useful initial measure.
Screening instruments for alcohol use disorders
Many of the standard screening instruments have not been designed for use with elderly people. The CAGE (Reference DunneEwing, 1984), for example, a widely used alcohol screening test, does not have high validity with older adults, in particular with older women (Reference Adams, Barry and FlemingAdams et al, 1996). It is also limited in that it assesses only lifetime alcohol use and does not ask specifically about current drinking habits. In a large study involving more than 5000 consecutive primary care patients aged 60 and older the CAGE identified less than half of the heavy or binge drinkers (Reference Adams, Barry and FlemingAdams et al, 1996).
However, some existing tools are more appropriate for older people. These include the geriatric version of the Michigan Alcohol Screening Test (MAST–G; Reference Blazer and WilliamsBlow, 1991), which has high specificity and sensitivity with older people in a wide range of settings, including primary care clinics and nursing homes. Although the Alcohol Use Disorders Identification Test (AUDIT; Babor et al, 1992) has not been evaluated for use with elderly people it has been validated cross-culturally. It may therefore be useful for screening older people from minority ethnic groups.
It is important to bear in mind that frequency and level of consumption are commonly used criteria for identifying alcohol use disorders, but these should be used with care when assessing older people because they tend to have higher sensitivity and higher blood levels at lower alcohol consumption (Reference Schutte, Brennan and MoosSmith, 1995). The consumption level that brings an individual to the threshold of dependency is considerably lower for older drinkers (Reference Brower, Mudd and BlowCermak et al, 1996). The behavioural and health effects of alcohol are clearer indicators of alcohol use disorders in elderly people (Reference Oslin, Pettinati and VolpicelliReid & Anderson, 1997). Thus the commonly used diagnostic criteria in ICD–10 (Reference Woodhouse, Keatinge and ColeshawWorld Health Organization, 1992) and DSM–IV (American Psychiatric Association, 1994), particularly for dependence, may not apply to many older people and this should be borne in mind during assessment.
Screening for cognitive dysfunction
Cognitive dysfunction may be an indicator of alcohol use disorders and screening for it can easily be done in a clinical setting using instruments such as the Mini-Mental State Examination (MMSE; Reference Fleming, Manwell and BarryFolstein et al, 1975). However, as the MMSE is insensitive to subtle cognitive impairment and is weak on visuo-spatial testing, it may be appropriate to augment it with the ‘draw-a-clock task’ (Reference VaillantWatson et al, 1993).
Studies have demonstrated that abstinence after long-term alcohol misuse by elderly people without dementia leads to marked improvement in cognitive deficits (Reference Blow, Walton and ChermackBrandt et al, 1983; Reference Goodman and WardGrant et al, 1984). However, Brandt et al also found in their study, which mostly included moderate drinkers with no history of dementia, that even after prolonged periods of abstinence there were still deficits in learning novel associations. Screening for cognitive deficits after establishing a baseline should be repeated several weeks after abstinence to establish more valid findings.
The purpose of screening
The aim of proactive screening of elderly people (Box 4) is to identify the presence and severity of alcohol problems that might otherwise be overlooked and to determine the need for further assessment. Screening can take place in a variety of settings, including primary care, specialty care and A&E departments. As already pointed out, comorbidities are a serious concern when working with elderly people. The direction of causality between comorbid conditions and alcohol use is not always clear from the research, but the associations between these factors should always be borne in mind when conducting health screening of older people.
Box 4 Goals and rationale for screening elderly people for alcohol problems
Goals
-
• Identify:
-
• at-risk drinkers
-
• problem drinkers
-
• dependent drinkers
-
• Determine need for further assessment and treatment
Rationale
-
• Incidence is high enough to justify routine screening
-
• Adverse effects on health and quality of life are significant
-
• Effective treatments exist
-
• Treatments available are cost-effective
Treatment
The ICD −10 classification of mental and behavioural disorders due to alcohol use has two major categories: harmful use (F10.1) and dependence syndrome (F10.2). Treatment interventions generally depend on the category into which the patient falls.
Few early studies of treatments for alcohol use disorders included older people (Reference Oslin, Pettinati and VolpicelliReid & Anderson, 1997), but this appears to be changing. Elderly people have been shown to be at least as likely to benefit from treatment as younger people (Reference Cooper, Arber and FeeCurtis et al, 1989). Furthermore, at least two studies have demonstrated that older adults follow treatment regimens more assiduously and have as good if not better treatment outcomes than matched, much younger patients (Reference Atkinson, Beresford and GombergAtkinson, 1995; Oslin et al, 2002).
Brief intervention
Brief intervention is a cost-effective and practical technique that can be used with those whose drinking meets the diagnostic criteria for harmful use. It can be delivered in primary care settings by a general practitioner or other trained healthcare professional. The intervention is based on concepts derived from motivational psychology and behavioural self-control (Reference MenningerMiller & Rollnick, 1991). A brief intervention involves one or more counselling sessions, which include assessment, motivational work, patient education and feedback, contracting (e.g. keeping a drink diary, and setting goals and incentives to reduce weekly consumption) and the use of written materials (Reference Finlayson, Hurt and DavisFleming et al, 1997).
Two studies suggest that brief intervention is useful with older people. Reference Fleming, Barry and ManwellFleming et al(1999) and Reference BlowBlow & Barry (2000) used brief intervention in randomised clinical trials in primary care settings to reduce hazardous drinking among older adults. These studies show that older adults can be engaged in brief intervention, that they find the technique acceptable and that it can substantially reduce drinking among at-risk drinkers.
Specialist treatments
Dependent drinkers require specialist treatment from, for example, community alcohol teams, in-patient detoxification units and structured day or residential programmes. Self-help groups such as Alcoholics Anonymous (AA) and other voluntary agencies may also play an important role in delivering care.
Detoxification
Acute alcohol withdrawal syndrome is more protracted and severe in elderly people than in younger patients with drinking problems of equal severity (Reference Brennan, Schutte and MoosBrower et al, 1994). Out-patient detoxification may not be appropriate for older adults who are fragile, live alone with limited family support or who have multiple medical problems and prescribed medications (Reference Lader and MeltzerLiskow et al, 1989). In view of this and the high degree of medical comorbidity in elderly people, it has been recommended that elderly alcohol-dependent patients undergo in-patient detoxification (Reference NortonO’Connell et al, 2003). Unless contraindicated, parenteral thiamine should be given initially to prevent Wernicke–Korsakoff syndrome.
Benzodiazepines are the mainstay of the pharmacological management of alcohol withdrawal. However, benzodiazepine-assisted withdrawal should be undertaken with care in elderly people because of the drug’s altered pharmacokinetics in this population and their increased sensitivity to its adverse effects (Reference Heller, McClearn, Beresford and GombergHurt et al, 1988). Some experts recommend that short-acting benzodiazepines be used with elderly people, to lessen the chances of sedation and drug interactions (Reference DerryDufour & Fuller, 1995).
Drug-maintained abstinence
The use of medications to promote abstinence has not been studied extensively in elderly people. Disulfiram should be used cautiously and only in the short term because of the risk of precipitating a confusional state (Reference DunlopDunne, 1994). It acts by preventing the breakdown of alcohol by acetaldehyde dehydrogenase. This leads to an extremely unpleasant reaction even after the ingestion of a small amount of alcohol. Reactions include flushing of the face, throbbing headache, palpitations, tachycardia, nausea and vomiting. A number of studies recommend that disulfiram should not be prescribed to elderly people because of the increased risk of serious adverse effects due to physical comorbidities and polypharmacy (Reference DerryDufour & Fuller, 1995; Reference Saunders, Copeland and DeweySchonfeld & Dupree, 1995).
Acamprosate is a γ-aminobutyric acid (GABA) analogue that is thought to act by reducing glutamate overactivity and enhancing inhibitory neurotransmission.
Compared with disulfiram, acamprosate has a benign side-effect profile, is less likely to cause dangerous drug interactions and is more effective even in people with liver damage. Acamprosate treatment should be initiated as soon as abstinence has been achieved. It prevents the biochemically based cravings for alcohol that usually arise in response to learned environmental cues such as passing a familiar pub. A meta-analysis of studies involving younger patients on acamprosate showed a 13% overall improvement in 12-month continuous abstinence rates (Reference Liskow, Rinck and CampbellMann et al, 2004).
Naltrexone, an opiate antagonist that has also been found to reduce cravings, is currently not licensed in the UK to treat alcohol dependence.
It is important to emphasise that pharmacotherapy should generally be adjunctive to psychological and social interventions. Involvement of family members in the monitoring of medication may result in better adherence and earlier identification of side-effects.
Psychological treatments
Psychological treatments include psychoeducation, counselling and motivational interviewing. Reference Blow, Cook and BoothBlow et al(2000) and Reference Schonfeld and DupreeSchonfeld et al(2000) found that cognitive–behavioural approaches were successful in reducing or stopping alcohol use. These included teaching older adults the skills necessary to rebuild social support networks and to use self-management to overcome depression, grief and loneliness.
Alcoholics Anonymous (AA) was founded nearly 70 years ago in the USA as a mutual self-help group. It is now a worldwide organisation, which is easily accessible, inexpensive and available in the evenings and at weekends. Participants need to have abstinence as their goal and new attendees are encouraged to attend 90 meetings in 90 days.Footnote 1 However, elderly people may believe that they would not fit into a group or have differing concerns from younger members. In addition, they may have age-related mobility or hearing problems that may prevent participation.
Norton (1998) has suggested that elderly people fare better in self-help groups of their peers. Older people may also find smaller groups less threatening. Healthcare professionals should explain the nature of these groups to patients to allay their anxieties. Other options are to help patients set up their own self-help groups or even to facilitate the development of local AA groups for elderly people. Although published research on the effectiveness of AA is limited, Reference Thomas and RockwoodVaillant (2003), in his prospective 60-year follow-up study in the USA of men from different social groups, found that one of the best predictors of sustained abstinence was AA attendance.
Elderly patients who are physically or cognitively very frail may need intensive support from geriatric and psychogeriatric services. They would also benefit from the involvement of local social services, voluntary and other community agencies for home care, transportation and other services. The involvement of family members in the treatment of elderly people is of critical importance and likely to improve adherence (Reference Dufour and FullerDunlop, 1990; Reference Atkinson, Tolson and TurnerAtkinson et al, 1993).
Conclusions
Alcohol use disorders in elderly people are a common but underrecognised problem. They are frequently associated with particular precipitants such as loss, social isolation and medical and psychiatric comorbidity. There is some evidence to suggest that elderly people benefit as much from treatment as do younger patients. However, owing to the difficulty of identifying and treating alcohol use disorders in elderly people, services need to develop an outreach approach. This should include the provision of well-placed information explaining the problem and the type of help available (Reference George, Landerman, Blazer, Robins and ReigerGoodman & Ward, 1995).
Training and awareness among health practitioners is important to change attitudes and identify alcohol misuse in elderly people. Good liaison between services is essential for promoting continuity of care (Derry, 2000). This is particularly important in the case of specialist substance misuse and psychogeriatric services. In view of the complexity of the health and social issues involved, integrated care pathways, joint assessments and case management are important for effective service provision. Close partnership with the voluntary sector is also an important factor in effective treatment.
At a policy level, it is important that the needs of elderly people are highlighted in national service frameworks and strategies. This does not appear to have been done so far, which might be because of wider issues of ageism and the reluctance of some specialist alcohol services to open their doors to elderly people.
Most of the evidence showing the effectiveness of treating alcohol use disorders in elderly people originates in the USA. Furthermore, much of this research is limited to White men in US veteran hospitals. Few empirical studies have compared treatment modalities and no studies have compared treatment with no treatment. Very few studies have addressed the safety and efficacy of pharmacotherapy to aid abstinence in elderly people. There is therefore an urgent need for further research, particularly in the UK. This would help treatment services to determine the exact extent of the problem and to develop and test time- and cost- effective screening methods and interventions to provide optimal care for a vulnerable, growing and underrecognised group.
Declaration of interest
None.
MCQs
-
1 Alcohol misuse in elderly people:
-
a is a very rare problem
-
b can be easily misdiagnosed
-
c can present as depression and self-neglect
-
d can be classified into two categories
-
e is more common in women than in men.
-
-
2 In elderly people:
-
a there are clear recommended sensible drinking limits
-
b there is greater vulnerability to the harmful effects of alcohol
-
c routine screening for alcohol problems is not useful
-
d alcohol problems are often triggered by loss and isolation
-
e health professionals are often reluctant to enquire about alcohol consumption.
-
-
3 Alcohol-related health problems in elderly people include:
-
a increased risk of coronary heart disease
-
b increased risk of falls
-
c increased risk of Alzheimer’s disease
-
d increased incidence of suicide
-
e decreased risk of prescribed drug interactions.
-
-
4 Management of alcohol problems in elderly people:
-
a may be hampered by health practitioners’ attitudes and training
-
b involves paying more attention to consumption levels rather than behavioural and health effects
-
c involves using appropriate screening tools such as the MAST–G
-
d involves principles that differ from those used for younger people
-
e always require admission to hospital.
-
-
5 In the treatment of alcohol problems in elderly people:
-
a brief intervention is efficacious and cost-effective
-
b in-patient treatment is recommended for most individuals requiring detoxification
-
c use of disulfiram is supported by extensive research
-
d cognitive–behavioural techniques are ineffective
-
e further research is urgently required to develop more evidence-based interventions.
-
MCQ answers
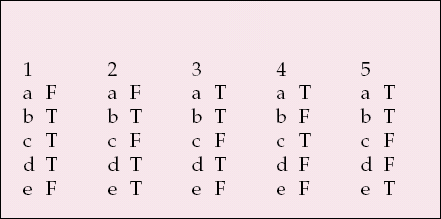
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | T | a | T | a | T |
| b | T | b | T | b | T | b | F | b | T |
| c | T | c | F | c | F | c | T | c | F |
| d | T | d | T | d | T | d | F | d | F |
| e | F | e | T | e | F | e | F | e | T |





eLetters
No eLetters have been published for this article.