Patients’ records are among the most basic of clinical tools and are involved in almost every consultation. They are there to give a clear and accurate picture of the care and treatment of patients and to assist in making sure they receive the best possible clinical care. They help doctors to communicate with other doctors, with other healthcare professionals and with themselves (Medical Defence Union, 2003), and are essential to ensure that an individual’s assessed needs are met comprehensively and in good time.
Psychiatric practice has moved from the unidisciplinary out-patient clinic and specialist in-patient assessment, with separate records being kept by each discipline, to the long-term management of chronic illness. The latter involves delegated and dispersed responsibility within teams comprising different disciplines and agencies and working from different sites, with emphasis on clinical guidelines and risk management. The tasks can be summarised as:
-
• increasing support for self-care
-
• strengthening and extending primary care
-
• offering responsive specialist care
-
• managing vulnerable people by anticipating their needs (Scottish Executive, 2005).
Thus, the shape and organisation of services, and the tasks performed by the workforce, have evolved beyond recognition. Despite this, case notes have not changed significantly for 40 years.
Good records do more than support good patient care; they are essential to it. This is exemplified by the standards set out by the General Medical Council (2001) and the Royal College of Psychiatrists (2004). Records remain the most tangible evidence of a psychiatrist’s practice and, in an increasingly litigious environment, the means by which it may be judged. The record is the clinician’s main defence if assessments or decisions are ever scrutinised. However, the primary purpose of the patient’s record is to enable clinicians to communicate with themselves.
This article reviews the purposes of record-keeping, the standards to which clinicians should aspire, some criticisms of current practice and the role of continuous quality improvement. It sets out good practice points which should be equally applicable in the development of electronic clinical records.
The purposes of record-keeping
The clinical record has many functions, the most important of which are listed in Box 1. It brings together historical and contemporaneous information from multiple sources, recorded by numerous individuals from many organisations. It is also used increasingly in the assessment of professional competence: review of case notes and other records is a suggested method for assessing key competencies (Royal College of Psychiatrists, 2006). These purposes are mutually interdependent. For example, a case record which is fit for purpose as a working document for day-to-day recording of patient care is more likely to generate useful information for research.
Box 1 The purposes of the clinical record
-
• To act as a working document for day-today recording of patient care
-
• To store a chronological account of the patient’s life, illnesses, its context and who did what and to what effect
-
• To enable the clinician to communicate with him- or herself
-
• To aid communication between team members
-
• To allow continuity of approach in a continuing illness
-
• To record any special factors that appear to affect the patient or the patient’s response to treatment
-
• To record any factors that might render the patient more vulnerable to an adverse reaction to management or treatment
-
• To record risk assessments to protect the patient and others
-
• To record the advice given to general practitioners, other clinicians and other agencies
-
• To record the information received from others, including carers
-
• To store a record to which the patient may have access
-
• To inform medico-legal investigations
-
• To inform clinical audit, governance and accreditation
-
• To inform bodies handling complaints and inquiries
-
• To inform research
-
• To inform analyses of clinical activity
-
• To allow contributions to national data-sets, morbidity registers, etc.
(Adapted from Scottish Office, 1995)
What is expected of psychiatrists?
Good psychiatric practice involves keeping complete and clear records and ensuring good communication with all agencies and between professionals (Royal College of Psychiatrists, 2004). Ways in which this can be achieved are set out in Box 2.
Box 2 Good practice in note-keeping and communication between agencies and professionals
Psychiatrists must:
-
• ensure that good clinical records are kept of all key decisions or assessments
-
• ensure that notes are legible and clearly identified
-
• ensure the inclusion in the clinical record of consent having been given by the patient for information to be shared with a family member or carer
-
• ensure the inclusion in the clinical record of information shared with or received from carers or family members
-
• communicate treatment decisions, changes in care plans and other necessary information to all relevant agencies and professionals, either in writing or personally, paying due regard to confidentiality
-
• not tamper with notes, or change or add to entries once they have been signed without identifying the change, dated and signed
-
• provide timely reports where appropriate
Unacceptable practice includes:
-
• retrospectively altering case notes
-
• not dating and signing all entries (all entries in case notes must be identifiable)
-
• not recording key decisions
(Royal College of Psychiatrists, 2004: p. 23)
Standards governing team-based care
Although doctors are not accountable to the General Medical Council for the decisions and actions of other clinicians, it is clear that they should do their best to ensure that patients receive a good standard of care. If doctors believe that this is not happening and they cannot take steps to resolve the problems, they should draw the matter to the attention of their trust or other employing or contracting body (Department of Health, 2005: p. 17). In the context of record-keeping, it is reasonable to conclude that a trust or other employing organisation has no alternative but to negotiate moves to a single clinical record, as no alternative can accommodate the recording of multidisciplinary practice.
A relatively recent review of clinical record-keeping and communication noted the lack of a standard model across the National Health Service (NHS) for documenting and communicating information in patients’ health records (Reference ScottScott, 2004). Drawing on guidance from the General Medical Council, Health Professions Council and Nursing and Midwifery Council, Scott described four aspects of good practice in this area:
-
• the readiness of individuals to keep up to date with legal requirements, proficient in record-keeping practice and adept at using the local systems
-
• the expectations that each professional body has of its members
-
• standardisation of recording and communication across the professions and organisations (healthcare and non-healthcare) involved in the provision of patient care
-
• provision by organisations of the appropriate systems and proper procedures to enable good practice to flourish.
The review identified four themes affecting individual practice:
-
• confidentiality and disclosure – covering, in addition, patient consent, rights of access to records, security of storage and awareness of the relevant legislation
-
• communication – information should be recorded or communicated simply, accurately and with sensitivity to the recipient’s awareness and understanding
-
• personal and professional knowledge and skills – each person has an obligation to develop the appropriate level of skill and awareness of best practice in communication, and of both national and local guidance
-
• process principles – for example, patients’ records should not include excessive abbreviations, jargon, value judgements and irrelevant or offensive speculation.
The effects of poor record-keeping
The standards of record-keeping in health services in general and mental health services in particular have been criticised by public bodies and official inquiries into deficiencies of care.
In 1995 the Audit Commission published the results of its study of record-keeping in NHS hospitals in England. It found the standard to be poor and strongly recommended that corrective action be taken. The key issues to be addressed were: the low priority given to records management; the lack of awareness of the importance of good record-keeping; the lack of information-sharing between professions and work units; the tendency to treat records as personal rather than corporate assets; the lack of coordination between paper and electronic information strategies; and the need to maintain confidentiality while legitimately freeing information (Audit Commission, 1995). All of these themes were echoed in the report of the Public Inquiry into children’s heart surgery at the Bristol Royal Infirmary (Secretary of State for Health, 2001).
There has been similar consistency in the shortcomings identified by inquiries into homicides by people with mental illness over the past 10 years. Findings that emerge again and again include: a lack of clarity in the planning and coordination of care; poor record-keeping; inadequate communication between key players, be they professionals, agencies or families; and poor implementation of statutory obligations and national and local guidance (Reference MackayMackay, 2004). Three of these four may result from the problems of multidisciplinary and multi-agency working when explicit priority is not given to recording and communicating activity to an accepted standard.
The Irish Ombudsman has also expressed his concern about the state of record-keeping (Reference BirchardBirchard, 2001). Despite reminders by professional bodies and medical indemnity providers that doctors must keep up-to-date records, the Ombudsman reported before a parliamentary committee in 2001 that some doctors and consultants were writing up their records long after the fact and his office suspected that, in some cases under investigation, records were not written until the investigation itself was launched. Birchard notes that the Medical Defence Union (MDU) was reported to agree with the Ombudsman:
‘At the MDU we see the problems which arise from poor, inadequate, or absent notes. We cannot stress enough the importance of clear, concise contemporaneous notes which serve primarily to enhance patient care but are also useful in protecting a doctor’s interests’.
Reference Findlayson and WatsonFindlayson & Watson (2004) think that poor-quality record-keeping may be so common partly because medical records are generally accorded a low priority and partly because national attempts at standardisation are often defeated by the sheer complexity of patient care. Although they do not say so explicitly, it might be inferred that, until keeping good case records starts to matter enough to clinicians, little general or no consistent change can be expected.
In its second review of the implementation of standards for schizophrenia across Scotland, NHS Quality Improvement Scotland (2004) noted that:
‘there is a lack of standardised approaches to documentation that would enable a continuous record of assessed needs, and resulting plans of care, to follow an individual with a long-term mental illness throughout his or her journey of care. In some services each professional group is still using separate case notes, held or stored in different places, and not likely to be available when required. There are few examples of integrated interagency records being used’ (p. 72).
The place of case records in the practice of local mental health services may show little appreciation of their importance. It is likely that compromises in safety, risk management and making full use of available information come to be accepted as normal. It is therefore unlikely that much time or effort will be invested in them or their improvement.
The following example shows an amalgam of practices from a number of services and does not relate to any particular hospital.
Undesirable practice
A modern district general hospital supports an accident and emergency (A&E) department and a full range of physical specialties. A psychiatric liaison service operates at the hospital around the clock, to give urgent patient assessments and treatment advice on the wards and in the A&E department. This is usually provided by a senior house officer (SHO). The psychiatric hospital for the NHS board area is 20 miles distant and is where psychiatric case records are stored.
In the absence of an electronic information system there is no means by which the psychiatric SHOs (still junior doctors) can check easily on previous contact with the service by a patient they are about to interview. Local custom does not make access possible to any existing psychiatric case record held at the psychiatric hospital. During working hours, if it is known that a case file exists, the medical records clerk may be persuaded to fax a few of the most recent letters filed in the case record (but these may not contain all relevant information). Out of hours and at weekends, no such facility exists. The best the doctor can then hope for is that a nurse on the psychiatric hospital acute ward will know the patient and be able to provide some relevant information.
Under such circumstances practice can only be based on assumption, guesswork and innuendo, ignorant of risk and liable to fail dangerously. A unified and available case record would not by itself make practice perfect, but it is an essential basis for good team communication.
Standards
The Royal College of Physicians’ Health Informatics Unit has developed 30 evidence-based standards for record-keeping, which are currently going through a process of consultation (Reference Mann and WilliamsMann & Williams, 2003). It has also designed an audit tool (Royal College of Physicians’ Health Informatics Unit, 2003a ).
Nationally, the NHS has included record-keeping in its Continuous Quality Improvement initiative. The NHS Litigation Authority, which is responsible for handling negligence claims made against NHS bodies in England, has produced a range of clinical risk management standards (http://www.nhsla.com/RiskManagement/). Similar arrangements are in place in Scotland (http://www.cnoris.com/).
Here we will concentrate on the Clinical Negligence Scheme for Trusts (CNST) Mental Health and Learning Disability Clinical Standards (NHS Litigation Authority, 2006). The scheme, which is administered by the NHS Litigation Authority (NHSLA), was developed to provide cost-effective claims management in England. National Health Service trusts receive a discount on their contributions to the scheme if they can demonstrate compliance with CNST standards. These standards, which are fully endorsed by the Royal College of Psychiatrists (NHS Litigation Authority, 2006: p. 4), are aimed at minimising risk and hence liability. The functions of the NHSLA are described in an introductory factsheet (NHS Litigation Authority, 2005).
CNST standards
Each standard is derived from a criterion based on published sources, with related guidance for the trust on how to ensure the standards can be met. For example, criterion 4.1.3 may be summed up ‘as all records should be designed in such a way as to make information readily accessible’. The guidance to achieve this suggests a physically robust record containing no ‘inside pockets or sleeves’, as these lead to misfiling or loss of documents. The quality of care that a patient receives will also suffer if case notes are poorly structured.
Standard 4 refers to clinical information and the care record. Level 1 sets out the basic elements of clinical risk management. Levels 2 and 3 are more demanding. Each standard is based on guidance.
Level 1
The lowest of the three levels requires, among other things, that:
-
• within the trust there is a committee responsible for care records, whose remit includes the format and quality of records
-
• a system is in place to identify whether a service user is receiving/has received care in any part of the trust
-
• all records used during in-patient admission contain instructions regarding filing and are designed so that key information (e.g. care programme approach and Mental Health Act documentation) is readily identifiable
-
• clear evidence is available of annual audit of record-keeping standards in at least 25% of services.
Level 2
Among Level 2 requirements are that:
-
• professionals have access to unified clinical information (one record per patient across the trust, or all records for a patient if more than one exists) at first new consultation
-
• there are interagency agreements on the sharing of information
-
• clear evidence is available of annual audit of record-keeping standards in at least 50% of services.
Level 3
The highest level requires that:
-
• the author of each entry is clearly and easily identifiable
-
• clear evidence is available of improvement in recorded-keeping standards across the trust through annual audit for all professional groups.
Training initiatives
Another project from the Health Informatics Unit is a portfolio of educational exercises (Royal College of Physicians’ Health Informatics Unit, 2003b ) in subject areas identified by the Chief Medical Officer for the foundation years of medical training (Department of Health, 2002). The portfolio includes modules on record-keeping and communication.
Quality improvement within an organisation springs from the development of its members (Royal College of Psychiatrists, 2001). The Health Informatics Unit’s training exercises are endorsed by the Royal College of Psychiatrists, which itself requires that its trainees acquire record-keeping skills and proficiency in the communication of the conclusions of psychiatric assessment clearly, accurately and in appropriate detail to general hospital staff (Royal College of Psychiatrists, 2006).
Improving case records
It is a truism that the way things are is the product of the wishes, decisions, values and priorities, explicit and implicit, of a sufficient number of people within the system in question. So it is with the locally prevailing practice in record-keeping anywhere in the UK. The lack of any development in the format and relevance to modern practice of the psychiatric case record suggests that few appreciate the need for change. As ever, in the successful management of change there has to be a systematic process of arousing awareness, recruiting the support of key decision makers and opinion formers and application of key quality improvement tools (adapted for the specific purpose). The emphasis has to be on achieving continuing improvement in practice, not just on finding out how things are. However, it is important to focus the improvement effort effectively. Excellent though they are, it is hard to see how focus can be maintained on all of the Royal College of Physicians’ 30 standards were they to be adapted for practice in the many and diverse mental health environments. It would be better to focus on five or six key areas, such as:
-
• all but the most transient contact with a patient or carer should be recorded
-
• the record should be made in an appropriately structured multidisciplinary clinical or care folder, under the general headings: reason for contact; findings; conclusion; action to be taken; and who was informed
-
• every entry should be legible, dated, timed and signed
-
• access to the folder should be clearly defined in local policies and procedures, but free access by the relevant user should be the usual practice (except in defined circumstances)
-
• the local organisation should be accountable for the quality of support, training and development provided for professionals and other workers
-
• record-keeping and communication should be subject to continual quality development under the umbrella of clinical governance.
Some practical ways of improving record-keeping are set out in Box 3.
Box 3 Practical ways of improving record-keeping
-
• Personally sign all typed letters and entries on the case record
-
• Sign and write name in block capitals for clear identification of handwritten entries
-
• Date and time all case-record entries
-
• Give as much thought to case-record entries as to dictated letters
-
• Be thorough but concise
-
• Include periodic summaries in the records of patients in long-term contact with services
-
• Be mindful that the quality of the case record will be assumed to reflect the quality of the care received
Electronic records
Clinical needs for record-keeping and information management should be the driver for the development of electronic records. Examples of progress in the mental healthcare arena are appearing.
Electronic records that are complete, integrated and legible offer added value; for example they can be accessed from multiple sites and can be used to generate risk alerts and prompts indicating that new information is available. In an earlier issue of APT Reference LewisLewis (2002) set out sound advice and guidance on the organisation of clinical information for electronic recording. His points remain relevant. He emphasises the importance of standardised approaches for the recording and organising of information as a means of facilitating good communication, without which there is a risk of poor patient care.
However, paper records will be with us for some time. It is important to recognise that the points that Lewis makes apply as much to written clinical records. The low priority given until now to medical records suggests that the information they contain is not valued highly, that the gain from an investment of time and effort in improving records is not seen as being worth the effort. The introduction of an electronic system will not in itself improve matters. Mental health services first need to develop ‘information mindedness’, a term that covers the development of an information culture, agreement on a minimum set of data to be collected for day-today purposes, and definition of the core purposes of information collection.
The way ahead
Although mental health services in the UK and Ireland have undergone regular structural and managerial changes over the past decade, for many psychiatrists their ways of working and record-keeping will have changed relatively little. However, demographic factors, including an ageing population, fewer school leavers and a developing health economy, require a more imaginative approach to expanding the mental healthcare workforce (Department of Health, 2004a ). The challenge is to use the skills of highly trained mental health professionals to the maximum benefit of services and service users. Psychiatrists will be asked to find new ways of working within teams that combine different disciplines and agencies and that rely on distributed rather than devolved responsibilities. This will raise important issues of responsibility, leadership and continuity of care (Department of Health, 2004a ).
Within its Changing Workforce Programme the Department of Health has designated a number of NHS mental healthcare trusts as pilot sites for new ways of working. One of these, the Avon and Wiltshire Mental Health Partnership NHS Trust, has attempted to resolve the confusion surrounding the limits of the responsibilities of consultant psychiatrists. It has collated guidance from the College of Psychiatrists, General Medical Council and Mental Health Act 1983, and has added guidelines of its own (Department of Health, 2004a ). This guidance includes: triage of referrals; multidisciplinary assessments; reduction or elimination of ‘routine follow-ups’ in consultant out-patient clinics; improving case-load management; and crisis team gatekeeping of in-patient beds (Department of Health, 2004a , b ,c). Considering the practicalities of these changes, teams will need robust processes for the allocation of work and the management of clinical risk. This will require integrated care planning with clear audit trails via a single health record that names the team and care coordinator for an episode of out-patient care, and the team and the consultant for an episode of in-patient care.
The wider recognition of family-friendly employment within the NHS (Department of Health, 2000), leading to more flexible and part-time working and real multi-agency care pathways, poses further challenges to the continuity and quality of care. These will be safely addressed only through changing roles and working practices, underpinned by improved standards of record-keeping.
Declaration of interest
The views expressed in this paper are the personal views of the authors and do not necessarily represent the policies of the Scottish Executive or NHS Quality Improvement Scotland.
MCQs
-
1 The Royal College of Psychiatrists’ publication Good Psychiatric Practice:
-
a requires that medical notes be typed for clarity
-
b encourages recording of information shared with others
-
c does not require typed entries to be signed
-
d requires key decisions to be recorded
-
e is adapted from the Medical Defence Union’s Good Medical Practice.
-
-
2 The standard of record-keeping has been criticised in many reports. Possible reasons cited for this are:
-
a the low priority given to records management
-
b notes being written up long after the event
-
c notes being seen as the property of one doctor
-
d to protect a doctor’s interests
-
e to protect confidentiality.
-
-
3 Good clinical records will:
-
a be multidisciplinary
-
b demonstrate appropriate risk assessment
-
c protect a doctor’s interests in the event of criticism or litigation
-
d contain clear instructions to guide filing
-
e be readily accessible in office hours but, for security reasons, not available out of hours.
-
-
4 For clinicians’ practice to improve:
-
a expected standards of record-keeping should be set out explicitly
-
b the results of poor practice should be exposed by national inquiries
-
c national organisations should warn of the risks of poor records
-
d there should be national agreement on what constitutes a good record
-
e keeping good records should be a fundamental part of training for all staff.
-
MCQ answers
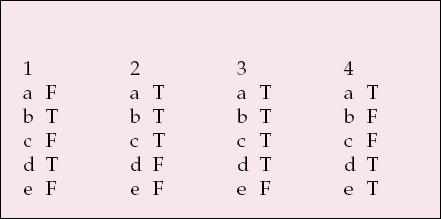
| 1 | 2 | 3 | 4 | ||||
|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | T |
| b | T | b | T | b | T | b | F |
| c | F | c | T | c | T | c | F |
| d | T | d | F | d | T | d | T |
| e | F | e | F | e | F | e | T |





eLetters
No eLetters have been published for this article.