Complementary therapies have become hugely popular. A colleague and I estimated that, in 1999, the total expenditure for such treatments in the UK was £1.6 billion (Reference Ernst and WhiteErnst & White, 2000). There is reason to believe that the usage of complementary medicine in the UK has increased since then (Reference Emslie, Campbell and WalkerEmslie et al, 2002). The lion's share of this amount is not covered by the NHS – by and large patients pay privately for complementary medicine. Herbal medicine is among the most popular complementary therapy: in the UK 34% of all users of complementary medicine take such remedies (Reference Ernst and WhiteErnst & White, 2000). Depression and anxiety are prominent indications for herbal medicines (Reference Eisenberg, David and EttnerEisenberg et al, 1998; Reference Kales, Blow and WelshKales et al, 2004; Reference Roy-Byrne, Bystritsky and RussoRoy-Byrne et al, 2005) and the majority of people with depression try complementary medicines (Reference Silvers, Woolley and HedderleySilvers et al, 2006).
People's reasons for trying herbal medicines are complex (Reference Ernst, Pittler and StevinsonErnst et al, 2001). British consumers have been shown to expect symptom relief, information, a holistic approach, improved quality of life and self-help advice from consulting complementary therapists (Reference RichardsonRichardson, 2004). American survey data suggest that significant associations exist between the specific domain of personality, coping strategies and social support on the one hand and use of complementary therapies on the other. Openness and perceived friend support were positively, and extroversion was inversely, correlated with the use of complementary medicine (Reference Honda and JacobsonHonda & Jacobson, 2005). We should also not underestimate the lure of the popular media. About 41 million websites offer information on the subject, much of which is unreliable or outright dangerous (Reference Ernst and SchmidtErnst & Schmidt, 2004). The UK daily press tends to be less than critical about complementary medicine (Reference Ernst and WeihmayrErnst & Weihmayr, 2000), and books for the layperson are frequently misleading: when colleagues and I extracted the recommendations from seven such texts, we found that the authors had recommended a total of 131 different treatments for anxiety and 87 for depression (Reference Ernst, Pittler and StevinsonErnst et al, 2001).
In this article, I will review the evidence for or against herbal remedies as treatments for depression and anxiety. My assessment is based on a systematic review of the published literature (literature searches in Medline, EMBASE, the Allied and Alternative Medicine Database (AMED) and the Cochrane Library up to June 2005) with an emphasis on controlled clinical trials and systematic reviews (Reference Ernst, Boddy and PittlerErnst et al, 2006). Its focus is on herbal medicine; thus, non-herbal supplements are excluded even if the evidence is encouraging, as it is for omega-3 fatty acids (Reference Freeman, Hibbeln and WisnerFreeman et al, 2006).
Depression
Ineffective remedies
Ginkgo biloba (maidenhair tree) was tested in a small (n = 27) trial involving people with ‘winter depression’. The results did not suggest that this approach was superior to placebo (Reference Lingaerde, Foreland and MagnussonLingaerde et al, 1999). It has, however, been shown to be effective for conditions such as dementia (Reference Ernst, Pittler and StevinsonErnst et al, 2001).
Promising remedies
Lavandula angustifolia (common lavender) was compared with imipramine in a small randomised controlled trial (RCT) including 45 individuals with moderate depression (Reference Akhondzadeh, Fallah-Pour and AfkhamAkhondzadeh et al, 2004). Both treatments seemed similarly effective but the study had significant methodological shortfalls (e.g. it was not designed as an equivalence trial). Another trial designed along the same lines suggested that Crocus sativus (saffron crocus) and imipramine were similarly effective (Reference Akhondzadeh, Kashani and FotouhiAkhondzadeh et al, 2003). Unfortunately, the same limitations applied.
Effective remedies
The only herbal remedy that has been shown beyond reasonable doubt to be effective as a treatment for mild to moderate depression is Hypericum perforatum (St John's wort). The active ingredients of this herbal medicine are probably hypericin and/or hyperforin. Its antidepressive activity seems to be due to inhibition of both serotonin reuptake and monoamine oxidase.
An authoritative systematic review and meta-analysis included 30 RCTs involving individuals mostly (but not exclusively) with mild to moderate depression (Reference Roder, Schaefer and LeuchtRoder et al, 2004). The methodological quality of these trials was variable but many scored highest marks. Twenty five of them, involving a total of 2129 patients, compared St John's wort with placebo. The results strongly favoured the former over the latter (risk ratio = 0.66, 95% CI 0.57–0.78, number needed to treat = 42). Five trials, involving a total of 2231 patients, compared St John's wort with conventional antidepressants (including selective serotonin reuptake inhibitors (SSRIs)). The risk ratio of 0.96 indicates equivalence of these approaches. A subsequent Cochrane Review (Reference Linde, Mulrow and BernerLinde et al, 2005) reported similarly encouraging results.
So why use this herbal remedy if it is not better than conventional drugs? One answer could be that many patients prefer ‘natural’ treatments. A perhaps more convincing answer is that its adverse effects profile is preferable. In fact, St John's wort is associated with similar frequency and severity of adverse effects as placebo. There are, however, two caveats. Extracts of St John's wort powerfully interact with the cytochrome P450 enzyme system and thus increase the plasma level of a wide range of other drugs (Reference Mills, Montori and WuMills et al, 2005). It seems to follow that it is safe only for people who use no other medication. The second caveat is the suspicion that St John's wort can trigger psychoses, particularly in patients who concomitantly take SSRIs (Reference Izzo and ErnstIzzo & Ernst, 2001).
Anxiety
Ineffective remedies
No anxiolytic effects of valerian (Valeriana officinalis) extract were noted in an RCT involving 66 people with generalised anxiety disorder (Reference Adreatini, Sartori and SeabraAdreatini et al, 2002).
Promising remedies
A large RCT found that a combination of Crataegus oxyacantha (hawthorn), Eschscholzia californica (Californian poppy) and magnesium was more effective than placebo in reducing anxiety in 264 individuals with generalised anxiety disorder (Reference Hanus, Lafon and MathieuHanus et al, 2004). There is some evidence for the efficacy of Matricaria recutita (German chamomile) in the treatment of anxiety (Reference Wong, Smith and BoonWong et al, 1998), but the study was methodologically weak. Short-term anxiolytic effects were noted after administration of Melissa officinalis (lemon balm) to healthy volunteers (Reference Kennedy, Little and ScholeyKennedy et al, 2004). Passiflora incarnata (passion flower) generated encouraging anxiolysis in an RCT with 36 people who had generalised anxiety disorder (Reference Akhondzadeh, Naghavi and VazirianAkhondzadeh et al, 2001). Even though these results are encouraging they do require independent replication before firm recommendations can be made.
Effective remedies
The only herbal remedy that is demonstrably effective in reducing anxiety is Piper methysticum (kava). Our Cochrane Review included 11 RCTs, involving a total of 645 patients (Reference Pittler and ErnstPittler & Ernst, 2003). The methodological quality of these studies was variable but some were excellent. Without exception, these trials showed anxiolytic effects of kava that were superior to placebo.
Despite these clearly positive efficacy data, kava cannot currently be recommended for clinical use. This is because it has been associated with (sometimes severe) hepatotoxicity (Reference ErnstErnst, 2004). Recently there has been much debate about whether this association is causal or not. At present, however, this herbal remedy remains banned from the UK market.
Comments
Most clinicians will find this summary of the trial data (Table 1) less than encouraging: apart from St John's wort, there is hardly anything within the realm of herbal medicine that can be recommended to patients suffering from anxiety or depression. Some remedies might work but, at present, we cannot be sure. Why is there still so much uncertainty in herbal medicine – after all, it is millennia older than pharmacology?
Table 1 Herbal medicines for depression and anxiety

| Not effective | Promising | Effective | |
|---|---|---|---|
| Depression | Ginkgo biloba (maidenhair tree) |
Lavandula angustifolia (common lavender) Crocus sativus (saffron crocus) |
Hypericum perforatum (St John's wort) |
| Anxiety | Valeriana officinalis(valerian) |
Matricaria recutita (German chamomile) Melissa officinalis (lemon balm) |
Piper methysticum (kava) (but banned in UK) |
Research difficulties
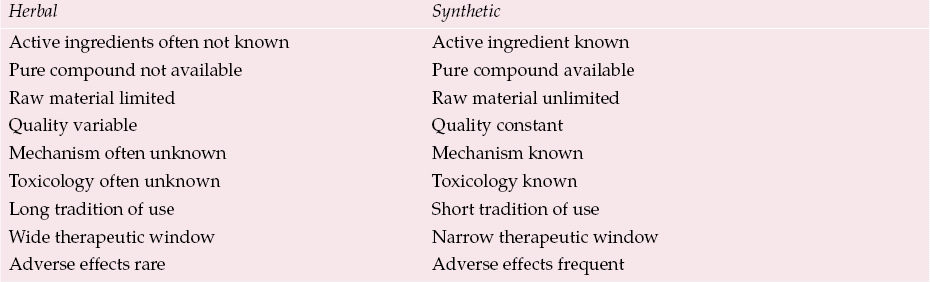
Herbal medicines are mixtures of many active ingredients. They differ from synthetic drugs in several ways (Table 2). Often it is more than one herbal active ingredient that brings about the clinical effects we observe in patients. In many instances we have not yet identified any or all of the active ingredients. Moreover, the quality of herbal remedies varies considerably (Reference Garrard, Harms and EberlyGarrard et al, 2003) owing to a range of factors: plant species, soil, climate, storage, extraction method, etc. This complexity complicates research.
Table 2 Herbal medicines v. synthetic drugs
| Herbal | Synthetic |
|---|---|
| Active ingredients often not known | Active ingredient known |
| Pure compound not available | Pure compound available |
| Raw material limited | Raw material unlimited |
| Quality variable | Quality constant |
| Mechanism often unknown | Mechanism known |
| Toxicology often unknown | Toxicology known |
| Long tradition of use | Short tradition of use |
| Wide therapeutic window | Narrow therapeutic window |
| Adverse effects rare | Adverse effects frequent |
The clinical effects of herbal medicines are usually moderate and often appear only after prolonged periods of administration. Clinical trials therefore need to be large and long-term. These facts tend to render clinical trials more expensive. Even though the sector as a whole achieves a sizeable turnover (Reference WrightWright, 2005), single herbal manufacturers are usually relatively small and, compared with ‘big pharma’, they are typically not financially powerful. To make things worse, normally there is no patent protection of herbal extracts. Thus, there is little money to support expensive trials and even less impetus to spend it on research. This already bleak situation will be further aggravated by recent legislation: the European Directive on Traditional Herbal Medicinal Products, which came into force in October 2005, does not require proof of efficacy through clinical trials for registering herbal medicines under this scheme. Thus the incentive to conduct such research approaches zero.
Is there a way out of this dilemma? One solution would be to follow the American example and set aside ‘ring-fenced’ public funds for supporting research into herbal medicine. Research that emerges from initiatives funded by the National Institutes of Health is usually of outstanding methodological quality. Perhaps the UK authorities should consider this approach and develop a strategy along similar lines.
Product safety
From a clinical perspective, we need to consider not just efficacy but also (and perhaps foremost) safety (Box 1). Consumers often assume herbal medicines to be safe; a survey conducted in Israel, for instance, showed that 56% of them believed they cause no side-effects at all (Reference Giveon, Liberman and KlangGiveon et al, 2004). Unfortunately, this is not true. Most herbal remedies have been associated with (usually mild and transient) adverse effects (Reference Ernst, Dukes and AronsonErnst, 2000). In addition, a systematic review showed that herbal medicines taken for non-psychiatric indications can cause psychiatric adverse effects, including delirium, coma, confusion, hallucinations, mood disturbances and seizures (Reference ErnstErnst, 2003). Research also confirms that many herbal medicines have the potential to interact with prescribed drugs (Box 2). The notion that ‘natural’ equals ‘safe’ can therefore be dangerously misleading.
Box 1 Major safety issues with herbal medicine
-
• Inherent toxicity (e.g. liver damage after kava intake)
-
• Contamination (e.g. heavy metals in Ayurvedic preparations)
-
• Adulterations (e.g. sildenafil in herbal aphrodisiacs)
-
• Interactions (e.g. St John's wort lowers the plasma level of about half of prescription drugs)
Box 2 Examples of interactions between herbal and synthetic medicines
-
• St John's wort can increase the effects of conventional SSRIs
-
• Kava can interact with levodopa and alprazolam, causing extrapyramidal symptoms or lethargy
-
• Valerian can interact with loperamide and fluoxetine, causing delirium
-
• Evening primrose oil can interact with phenothiazide, causing epileptic seizures
In conclusion, the scientific knowledge about the potential benefits or harms of herbal treatments for anxiety or depression is incomplete and the information patients receive can be highly misleading. Psychiatrists should be aware of the essential facts and advise their patients accordingly.
Declaration of interest
None.
MCQs
-
1 In 1999 the total annual expenditure for complementary therapies in the UK was estimated to be:
-
a £16 billion
-
b £ 1.6 billion
-
c £ 1.6 million
-
d £ 0.16 million
-
e £160 billion.
-
-
2 The number of websites currently informing patients about ‘alternative medicine’ is about:
-
a 40 thousand
-
b 4 million
-
c 4 thousand
-
d 40 million
-
e 400 million.
-
-
3 Efficacy of St John's wort is best documented for:
-
a insomnia
-
b anxiety
-
c depression
-
d hay fever
-
e none of the above.
-
-
4 Kava, used for anxiety, is associated with:
-
a memory loss
-
b liver problems
-
c kidney problems
-
d gastrointestinal problems
-
e impaired vision.
-
-
5 The hypothesis that ‘natural’ equals ‘safe’:
-
a is biologically plausible
-
b is false and misleading
-
c is a well-established fact
-
d is the subject of current research
-
e was first advanced by Samuel Hahnemann.
-
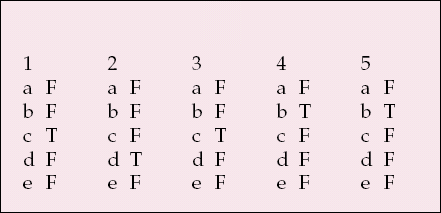
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| A | F | a | F | a | F | a | F | a | F |
| b | F | b | F | b | F | b | T | b | T |
| c | T | c | F | c | T | c | F | c | F |
| d | F | d | T | d | F | d | F | d | F |
| e | F | e | F | e | F | e | F | e | F |







eLetters
No eLetters have been published for this article.