LEARNING OBJECTIVES
-
Understand best primary care practice in the management of depression and related disorders, unexplained physical symptoms, severe and enduring mental illness, and dementia
-
Understand the implications for secondary care of best primary care practice in these areas
-
Appreciate the expanding role of primary mental healthcare in LMIC, and how this interacts with psychiatric services
Since my previous contribution to BJPsych Advances (Reference DowrickDowrick 2001), there has been substantial expansion of high-quality research into the management of mental health problems in primary care. There has also been substantial expansion of the need for effective primary mental healthcare. The global economic crisis of 2008 and subsequent austerity measures in many Western countries have increased pressure on specialist mental health services. Hence there is now greater emphasis than ever on the importance of providing timely, high-quality services in primary care for people experiencing mental health problems.
This article provides an update on evidence for best practice in primary care management of three mental health problems experienced by adults: depression and related disorders, unexplained physical symptoms and severe and enduring mental illness. It also considers the emerging role of primary care in the management of dementia, and draws attention to the expansion of primary mental healthcare in low- and middle-income countries (LMIC).
Hope and a positive way forward
Before considering the management of these specific conditions, it is important to note the fundamental importance of the primary care consultation itself. The most common but perhaps least recognised way in which primary care practitioners alleviate the mental health problems presented by their patients is by acknowledging the reality of their experiences and offering them hope of an alternative. Box 1 gives an example of an experienced general practitioner (GP) shaping the narrative of a patient with depression related to muscular dystrophy, by reversing the patient's metaphor of their condition being ‘on top of them’: although accepting that the muscular dystrophy is not going to improve, this gives the patient room to hope that their reactions to it may change for the better.
GPs can be adept at identifying a patient's understanding of their problems and working with them to shape an explanatory framework which provides the possibility of a positive way forward (Reference Cape, Geyer and BarkerCape 2010; Reference Karasz, Dowrick and ByngKarasz 2012). This fundamental set of skills should not be forgotten when considering the range of specific management options available to primary care practitioners working with patients with psychiatric conditions.
BOX 1 Example of general practitioner (GP) shaping a patient's narrative

| Patient: | ‘…It's [muscular dystrophy] just quite painful and tiring and depressing.’ |
| GP: | ‘Yeah, yeah.’ |
| Patient: | ‘… and I've been really cold since I came back, just can't seem to get warm so it's just very diff-, very depressing. Sorry [laughs].’ |
| GP: | ‘It's not easy to put up with, this, is it? (no) You're obviously somebody, you like to keep very active and getting around the place and doing what you want to do.’ |
| Patient: | ‘I just don't want it to be on top of me (yes) and it feels like it's on top of me.’ |
| GP: | ‘We've got to reverse that, haven't we? We can't get rid of the (no) dystrophy, but you can be on top of it rather than the other way (yeah), rather than the other way round somehow.’ |
(Reproduced with permission from Reference Cape, Geyer and BarkerCape 2010)
Depression and related disorders
Depression, anxiety and related disorders are commonly diagnosed in primary care. There is increasing recognition of the relationship between the depressive symptoms and the presence of chronic physical problems, which may be mediated via self-perceived health-related quality of life (Reference Gunn, Ayton and DensleyGunn 2012). Patients’ ratings of their health are an independent predictor of prognosis for depression. Patients with depression who rate their health as fair or poor are more than twice as likely to still have depression 5 years later, compared with patients with depression who rate their health as good to excellent (Reference Ambresin, Chondros and DowrickAmbresin 2014).
Primary care practitioners now have a wide variety of options available to help patients manage these conditions.
Antidepressant medication
The prevalence of depression in Western societies is static, yet rates of prescribing antidepressant medication have risen markedly in primary care. Although this may in part be due to better recognition of psychiatric disorders, it is more likely to be the result of overprescription. About 11% of the US population aged over 11 now take an antidepressant, including 23% of women in their 40s and 50s. In England, antidepressant prescribing increased by over 10% each year between 1998 and 2010, mainly due to an increase in long-term prescriptions (Reference Dowrick and FrancesDowrick 2013a).
The weight of evidence from meta-analyses of placebo-controlled trials is that antidepressant drugs have little or no effect in mild depression. They should be reserved for moderate and particularly for severe depression, where evidence of benefit is strongest. They should also be used in combination with psychosocial interventions, unless patients indicate a clear preference otherwise (Reference Dowrick and FrancesDowrick 2013a).
When choosing the most appropriate antidepressant, it is important to consider the balance of clinical benefits, side-effects and costs. A meta-analysis by Reference Cipriani, Furukawa and SalantiCipriani et al (2009) concluded that sertraline has the most favourable balance between benefits, acceptability and acquisition costs. Clinical guidelines recommend that medication be continued for 6 months after remission of symptoms, then tapered and stopped. Long-term antidepressant prescription should be considered if a patient has three or more depressive episodes (National Institute for Health and Care Excellence 2009a).
Current research is focused on improved targeting of antidepressant medication with respect in particular to the severity and duration of illness, and into effective methods of enabling the discontinuation of long-term medication where there is no evidence of continuing benefit.
Non-medical interventions
There is expanding evidence of effectiveness for a wide variety of non-medical interventions for depression and related disorders, to which GPs and other primary care practitioners should have access (Box 2).
BOX 2 Non-medical interventions for depression and related disorders
-
Psychosocial therapies
-
Cognitive–behavioural therapy
-
Interpersonal therapy
-
Problem-solving treatment
-
Behavioural activation
-
-
Mindfulness
-
Exercise
-
Personal resilience
-
Smoking cessation
Psychosocial therapies
Psychosocial therapies such as cognitive–behavioural therapy (CBT), interpersonal therapy, problem-solving treatment and behavioural activation have robust evidence of effectiveness across the range of common mental disorders (Reference Nieuwsma, Trivedi and McDuffieNieuwsma 2012; Reference Ekers, Webster and van StratenEkers 2014). Among these, problem-solving treatment and behavioural activation are most readily applicable by GPs and other practitioners working in primary care. The basic elements of problem-solving treatment were outlined in my previous article (Reference DowrickDowrick 2001) and key aspects of behavioural activation are presented here. The goal of behavioural activation is to enable patients to regain lost or reduced functionality. It focuses on helping patients in three key domains: increasing routine activities, increasing pleasurable activities and addressing necessary issues such as unpaid bills. The four essential steps are to record current activity, list things the patient would like to do, order these lists and then plan how to start doing them (Box 3).
BOX 3 The four key steps in behavioural activation
-
1 Record in a diary what you are doing now on a daily basis
-
2 Make lists of routine, pleasurable and necessary things that you would like to do
-
3 Order these separate lists into one big list:
-
most difficult activities at the top
-
easier activities at the bottom
-
mix routine, pleasurable and necessary activities
-
-
4 Create a diary sheet to plan how to start doing these things
The combination of psychosocial therapies and antidepressant medication is superior to antidepressant medication alone for the treatment of major depression, panic disorder and obsessive–compulsive disorder. A meta-analysis of 52 studies found a moderately large and clinically meaningful difference in favour of combined treatment, corresponding to a number needed to treat of 4.2 (Reference Cuijpers, Sijbrandij and KooleCuijpers 2014). For the long-term treatment of major depression, psychosocial interventions may be more effective than antidepressant medication (Reference Karyotaki, Smit and CuijpersKaryotaki 2014).
GPs can also advise patients to make use of self-help and internet-guided psychosocial interventions such as MoodGYM (https://moodgym.anu.edu.au) or Beating the Blues (www.beatingtheblues.co.uk). These have medium to large effect sizes, which are comparable to face-to-face treatments when accompanied by sufficient guidance (Reference DowrickDowrick 2015).
Meditation
Meditation programmes such as mindfulness enable us to be fully in the present moment, accepting emotions, thoughts and sensations without judgement or evaluation, and without trying to avoid or solve problems. They are now readily accessible in most Western countries and are also available online, for example through the mindfulness programme Headspace (www.headspace.com). Meditation can reduce multiple negative dimensions of psychological stress. Reference Goyal, Singh and SibingaGoyal et al (2014) conducted a systematic review and meta-analysis of 47 trials and found moderate evidence of improvement in anxiety, depression and pain-related symptoms. Mindfulness-based cognitive therapy is as effective as antidepressant medication in reducing the risk of relapse in recurrent depression (Reference Kuyken, Hayes and BarrettKuyken 2015).
Exercise
Exercise such as gym workouts, running, swimming and (for older people) walking and gardening appears to be more effective than control treatments in reducing symptoms of depression, and to have similar benefits to psychotherapy and pharmacotherapy (Reference Cooney, Dwan and GreigCooney 2013). However, there are relatively few high-quality studies of exercise as an intervention for depression, and not all demonstrate positive effects (Reference Chalder, Wiles and CampbellChalder 2012).
Personal resilience
There is preliminary evidence from observational studies of the benefits of encouraging personal resilience in reducing the symptoms of depression. These include taking steps to build personal strengths and expand positive emotions, for example through physical activity, yoga or productive work (Reference Griffiths FE Boardman and ChondrosGriffiths 2015).
Smoking cessation
GPs frequently advise patients about smoking cessation. There is now good evidence that this is associated with reduced depression, anxiety and stress, and improved positive mood and quality of life compared with continuing to smoke. The effect size of smoking cessation is equal to or larger than antidepressant treatment for mood and anxiety disorders (Reference Taylor, McNeill and GirlingTaylor 2014).
Collaborative care
Collaborative care for depression is a multifaceted organisational intervention which typically includes three components (Reference Bower, Gilbody and RichardsBower 2006):
-
1 introduction of a new role (case manager) into primary care, to assist in the management of patients with depression through structured and systematic delivery of interventions;
-
2 introduction of mechanisms to foster closer liaison between primary care clinicians and mental health specialists (including case managers) around individual patient care;
-
3 introduction of mechanisms to collect and share information on the progress of individual patients.
Collaborative care is beneficial, although effect sizes may not be as great as suggested by the original US-based studies. A collaborative stepped-care intervention led by lay health counsellors for patients with common mental disorders was trialled in Goa, India: there were strong benefits for patients attending public facilities, although not for those attending private clinics (Reference Patel, Weiss and ChowdharyPatel 2010).
The Clinical and Cost Effectiveness of Collaborative Care for Depression in UK Primary Care Trial (CADET) was a UK-based study which involved a combination of case manager coordinated support and brief psychological treatment, together with enhanced specialist and GP communication. This trial found small but persistent positive effects up to 12 months, clear patient preference for collaborative care, and health gains achieved at relatively low cost (Reference Richards, Hill and GaskRichards 2013).
Collaborative care that includes psychological treatment, with or without antidepressant medication, improves depression more than care without psychological treatment. Trials that use systematic methods to identify patients with depression, and include patients with a chronic physical condition, report improved use of antidepressant medication (Reference Coventry, Hudson and KontopantelisCoventry 2014). For common mental health problems in marginalised groups, such as elders or people from minority ethnic communities, collaboration between primary care and local community organisations improves both access and outcomes of care (Reference Dowrick, Chew-Graham and LovellDowrick 2013b).
The majority of the evidence in this section is readily applicable to the primary care management of depression in the context of chronic physical conditions. The National Institute for Health and Care Excellence (NICE) guideline on this topic gives more specific information (NICE 2009b).
Unexplained physical symptoms
Unexplained physical symptoms, or medically unexplained symptoms (MUS), are those for which doctors cannot find any disease or problem in the body that would account for them. They are presented in up to a quarter of primary care consultations.
My previous review (Reference DowrickDowrick 2001) suggested that enhanced or structured primary care, for example training GPs in the process of reattributing physical symptoms to a psychological cause, may be promising interventions. However, more recent evidence indicates that such reattribution is often unnecessary, and that enhanced care models such as reattribution may be too simplistic in their current form to address the needs of many people presenting with MUS in primary care (Reference Gask, Dowrick and SalmonGask 2011; Reference Rosendal, Blankenstein and MorrissRosendal 2013).
So what should GPs do? The primary care consultation is best seen as a conversation and ongoing negotiation between doctor and patient, in which there are no certainties about the presence or absence of organic pathology. GPs can have a positive effect on patients with MUS by taking their problems seriously, helping them to manage symptoms and improve functionality, offering continuity of care and being reassuring, though honest about uncertainties (Box 4).
BOX 4 Key elements in managing patients with unexplained physical symptoms
People want to be taken seriously – show you believe them:
-
ask yourself and the patient ‘Am I hearing and understanding what you are trying to tell me?’
Doctors can make a difference to the patient's well-being even when their symptoms are unexplained:
-
concentrate on helping to manage symptoms and improve functionality
Sometimes the only ‘therapy’ needed may be the strength of your doctor–patient relationship – continuity of care and the long-term relationship helps:
-
be pre-emptively reassuring, yet show you have an open mind and will continue to reassess
-
explain rather than just ‘normalise’
Be explicit about your thoughts, your uncertainties and your expectations of referrals to specialist care:
-
proactively communicate with other clinicians
(Reproduced with permission from Reference Chitnis, Dowrick and ByngChitnis 2011)
There is preliminary evidence of benefit from a dedicated primary care symptoms clinic, in which a GP with a special interest in MUS sees patients for a set of structured longer appointments (Reference Burton, Weller and MarsdenBurton 2012). GPs should also consider seeking additional help for patients with persistent MUS. A systematic review by Reference Van Dessel, Den Boeft and van der WoudenVan Dessel et al (2014) found psychological therapies such as CBT to be superior to usual care or waiting list in terms of reduction of symptom severity, although effect sizes were small. Psychological therapies generally were of similar efficacy to enhanced or structured primary care. Compared with pure GP training, a collaborative group intervention involving GPs and patients with MUS can achieve a progressive, clinically meaningful improvement in mental quality of life (Reference Schaefert, Kaufmann and WildSchaefert 2013).
Severe and enduring mental illness
The emphasis in primary care management of severe and enduring mental illnesses such as schizophrenia or bipolar disorder is on working in partnership with specialist care, with a focus on the physical aspects or sequelae of the psychiatric illness.
GPs need to consider the consequences of lack of self-care which affect lifestyle, smoking, obesity and (in younger patients) substance misuse, and lead to an increased risk of cardiovascular and respiratory diseases. In combination these problems lead to a life expectancy of about 20% lower than in the general population (Reference Crawford, Jayakumar and LemmeyCrawford 2014). GPs also need to consider the side-effects of psychiatric treatment. For common second-generation antipsychotics such as clozapine and olanzapine there is an increased risk of weight gain and reduced insulin sensitivity, leading to diabetes and the possible emergence of tardive dyskinesia in the longer term.
NICE guidance states that GPs and other primary care professionals should monitor the physical health of people with certain types of mental health problems including schizophrenia, bipolar disorder and psychosis at least once a year. The list of parameters to be monitored in primary care according to the Quality Outcomes Framework (a method of monitoring performance used in UK primary care; http://bma.org.uk/qofguidance) is summarised in Box 5.
BOX 5 Annual primary care health checks for patients with severe and enduring mental illness (SEMI)
All patients with SEMI:
-
alcohol consumption
-
smoking habits
-
body mass index
-
blood pressure
-
lipids, glucose/glycosylated haemoglobin
-
cervical screening (for women)
Bipolar disorder:
-
thyroid-stimulating hormone and creatinine
-
lithium therapy in range
Multidisciplinary approaches can help to bridge the gap between mental and physical health. Community psychiatric nurses have an important role to play in liaison between psychiatric and primary care teams, which is becoming easier as mental health teams are increasingly based in the community. In London, the Well-Being Support Programme led by nurses provides a care system whereby physical problems are identified and appropriate treatment and monitoring initiated by prompt referral to suitable specialist services or GPs. Other problems such as unhealthy lifestyles and obesity are managed by the nurse advisor running the programme. Interventions such as weight counselling/groups and structured exercise programmes are beneficial in terms of encouraging healthier lifestyles, managing obesity and improving self-esteem (Reference Ohlsen, Peacock and SmithOhlsen 2005).
Dementia
The diagnosis and management of dementia have become significant elements of the primary care role in recent times. GPs need to be aware of the complex and uncertain links between general cognitive decline and dementia, their role in the assessment of patients with dementia, and the potential benefits of collaborative care programmes.
Assessment
Cognitive decline and mild cognitive impairment (MCI) have important implications for patients and their families and require clinicians to be skilled in identifying and managing this common disorder. The diagnosis of dementia is a shared responsibility between generalist and specialist disciplines. GPs should explore patients’ ideas and concerns about their symptoms prior to referral and tentatively discuss possible diagnoses. Current evidence supports aerobic exercise, mental activity and cardiovascular risk factor control in reducing the risk of progression for patients with MCI, but there is no indication for nutritional or pharmacological interventions (Reference Langa and LevineLanga 2014).
Clinical data usually collected on medical history by primary care practitioners are useful in identifying patients with MCI and dementia and also in predicting MCI outcome. Independent predictors of progression from MCI to Alzheimer's disease include being female, resisting help, becoming upset when separated from a caregiver, difficulty shopping alone, forgetting appointments, number of words recalled from a ten-word list, orientation and difficulty drawing a clock (Reference Lee, Ritchie and YaffeLee 2014).
Principles of management
Once the diagnosis has been confirmed, the GP should provide both practical and emotional support to allow the patient and their family to come to terms with living with dementia, and refer them for additional psychosocial support if required. Practitioners, patients and their families need to consider pathways through diagnosis, including: its impact on identity, roles and relationships; the resolution of conflicts to accommodate a diagnosis, including the acceptability of support, and the use or avoidance of knowledge; and strategies and support to minimise the impact of dementia (Reference Iliffe, Robinson and BrayneIliffe 2009; Reference Bunn, Goodman and SwornBunn 2012).
Caring for people with dementia in primary care demands the same systematic approach as the management of other long-term conditions. The systematic follow-up of both the person and their carers should be integrated into primary care. Reframing dementia – with an emphasis on abilities retained – may allow patients and their families to develop more effective coping strategies. It can also improve the management of behavioural problems (Reference Robinson, Iliffe and BrayneRobinson 2010).
Annual dementia review, as supported by the Quality Outcomes Framework in Britain, provides an important opportunity for primary care teams to enhance the quality of care for people living with dementia, especially if linked systematically with reviews of depression and of medication for cognitive and psychotic symptoms (Reference Connolly, Iliffe and GaehlConnolly 2012). An important element of the review is discussion with carers about their support needs. A template for undertaking the review is presented in Box 6.
BOX 6 Template for annual dementia review in primary care
Conduct an annual face-to-face review with the patient and carer
Focus on the support needs of both patient and carer and record in the patient notes key problems that are addressed
Components of the review
-
Social care review
-
Mental health review, including consideration of depression, with:
-
a depression screen for patients with diabetes and/or coronary heart disease
-
an assessment of severity for newly diagnosed depression
-
-
4 Medication review
-
review of antipsychotic medication
-
for patients with Alzheimer's disease, a check of eligibility to receive medication to slow cognitive decline
-
review of medication for cognitive and non-cognitive symptoms
-
-
5 A talk with the carer, including discussion of any information they need, their health, their social care needs and the impact of being a caregiver
Case management
The benefits of collaborative care have already been noted in the management of depression in primary care. Similar processes have also been tested in dementia care, on the assumption that case management offers a way of coordinating services for people with dementia along the care pathway and therefore can provide them with individualised support. However, evidence for effectiveness in dementia is not yet available in UK primary care settings.
The CAREDEM study
In the Collaborative cARE for people with DEMentia in primary care (CAREDEM) study (Reference Karyotaki, Smit and CuijpersIliffe 2014), case management was tested in four volunteer general practices for its acceptability to key stakeholders (patients, carers and professionals) and its feasibility for use in UK primary care. Two practices seconded one of their practice nurses to the case management project for one session per week. The other two had access to a full-time social worker seconded from local authority adult services. People with dementia were identified from practice dementia registers. Case managers were asked to document their needs assessments and any subsequent action taken. A specialist community nurse provided regular mentoring for the case managers, visiting the practices as needed.
People with dementia and their carers were positive about the intervention, although the direct benefits to them during the short duration of the study were limited. Stakeholders identified a range of potential benefits of case management, but only one of the four practices achieved a level of case management activity likely to have an effect on outcomes for people with dementia or their carers. Barriers to effective case management included: erosion of case manager time by other clinical tasks in practices in which nurses fulfilled the role; difficulties in identifying and acting on ‘low level’ unmet needs; a lack of clarity over case management; poor integration with local services; and a lack of embeddedness within the primary care team.
The CAREDEM study team concluded that the skills and attributes that appear to be needed for potentially effective case management for people with dementia are not widely available in the existing primary care workforce. Different approaches to recruiting and training case managers, and to identifying people with dementia who might benefit from case management, are needed (Reference Karyotaki, Smit and CuijpersIliffe 2014).
Primary mental healthcare in low- and middle-income countries
World Health Organization and the World Organization of Family Doctors
The World Health Organization (WHO) and the World Organization of Family Doctors (WONCA) are actively collaborating to enhance the role of primary care in the provision of mental health services in LMIC. This is part of a global policy initiative to reduce the emphasis on institutional provision of psychiatric services and enable much greater access to community-based care.
A joint report (World Health Organization 2008) shows through detailed examples of best practice from 12 nations that, even though the current provision of mental health in primary care is globally insufficient and unsatisfactory, integration can be successfully achieved in a variety of socioeconomic contexts. Although mental disorders represent 13% of the total burden of disease, the gap between the number of people affected and the number receiving care and treatment, even for severe conditions, remains enormous. Data presented in the report show that up to 75 to 86% of people with severe mental disorders in LMIC had received no treatment in the previous 12 months.
The report also outlines ten broad principles to guide countries in their efforts to successfully integrate mental health into primary care (Box 7). These principles have been derived from an in-depth analysis of the best practices, and range from clear policy directions and resource allocation at national level through to local-level commitment and capacity building on the ground.
BOX 7 Ten principles for integrating mental health into primary care
-
1 Policy and plans need to incorporate primary care for mental health
-
2 Advocacy is required to shift attitudes and behaviour
-
3 Adequate training of primary care workers is required
-
4 Primary care tasks must be limited and doable
-
5 Specialist mental health professionals and facilities must be available to support primary care
-
6 Patients must have access to essential psychotropic medications in primary care
-
7 Integration is a process, not an event
-
8 A mental health service coordinator is crucial
-
9 Collaboration with other government non-health sectors, non-governmental organisations, village and community health workers, and volunteers is required
-
10 Financial and human resources are needed
WHO Mental Health Gap Action Programme
The WHO Mental Health Gap Action Programme (mhGAP) aims at scaling up services for mental, neurological and substance use disorders for LMIC. The programme asserts that with proper care, psychosocial assistance and medication, tens of millions of people could be treated for depression, schizophrenia and epilepsy, prevented from suicide and begin to lead normal lives: even where resources are scarce. Information and training resources are available to help reduce the mental health treatment gap and enhance the capacity of LMIC to respond to the large burden of mental, neurological and substance use disorders (World Health Organization Mental Health Gap Action Programme 2014).
Conclusions
This article has updated and extended evidence of best practice in primary care for the management of a range of mental health problems. The focus has been on high-income countries, but readers are also reminded of the need to be cognisant of different issues arising in LMIC.
It is hoped that the information provided here will be of benefit to psychiatrists as they seek to improve the care of their own patients. There is increasing synergy between primary and secondary care in the mental health field, and an enhanced understanding of what primary care is capable of should enable psychiatrists to plan how best to develop and integrate effective care pathways.
It should not be assumed that such developments will always be straightforward. First, health systems operate differently in different countries, even within the sphere of ‘advanced Western medicine’ and the prominence and influence of primary care can vary markedly. Second, best practice – for example in the field of collaborative care for depression or regular review of patients with dementia – may not yet exist in many settings. Finally, the effects of austerity are as likely to be noted in primary care as they are in specialist settings, such that even those keen to achieve excellence may be hampered from so doing. Nevertheless, an awareness of what is possible provides a basis for dialogue between psychiatric and primary care colleagues, and a platform on which both can act as advocates for change.
MCQs
Select the single best option for each question stem
-
1 When considering antidepressant medication in the treatment of depressive disorders:
-
a sertraline is a cost-effective option
-
b antidepressants are the first-choice treatment for mild depression
-
c antidepressants are more effective alone than in combination with psychotherapy
-
d long-term treatment should be considered after one depressive episode
-
e adherence is not improved by collaborative care.
-
-
2 When considering non-medical interventions for depression and related disorders:
-
a behavioural activation is an ineffective intervention
-
b internet-based or self-help options should be avoided
-
c mindfulness meditation is less effective than antidepressant medication in reducing relapse of depressive disorders
-
d exercise is always beneficial
-
e smoking cessation is associated with reduction in symptoms of anxiety and depression.
-
-
3 In the management of MUS:
-
a reattribution of physical symptoms to psychological causes is always necessary
-
b it is always important to take patients’ symptoms seriously
-
c continuity of care makes little difference
-
d structured symptoms clinics are unhelpful
-
e collaborative group interventions are less effective than structured GP care.
-
-
4 Patients with severe and enduring mental illness:
-
a have a similar life expectancy to the general population
-
b the GP's main role is to initiate prescription of antipsychotic medication
-
c GPs have an important role in managing the physical sequelae of the illness and its treatment
-
d GPs should check patients’ body mass index and blood pressure every month
-
e nurses do not provide effective liaison between psychiatrists and GPs.
-
-
5 In the primary care management of patients with dementia:
-
a routine history-taking is of no value in enabling GPs to identify patients at risk of dementia
-
b reframing diagnoses in terms of abilities retained has no impact on patients’ behaviour
-
c annual review need not consider the needs of carers
-
d annual review should include screening for depression
-
e case management has been demonstrated to be an effective intervention in the UK.
-
MCQ answers
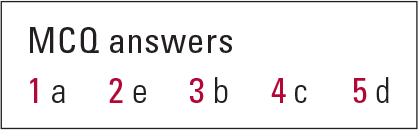
| 1 | a | 2 | e | 3 | b | 4 | c | 5 | d |






eLetters
No eLetters have been published for this article.