Despite the fact that suicide and its prevention continues to be a priority area for health care in the UK, suicide in the elderly remains a neglected subject receiving little interest and research attention. The Green Paper Our Healthier Nation (Secretary of State for Health, 1998) maintained the concept of setting targets for suicide reduction originally proposed in The Health of the Nation strategy. The new target proposes that by the year 2010 the death rate from suicide and undetermined injury will be reduced by at least a further sixth (17%) from the baseline of 1996. The setting of such targets has always been a contentious issue among many psychiatrists, who have concerns that they may be used as a quality measure of psychiatric services, especially as some consider that social influences predominate over health care issues. The subsequent debate has focused on targeting specific at-risk groups, notably severely mentally ill young men, Asian women and those who deliberately harm themselves.
One group who are rarely considered in such debates is the elderly. This is a matter of particular concern given the importance of psychiatric and physical health factors, which previous and recent research continue to emphasise. Fundamentally, suicide rates in most industrialised nations increase with age, the highest rates of all occurring in elderly men. The notion that most elderly suicides are ‘rational’ acts in response to irreversible, understandable situations is not supported by available clinical research. Suicidal behaviour in the elderly is undertaken with greater intent and with greater lethality than in younger age groups, and health care staff play a vital role in the recognition and prevention of suicide in this age group. This paper deals principally with completed suicide in the elderly, although attempted suicide and related issues are included where relevant for emphasis. The epidemiological, social, neurobiological, psychiatric and physical antecedents will be discussed, followed by a consideration of preventive measures.
The few comprehensive studies into elderly suicide employ a method known as ‘psychological autopsy’, which generally involves establishing a detailed profile of the mental state, personal circumstances and concerns of the person before suicide through structured interviews with surviving relatives, friends, etc., supplemented by additional information from primary and secondary care services where relevant (Reference Barraclough, Bunch and NelsonBarraclough et al, 1974; Reference Conwell, Olsen and CaineConwell et al, 1991, Reference Conwell, Olsen and Caine1996; Reference Rich, Young and FowlerRich et al, 1986; Reference Henriksson, Marttunen and IsometsaHenriksson et al, 1995). As suicide is a relatively rare event, these studies are limited in size. Larger samples may be analysed using information obtained from coroners’ inquests and other sources. Several studies have focused specifically on the elderly in recent years (Reference CattellCattell, 1988; Reference Cattell and JolleyCattell & Jolley 1995; Reference Duckworth and McBrideDuckworth & McBride, 1996; Reference Osuna, Perez-Carceles and ConejeroOsuna et al, 1997; Reference Purcell, Thrush and BlanchettePurcell et al, 1999).
Epidemiology
Suicide rates
Males aged 75 and over have the highest rates of suicide in nearly all industrialised countries, and among many of these nations suicide rates rise with age. However, many countries have recorded a decline in rates among the elderly in recent years. In England and Wales between 1983 and 1995, suicide rates for men decreased by between 30 and 40% in the age groups 55–64, 65–74 and 75–84 (Reference Kelly and BuntingKelly & Bunting, 1998). Rates for the most elderly men (males over 85 years) during this period remained fairly static, this group still having the highest rates of any group (see Box 1). In contrast, the 25- to 34-year-old male group exhibited a 30% rise between 1983 and 1995 and are becoming the group with the second highest rate, while the 15- to 24-year-old male group demonstrated a 55% increase over the same period. Female suicide rates have shown a similar overall decrease, falling by between 45 and 60% during the years 1983–1995 in the 45–84 age group. Elderly women, however, retain the highest rates throughout the life span. The ratio of male to female elderly suicide deaths remains around 3:1. Cross-cultural differences clearly influence suicide rates. For example, in the UK, rates in elderly first-generation immigrants from the Indian subcontinent are low compared with the indigenous elderly population (Reference Raleigh, Bulusu and BalarajanRaleigh et al, 1990). Nationwide analysis may also obscure local variations, as demonstrated in a recent study from a deprived inner-city area where rates among young White men exceeded those among elderly men (Reference Neeleman, Mak and WesselyNeeleman et al, 1997). In the USA, the highest suicide rates occur among elderly White men, although rates among Black men are higher in younger age groups.
Box 1. Risk factors for elderly suicide
Older age
Male gender
Living alone
Bereavement (especially in men)
Psychiatric illness
Depression
Alcohol misuse
Previous suicide attempt
Vulnerable personality traits
Physical illness
Pain
Method of suicide
The method of suicide employed varies over time, with age, gender and sociocultural factors. It is a general principle that elderly men adopt more violent methods than women, which may partially explain the gender difference in rates. In England and Wales, hanging currently remains the most common method employed by men, while self-poisoning is most often used by women. In the USA, firearms are used by over 60% of all completed suicides, with elderly White men employing this method most frequently.
Neurobiology
The concept of suicidal behaviour as a distinct neurobiological entity has been investigated over the past few decades in the search to identify potential biological markers. These studies have been undertaken almost exclusively on a younger population with the elderly receiving scant attention. This may be partially attributable to the inherent and often contradictory data on the effect of ageing on central nervous system neurotransmitter systems. The most consistent findings in the biology of suicidal behaviour suggest dysregulation of the serotonergic system, shown by reductions in brain-stem cerebrospinal fluid (CSF) 5-hydroxyindoleacetic acid (5-HIAA) evident on post-mortem studies of suicide victims. Low CSF 5-HIAA and homovanillic acid (HVA) have been reported as having predictive value in determining further suicide attempts after a failed attempt. More recent studies have focused on platelet type 2 serotonin receptor (5-HT2) increases being found among suicidal patients, independent of psychiatric diagnosis. Seemingly, only one study has focused on biological markers in the suicidal elderly, finding significantly lower concentrations of CSF 5-HIAA and HVA in suicidal patients compared with non-suicidal and normal controls (Reference Jones, Stanley and MannJones et al, 1990).
Social factors
The role of social isolation as a risk factor for elderly suicide has been stressed in earlier studies. Barraclough (1971), for example, cites living alone as the most important social variable. Subsequent studies have found the association to be less significant and several have found no difference between living alone and number of social contacts compared with younger suicides (Reference Carney, Rich and BurkeCarney et al, 1994; Reference Heikkinen and LonnqvistHeikkinen & Lonnqvist, 1995). The general conclusion is, however, that social isolation and loneliness are important contributors. The antecedents in terms of precipitating life events appear to be different in the elderly population compared with younger and middle-age groups. The latter are associated more closely with interpersonal and relationship problems, financial, legal and occupational difficulties, and less with physical illnesses and other losses. The role of bereavement does appear to be a significant influence, with studies of completed and attempted suicide citing its relevance. Elderly men seem especially vulnerable – one study reports a relative risk for widowed men being over three times that of married elderly males, whereas widowed and married elderly women showed similar risk (Reference GuohuaGuohua, 1995). The first year of widowhood seems to be a vulnerable period.
With regard to marital status, widowed, single or divorced people seem to be more at risk, while marriage appears to be a protective factor. The great majority of suicides occur in a community setting, usually in the individual's home. The relatively small number of in-patient suicides do not show the expected rise in rate with age (Reference Shah and DeShah & De, 1998).
Psychiatric illness
Comprehensive studies are consistent in showing very high levels of psychiatric disorder – around 90% – in suicides of all ages, and the elderly are no exception. Among the elderly, however, depressive illness is the most important predictor of suicide and this needs to be emphasised. Most comprehensive studies in elderly suicide employing the psychological autopsy method report the prevalence of major depression and other mood disorders to be between 60 and 90%. Barraclough's classic study (1971) demonstrated a prevalence of affective disorder of 87% in his sample of 30 over-65-year-olds, and this finding has provided ample support for the primacy of depressive illness in subsequent research. Conwell et al (1996), examining the relationship of age and Axis 1 diagnoses in a sample of 141 completed suicides aged between 21 and 92 years, found 71% and 64% of the 75- to 92- and 55- to 74-year-old cohorts, respectively, to exhibit mood disorders, compared with 30% of the 21- to 34-year-old group. Major depression was diagnosed in almost 60% of the most elderly suicides, with other mood disorders accounting for between 10 and 20% of the sample in this study. The elderly sample constituted the most homogeneous group in which non-affective psychoses were rare, addictive disorders less common and late-onset major depression the rule.
The symptom profiles of elderly suicides with depression are uncommonly described but are likely to be important in determining specific at-risk presentations. Barraclough's study (1971) reported complaints of insomnia (90%), weight loss (75%), guilt feelings (50%) and hypochondriasis (50%) (see Box 2). Elderly people with depression are less likely to complain of depersonalisation, loss of libido and suicidal feelings compared with younger sufferers, and this indicates the importance of enquiry into the presence of suicidal ideation. There is no substance to the idea that such enquiries precipitate suicidal acts and most patients are grateful for this kind of discussion as such ideas often generate feelings of guilt. The importance of assessing depth of hopelessness is equally relevant in the elderly as in younger individuals, and particular attention should be given to a person's attitudes and values, especially in the face of loss events.
Box 2. Prominent symptoms prior to elderly suicide
Insomnia
Weight loss
Guilt feelings
Hypochondriasis
A number of studies have examined the prevalence of suicidal thoughts in the elderly population. Skoog et al (1996) examined the prevalence of suicidal feelings in a population of mentaly healthy 85-year-olds and found that none had seriously considered suicide and only 4% felt that life was not worth living or wished they were dead. The presence of mental disorder, however, was strongly correlated with suicidal feelings, especially major depression, with nearly 30% expressing pessimistic thoughts and death wishes. Forsell et al (1997) in a study of nearly 1000 over-75-year-olds found that 50% of those who had frequent suicidal thoughts were exhibiting features of major depression. The conclusion from both these studies was similar, notably that suicidal thoughts are strongly associated with the presence of depressive disorder and that a careful psychiatric assessment that is focused particularly on the possibility of depression is essential before any rational basis for suicidal thoughts is considered.
Primary substance use disorders account for a smaller proportion of suicides than in younger age groups, with prevalence estimates ranging between 5 and 40%. Similarly, non-affective psychoses are uncommonly reported compared with younger suicides. The role of medicines of potential misuse contributing to suicide in the elderly should not, however, be underestimated. For example, in a recent study from Honolulu analysing 96 elderly suicides via screening of coroners’ inquest reports (Reference Purcell, Thrush and BlanchettePurcell et al, 1999), of those where toxicological screening was done at the time of death, over 54% revealed alcohol or potentially habituating substance misuse on post-mortem.
Although well-established dementia is likely to be a protective factor against suicide, the significance of an early dementing illness is a matter of speculation receiving scant attention. For some individuals, the fear of dependency and the concept of ending one's life in an ‘institution’ is an important dynamic, irrespective of the presence of cognitive deficits.
The role of personality in elderly suicide also has a small literature base. Using the NEO-Personality inventory, Duberstein (1995) reported a lower openness to experience (OTE) score in elderly suicides compared with younger suicide victims and normal controls. The low OTE profile may be summarised as a cognitive propensity to perceive problems in dichotomous, black and white terms, a rigidly defined self-concept and a diminished behavioural repertoire, thus decreasing the capacity to adapt to loss and change.
Attempted suicide should always be taken seriously in the elderly and is most likely to represent a failed bid. It is associated with high rates of depression (up to 90%), with major depression accounting for over 50% and physical illness being a significant contributor in around 60–70% of cases (Reference DraperDraper, 1996). Attempts in the elderly are a much stronger predictor of subsequent completed suicide compared with attempts in younger people, with a ratio of attempts to completion estimated to be around 4:1 compared with between 8 and 200:1 for young people who attempt suicide. The profile of elderly people who attempt suicide (more so than in other age groups) resembles that of those who complete, and suicidal intent scores are reported to be at their highest (Reference Merrill and OwensMerrill & Owens, 1990).
Physical illness
The association of complaints of physical ill health as a major antecedent in the study of elderly suicide has long been emphasised and distinguishes elderly suicides from younger cases, in which the prevalence of physical ill health is substantially less prevalent. Several early studies reported medical illness directly contributing to suicide in around 60–70% of elderly suicides, with evidence of higher rates of physical illness among elderly male suicides compared with females. Heikkinnen & Lonnqvist (1995) emphasise the importance of physical illnesses as a life event in the three months prior to death in elderly men. Elderly males display an excess of serious somatic illness compared with elderly females (55 v. 31%) suggesting that there are gender differences in coping with such age-normative stressors. In other studies, the relevance of ill health as a risk factor is reflected in associated findings. Cattell & Jolley (1995), for example, reported that within the 12 months preceding suicide, 23% of a series of 100 consecutive elderly suicides had been hospitalised for the investigation and treatment of physical disorders. Elwood & De Silva (1998), in a study of 67 subjects who had made contact with general hospital services but were unknown to psychiatric services, found the elderly to be over-represented. Out of the nine completed suicides who had received hospital care in the month prior to death, eight were over 65 years old.
A number of specific central nervous system and systemic disorders have been linked with increased risk of suicide. These include epilepsy, multiple sclerosis, Huntington's chorea, head injury, peptic ulcer and rheumatoid arthritis. The association of suicide with cancer is inconsistent, with several studies supporting such an association, while others refute the risk, especially in hospitalised patients. Duckworth & McBride (1996), in a Canadian study of 543 elderly suicides using coroners’ inquest data, reported that those with medical illnesses were significantly less likely to receive a psychiatric referral than those without a medical illness, and the discrepancies in referral patterns were even greater for those patients with cancer. In this study, patients with terminal illness, which in the sample comprised almost 9% of the total, were least likely of all to be referred for psychiatric assessment. The subjective reporting of pain symptoms prior to suicide would appear a fairly consistent finding and is worthy of emphasis. For example, in the Honolulu study (Reference Purcell, Thrush and BlanchettePurcell et al, 1999), upon retrospective analysis of 96 elderly suicides, 42% reported pain complaints, with nearly 20% indicating it to be a major concern prior to death.
The lesson to be learnt is that the presence of physical illness should not detract from a close examination of the mental state with particular regard to a coexistent depressive illness and associated suicidal feelings. Hypochondriacal and somatic symptoms may mask the underlying depression and there is some evidence that this symptom profile may particularly predispose to suicide. This form of presentation of depression may be of particular importance in elderly men, who may be less likely to verbalise depressed mood or admit to suicidal thoughts. Suicidal ideation and pessimistic thoughts are not uncommon among acutely medically ill and continuing-care geriatric in-patients, necessitating the training of staff in these facilities in the recognition and treatment of underlying disorders (Reference Shah, Dighe-Deo and ChapmanShah et al, 1998)
These general findings for completed suicide have their parallel in findings from studies of elderly people who attempted suicide. Hepple & Quinton (1997), for example, found 53% of a series of 100 consecutive people who attempted suicide to be suffering from significant physical illness at index assessment following the attempt. Follow-up data revealed a mortality from natural causes of 8.6% per year, representing an increase of 1.6:1 compared with the age- and gender-matched population. In this study, after an average of three and a half years, 42% of the original subjects had died.
Prevention
Risk assessment
An act of suicide is a complex phenomenon involving multiple psychological, physical and social factors operating at a crucial moment in the life of a vulnerable individual, and any risk assessment needs to reflect these varied antecedents. A typical high-risk individual may be described as an elderly male, living alone following recent bereavement, who may have coexistent painful, chronic health problems. He may have made serious previous suicide attempts and be currently depressed.
The main difficulty in applying risk factors lies in the generation of high false-positive predictions associated with the relatively low base rate of completed suicide, and as yet no instruments have been developed with adequate sensitivity and specificity to be clinically useful as a risk assessment scale in the elderly. It is the clinical interview that remains the cornerstone of such assessment and needs to clarify key variables. There is some evidence that elderly suicides are less likely to express suicidal intent compared with their younger counterparts, raising issues around the detection of the suicidal elderly being a more difficult task than detection in younger people (Reference Carney, Rich and BurkeCarney et al, 1994). Protective factors are often overlooked in elderly suicide research, but clinical experience suggests that relevant factors may be concern over the impact of suicide on family members and a belief in the sanctity of life.
Availability of lethal methods
Reducing the availability of means of suicide as a preventive strategy has been advocated as an important strategic initiative. This is perhaps best exemplified by the significant reduction in the elderly suicide rate following the detoxification of the domestic gas supply in the 1960s. Contemporary means of restricting availability include the employment of catalytic converters to car exhaust emissions, reduced availability of firearms, limitation of paracetamol via over-the-counter sales, and alterations in prescribing habits for older antidepressants.
Service provision
Primary care services
The role of primary care services in suicide prevention is of considerable interest. Most studies report substantial levels of contact: 40–70% of elderly suicides seeing their general practitioner (GP) in the 30 days preceding their death, and between 20 and 50% attending in the preceding week. This raises the important issue of effective intervention at a time when the individual is particularly vulnerable. The importance of training and education programmes for GPs in the recognition and treatment of depression as a means of reducing the suicide rate arises from the Gotland Study conducted by Rutz et al (1989). In the year following training (1983–1984), suicide rates on the island fell significantly compared with other parts of Sweden, and the fall was accounted for largely by the proportion of suicides with major depression. Although not specific to the elderly, such research requires replication (see Box 3).
Box 3. Strategies for suicide prevention in the elderly
Recognition and treatment of psychiatric disorders, especially depression, in both primary and secondary care settings
Development of community-based outreach services
Public health initiatives to reduce availability of lethal methods
Secondary care services
Research evidence also suggests that a minority of elderly suicides have been in contact with secondary psychiatric services prior to their death. The Report of the Confidential Inquiry into Homicides and Suicides by Mentally Ill People (Steering Committee, 1996) documented the original scrutiny of 240 suicides known to be in contact with psychiatric services between June 1993 and December 1994 and revealed that in England a total of 54 (22.5%) were aged over 60 years, with men accounting for 54% of this cohort.
Cattell & Jolley (1995) reported that 20% of their series had contact within six months and 14% within one month. Osuna et al (1997) reported on a large elderly series from Madrid and found similar results of 16% and nearly 10%, respectively. Recent data from the National Confidential Inquiry, however, reported essentially similar findings for the general population, with 24% having been in contact with psychiatric services in the preceding 12 months (Reference Appleby, Shaw and AmosAppleby et al, 1999). The Inquiry also highlighted the greatest risk occurring in the week following discharge for former in-patients, although whether this also applies specifically to the elderly awaits confirmation. These findings emphasise the importance of community outreach services, especially as the elderly may be more susceptible to social isolation and both objective and subjective loneliness. It is important to realise that around 30–60% of suicides have no contact with medical services prior to their death, despite the high prevalence of psychiatric disorder.
Treatment adequacy
Despite the importance of depressive illness in elderly suicide, most studies report substantially inadequate or inappropriate use of antidepressant medication prior to death. Conwell (1997) described the recognition and treatment of psychiatric symptoms in primary care settings for 51 elderly suicides and found only two who had received adequate treatment, with men and those with coexistent physical illness presenting the greatest challenge. Information from several inquest studies shows low antidepressant treatment levels of around 10–25% (Reference CattellCattell, 1988; Reference Cattell and JolleyCattell & Jolley 1995; Reference Duckworth and McBrideDuckworth & McBride, 1996), although a more optimistic finding has been reported from Sweden where 50% of a cohort of 75 elderly suicides had a documented history of treatment for affective disorder in the six months prior to death (Waern et al, 1966).
Preventive strategies
Strategies for the prevention of elderly suicide have been recently reviewed from an international perspective (Reference Pearson, Conwell and LindesayPearson et al, 1997). It would be fair to say that there are limited data on the effectiveness of specific assertive outreach programmes targeting the elderly, although some encouraging initiatives have been described. DeLeo et al (1995) describe a Tele-Help/Tele-Check service for a population of 12 000 over-65-year-olds in Padua, Italy. The service provides active contacts to clients by trained staff giving information, support and prompt intervention in medical and psychological emergencies. After four years of this service, only one suicide was reported, which was significantly lower than expected.
In the USA, the Gatekeepers Program of Spokane, Washington, addresses the need to contact non-self-referrals by training business personnel in the recognition and referral to health professionals of elderly distressed individuals. Such personnel include apartment managers, pharmacists, meter readers, etc. In the UK, the implementation of screening policies for the elderly, the development of community-based old age psychiatry services maintaining close links with primary care facilities, improved education and liaison links with general hospital services, and local and national audit programmes are likely to be useful.
Conclusion
Although suicide and its prevention remain a significant public health concern, suicide in the elderly still receives little focus in terms of specific preventive strategies or research. This is unfortunate given the established evidence that elderly suicide rates are among the highest, and are in turn more closely related to serious mental illness (especially major depressive illness) and significant physical health problems than in any other group. The situation is compounded by the failed recognition and failed treatment of those elderly who come into contact with services. Fundamental to this process is the need to educate health professionals and society in general that the act of suicide in late life is rarely a rational act or an unavoidable tragedy.
Multiple choice questions
-
1. Suicide rates among the elderly in England and Wales:
-
a have shown an overall decline in recent years
-
b remain at their highest in the most elderly men
-
c are higher in men compared with women
-
d are the highest among psychiatric in-patient suicides
-
e fell significantly following the detoxification of the domestic gas supply.
-
-
2. Regarding the sociodemographics of elderly suicide:
-
a in UK males, hanging is the most common method
-
b living alone is an important contributor
-
c suicidal thought is a common phenomenon in elderly people not suffering from depression
-
d bereaved men are at increased risk compared with bereaved women
-
e interpersonal discord and financial worries are the most typical stressful life events leading to suicide.
-
-
3. In relation to psychiatric illness:
-
a major depression and other mood disorders are found in between 60 and 90% of elderly suicides
-
b primary substance use disorders account for as many suicides in elderly as in younger groups
-
c hypochondriasis and insomnia are common clinical symptoms preceding suicide
-
d suicide attempts are associated with a lower degree of intent in the elderly
-
e attempts are a stronger predictor of successful suicide than they are in younger people.
-
-
4. Regarding physical illness:
-
a physical ill health is more important in elderly suicide
-
b subjective reporting of pain is not a finding associated with elderly suicide
-
c hospitalisation for physical ill health prior to suicide is rare
-
d somatic symptoms of depression are often overlooked as manifestations of physical illness
-
e increased risk of suicide has been associated with Huntington's chorea, multiple sclerosis and epilepsy.
-
-
5. Regarding preventive strategies in elderly suicides:
-
a contact with primary care services is rarely made in the preceding month
-
b the majority have received adequate antidepressant therapy prior to death
-
c limiting access to lethal methods may reduce rates
-
d evaluation of community outreach initiatives has found no benefit
-
e Our Healthier Nation targets the reduction of suicide by a further 17% by the year 2010.
-
MCQ answers
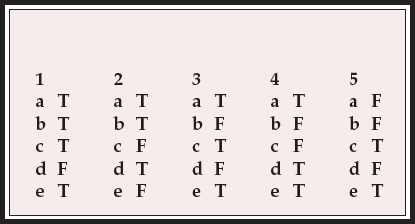
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | T | a | T | a | T | a | F |
| b | T | b | T | b | F | b | F | b | F |
| c | T | c | F | c | T | c | F | c | T |
| d | F | d | T | d | F | d | T | d | F |
| e | T | e | F | e | T | e | T | e | T |





eLetters
No eLetters have been published for this article.