There is a current gap in the nomenclature of psychiatric in-patient services. There are few descriptions of types of in-patient care and over recent years the literature has abounded with debates concerning alternatives. However, it may be argued that these debates have been based on the creation of the ‘straw man’ of the psychiatric admission, which is only fit for knocking down. Although a post-war consensus has emerged concerning the need to abandon the Victorian asylums, this has often been misrepresented as the need to avoid in-patient admission. The poorly articulated and emotional concept of community care and its lack of clear and consistent definition in public policy and key legislation have contributed to this (Reference BulmerBulmer, 1987). Recent changes in our view of community care have led to a refining of the concept and a shift from its comforting appellations (Reference Titmus and TitmusTitmus, 1968) to a pragmatic approach that matches it to empirical experiences and new resources. This approach sees psychiatric services for adults as being based locally and provided by a spectrum of services – in-patient, residential and ambulatory (Department of Health, 1996) – based on best available evidence. This article has been written with these issues in mind. We will address the current problems of in-patient care and the current literature on alternatives and supplements to traditional in-patient units.
Psychiatric in-patient care in the UK
Psychiatric in-patient care in the 20th century has been associated with large Victorian asylums and, latterly, with district general hospital (DGH) units. The Victorian hospitals reached their peak occupancy in the mid-1950s and had become associated with overcrowding, remoteness from local communities, poor-quality care and scandals. The advent of the National Health Service (NHS) gave psychiatric patients the same admission status as others, and acute in-patient units in DGHs were created in the 1960s. Urged by successive government policies there has been a reduction in psychiatric beds in England and Wales and, more recently, the successful closure of many of the large asylums. In real terms, these bed losses have been mainly those occupied by ‘long-stay’ patients and the number of acute admission beds has remained relatively constant. These changes have often not been balanced by the development of adequate community-based services (including residential services) and have occurred at the same time as rapid social changes such as an increasing diversity of social groups, widespread drug misuse and heightened public expectations. The result of this for in-patient units has been an accumulation of younger long-term patients and an increasing demand for acute beds in the context of decreasing quality of the ward environment and staff demoralisation.
The ‘bed crisis’
There has been an increase in emergency admissions across the entire NHS (Reference CapewellCapewell, 1996) and in psychiatry this has been particularly evident in London (MILMIS Project Group, 1995). This increased demand for psychiatric beds, compounded by a decrease in bed numbers, has led to over-occupancy, an increased use of extra-contractual referrals and an accumulation of difficult and disturbed patients on acute wards. Issues such as over-occupancy are not confined to London (Reference Hodgson and BoardmanHodgson & Boardman, 1996a ) and it is recognised that the quality of care provided in acute units often falls below acceptable standards (Sainsbury Centre for Mental Health, 1998). The rising demand for acute beds is exacerbated by an accumulation of patients on acute wards who block further admissions. Many of these patients constitute the ‘new long-stay’ who make a considerable contribution to the overall lengths of stay of patients on acute wards (Reference Lelliott and WingLelliott & Wing, 1994; Reference Shepherd, Beadsmoore and MooreShepherd et al, 1997). A significant number of admissions could be avoided if suitable alternatives were available, and many patients with prolonged stays could be discharged if appropriate community and residential options existed (Reference Beck, Croudace and SinghBeck et al, 1997; Reference Shepherd, Beadsmoore and MooreShepherd et al, 1997).
Solutions to the bed crisis
Underlying these problems with acute psychiatric services are a variety of factors that reflect both the supply and the demand sides of the equation (Reference Shepherd, Beadsmoore and MooreShepherd et al, 1997). As a result, there is no single solution but there is an increasing recognition of the need to provide a spectrum of care in which both residential and non-residential options are available (Reference Davies, Presilla and StrathdeeDavies et al, 1994; Department of Health, 1996; Reference Shepherd, Beadsmoore and MooreShepherd et al, 1997; NHS Executive, 1996). Attempts to deliver quality services outside these traditional settings have led to innovations in service delivery. Some alternatives have been identified and evaluated and there is an increasing literature on home-based treatments (Reference Marshall and LockwoodMarshall & Lockwood, 1999). The desire to provide alternatives to acute psychiatric ward care has been driven by both social and economic considerations. For example, the need for non-hospital-based acute care has been highlighted by user and advocacy groups (Reference Davies, Presilla and StrathdeeDavies et al, 1994). The Government has also issued guidance to purchasers on the range of settings for treatment and social care (Department of Health, 1996). Nevertheless, there is a gap in the British literature in reporting alternatives or supplements to traditional acute hospital care or home-based treatment. Finding a Place, the Audit Commission's analysis of mental health (Audit Commission, 1994), recommends that traditional hospital care is reviewed with resources redirected towards community care and alternative accommodation services. However, there is a vagueness regarding these alternatives and a lack of references. The NHS Executive (1996) publication, 24 Hour Nursed Care for People with Severe and Enduring Mental Illness, details service specifications but lacks any reference to previous evaluations of such units. The Sainsbury Centre (1998) report pointed out the need to overhaul the care and amenities on acute wards, to improve staffing loads and training, to examine bed management methods and to view acute 24-hour care as one component of a comprehensive and integrated service. There is little evaluative work on residential alternatives or supplements to acute in-patient care (Reference Davies, Presilla and StrathdeeDavies et al, 1994; Reference HollowayHolloway, 1997).
Alternatives to psychiatric in-patient care
There are currently several alternatives to the traditional acute ward (Box 1). The most obvious alternative to hospital-based care is care in the patient's own home, and successful home treatment initiatives have been described and evaluated (Reference Marshall and LockwoodMarshall & Lockwood, 1999). One aspect of home treatment is the use of foster families. This is not a new treatment as families in Gheel, Belgium, have taken mentally ill people into their homes for over 600 years (Reference AiringAiring, 1974) and the mentally ill were also managed in alternative accommodation in this country (Reference AllderidgeAllderidge, 1979). There can be pitfalls with these arrangements, including the emergence of high expressed emotion and attitudes in the foster family. In a crisis, these families need intensive and continuing professional support. A rigorous screening process for potential foster families is also necessary.
Box 1. Alternatives to the traditional acute ward
Home treatment
Foster families
Crisis houses
Halfway hospital
Day hospital
Hostel
Morgan (1993) advocates the development of crisis houses that should be in the form of ordinary housing with stays varying from “a few days up to a few months”. He envisages this accommodation having a number of roles in addition to being a direct alternative to acute hospital admission. These include transfer from an acute ward before final discharge, crisis intervention and as a trial base for people considering independent accommodation. Whether all these roles are complementary is debatable and little is mentioned regarding staffing, admission criteria and support services.
Crisis housing has been evaluated in the USA and Stroul (1988) has suggested five criteria that this type of service should meet:
-
• they provide housing during a crisis
-
• their services are short-term
-
• they provide acute treatment and support services
-
• they serve individuals or small groups of clients
-
• they are used to avoid hospitalisation.
Bond et al (1989) compared two crisis-housing alternatives in Chicago. One programme met crisis-housing needs by purchasing accommodation in hotels and boarding houses, and the other had a dedicated eight-bed crisis house. Patients were referred by hospital after emergency-room screening. It appears that some patients were admitted to hospital for up to three days prior to their transfer. The emphasis was on a cost outcome, which revealed no significant difference. No clinical ratings were made and the re-hospitalisation rates were the same in the two groups. Patients in the boarding house/hotel programme showed an increase in substance misuse problems. The authors also noted a high staff turnover in the crisis house and suggest that this may be a result of the stressful nature and undesirable hours of the work.
A crisis unit within a state hospital has been described by Ash & Galletly (1997). This four-bed unit treated 14% of all patients admitted to the hospital. Three-quarters of patients were discharged directly back to the community and the average length of stay was three days. Only 18% of patients were re-admitted within the following six months. Most patients were suffering from either adjustment reactions or personality disorders.
Other models also exist in the USA. For example, in San Francisco (Reference Molzen, Gurevitz and RapaportMolzen et al, 1987) acute treatment is provided in a 6–50-bed non-hospital setting with variable staffing. Some of these places are in institutional settings with high rates of detained patients. Nevertheless, clinical outcomes equal to traditional acute ward care are achieved at a 40% cost saving. Sledge et al (1996) compared acute respite and day hospital care with in-patient care. The study was of a random controlled design and confined to voluntary patients, 197 of whom were recruited and followed-up for 10 months. There were no statistical differences between the groups in clinical and social outcomes, although, overall, the day hospital/respite care group had the more positive outcome. This option was cheaper, especially for patients not suffering from psychosis.
The Department of Health (1975) advocated the development of hospital hostels and defined their characteristics and numbers. It was thought that 4–6 places would be required per 100 000 population, depending on deprivation. In addition, hospital hostels should combine the clinical expertise and back-up of hospital resources with a domestic environment. This means high staffing levels, intensive professional input, and individualised programmes in a setting that is non-institutional, ‘homely’ and allows access to local facilities.
The Maudsley pioneered the first hospital hostel in 1977 (Reference Wykes and WingWykes, 1982). It consisted of a Victorian house that faced the main road but remained on hospital grounds. Places for 14 residents were provided in seven double rooms. The emphasis was on fostering a non-institutional environment and independence for the residents. Subsequent hospital hostel developments described in the literature have invariably had a primary focus of rehabilitation for patients with severe and enduring illness (Reference Goldberg, Bridges and CooperGoldberg et al, 1985).
Supplementing acute in-patient care
Rationale for development of community in-patient units and halfway hospitals
Day patient and home-based treatments do not fulfil the needs of all patients, with most treatment studies reporting a significant rate of hospitalisation (Reference Marshall and LockwoodMarshall & Lockwood, 1999). In-patient care is indicated for many patients who lack community support, lack housing or are precariously housed. The nature and severity of a person's illness also influences the need for admission. Acute in-patient units face two types of pressure: first, the pressure of demand for admission. As discussed in the introduction, the decline in psychiatric bed numbers and subsequent over-occupancy (Reference Hodgson and BoardmanHodgson & Boardman, 1996a ,Reference Hodgson and Boardman b ) often militates against admission and, if admitted, the patient may encounter a structural and therapeutic environment of poor quality. The second pressure is that of discharge; the demand pressures mean that patients may be prematurely discharged to make way for new admissions and thus it may not be possible to adequately plan after-care arrangements and transfer back to the community teams – elements of good practice covered by the Care Programme Approach. As a result, the long-term needs of patients may not be adequately met (Sainsbury Centre for Mental Health, 1998). The divide between in-patient units and community teams may result in a ‘treatment gap’ between hospital and community services.
The Nottingham Acute Bed Survey (Reference Beck, Croudace and SinghBeck et al, 1997) identified patients who, while requiring admission, did not need acute ward care and also highlighted patients who needed continuing stays on non-acute wards. The authors identified the need for beds that would:
“…provide a service for patients who required admission, but not at the high intensity of supervision and care that an acute ward provides, or a ‘step down’ support facility between the acute ward and the environment. Such a facility would allow for the care of patients in need of respite and recuperation in a therapeutic environment away from patients with acute psychotic illness”.
Little is currently known about this type of unit – three have been documented in the literature and one has been evaluated. One of the authors (A.B.) runs a fourth such unit in North Southwark, in south-east London, about which nothing is currently published. There may be other such units but they are not known to the authors. There is currently no widely accepted name for these units but they may be referred to as ‘community in-patient units’ or ‘halfway hospitals’. In some ways, precedents have been set for the function of these units as it was often traditional in psychiatric hospitals to have wards into which patients were transferred after acute admission or for different lengths of stay. These new units may retain a similar function, but are differentiated by being based near to the community team and are not designed for long-stay care.
Examples
There are three published examples of such units (Reference Boardman, Hodgson and LewisBoardman et al, 1997; Reference Thomas, Greenwood and KearneyThomas et al, 1996; Reference Scott, Normanton and McKennaScott et al, 1992). The authors are not aware of other published accounts of similar units.
Thomas et al (1996) reported the characteristics of a community support bed unit serving an isolated rural community. The unit provides eight beds, serves a population of 33 100 and is geographically remote from the local DGH unit. It is designed to provide a local alternative to the DGH unit and was fully operational by the end of 1994. Owing to its relative isolation and levels of nursing support, patients with the following risk factors are not admitted:
-
• acute admission under 1983 Mental Health Act
-
• risk of harm to self or others
-
• serious physical health problems
-
• primary problem of learning disability or substance misuse.
In the 12 months prior to the community support bed unit opening, there were 116 admissions to the sector's DGH. In the 12 months after the unit opened, there were a total of 110 sector admissions, of which 54 entered the unit. Middle-aged patients and women were more frequently admitted to the community support bed unit. Patients with psychosis were more likely to be admitted to the DGH unit but this was not statistically significant. However, from the information provided, it would appear that most patients suffering from an acute psychotic disorder were not admitted to the community support bed unit, which catered for planned admissions. In conclusion, the authors believed that the unit offered patients “more choice about where and when they received help”.
Scott et al (1992) describe an “admission facility” in north-east England that is not based on a hospital site. Patients are admitted to the unit for the following reasons:
“to treat those in acute, severe crisis; to provide an alternative setting when family or social networks are unable to cope and to offer ‘asylum’ to those in need of brief respite”.
This four-bed in-patient unit treats 76 patients a year (14% of all patients admitted to hospital) and emphasises integration with the day hospital and other community services. The average length of stay is three days. When 78 crisis unit patients were studied, it appeared that 77% were discharged directly to the community and only 18% were readmitted within six months. The principal diagnosis was either adjustment disorder or personality disorder. Only 10% of patients were suffering from a psychosis. Patients admitted tend to be demanding and disruptive. Treatment contracts and firm limit-setting are integral to the management of patients. The authors believe that this unit prevents long stays in the main hospital.
North Staffordshire community in-patient units
Two community mental health centres (CMHCs), Lymebrook and The Sutherland Centre in North Staffordshire, have eight-bed units attached to them (Reference Boardman, Hodgson and LewisBoardman et al, 1997). Both CMHCs are purpose-built and were completed in 1991, with the in-patient units becoming fully operational during 1992. The units are situated in an annexe to the main centre and, as the buildings are single-story, have become known as ‘bungalows’, a description that emphasises their non-hospital setting. When conceived they were known as ‘PIR beds’ as they were intended to be used for prevention of relapse, intervention following early relapse and respite care. The resulting acronym is useful in understanding their use, but subsequent development has resulted in a considerable overlap between these functions. The key features are listed in Box 2.
Box 2. Key functions of community in-patient units and halfway hospitals
‘Step-down’ from traditional acute ward
Rehabilitation
Integration into after-care prior to discharge
Brief crisis interventions
Brief assessments
Initiation of clozapine or change of medication
Respite care
Each patient has his or her own room that contains a single bed, simple furniture, and a washbasin. There is also a communal kitchen, dining room and lounge. A ‘homely’ atmosphere is encouraged and the standard of decor is high, especially when compared with the acute admission wards. The philosophy of care for these beds emphasises the development of independent living skills and active involvement in appropriate day facility activities. Therefore, patients shop for and prepare their own meals, although there is a ‘cook–chill’ option on weekday lunchtimes. There is no full-time specific day care programme for bungalow patients, but they use the day centre facilities in the CMHC, which ensures they are integrated into their after-care arrangements prior to discharge.
The bungalows are staffed by two nurses at all times. These nurses come from the general pool of the CMHC's staff complement, so there are no specific bungalow staff as all staff rotate. Medical cover is provided by a five-session clinical assistant and the sector consultant. Out-of-hours cover is provided by local general practitioners or the on-call consultant. Therefore, admissions are only accepted during office hours. The bungalow can only accept patients who do not require a high level of nursing care. If problems arise, patients can be transferred back to the acute unit. In practice, this is usually because of a physical health problem. Although admissions are not accepted out of hours, patients and their relatives can contact the unit for advice and support.
Almost half of the patients admitted to the units are transferred from the acute patient wards, the remainder being directly admitted for respite, assessment or crisis prevention (Reference Boardman, Hodgson and LewisBoardman et al, 1997). All have a severe mental illness and the majority have a functional psychosis.
Evaluation of community in-patient units and halfway hospitals
To the authors’ knowledge, only one outcome study (Reference Boardman, Hodgson and LewisBoardman et al, 1999; Reference Haycox, Unsworth and AllenHaycox et al, 1999) has been undertaken. In North Staffordshire, the population of 460 000 is covered by six sectorised services. Patients admitted to the two sectors with the bungalow beds described above were compared with those admitted to two zones with similar populations, deprivation indices and treatment facilities. Baseline evaluations were undertaken using standardised instruments covering clinical variables, social function, quality of life, service satisfaction and carer involvement. These measures were repeated at six and 12 months. An economic evaluation was also completed (Reference Haycox, Unsworth and AllenHaycox et al, 1999).
The study involved 177 patients with severe mental illness. Overall, the patients using the community beds showed significantly better symptomatic and social behavioural outcomes, significant reduction in unmet need and reduced use of acute in-patient beds. Users’ satisfaction with services was much higher in those using the community beds services. The use of community beds appears to have significant benefits for patients with severe mental illness (Box 3). The bungalow beds were more expensive to operate, but this was not inevitable (Reference Haycox, Unsworth and AllenHaycox et al, 1999).
Box 3. North Staffordshire Community Beds Study – summary of results
The community beds arm of the study resulted in:
Better symptomatic outcomes
Better social behavioural outcomes
Better reduction in unmet needs
Better patient satisfaction
Longer overall lengths of stay
Shorter acute lengths of stay
Fewer acute readmissions
Patients more likely to remain in contact with services
Higher public sector costs
Higher overall costs may not be inevitable
Wykes (1995) has identified four components to the potential ‘toxicity of community care’: toxicity to patients, to their families, to the community or to staff. The results of the study demonstrate good outcomes for both patients and their families. No direct evaluation of staff was undertaken, although this was partially evaluated by Beech (1997), who found no evidence of high staff burnout rates. There is also no evidence that the bungalow beds adversely affect the local community.
Desirable features of community in-patient units and halfway hospitals
These units should be integrated with the community mental health team (CMHT), which in practice means that the CMHT and beds are housed in one multi-purpose building. This means that patients can be introduced to their after-care activities prior to discharge and, perhaps more importantly, meet members of the CMHT on a regular basis. Having seen the unit's activities, care is seamless and discharge does not result in any abrupt changes in the patients’ after-care, about which patients are able to make an informed decision – this underpins the philosophy of the Care Programme Approach. Patients have to negotiate many boundaries when transferred from hospital to the community and the effects this may have on adherence with subsequent treatment regimes.
Although integration with the rest of the CMHC's activities is important, the in-patient unit needs to have its own identity. This is achieved by ensuring that only in-patients use its sitting-room, kitchen, etc. Siting the in-patient unit in one self-contained annexe is important. There must also be activities that are specific to the in-patients’ needs and restricted to them. The unit's identity is enhanced by regular community meetings.
It is important that a unit is sited in the centre of its catchment populations and easily accessible by public transport. It should be within easy walking distance of shops as this facilitates many therapeutic and self-care activities. It should not be built on the site of a main psychiatric in-patient unit for a variety of practical and conceptual reasons. If the unit is on site, it is difficult to dispel the idea that it is just another ward, which dilutes the ethos of such units. It also identifies the unit with the local community. However, in North Staffordshire we have found that having one unit near a cottage hospital and the other on the site of a continuing care hospital for the elderly has had a number of advantages in the provision of support services without any major disadvantages. One unit is near a busy main road and this has caused some difficulties secondary to traffic noise.
Practical considerations
We have demonstrated that halfway hospitals can be effective and increase patient satisfaction, however, they cannot be considered as a viable option for all patients (Box 4). For example, some patients do not have the self-care skills or do not wish to be transferred. The number of beds available is the rate-limiting step, with about a fifth of patients who fulfil the criteria for a step-down admission having to remain on an acute ward. This has been a problem for the North Southwark unit in view of the high demand for acute beds in the inner city. Very few patients are thought to be unsuitable for the bungalow beds by staff. In general, these are patients who have active comorbid substance misuse problems or who are too disturbed and pose too high a risk in an isolated unit. In view of the relative isolation of these units, nursing staff are actively involved in the admission decision. But as experience has accumulated over the six years that the beds have been open, fewer patients are perceived to be unmanageable. An on-call response team has recently been developed to try to address the relative isolation of these units.
Box 4. Admission criteria for community in-patient units
Patient known to service
Low risk of self-harm behaviour
Low risk of harm to others
Low risk of absconding
High level of nursing observation not required
Absence of serious acute medical illness
Rudimentary self-care skills
Having the community in-patient units alongside the CMHC often means that staff have to work a shift system to staff the beds on a 24-hour basis. This can result in some disruption to day hospital activities when staff are rostered to night shifts. However, in-patients have the opportunity to meet the majority of the unit's staff during their stay. This has the advantage that if, post-discharge, patients’ keyworkers are unavailable, they are usually able to access a member of staff whom they know and who personally knows them. As a result of the unit being permanently staffed, a 24-hour helpline is available to patients known to the service.
Conclusions
In the UK, residential psychiatric care is slowly diversifying and alternatives to traditional hospital based-care are evolving. There is an increasing realisation that we need to provide a range of local services for people with mental illnesses that incorporates in-patient, residential and ambulatory options provided by secondary and primary health care, social services and voluntary sector organisations. In-patient care is a central part of this spectrum and it is unlikely that CMHTs can operate effectively without adequate in-patient provision and residential places. There is a need to critically examine the nature of our current in-patient care and to provide a range of facilities for those with severe and long-term mental illness that acknowledges the need for acute care, rehabilitation, respite, asylum and delivery of therapies. The supplements to in-patient care described here may contribute to this critical appraisal.
Multiple choice questions
-
1. Acording to Stroul (1988) crisis housing should:
-
a provide long-term care
-
b facilitate acute hospitalisation
-
c provide housing during a crisis
-
d accommodate a large number of residents in the same building
-
e not provide treatment.
-
-
2. The evaluation of psychiatric beds in North Staffordshire demonstrated that patients in the community beds arm of the study were:
-
a less likely to be readmitted
-
b more dissatisfied with their treatment
-
c more likely to have unmet needs at the end of the study period
-
d more costly to treat
-
e more likely to have a poor symptomatic outcome.
-
-
3. The following admission scenarios would preclude admission to North Staffordshire's community beds:
-
a detention under the 1983 Mental Health Act
-
b an admission occurring in the evening
-
c admission for respite care
-
d the direct admission of a patient new to the service
-
e a patient with an acute confusional state.
-
-
4. The following are accurate statements:
-
a the total number of psychiatric beds in England and Wales has fallen since 1955
-
b the total number of acute psychiatric beds in England and Wales has fallen since 1955
-
c no asylums have closed in England and Wales since 1980
-
d the Department of Health recommended that psychiatric care should be provided by a spectrum of services
-
e the occupancy of large asylums in England and Wales has fallen steadily since 1920.
-
MCQ answers
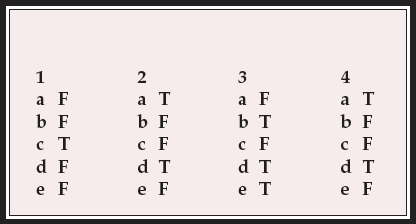
| 1 | 2 | 3 | 4 | ||||
|---|---|---|---|---|---|---|---|
| a | F | a | T | a | F | a | T |
| b | F | b | F | b | T | b | F |
| c | T | c | F | c | F | c | F |
| d | F | d | T | d | T | d | T |
| e | F | e | F | e | T | e | F |





eLetters
No eLetters have been published for this article.