Depression is a frequently occurring symptom in schizophrenia. While today it is often under-recognised and under-treated, historically such symptoms were the focus of much attention. Affective symptoms were used by Kraepelin as an important criterion with which to separate dementia praecox from manic–depressive illness. Kraepelin also recognised the importance of depression as a symptom in schizophrenia and identified several depressive subtypes of the illness. Mayer-Gross emphasised the despair that often occurs as a psychological reaction to acute psychotic episodes and Bleuler considered depression to be one of the core symptoms of schizophrenia.
Depressive symptoms in schizophrenia are important not only because they contribute significantly to the suffering caused by the illness, whether ‘positive’ psychotic symptoms are active or quiescent, but also because they exacerbate deficits in psychosocial functioning and commonly precede attempted and completed suicide. It is important to define and clinically assess such symptoms accurately as there is now increasing evidence that they can be treated successfully.
Differential diagnosis of depression in schizophrenia
There are a number of important differential diagnoses of depressive symptoms in schizophrenia. We can assume that depression and schizophrenia are not simply two independent illnesses occurring together by chance, on the basis of the epidemiology of each illness. Differential diagnoses to consider include schizoaffective disorder, organic conditions and the negative symptoms of schizophrenia. It has been argued by some that depression may in some way be ‘caused’ by antipsychotic medication and this issue will be discussed in detail. Depression may also be an understandable psychological reaction to schizophrenia. When all of these possibilities have been excluded, there is evidence that depression is perhaps most often an integral part of the schizophrenic process itself.
Schizoaffective disorder
Differentiating schizophrenia with clinically significant depressive symptoms from schizoaffective disorder is not always easy. Clearly, the exact dividing line between the two conditions is a conceptual one. Operationalised criteria such as ICD–10 (World Health Orgnization, 1992) allow us to make such a differentiation on a day-to-day basis (see Boxes 1 and 2) and will dictate treatment options to an extent. The nature and treatment of schizoaffective disorder falls outside the remit of this review.
Box 1. ICD–10 diagnostic guidelines for post-schizophrenic depression
The patient has met general criteria for schizophrenia within past 12 months
Some schizophrenic symptoms are still present, but no longer dominate the clinical picture (symptoms may be ‘positive’ or ‘negative’, though the latter are more common)
The depressive symptoms are prominent and distressing, fulfilling at least the criteria for a depressive episode, and have been present for at least two weeks (they are rarely sufficiently severe or extensive to meet criteria for a severe depressive episode)
Box 2. ICD–10 diagnostic guidelines for schizoaffective disorder – depressed type
Both definite schizophrenic and definite affective symptoms are prominent simultaneously, or within a few days of each other, within the same episode of illness
As a consequence of this, the episode of illness does not meet criteria for either schizophrenia or for a depressive or manic episode
There must be prominent depression accompanied by at least two characteristic depressive symptoms or associated behavioural abnormalities as for a depressive episode
At least one and preferably two typically schizophrenic symptoms, as specified for schizophrenia, must be present
Adjustment reactions
Schizophrenia carries a heavy psychological burden and it is not surprising that disappointment reactions to life's vicissitudes occur commonly. Acute reactions, lasting less than two weeks, are self-limiting and require supportive treatment or manipulation of the environment only. Often, a clear precipitating cause can be identified.
There are some patients who can be characterised as suffering from a demoralisation syndrome or a chronic disappointment reaction. Differentiating such a syndrome from depression is not always easy. It is characterised by hopelessness and helplessness, with a lack of confidence and feelings of incompetence. The appropriate treatment is supportive or rehabilitative rather than pharmacological.
Clearly, a reactive process cannot explain the majority of cases of depression in schizophrenia. If such a process, dependent to an extent on the return of insight, is at work, then depressive symptoms should become more common as acute psychotic symptoms respond to treatment. The opposite appears to be the case, however, with depressive symptoms more often resolving as positive symptoms resolve.
Organic factors
Depression-like syndromes can occur secondary to a range of medical conditions (Table 1). Neoplasms, anaemias, infections, neurological disorders and endocrine disorders can induce psychological symptoms directly in the person with schizophrenia, or depressive symptoms may occur as a reaction to illness. A myocardial infarction, for example, may present as agitation and emotional distress in someone with schizophrenia as there can be an altered pain threshold and inability to describe symptoms adequately. The medication used to treat medical disorders may also cause depressive symptoms as a side-effect. Antihypertensives, corticosteroids, anticonvulsants and L-dopa, among others, may give rise to problems. The medical history of any patient presenting with depressive symptoms should thus be carefully scrutinised. In addition, the entire range of medication that they receive, not just their psychotropic medication, and any recent changes in medication, should be considered as possible aetiological factors.
Substance misuse is also a common cause of depressive symptoms, either as a direct effect of the substance concerned or as a withdrawal phenomenon. Alcohol is undoubtedly the most common substance causing problems. Arguably, cannabis can cause depressive symptoms with long-term use, and nicotine and caffeine may cause dysphoria upon withdrawal. Cocaine, less commonly used and more often associated with manic symptoms, can cause depression upon withdrawal. The same applies to other psychostimulants (Table 1).
Differentiating depressive from negative symptoms
The ‘negative’ features of schizophrenia have many clinical similarities to the syndrome of depression. Lack of energy, anhedonia and social withdrawal may cause particular problems when attempting to differentiate between the two syndromes. Observed sadness is an unreliable indicator of depression in schizophrenia. Prominent subjectively low mood, suggesting depression, and prominent blunting of affect, suggesting negative symptoms, are the two features which are most helpful in differentiating the two syndromes (Reference SirisSiris, 1994). An emphasis on the patient's view of him- or herself may thus be a useful approach in detecting important aspects of depressive symptomatology in schizophrenia. Other symptoms that help to establish the diagnosis of depression include some of the main psychological features that occur in primary depressive illness, such as hopelessness, helplessness, worthlessness, guilt, anxiety and suicidal thinking. In schizophrenia, the biological features of the depressive syndrome, such as insomnia and retardation, are not always present – and if they are present, they can be more difficult to disentangle from negative symptoms and can be an intrinsic part of the illness separate from any superimposed depressive syndrome.
The role of antipsychotic medication
The role of antipsychotic medication in the aetiology of depressive symptoms in schizophrenia is somewhat controversial. There have been three principal proposed roles (Table 2).
Thirty years ago, it was proposed that antipsychotics acted directly causing ‘pharmacogenic depression’ (Reference De Alarcon and CarneyDe Alarcon & Carney, 1969). There is a possible theoretical explanation for this as antipsychotics act primarily on dopaminergic pathways and dopamine plays a major role in reward and pleasure mechanisms. An alternative hypothesis proposed that akinesia, an extrapyramidal side-effect of antipsychotic medication, and not necessarily accompanied by other symptoms, such as tremor, can mimic depression. This phenomenon has been termed ‘akinetic depression’ (Reference Van Putten and MayVan Putten & May, 1978). Patients behave ‘as if their starter motor is broken’ and display anergia and akinesia, sometimes with accompanying low mood. Van Putten & May considered this to be a new symptom of extrapyramidal disorder, not part of Parkinsonian syndrome. Whether it can be reliably differentiated from Parkinsonian syndrome and is in fact a separate clinical entity remains open to question.
Although some observations have supported these hypotheses, the weight of evidence has been against, suggesting that antipsychotics are responsible for relatively few cases of depression in schizophrenia. Depression can occur in antipsychotic-free patients with schizophrenia (Reference JohnsonJohnson, 1981a ), the prevalence of significant depression falls when antipsychotic treatment is commenced (Reference Hirsch, Jolley and BarnesHirsch et al, 1989) and when antipsychotics are discontinued there is an increase in the percentage of patients requiring antidepressants (Reference Hirsch, Gaind and RohdeHirsch et al, 1973). Several studies have shown no difference between depressed and non-depressed patients with schizophrenia in the dosage of antipsychotic medication received.
Johnson (1981b) estimated that ‘akinetic depression’ accounts for 10–15% of depressive-type symptoms. It is difficult to know how accurate this claim is, but akinetic depression should always be considered as a possibility and anticholinergics as a treatment option. Depressive symptoms are as common in patients on anticholinergics as in those who are not, and anticholinergics are not an effective treatment for depressive symptoms (Reference JohnsonJohnson, 1981a ).
More recently, attention has focused on the concept of antipsychotic-induced dysphoria. One study in normal volunteers (Reference King, Burke and LucasKing et al, 1995) demonstrated that dysphoria often occurs in the absence of motor restlessness and can thus be under-diagnosed. It is possible that some patients with schizophrenia presenting with depressive symptoms may in fact be troubled by antipsychotic-induced dysphoria, without the associated motor aspects of akathisia that make the diagnosis more obvious. If present, dysphoria/akathisia is not a trivial side-effect and has even been associated with suicide (Reference Drake and EhrlichDrake & Ehrlich, 1985).
Depression as a core symptom of schizophrenia
Although the above factors must always be considered, it is probably the case that the majority of patients with schizophrenia who also complain of significant depressive symptoms have these symptoms as an aspect of the illness process itself. Table 3 summarises the situations in which this occurs and the main approaches to management for these.
Depression as a prodromal syndrome
Depressive symptoms are common in the prodromal period prior to acute psychotic episodes. Herz & Melville (1980) found that the symptoms most frequently mentioned by patients and their families were:
“symptoms of dysphoria that non-psychotic individuals experience under stress, such as eating less, having trouble concentrating, having trouble sleeping, depression and seeing friends less”.
Indeed, depression, as described above, was described by 60% of patients and more than 75% of their relatives. Johnson et al's (1983) findings were less dramatic, with 20% of their cohort experiencing more prominent affective symptoms prior to relapse. The emergence of affective symptoms may represent a psychological reaction to impending relapse, may reflect an underlying biological process mediating both these symptoms and positive psychotic symptoms, or may be an epiphenomenon. In any event, newly emerging affective symptoms are a useful early warning sign of impending relapse.
Depressive symptoms during acute episodes
Depressive symptoms are most frequently associated with the acute phase of the illness. Such symptoms are most prevalent before medication is commenced (Reference Knights and HirschKnights & Hirsch, 1981) and occur in more than half of first-episode or drug-free patients (Reference JohnsonJohnson, 1981a ). The prevalence of depressive symptoms falls dramatically during the course of an admission for an acute relapse, and occurs in approximately 25% of patients during the six months following discharge. The close association between depressive symptoms and acute episodes adds weight to the hypotheses that such symptoms are a core feature of schizophrenia and suggests that depressive symptoms and more typically schizophrenic symptoms may share common pathophysiological processes.
Depressive symptoms in chronic schizophrenia
Lower rates of depressive symptoms are seen in the chronic phase of the illness with a range of 4–25% and an estimated mean of 15% (Reference Leff and DeLisiLeff, 1990). Most of the reported studies on chronic patients do not define the clinical stability or otherwise of the patients involved. In one study (Reference Pogue-Geile, Williams and DalbyPogue-Geile, 1989), only patients who were clinically stable (not hospitalised in the previous six months, no medication changes in previous six weeks and judged by their clinician to be stable) and who were living in the community were assessed, and 9% were found to be currently depressed. Persistent positive symptoms in the chronic phase of the illness may lead to distress, demoralisation and depression.
Post-psychotic depression
The occurrence of depressive symptoms during the chronic phase of schizophrenia has been given close attention in recent years. The terms ‘post-psychotic depression’, ‘post-schizophrenic depression’ and ‘secondary depression’ have been used to describe this phenomenon. Unfortunately, as Siris (1990) has argued, the term ‘post-psychotic depression’ has been used to describe three similar, but clinically distinct, groups of patients. In one group, depressive symptoms are clearly present during an acute psychotic episode and resolve as the positive psychotic symptoms resolve, although sometimes more slowly. These depressive symptoms only become apparent as the positive symptoms resolve, and the term ‘revealed depression’ is sometimes applied. The second definition overlaps somewhat with the first but describes patients who develop depressive symptoms as their positive psychotic symptoms resolve. The third group of patients are those in whom significant depressive symptoms appear after the acute episode has resolved. The multiplicity of terms and the different ways in which they have been used has not added to the clarity of the literature. The studies in this area have varied widely in methodology, including their definitions of significant depression.
The concept of post-schizophrenic (or post-psychotic) depression has now been incorporated into the ICD–10 (World Health Organization, 1992) classification system (and in the appendix of DSM–IV; American Psychiatric Association, 1994). ICD–10 offers an operationalised definition of post-schizophrenic depression (Box 1) and attempts to avoid confusion by specifically stating that it is immaterial to the diagnosis whether depressive symptoms have been revealed or are a new development, and it is similarly immaterial whether depression is an intrinsic part of schizophrenia or a psychological reaction to it.
Importance of depressive symptoms
Bleuler considered prominent affective symptoms to be a good prognostic sign in schizophrenia. This notion persisted for many decades despite the lack of good evidence to support it, and evidence to the contrary is now accumulating.
Depression is an associated risk factor for death by suicide in schizophrenia. Given that 10% of patients with schizophrenia end their own lives, this is of obvious importance. Patients who kill themselves are more likely to have a history of depressive episodes and to have exhibited depressive symptoms at their last contact. Suicide in schizophrenia appears to be correlated more with hopelessness and the psychological aspects of depression than with vegetative features (Reference Drake and CottonDrake & Cotton, 1986). Depression is also associated with attempted suicide (Reference PrasadPrasad, 1986).
Cheadle et al (1978) suggested that neurotic symptoms, many of them depressive in nature, are the principal symptoms causing distress to patients with chronic schizophrenia in the community. Johnson (1981a) found that over a two-year follow-up period the total morbidity from depression was more than twice the duration of morbidity from acute schizophrenic symptoms and that the risk of an episode of depression was over three times the risk of an acute schizophrenic relapse. Follow-up studies have shown that depression can be the main indication for 40% of admissions (Reference Falloon, Watt and ShepherdFalloon et al, 1978) and that patients who manifest post-psychotic depression are more likely to experience a psychotic relapse.
Glazer et al (1981) demonstated a link between depressive symptoms and poor performance in social roles, including difficulties in relationships with others. There also appears to be a correlation between post-psychotic depression and poor premorbid social adjustment and with insidious onset of the first psychotic episode.
Cause of depression in schizophrenia
The cause of depression, as a core symptom in schizophrenia, is not known. Interestingly, early parental loss is more common among patients with post-psychotic depression (Reference Roy, Thompson and KennedyRoy et al, 1983), as is a family history of affective disorder (Reference Subotnik, Nuechterlein and AsarnowSubotnik et al, 1997). Depressive symptoms are equally common in male and female patients (Reference Addington, Addington and PattenAddington et al, 1996). Recent work has shown an association between depressive symptoms and attentional impairment, suggesting frontal lobe dysfunction (Reference Kohler, Gur and SwansonKohler et al, 1998a ) and increased bilateral temporal lobe volumes and decreased laterality (Reference Kohler, Swanson and GurKohler et al, 1998b ). These findings among others suggest that the neurobiology of depressive symptoms in schizophrenia may have similarities with that of depressive illness itself. Further work is required to clarify the issue.
Treatment issues
The assessment and treatment of depressive symptoms in schizophrenia remains clinically challenging. Recent advances in psychopharmacology and other treatment approaches elevate the importance of establishing the diagnosis at an early stage. The therapeutic goal is significantly to reduce the excess morbidity and mortality associated with depressive symptoms.
The first steps are to exclude cases of schizoaffective disorder and to treat them appropiately, to treat any medical conditions that are present, and to consider the possibility of substance misuse as a contributing factor. Any evidence that antipsychotic medication is producing akinesia should lead to a reduction in dosage and/or the introduction of anticholinergic medication. Akathisia, with its concomitant feeling of dysphoria, should always be considered in patients describing subjective mood disturbance. The akathisia/dysphoria syndrome, if present, requires active management. Use of an anticholinergic drug is generally effective. Other options include β-adrenoceptor antagonists (e.g. propranolol), a benzodiazapine or a change in antipsychotic drug.
If the above factors have been addressed and the clinician is sure that negative symptoms are not being mistaken for depressive symptoms, then the treatment options are largely dictated by the stage of the illness.
An expectant approach, with increased psychosocial support, may be the way foward if emerging depressive symptoms are thought to herald an acute relapse. Clearly, antipsychotic medication should be introduced or increased if there is serious concern that an acute episode is developing. Indeed, follow-up studies indicate that early intervention at the first signs of relapse improves outcome (Reference Johnstone, Owens and GoldJohnstone et al, 1984).
During acute episodes, depressive symptoms should not be treated separately from other symptoms and are likely to resolve as the episode resolves. In the majority of cases increased antipsychotic medication, increased psychosocial support and, if necessary, hospitalisation, will successfully treat depression as well as positive symptoms.
There is accumulating evidence that the new atypical antipsychotics are more efficacious in treating the depression associated with an acute episode. Olanzapine, for example, was superior to haloperidol in this regard in a recent study (Reference Tollefson, Beasley and TranTollefson et al, 1997). Other atypicals, such as risperidone, ziprasidone and zotepine, may also have a mood-elevating effect. The atypicals may prove to be useful for the depression that emerges during the chronic phase of the illness. Clozapine has been shown to reduce hopelessness, depression and suicidality in people with chronic schizophrenia (Reference Meltzer and OkalyiMeltzer & Okalyi, 1995).
There is a good case for the prescription of an antidepressant when the patient has persistent depressive symptoms and is not in a phase of acute illness. There have been 11 published double-blind, placebo-controlled trials of tricyclic antidepressants. The results of these demonstrated improvement v. placebo in five, and no improvement in six. Unfortunately, these studies vary in patient selection criteria, particularly in relation to the patient's phase of illness, but the better-conducted trials tend to support a treatment effect (Reference PlaskyPlasky, 1991). A caveat with the tricyclics, however, is that occasionally there can be a worsening of the positive psychotic symptoms.
Clinical trials of selective serotonin reuptake inhibitors (SSRIs) have overall been in favour of an effect on depressive symptoms in schizophrenia. Some of the studies have focused more on negative symptoms and have not included patients with severe depressive symptoms. However, in general, patients seem to do better on an SSRI than with placebo. A recent study designed specifically to compare an SSRI with placebo in patients with schizophrenia with moderate or severe depression also found clear benefit (Reference Mulholland, Lynch and CooperMulholland et al, 1997). Given the relative safety of SSRIs compared with the tricyclics, they would seem to be the antidepressants of choice. However, it is necessary to bear in mind possible pharmacokinetic interactions with antipsychotics because of the enzyme inhibitory effects of some of the SSRIs on the CYP450 system.
Electroconvulsive therapy (ECT) was in earlier years often advocated for patients with schizophrenia experiencing prominent affective symptoms. This practice appears to stem from clinical observations made in the 1940s (when ECT was the only effective treatment) that patients with schizophrenia who improved with ECT often had strong affective components. However, some of these statements emanated from the USA, where many patients diagnosed as having schizophrenia would, in Europe, have received a diagnosis of affective psychosis. Chart review studies of patients given ECT in 1950, 1970 and 1985 did not find consistent evidence that patients with affective symptoms did better with ECT than others. Modern, placebo-controlled clinical trials in the 1980s did not find significant improvement in depressive symptoms in patients with schizophrenia given ECT, but did so in patients with psychotic symptoms (Reference Cooper, Kelly, McClelland and KingCooper et al, 1995).
Rehabilitation, social support and work opportunities are likely to lessen the demoralisation seen in schizophrenia. Cognitive therapy has been shown to be effective (Reference Kingdon, Turkington and JohnKingdon et al, 1994), although its role in the treatment of depressive symptoms in particular has not been studied. Given its usefulness in treating depressive illness, this is worth exploring.
In summary, depressive symptoms in schizophrenia are common, are a significant cause of morbidity and mortality and can be adequately differentiated from other symptoms and medication effects. Such symptoms are amenable to treatment and should be actively sought out in all patients.
Multiple choice questions
-
1. Depression in schizophrenia:
-
a is most often seen during periods of remission
-
b is associated with an increased risk of attempted suicide
-
c may be an early sign of impending relapse
-
d is an insignificant cause of morbidity
-
e is a good prognostic sign.
-
-
2. In the differential diagnoses of depression in schizophrenia:
-
a alcohol misuse must be excluded
-
b confusion with negative symptoms sometimes occurs
-
c medical conditions are not important
-
d more consideration should be given to subjective depression
-
e the possibility of impending relapse should be considered.
-
-
3. Symptoms which help to differentiate negative from depressive symptoms include:
-
a hopelessness
-
b suicidal thinking
-
c subjective low mood
-
d retardation
-
e anxiety.
-
-
4. Antipsychotic medication:
-
a frequently causes a ‘pharmacogenic’ depression
-
b may cause dysphoria without associated motor movements
-
c should be decreased if depressive symptoms appear in a previously stable patient
-
d ‘akinetic’ depression may account for up to 25% of cases of depressive symptoms in schizohrenia
-
e will often treat depressive as well positive symptoms present during acute episodes.
-
-
5. Treatments likely to be useful in the treatment of depression in schizophrenia include:
-
a tricyclic antidepressants
-
b atypical antipsychotics
-
c increased psychosocial support
-
d selective serotonin reuptake inhibitors
-
e hospitalisation.
-
Table 1. Main differential diagnoses of depressive symptoms in schizophrenia
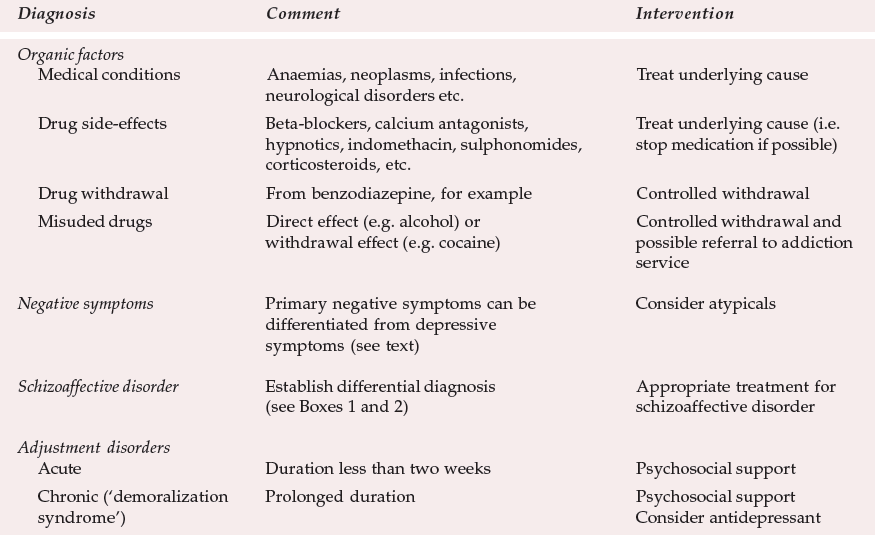
| Diagnosis | Comment | Intervention |
|---|---|---|
| Organic factors | ||
| Medical conditions | Anaemias, neoplasms, infections, neurological disorders etc. | Treat underlying cause |
| Drug side-effects | Beta-blockers, calcium antagonists, hypnotics, indomethacin, sulphonomides, corticosteroids, etc. | Treat underlying cause (i.e. stop medication if possible) |
| Drug withdrawal | From benzodiazepine, for example | Controlled withdrawal |
| Misuded drugs | Direct effect (e.g. alcohol) or withdrawal effect (e.g. cocaine) | Controlled withdrawal and possible referral to addiction service |
| Negative symptoms | Primary negative symptoms can be differentiated from depressive symptoms (see text) | Consider atypicals |
| Schizoaffective disorder | Establish differential diagnosis (see Boxes 1 and 2) | Appropriate treatment for schizoaffective disorder |
| Adjustment disorders | ||
| Acute | Duration less than two weeks | Psychosocial support |
| Chronic (‘demoralization syndrome’) | Prolonged duration | Psychosocial support |
| Consider antidepressant |
Table 2. Antipsychotic medication and depressive symptoms in schizophrenia

| Proposed term | Proposed mechanism | Evidence for hypothesis | Intervention |
|---|---|---|---|
| ‘Pharmacogenic’ depression | Antipsychotics cause depression by depressiona direct effect (?dopaminergic) | Very weak | |
| ‘Akinetic’ depression | Antipsychotics produce extra-pyramidal side-effects such as bradykinesia and loss of spontaneity, mimicking depression (clinical phenocopy of depression) | Possibly explains 10–15% cases of ‘depression’ in schizophrenia | Reduce antipsychotic |
| Low mood can also occur secondary to akinesia | Anticholinergic medication | ||
| Consider atypical antipsychotics | |||
| Antipsychotic-induced dysphoria | Dysphoria with or without motor features of akathisia. | Chronic akathisia presents in 25% of patients | Anticholinergic drugs (but less useful than in akinesia |
| May presentlike (agitated) depression | Proportion with significant dysphoria unknown | ||
| Benzodiazepines | |||
| Beta-blockers | |||
| Reduce antipsychotic dose | |||
| Consider atypical drug |
Table 3. Depressive symptoms and the time-course of schizophrenia

| Stage | Relationship to acute episodes | Estimated prevalence | Treatment |
|---|---|---|---|
| Depression as a prodromal symptom | Sign of impending relapse | 50% | Increase psychosocial support |
| Do not decrease anti- psychotics prematurely Increase may be required | |||
| Depressive symtoms as prominent component of acute episode | Clearly present during an acute psychotic episode (differentiate from schizoaffective disorder) | 22-80% | Requires effective antipsychotic drug treatment initially |
| ‘Revealed depression’ - present during acute episode but only revealed as positive symptoms respont to treatment | Consider atypical antipsychotics | ||
| Require careful clinical follow-up as risk of suicide | |||
| EarlyEarly post-psychotic depression (first six months after acute episode) | Depressive symptoms resolve more slowly than other symtoms of acute episode | 25% | (Below assumes other possible causes eliminated) Require to continue adequate antipsychotic treatment |
| Consider an atypical anti- psychotic | |||
| If severe, may need an antidepressant | |||
| Late post-psychotic depression (more than six months after acute episode) | Depressive symptoms develop in aftermath of acute episode or persist for more than six months after acute episode, i.e. course of depressive symptoms does not correlate with course of acute symptoms | 13–33% (in patients) | An antidepressant should be considered (SSRI firstline) |
| Change of antipsychotic may help a few patients If no improvement, then consider clozapine |
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | T | a | F | a | T |
| b | T | b | T | b | T | b | F | b | T |
| c | T | c | F | c | T | c | T | c | T |
| d | F | d | T | d | F | d | T | d | T |
| e | F | e | T | e | T | e | T | e | T |







eLetters
No eLetters have been published for this article.