Patients with borderline personality disorder (BPD; known in ICD–10 (World Health Organization, 1992) as emotionally unstable personality disorder) pose some of the most difficult management problems facing the clinical psychiatrist. They frequently present in crisis, but are often difficult to engage in any form of treatment. Their behaviour causes considerable anxiety but their ambivalence about treatment often leaves professionals feeling frustrated and resentful. These feelings can all too easily be transformed into therapeutic nihilism. As well as being a significant problem in its own right, comorbid personality disturbance complicates the management of other psychiatric disorders and has a negative effect on their prognosis (Reference Reich and VasileReich & Vasile, 1993).
Borderline personality disorder has an estimated prevalence of up to 2% in the community (Reference Widiger and WeissmanWidiger & Weissman, 1991) and 15 % among psychiatric in-patients (Reference Kroll, Carey and SinesKroll et al, 1982). Yet, despite an extensive psychoanalytic literature and growing attention in the USA, BPD has until recently received relatively little attention in the British psychiatric literature. However, this situation is beginning to change as a result of recent developments in both research and treatment. Developmental research is shedding increasing light on the aetiology of BPD, new models of treatment have been developed and long-term research on outcome is helping to dispel some of the pessimism that has long surrounded the disorder. This paper will review some of these developments.
Box 1. DSM–IV (American Psychiatric Association, 1994) diagnostic criteria for borderline personality disorder
At least five of:
Intense and unstable personal relationships
Frantic efforts to avoid real or imagined abandonment
Identity disturbance or problems with sense of self
Impulsivity that is potentially self-damaging
Recurrent suicidal or parasuicidal behaviour
Affective instability
Chronic feelings of emptiness
Inappropriate intense or uncontrollable anger
Transient stress-related paranoid ideation or severe dissociative symptoms
New perspectives on aetiology
Research over the past decade or so has emphasised the importance of childhood experiences in the aetiology of BPD. Ideas derived from psychoanalysis have received some empirical support and the central aetiological role of childhood trauma has become apparent. Attachment, identity and the ability to make sense of feelings are increasingly seen as interlinked and all are adversely affected by abuse or neglect in childhood.
Trauma, affect regulation and self-harm
Childhood abuse and neglect are extremely common among borderline patients: up to 87% have suffered childhood trauma of some sort, 40–71% have been sexually abused and 25–71% have been physically abused (Reference Perry, Herman and ParisPerry & Herman, 1993). The effect of abuse seems to depend on the stage of psychological development at which it takes place; in general, the earlier it takes place, the more damaging it is likely to be (Reference Van der Kolk, Hostetler and Herronvan der Kolk et al, 1994). This is probably due to the young child's cognitive immaturity and consequent inability to make sense of traumatic experiences. Sexual abuse, as well as being damaging in its own right, may also reflect the generally dysfunctional nature of families who are unable to protect their children adequately.
There is considerable evidence that borderline patients have difficulty modulating emotion, and this appears to be linked with early trauma (Reference Van der Kolk, Hostetler and Herronvan der Kolk et al, 1994). Trauma, in the form of sexual abuse, is also strongly correlated with self-mutilation in borderline patients (Reference Herman, Perry and KolkHerman et al, 1989). Self-mutilation such as cutting is often experienced as painless at the time, suggesting that it takes place in a dissociated state. Indeed, the combination of severe trauma and dissociative phenomena in BPD has led some researchers to link it with post-traumatic stress disorder.
Attachment and reflective self-function
Research based on attachment theory is beginning to elucidate the links between childhood trauma and the capacity to think about oneself and others. Borderline patients are typically preoccupied with their disturbed early relationships yet unable to give a coherent account of them (Reference Patrick, Hobson and CastlePatrick et al, 1994; Reference Fonagy, Leigh and SteeleFonagy et al, 1996). Severe childhood trauma in these patients appears to result in a specific inability to think about their own thoughts and feelings, as well as those of others.
This finding is consistent with the observation that maltreated children have difficulty in expressing both negative and positive feelings. As well as contributing to problems in interpersonal relationships, the inability to think about feelings may combine with defective affect regulation to produce the impulsivity which is so characteristic of borderline patients.
Box 2. Possible effects of childhood trauma in borderline personality disorder
Self-mutilation
Defective affect regulation
Lack of reflective capacity
Dissociation
Impulsivity
Disturbed interpersonal relationships
Identity and the self
The lack of a sense of self is a core feature of the psychopathology of BPD, and psychoanalysts have traditionally linked this phenomenon to pathological splitting of the ego and object. Splitting is often very marked in borderline patients, who may engender powerful yet conflicting feelings in different members of the psychiatric team. Such splitting has traditionally been thought of as a ‘primitive’ defence mechanism that indicates arrested psychological development. However, it may be an appropriate response to abuse from someone who is also a parent or carer. Recent research confirms the link between splitting and sexual abuse and suggests that it may, in fact, be a relatively sophisticated psychological mechanism for dealing with traumatic experience (Reference Calverley, Fischer and AyoubCalverley et al, 1994).
The concept of self is central to the work of Heinz Kohut and the branch of psychoanalysis known as self-psychology (Reference KohutKohut, 1984). Kohut's ideas have been incorporated into the treatment approach developed by Stevenson & Meares (1992). Ryle (1997), from the somewhat different perspective of cognitive–analytic therapy, has developed an aetiological model of BPD based on the concept of multiple self-states. These are partially dissociated states between which the patient switches abruptly. Each self-state is linked to specific moods, behaviours and symptoms and is associated with corresponding interpersonal roles. Both these therapies are described later in this paper.
New developments in treatment
Several new forms of treatment for BPD have been developed over the past few years and evidence is also emerging for the effectiveness of some of the more established approaches.
Dialectical behaviour therapy
Dialectical behaviour therapy (DBT; Linehan, 1993) is based on the principle that BPD is essentially the result of deficits in interpersonal and self-regulatory skills and that these skills can be taught in therapy. Defective affect regulation is seen as particularly important. Treatment consists of weekly individual and group therapy sessions based on a skills-training model, together with out-of-hours telephone contact with the therapist.
Dialectical behaviour therapy has been shown, in a single study, to be superior to ‘treatment as usual’ in reducing self-harm and time spent in hospital, but not subjective experiences such as depression and hopelessness (Reference Linehan, Armstrong and SuarezLinehan et al, 1991). There were also significant improvements in social and global functioning and anger (Reference Linehan, Tutek and HeardLinehan et al, 1994). However, by one year after the end of treatment, rates of self-harm were no different in the DBT and treatment-as-usual groups, although both had improved (Reference Linehan, Heard and ArmstrongLinehan et al, 1993).
Box 3. New therapies for borderline personality disorder
Cognitive analytic therapy
Brief psychoanalytic psychotherapy
Interpersonal psychotherapy
Dialectical behaviour therapy
Schema-focused cognitive therapy
Despite this essentially negative finding, DBT has attracted considerable interest; however, Linehan's study is open to a number of methodological criticisms. Only 39 patients were studied, all of them female, and of these only 20 were fully assessed. The level of self-harm required for entry into the study (two episodes in the last five years and one in the last eight weeks) may have led to the inclusion of patients who were less severely disturbed than those commonly seen in clinical practice. Furthermore, DBT involves a high level of input from professionals and it is not yet clear whether it is the skills training itself or simply the high level of support which leads to the reduction in self-harm.
Psychoanalytic psychotherapy
Psychoanalytic psychotherapy has long been used in the treatment of borderline patients but has never been subjected to formal evaluation. The available data suggest that only a minority of borderline patients benefit from psychoanalytic psychotherapy in its traditional form (Reference Waldinger and GundersonWaldinger & Gunderson, 1984). However, a modified approach, which emphasises current rather than past experiences and in which the therapist takes a more active role, may be more suitable for the treatment of BPD.
Stevenson & Meares (1992) have described encouraging results using a specialised form of brief psychotherapy which is designed specifically to meet the needs of borderline patients. This model draws on both self-psychology and Hobson's ‘conversational model’ (Reference HobsonHobson, 1985). Patients are seen twice-weekly for a year and therapy can be delivered by trainee therapists following a treatment manual. In their study, this form of therapy produced significant improvements in violent behaviour, use of medication, self-harm and hospital admissions. Improvements were also observed in impulsivity, affective instability and suicidal behaviour and by the end of treatment, 30% of patients no longer met DSM–III–R (American Psychiatric Association, 1987) criteria for BPD.
Therapeutic communities
Recent work has provided evidence for the effectiveness of therapeutic community treatment. Dolan et al (1997) compared 70 patients treated at the Henderson Hospital with those referred but refused funding by their health authorities. Eighty per cent of their patients had a diagnosis of BPD and many also met the diagnostic criteria for other personality disorders. Forty-three per cent of the treated patients showed a clinically significant change in core borderline psychopathology at one year after discharge, compared with 18% of those who had been refused funding.
Another approach to evaluating the effectiveness of therapeutic community treatment is to calculate service consumption and costs to public services before and after treatment. Recent studies have found substantial reductions in service consumption and costs following treatment in three National Health Service therapeutic communities: the Cassel and Henderson Hospitals in London and Francis Dixon Lodge in Leicester (Reference Chiesa, Iacoponi and MorisChiesa et al, 1996; Reference Dolan, Warren and MenziesDolan et al, 1996; Reference Davies, Campling and RyanDavies et al, 1999).
Interpersonal therapies
Interpersonal difficulties are one of the most common presenting features of BPD. Not only do they cause considerable suffering to the patient but they are also likely to manifest themselves in complex and ambivalent relationships with professionals.
Benjamin (1996) has developed a technique for analysing patterns of interpersonal behaviour known as the Structural Analysis of Social Behavior (SASB). This instrument allows dysfunctional interpersonal patterns to be identified and coded and has led to the development of a therapeutic approach that is aimed at modifying interpersonal behaviour. In therapy, maladaptive interpersonal patterns are identified and their origins explored. An eclectic mix of techniques is used including role play, free association, dream analysis and educational assignments. When the patient is ready to do so, the therapist helps him or her to ‘block’ maladaptive patterns and learn new ways of functioning.
The brief interpersonal therapy (IPT) developed by Klerman and his colleagues (Reference Klerman, Weissman and RounsavilleKlerman et al, 1984) has also been adapted for use with borderline patients. Originally designed to treat depression, IPT is a structured and time-limited therapy which focuses on the relationship between symptoms and interpersonal difficulties. A small pilot study has been carried out using an 18-session programme for borderline patients (Reference Angus and GilliesAngus & Gillies, 1994), but the results have yet to be published.
Cognitive–analytic therapy
Cognitive–analytic therapy (CAT) for borderline patients employs a collaborative approach between patient and therapist in order to identify self-states (Reference Ryle, Leighton and PollockRyle et al, 1997). Inadequate parenting is thought to result in an inability to integrate these self-states, leading to rapid shifts between them. These shifts between self-states and their associated interpersonal roles are seen as a cause of the instability that borderline patients display.
In therapy, the patient is helped to make links between early experience and current behaviour. The collaborative nature of the therapeutic relationship also gives the patient experience of a new and more healthy way of relating and thus contributes to the process of change. Although promising, CAT has yet to be evaluated adequately in clinical practice.
Schema-focused cognitive therapy
Another novel but untested approach is schema-focused cognitive therapy (Reference YoungYoung, 1994). This therapy concentrates on identifying and modifying the ‘early maladaptive schemas’ thought to underlie BPD. Schemas are:
“broad pervasive themes regarding oneself and one's relationship with others, developed during childhood and elaborated throughout one's lifetime, and dysfunctional to a significant degree” (Reference YoungYoung, 1994).
Early maladaptive schemas have their origins in adverse childhood experiences and are particularly resistant to change. They cover themes familiar to psychoanalytic psychotherapists and are organised into five principal domains: disconnection and rejection; impaired autonomy and performance; impaired limits; other-directedness; and overvigilance and inhibition.
Therapy consists initially of identifying and activating core schemas (for example, with the use of imagery), which therapist and patient then discuss. Schemas are then modified using cognitive reconstruction, behavioural and experiential techniques and discussion of issues arising in the therapist–patient relationship.
Long-term outcome
Several studies have now established that the long-term prognosis in BPD is significantly better than is often assumed and that the majority of patients improve over time (for review see Stone, 1993). For example, Links et al (1998) found that 53% of patients followed-up for seven years no longer met diagnostic criteria for BPD. In one of the largest studies, long-term follow-up of a cohort of patients treated at the New York Psychiatric Institute found that two-thirds were clinically well (Reference Stone, Hurt and StoneStone et al, 1987).
Future developments
Our understanding of the aetiology of BPD has grown considerably over the past decade and it is increasingly being seen as a disorder of psychological development. However, major questions remain. Are some individuals more vulnerable to the development of the disorder than others? Are there potentially protective factors? Perhaps most crucially of all, can early intervention with at-risk families help to prevent the development of BPD?
At the clinical level, there is an urgent need for more research into the outcome of different forms of treatment. Studies of treatments such as DBT and brief psychoanalytic psychotherapy need to be replicated, and the effectiveness of therapies such as CAT and IPT needs to be evaluated. The relative merits of different therapies have yet to be assessed and it is unclear how best to match patients to therapies. Many of the new therapies for BPD share a theoretically coherent, manual-based structure and it may be that the coherence and consistency this provides is particularly important for borderline patients. We do not yet know whether these structured, short-term therapies will prove sufficient on their own or will in future be used as a prelude to more exploratory therapy for suitable patients. Moreover, it is probable that most borderline patients will continue to be managed by general psychiatrists and the place of such specialised therapies within generic mental health services will need to be determined.
The apparent success of these brief therapies is somewhat at odds with the view held by many clinicians that borderline patients benefit from a relatively prolonged relationship with a therapist or therapeutic team. This view is consistent with the evidence for disordered attachment in BPD, which suggests that a stable therapeutic attachment may be helpful in allowing patients to develop psychologically in a more functional way. Long-term follow-up studies will be needed to clarify whether the effects of brief therapies persist beyond the end of the treatment period.
Despite many unanswered questions, recent developments give grounds for optimism. It is now difficult to sustain the view that all borderline patients are untreatable. Psychoanalysis, cognitive therapy and empirical research are converging, and a coherent aetiological model of the disorder is beginning to emerge. The outlook for this challenging group of patients may be starting to improve.
Multiple choice questions
-
1. The prevalence of borderline personality disorder among in-patients is estimated to be:
-
a 10%
-
b 15%
-
c 20%
-
d 12%
-
e 5%.
-
-
2. Multiple self-states are associated with:
-
a schema-focused cognitive therapy
-
b self-psychology
-
c cognitive–analytic therapy
-
d dialectical behaviour therapy
-
e interpersonal therapy.
-
-
3. In borderline personality disorder:
-
a a disturbed sense of self is common
-
b patients are preoccupied with disturbed early relationships
-
c pathological splitting is uncommon
-
d the New York Psychiatric Institute follow-up study found that one-third were clinically well
-
e therapeutic community treatment produces a reduction in service consumption.
-
-
4. With respect to childhood trauma:
-
a physical abuse is more common than sexual abuse
-
b defective affect regulation is related to early trauma
-
c trauma has been linked to difficulty thinking about oneself and others
-
d sexual abuse is strongly correlated with self-mutilation
-
e up to 87% of patients have suffered childhood trauma.
-
-
5. In the treatment of borderline personality disorder:
-
a dialectical behaviour therapy is clearly superior to treatment as usual
-
b dialectical behaviour therapy reduces depression
-
c cognitive–analytic therapy is more effective than interpersonal therapy
-
d theoretical coherence may be important
-
e interpersonal therapy was originally developed to treat depression.
-
MCQ answers
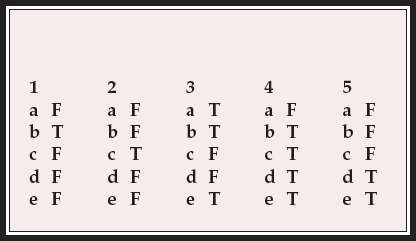
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | T | a | F | a | F |
| b | T | b | F | b | T | b | T | b | F |
| c | F | c | T | c | F | c | T | c | F |
| d | F | d | F | d | F | d | T | d | T |
| e | F | e | F | e | T | e | T | e | T |

Fig. 1 An aetiological model of borderline personality disorder






eLetters
No eLetters have been published for this article.