The recent film Boys Don't Cry illustrates in a highly dramatised form the problems that the phenomenon of gender identity disorder can create in an extreme situation. The film is based on the true story of a young person, Brandon, with a female body who perceived himself as a male. In the film we do not know when the issue of his male gender identity first appeared, but we see him living in a male role as a teenager trying to conceal, to his peers, the reality of his female body. (I refer to Brandon as ‘he’ because this is how Brandon presents himself in the film. The dilemma about using ‘he’ or ‘she’ typically confronts professionals in the management of teenagers like Brandon.) The struggles of these concealments are well portrayed, as in the scene when he steals tampons from a shop. He joins in male activities and displays of physical strength as a confirmation of his male role. He is well accepted as a boy within a troubled and troublesome group of young people. He falls passionately in love with a girl, Lana, who accepts him as he is without much questioning, and a close intimate relationship develops, which the peer group seems to accept. The reality of his body is eventually revealed. His girlfriend can accept the new situation, but had she really not known or had she turned a blind eye? Unfortunately, two young men become more and more disturbed by this realisation. It stirs a primitive violence in them, which leads first to Brandon's rape and then to his murder.
How can we make sense of this complex tragedy? Here I would like to suggest that a sense of unbearable identity confusion in the two young people is what leads to the violence. It is aimed at changing Brandon and eventually destroying him when their attempt to make him submit to their views of order on gender and sexual matters fails. For them, having a female body is inextricably connected with having a female identity. Any digression from this rule is a terrible threat to their flimsy sense of identity. Obviously, other factors can be invoked in making sense of their behaviour, but these are beyond the scope of this paper.
The establishment and maintenance of secrecy can have serious psychosocial consequences, as the film shows when secrecy is suddenly broken. On the other hand, people who are aware and come into contact with a child or teenager with a gender identity disorder often experience a sense of confusion. Breaking a cycle of secrecy by promoting openness and creating the conditions for the tolerance of confusion and uncertainty are important issues in the management of gender identity disorders (see ‘Primary therapeutic aims’, Box 3).
Before the 1960s, secrecy and confusion dominated the area of atypical gender identity development. The first definition of the term ‘gender role’ was given by John Money (1955). Money wanted to differentiate a set of feelings, assertions and behaviours that identified a person as being a boy or a girl, or a man or a woman, from the contrasting conclusion one could have reached by considering only their gonads. In the vast majority of cases he described, the gender role adopted by the individuals was consistent with their rearing.
The term ‘gender identity’ appeared in the mid-1960s in association with the establishment of a gender identity study group at the University of California. Stoller (1992: 78) defines it as:
“A complex system of beliefs about oneself: a sense of one' masculinity and femininity. It implies nothing about the origins of that sense (e.g. whether the person is male or female). It has, then, psychologic connotations only: one's subjective state.”
The concept of gender identity and role having been formulated, it became possible to make sense of, and give order to, conditions that had until then been ill-defined and poorly understood. Incongruity between the biological sex and the psychological behavioural manifestations of gender identity indicated the presence of a gender identity disorder.
Classifications of gender identity disorders of childhood
Over the past 20 years, four diagnostic models have been proposed. The first is the Diagnostic and Statistical Manual of Mental Disorders (4th edn) (DSM—IV; American Psychiatric Association, 1994). This sets criteria for children, adolescents and adults (Box 1) and requires that four criteria be satisfied for the diagnosis to be made. Criteria A and B refer to two aspects of gender identity disorder: A to evidence of cross-gender identification; and B to the experience of discomfort about one's biological sex and the feeling of inappropriateness in the gender role of that sex.
The second is the International Classification of Diseases, Tenth Revision (ICD—10, F64.2; World Health Organization, 1992). In this classification there is no distinction between criteria A and B and “the diagnosis requires a profound disturbance of the normal gender identity; mere tomboyishness in girls or girlish behaviour in boys is not sufficient”.
Third is Rosen et al's (1977) distinction between cross-gender identification and gender-behaviour disturbance. This classification has proved unsatisfactory, as a large number of children (71%) present both characteristics (Reference Bentler, Rekers and RosenBentler et al, 1979).
Fourth is Stoller's (1968) diagnosis of ‘male childhood transsexualism’. This is based on the presence in a boy of “a fixed belief that he is a member of the opposite sex and will grow up to develop the anatomical characteristics of the opposite sex” (p. 195).
Box 1 Criteria for diagnosis of gender identity disorders from the Diagnostic and Statistical Manual of Mental Disorders (4th edn) (DSM—IV; American Psychiatric Association, 1994)
-
1 A strong and persistent cross-gender identification (not merely a desire for any perceived cultural advantages of being the other sex)
-
In children the disturbance is manifested by four (or more) of the following:
-
• repeatedly stated desire to be, or insistence that he/she is, the other sex;
-
• in boys, preference for cross-dressing or simulating female attire; in girls, insistence on only wearing stereotypical masculine clothing;
-
• strong and persistent preferences for cross-sex roles in make-believe play or persistent fantasies of being the other sex;
-
• intense desire to participate in the stereotypical games and pastimes of the other sex;
-
• strong preference for playmates of the other sex
-
-
In adolescents and adults, the disturbance is manifested in symptoms such as:
-
• stated desire to be the other sex
-
• frequent passing as the other sex
-
• desire to live and be treated as the other sex
-
• conviction that he/she has the typical feelings and reactions of the other sex
-
-
-
B Persistent discomfort with his/her sex or sense of inappropriateness in the gender role of the sex
-
In children, the disturbance is manifested by any of the following: in boys, the assertion that their penis and testes are disgusting or will disappear, or assertion that it would be better not to have a penis, or aversion towards rough and tumble play and rejection of male stereotypical toys, games and activities; in girls, the rejection of urinating in a sitting position, assertion that they have or will grow a penis, or assertion that they do not want to grow breasts or menstruate, or marked aversion toward normative female clothing.
-
In adolescents and adults, the disturbance is manifested by symptoms such as preoccupation with getting rid of primary and secondary sex characteristics (e.g. request for hormones, surgery or other procedures to alter sexual characteristics physically to simulate the other sex) or belief that they were born the wrong sex.
-
-
C The disturbance is not concurrent with a physical intersex condition
-
D The disturbance causes clinically significant distress or impairment in social, occupational or other important areas of functioning
The following case study illustrates an initial clinical presentation.
Case study 1: James
James was referred to the Gender Identity Development Service at the age of 8 years.
At the assessment interviews, he said that since the age of 4 or 5 years he had very much wished he were a girl. He had been secretly dressing up in his mother's clothes. He liked to play with dolls and cuddly toys and fantasised that he was a mother feeding them. He played weddings and liked to be in the role of the bride. At school he wanted to play with girls and avoided rough-and-tumble play or other activities with boys.
His maternal grandmother had looked after him from age 6 months to 5 years, as his mother was away often for her work. The grandmother involved him in many activities, including cooking and tidying up the house. After her sudden death in hospital, James developed a gender identity disorder. He could not talk about the loss of his grandmother or even mention her, but he concretely identified with her and persistently wished to continue with all the activities in exactly the same way as he had once with her. Family therapy, focusing on a family tree constructed over many sessions, enabled the narrative of his experiences with his grandmother to be developed. The clinical features of his gender identity disorder gradually reduced in intensity and disappeared.
In this case the psychological work focused not only on mourning processes, but it also removed the secrecy about his gender problem, encouraged curiosity about its origins and established a link between his atypical gender development and the way he had coped with the loss of his grandmother. Symbol formation was stimulated, so that he could have a mental picture of her and memories of the past, rather than concretely identifying with and becoming her. Increased contact with his father seemed also to play an important role.
Epidemiology
The incidence of childhood cross-gender identification in the general population and in the psychiatric population has not yet been definitely established. The studies that have been carried out have used differing criteria, such as single behaviours or identity statements. No large-scale investigation with standardised criteria, such as those of DSM—IV, has yet been conducted.
Zuger and Taylor (1969) interviewed the mothers of boys aged about 7 years with regard to the presence of six cross-gender behaviours. Table 1 shows the percentage of positive occurrences for each behaviour. The mothers were not asked how long the behaviours had been apparent nor when they started. Zuger and Taylor also showed that these behaviours were not frequently found in children (73% never engaged in any of them).
Table 1 Maternal report of cross-gender behaviour in boys aged about 7 years (from Zuger & Taylor, 1969)

| Behaviour | Number | % positive occurrence |
|---|---|---|
| Desire to be female | 46 | 7 |
| Feminine dressing | 95 | 13 |
| Wearing lipstick | 94 | 7 |
| Doll play | 95 | 7 |
| Preference for girl playmates | 41 | 15 |
| Aversion to boys' games | 93 | 2 |
Feinblatt and Gold (1976) found that of 193 children referred to a Connecticut child guidance clinic, four boys and three girls (3.6% of the total) were referred primarily because of ‘gender-role inappropriate behaviour’.
Epidemiological data suggest that “extreme forms of cross-gender behaviour are uncommon among boys in the general population” (Zucker, 1985; see also Zucker & Bradley, 1995). One could fairly confidently say that cross-gender behaviour is not “a common phase in boyhood behaviour” (Reference GreenGreen, 1968). There is insufficient epidemiological research regarding girls to be able to make a similar statement.
Long-term follow-up studies
The most scientifically accurate follow-up study was conducted by Green (1987). He reports that of the 66 males in the original ‘feminine boy’ group, two-thirds were re-interviewed in adolescence or young adulthood, when three-quarters of them were found to be homosexual or bisexual. Only one boy in this study had a transsexual outcome.
Zucker (1985) collated all the long-term follow-up studies of children identified as cross-gender referred to mental health professionals (Table 2).
Table 2 Long-term follow-up studies of children with gender identity disorders (from Zucker, 1985)
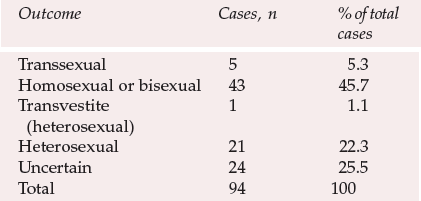
| Outcome | Cases, n | % of total cases |
|---|---|---|
| Transsexual | 5 | 5.3 |
| Homosexual or bisexual | 43 | 45.7 |
| Transvestite (heterosexual) | 1 | 1.1 |
| Heterosexual | 21 | 22.3 |
| Uncertain | 24 | 25.5 |
| Total | 94 | 100 |
Money and Russo (1981), explaining the low incidence of a transsexual outcome, suggest that the “natural history of transsexualism is disrupted by the child's contact with the mental health profession” (Reference Zucker and SteinerZucker, 1985).
Green et al (1987) examined five types of behaviour in boys: role/doll play, cross-dressing, having female peers, rough-and-tumble play and the wish to be a girl. They found that doll play and role play as a girl associated more strongly with a homosexual outcome.
Comorbidity
Coates and Spector Person (1985) have shown that children with gender identity disorders also present with separation anxiety, depression and emotional and behavioural difficulties. In a number of cases referred to the Gender Identity Development Service (GIDS) at the Portman Clinic, learning difficulties and school refusal are also present. In a small percentage of cases, child sexual abuse has been associated with a gender identity disorder. Suicide attempts in adolescence are frequent and in some cases this is how adolescents with gender identity disorders come to professional attention.
In a survey of the first 124 cases referred to the GIDS at the Portman Clinic, we found that the most common associated features were relationship difficulties with parents or carers (57%), relationship difficulties with peers (52%), depression/misery (42%), family mental health problems (38%), family physical health problems (38%), being the victim of harassment or persecution (33%) and social sensitivity (31%). These data suggest that children with gender identity problems may experience considerable isolation owing to difficulties in their relationships with significant adults and peers. They can also become the victims of persecution, which may contribute to feelings of depression and misery. In this sample, boys appear to experience more harassment than girls and this may be due to the fact that gender non-conformity in boys is less socially acceptable than in girls. The high percentages of mental and physical health problems in the families of children and adolescents referred may indicate that factors such as parental depression or major physical illness may represent a traumatic event for the child, possibly contributing to the gender identity problem. This survey also showed that associated difficulties and case complexity increase during adolescence.
Aetiology
No single cause has yet been found with certainty for the development of a gender identity disorder.
Hereditary factors (Reference Bailey and PillardBailey & Pillard, 1991) have been suggested for male homosexuals. The contribution of such factors to the development of gender identity disorders in children, however, is unclear and further research is needed.
Hormonal influences on the brain during foetal development have also been suggested, with androgens masculinising the brain during a critical period of foetal life.
In humans the third interstitial nucleus of the anterior hypothalamus is usually larger in the male. LeVay (1991) has shown that in the brain of homosexual men this nucleus is similar in size to that of women and about half the volume of that in heterosexual men.
However, each of these factors alone may be insufficient to produce a gender identity disorder.
Stoller (1968) has described particular family constellations associated with gender identity disorders in boys and girls. For boys, he suggests there is an overclose relationship with the mother and a distant father. For girls, he suggests a depressed mother during the early months of the child's life and a father who is absent and does not support the mother, but encourages the child to assuage the mother's depression.
Marantz and Coates (1991) have described very early maternal influences that negatively affect the early development of the child.
Bleiberg et al (1986) have linked the development of gender identity disorders in some children to their inability to mourn a parent or an important attachment figure in early childhood.
A parent's wish for a child of the other gender, or direct parental pressure in rearing the child in the gender role opposite to the biological sex, are not sufficient on their own to produce a marked gender identity disorder.
A number of authors (e.g. Coates et al, 1991; Money, 1994) would agree that many of these factors need to be present simultaneously and work together during a critical period to produce a full-blown gender identity disorder. This would also explain the rarity of the condition.
Case study 2: Mark
Mark, aged 16 years, presented a gender identity disorder of a transsexual type. He hated his male body intensely. Socially isolated and in despair, he had attempted suicide. Since the age of 3 or 4 years he had felt that he was a girl. At the age of 7 years his father sexually abused him and this experience confirmed for him that he was a girl as, at that time, he thought that men were sexually attracted only to women. At the time of the referral he felt that his body should be changed immediately, as he could not bear living in a contradictory situation. There was also a real possibility of further suicide attempts.
A structured therapeutic programme, including individual and family sessions, and also consultation with a paediatric endocrinologist, made him feel that mind and body had been taken into consideration and helped him to tolerate a transitional phase of uncertainty by containing his feelings of despair. It also supported his hope that the incongruence between his mind and body would eventually be overcome. It was important that network meetings of the professionals involved with his care were held at regular intervals.
Exploration of the patient's expectations, gender identity and roles, body image, self-perception and other people's perception of the individual is essential preparation for the young person before referral to a gender identity service for adults at the age of 18 years. No irreversible physical intervention should be undertaken before this age.
Nature of atypical gender identity organisation
In 1964 Stoller proposed the concept of core gender identity. He saw this as:
“produced by the infant—parent relationship, the child's perception of its external genitalia, and a biologic force, which results from the biologic variables of sex (chromosomes, gonads, hormones, internal accessory reproductive structures and external genitalia)”.
Stoller believed that the core gender identity is established before the fully developed phallic stage, although gender identity continues to develop into adolescence or beyond (1964: 453). He further stated that the beliefs comprising the “mental structure” of the core gender identity are the earliest part of gender identity to develop and are relatively permanent after the child reaches 4 or 5 years of age (1992: 78).
Further research and clinical experience shows that there may be more flexibility in gender identity development than Stoller's concept of core gender identity would imply. Only in some children and adolescents with an atypical development does the core gender identity have the structural characteristics described by Stoller. In 1998 I proposed the concept of atypical gender identity organisation (AGIO) as a clinical entity that can be examined under a number of parameters relevant to clinical management (Box 2; Di Ceglie, 1998a). These are as follows.
Box 2 Clinical features of atypical gender identity organisation (AGIO; from Di Ceglie, 1998a)
Rigidity—flexibility
Timing of formation of the AGIO
Presence/absence of traumatic events in the child's life in relation to formation of the AGIO
Position of the AGIO on continuum from the paranoid—schizoid to the depressive position
Rigidity—flexibility.
This refers to the capacity of the organisation to remain unchangeable or, alternatively, to be amenable to evolution in the course of development. Only in particular cases will it possess the unchangeable structural qualities of Stoller's core gender identity.
Timing of the AGIO formation.
Atypical organisations that develop very early in the child's life may be more likely to become rigidly structured than organisations that develop later.
Identifiable traumatic events in the child's life in relationship to the AGIO formation.
In some cases the AGIO is formed as a psychological coping strategy in relation to a traumatic event in childhood. The earlier the trauma occurs, the more likely it is that the organisation will acquire rigid and unchangeable qualities.
Where the formation of the AGIO can be located on the continuum from the paranoid—schizoid to the depressive position.
The hypothesis here is that if the AGIO is formed within a mental functioning dominated by paranoid—schizoid processes in response to a traumatic event, it is more likely to become very structured and therefore not amenable to change. Alternatively, if it is formed within a mental functioning of the depressive position it is likely that the organisation will be amenable to evolution.
Therapeutic exploration over a long period of time may be able to elucidate the characteristics of the organisation and therefore guide management. The following clinical example illustrates this point.
Case study 3: Jennifer
Jennifer was 17 when I saw her following three suicide attempts. She was a female to male transsexual who presented with depressive episodes and a number of borderline features. Her mother, who had died just before Jennifer came to see me, suffered depression after Jennifer's birth, and her father had been physically violent towards his wife during Jennifer's childhood, until they separated. During her psychotherapy sessions with me, she vividly remembered episodes when her father in fits of temper had kicked her mother, even in the stomach. In one session she admitted, not without a sense of embarrassment and shame, that she had identified with him, an experience that she could not explain. She loved her mother, and her main aim in life was to do something extraordinary that would have made her mother happy. There was no recollection that Jennifer herself had been physically abused by her father, but witnessing violence between her parents had been a traumatic childhood experience.
One defensive manoeuvre she used to cope with the fear of damage to her mother and possibly to herself was to identify with a male possessing the strength of a physical masculine body. This belief, once established, allowed her an omnipotent sense of survival and also of protecting her ‘damaged’ mother. A female representation of herself had to be strongly avoided, as this was equated in her mind with being weak and damaged.
Another important factor also seemed to play a part. After the birth of two older sisters, her mother had miscarried a baby boy. One year later, Jennifer was born. Jennifer seemed to feel that her mother had expected her to be a boy, and in one session she alluded to her mother having “psychic qualities”, as if she had been part of a magical experience in which she and her mother could read each others' minds. She had probably received, and made her own, her mother's wish that she were a boy. This wish was probably never consciously expressed by her mother, but remained unconsciously active in the relationship between them.
Two years' psychotherapeutic exploration with this patient allowed me to make this partial reconstruction of her childhood relating to her atypical gender identity development. However, my attempts to explore this understanding with Jennifer led to continuous interruptions to the therapeutic work, which showed her extreme resistance and fears of having the foundation of her gender identity revisited.
Even if she retained some of this understanding, it certainly did not alter Jennifer's gender identity development — that is to say, the sense of who she was — within the limitations of twice-a-week psychotherapy. Her atypical gender identity organisation (AGIO) was well established and not amenable to evolution. It formed very early in her life, and traumatic events had played a large part in it. Its formation seemed to have occurred under the dominance of the paranoid—schizoid position, constituting a rigid nucleus of gender identity on which her development had been based.
Other aspects of her life improved. She did not attempt suicide again, she settled in a job and she was more able to establish relationships with other people. One might say that therapy had helped her to reduce the hold of the AGIO on other aspects of her development and of her life.
Management and therapy: the staged approach
Behavioural therapy, individual psychotherapy, family therapy and group therapy have been used with these children and their families. Their efficacy is unproven.
As the aetiology of gender identity disorder is unclear and probably multi-factorial, at the GIDS we have developed a model of management in which altering the gender identity disorder per se is not a primary therapeutic objective. Our primary therapeutic concern is the developmental processes that, on clinical and research experience, seem to have been negatively affected in the child (Box 3).
While changing the gender identity disorder itself is not the primary aim, it is possible that by targeting and improving the developmental processes that may underpin gender development, it will be affected in a secondary way and will not lead to establishment of an atypical gender identity in adulthood. The aims outlined in Box 3 could be achieved through various psychotherapeutic interventions, ranging from individual to family and group therapy. Social and educational interventions are also useful. It is important that these are well coordinated and integrated in a comprehensive management plan.
Box 3 Primary therapeutic aims (from Di Ceglie, 1998a)
To foster recognition and non-judgemental acceptance of gender identity problems
To ameliorate associated behavioural, emotional and relationship difficulties (Reference Coates and Spector PersonCoates & Spector Person, 1985)
To break the cycle of secrecy
To activate interest and curiosity by exploring the impediments to them
To encourage exploration of the mind—body relationship by promoting close collaboration among professionals in different specialities, including a paediatric endocrinologist
To allow mourning processes to occur ( Reference Bleiberg, Jackson and Ross Bleiberg et al, 1986 )
To enable symbol formation and symbolic thinking (Reference SegalSegal, 1957)
To promote separation and differentiation
To enable the child or adolescent and the family to tolerate uncertainty in gender identity development
To sustain hope
These aims are more relevant in some cases than in others. The three case studies above give a brief illustration of how these therapeutic objectives could be tackled in clinical work; for a more detailed account see Di Ceglie (1998b).
The recognition and non-judgemental acceptance of the gender identity problem, which is not the result of the child's conscious choice, is important. Without this the child would experience feelings of rejection, psychological splitting processes would increase to cope with this and no further therapeutic work could be undertaken. Group work for parents of children with gender identity disorders can be very helpful in this respect, as it helps the parents to realise that their problem is not unique.
Where an inability to mourn attachment figures has interfered with gender identity development, work enabling mourning to occur may secondarily alter an atypical gender identity development, as shown in case study 1.
The general approach to the management of gender identity disorder can be best conceptualised as a process involving four stages, in line with the guidance for management issued by the Royal College of Psychiatrists (1998), summarised in Box 4.
Stage 1 of the process for children and adolescents is a therapeutic exploration, as described above. In adolescents, if the AGIO persists and shows a high level of rigidity and therefore evolution towards transsexualism, then physical interventions could be considered if they are requested by the adolescent and his or her family. There is often pressure for physical intervention because of the high level of distress brought about by the reality of the changing body at puberty. However, the move towards physical intervention should be cautious.
Stage 2 includes wholly reversible intervention. This involves the use of hypothalamic blockers, which suppress the production of oestrogens or testosterone and produce a state of biological neutrality. In order that adolescents and parents may make a properly informed decision, the Royal College of Psychiatrists' guidance recommends that young people have some experience of themselves in the post-pubertal state of their biological sex. When this intervention has been properly assimilated, while continuing psychological exploration, support and physical monitoring by a paediatric endocrinologist, stage 3 can be considered.
Stage 3 includes partially reversible interventions, such as hormonal treatment that masculinises or feminises the body.
Finally, stage 4 includes irreversible interventions, such as surgical procedures. The College guidance recommends that:
“surgical intervention should not be carried out prior to adulthood, or prior to a real life experience for the young person of living in the gender role of the sex with which they identify for at least two years. The threshold of 18 should be seen as an eligibility criterion and not an indicator in itself for more active intervention, as the needs of many adults may also be best met by a cautious, evolving approach” (Royal College of Psychiatrists, 1998: 6).
Children, particularly adolescents, and their families often find the experience of a gender identity disorder painful and unbearable, and adolescents are at high risk of suicide attempts. This sense of despair frequently leads to extreme pressure being placed on clinicians to act and to provide immediate solutions, through physical intervention, which may not be clinically appropriate at the time of request. In such cases, a detailed discussion with the adolescent and the family of the treatment as a staged process may be containing, by creating space for thinking. This may allow time to explore the issues involved in each stage, and this may gradually reduce the pressure for immediate solutions that have not been properly thought through.
A follow-up study of transsexual adolescents who, after careful asssessment, started the process of sex reassignment during adolescence (after the age of 16) shows that they had acheived a good level of psychological and social adjustment at least 1 year after surgical intervention (Reference Cohen-Kettenis and van GoozenCohen-Kettenis & van Goozen, 1997).
Box 4 Summary of Royal College of Psychiatrists' (1998) guidance for management of gender identity disorders in children and adolescents
Gender identity disorders in children and adolescents:
-
• are rare
-
• are more common in boys
-
• are developmental
-
• involve psychological, biological, family and social issues
-
• have an outcome that cannot be easily predicted
-
• require early and careful assessment and attention to emotional and developmental needs
Consideration of physical interventions should be cautious, involve extensive psychological, family and social exploration, take into account adverse effects on physical growth and be undertaken only by specialist teams
A large element of management is promoting the young person's tolerance of uncertainty and resisting pressures for quick solutions
Surgical intervention cannot be justified until adulthood
Conclusions
Gender identity disorders remain complex conditions to treat. However, clinical practice and research in the past two decades have made it possible to create models of care that benefit children and adolescents. In Boys Don't Cry, Brandon could not avail himself of this type of help and support, which includes an integrated programme of psychological, social and physical interventions. The tragedy portrayed in the film clearly shows the need for making professional services available to people with gender identity problems and for educating society at large about these unusual life experiences.
Multiple choice questions
-
1. Gender identity disorders in children and adolescents are:
-
a frequent conditions
-
b phase of ordinary development
-
c precursors of adult transsexualism in all cases
-
d uncommon conditions
-
e more prevalent in boys than in girls.
-
-
2. The outcome of gender identity disorders in childhood is:
-
a transsexuality only
-
b transsexuality and homosexuality only
-
c transvestism and transsexuality only
-
d transsexuality, homosexuality, bisexuality, transvestism and heterosexuality
-
e paraphilias in adulthood.
-
-
3. Gender identity disorders are:
-
a usually pure conditions
-
b often associated with behavioural and relationship difficulties
-
c linked to a clear and well-defined aetiology
-
d commonly associated with sexual abuse
-
e caused by parental attitude and expectations
-
-
4. Atypical gender identity organisation is:
-
a present in all children who only cross-dress
-
b an alternative for the concept of core gender identity
-
c a research instrument
-
d useful in clinical management
-
e a less intense presentation of gender identity disorder.
-
-
5. The clinical management of gender identity disorders in children and adolescents involves:
-
a hormonal treatment only
-
b preparation for surgical intervention in all cases
-
c a staged approach, including psychosocial and physical interventions
-
d psychotherapy only
-
e the prevention of other symptoms and behavioural difficulties.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
| a | F | a | F | a | F | a | F | a | F |
| b | F | b | F | b | T | b | T | b | F |
| c | F | c | F | c | F | c | F | c | T |
| d | T | d | T | d | F | d | T | d | F |
| e | T | e | F | e | F | e | F | e | T |







eLetters
No eLetters have been published for this article.