Assessment of development constitutes one of the core components of any psychiatric evaluation. This is because evaluation of psychopathology generally entails determining the extent to which behaviours and experiences are appropriate for an individual's age and stage of development and because developmental disorders are common and frequently associated with psychiatric and behavioural disorders. I will describe methods of evaluating and diagnosing developmental disorders, but the principles and techniques also apply to evaluating development during any comprehensive psychiatric assessment.
The main developmental disorders classified in ICD–10 (World Health Organization, 1993) are summarised in Box 1. Disorders characterised by global delays in development (e.g. mild, moderate, severe and profound forms of ‘mental retardation’) are distinguished from disorders that affect specific functional domains (e.g. specific disorders of speech and language, scholastic skills or motor function), as well as from conditions that exhibit distinctive patterns of deviation from the normal developmental trajectory (e.g. the pervasive developmental disorders). The conditions are not mutually exclusive, however, and varying degrees of overlap may occur. Frequently, therefore, it is necessary to evaluate the extent to which development is progressing at the right rate, as well as the extent to which it is following the correct path.
Box 1. ICD–10 classification of developmental disorders
Mental retardation
Mild
Moderate
Severe
Profound
Pervasive developmental disorders
Autism
Atypical autism
Asperger's syndrome
Disintegrative disorder
Rett's syndrome
Other and unspecified
Specific developmental disorders
Speech and language: articulation; expressive speech; mixed expressive and receptive speech
Literacy: reading; spelling
Numeracy
Motor coordination
Mixed specific developmental disorder
Approaches to assessment
General principles
To establish an accurate understanding of developmental progress, it is best to obtain information from a variety of sources (parents, teachers, other professionals) and to use a number of different methods of gauging progress (developmental history, current functioning by report and on specific tests). This may require input from a range of professionals (psychiatrists, psychologists, speech/language and occupational therapists, physiotherapists) and entail some form of multi-disciplinary evaluation. Before an assessment, it is helpful to obtain details of any earlier assessments conducted by other professionals (e.g. speech therapists, educational and clinical psychologists and developmental paediatricians) and to review the reports from these evaluations. The information in these reports can be useful in filling in gaps in the developmental history, when parents have forgotten aspects of the child's early development, and in cross-checking the accuracy of the parents' recall of the child's behaviour with contemporaneous descriptions.
It may be necessary to undertake an initial evaluation, and then supplement this with further assessments selected to address specific issues. This can prevent unnecessary testing and can have the added advantage that conducting evaluations at different times and in different settings makes it possible to determine the extent to which difficulties are persistent and context-dependent.
Assessing the significance of delays and deviations in development
There are several ways in which the significance of delays and deviations can be assessed. First, the age at which milestones in development were achieved can provide a yardstick to the pace of development. For example, the ages at which the child was first able to sit, walk and speak can be compared to the normal range, to determine whether or not they were out of the ordinary. Second, standardised tests of development can be administered to check how much the child's current functioning is consistent with expectations. Ordinarily, these tests use some statistically determined cut-off point (often a score falling more than two standard deviations below the mean) to differentiate abnormal delays from normal variations in development. Third, the duration, pervasiveness and modifiability of symptoms and signs, as well as the extent to which they are associated with impairments in social role functioning, can be used to judge the significance of any deviations from the normal path of behavioural development.
Obtaining a developmental history
Interviewing parents or other informants about a child's early developmental history should be approached with two issues in mind. First, there is the need to ensure that the interview is conducted in a way that helps the parent/informant to remember details of the child's development and the timing of events as accurately as possible. Not surprisingly, perhaps, parents are better at recalling whether a milestone has been reached or behaviour exhibited than they are at recollecting the child's age when this happened. To improve their recall for the timing of events, it can be helpful to forewarn parents that you will be asking about these details when you meet with them and that they may find it helpful to bring to the interview baby books, etc. In addition, it is often helpful to get parents to focus on specific events that took place, as these can act as anchor points for dating milestones. For example, ask the parents to focus on events such as the first birthday, the birth of a sibling, move of home or change of job, and then to describe memories of the child's behaviour and abilities on these occasions. Cross-checking that the details reported on one occasion are consistent with descriptions obtained about another event closely related in time is also a useful way of ensuring that the report is accurate. For example, when a sibling was born at around the time of the child's second birthday, ask for descriptions of the child's behaviour on both occasions and compare them.
The second issue concerns parents' perceptions and preconceptions about the child's developmental status and behaviour. Not infrequently, the meaning of behaviours or skills is not fully appreciated by parents, and achievements may be imbued with special but unwarranted significance. The onus is on the clinician, therefore, to obtain a descriptive account of the child's behaviour rather than an account of the parents' views on the abilities of their child. Clearly, the clinician must be familiar with the key milestones in development, as well as the signs and symptoms of abnormal deviations from the developmental pathway. This ensures that appropriately focused questions are asked and that the coverage is comprehensive.
Framework for assessing development
It is useful to use a framework for collecting and collating information. Boxes 2, 3 and 4 summarise schemes for evaluating different aspects of the development of communication and social skills, as well as patterns of play, interests and activities. Box 5 summarises approaches to cognitive assessment, and Box 6 discusses the procedure for making a differential diagnosis. More detailed accounts of approaches to taking a developmental history are given by Rutter (1985), and descriptions of the psychometric tests used for assessing development, along with their relative merits, are reported by Sparrow & Davis (2000) and Volkmar & Marans (1999).
Box 2. Assessing communication skills
Milestones
Comprehension of speech: hearing; listening and attention; understanding instructions
Vocalisation and babble
First words
Phrase speech
Functioning at 4–5 years
Understanding: complexity of instructions followed
Number of words
Complexity of phrase speech: grammar and semantics
Articulation and intelligibility of speech
Abnormal qualities to speech: pronoun reversal; immediate and delayed echolalia; neologisms; stereotyped and repetitive speech; idiosyncratic phrases
Pragmatics
Conversational turn-taking
Social chat
Narrative skills
Meshing speech in dialogue
Intonation
Gesture
Linking of verbal and non-verbal communication
Box 3. Evaluation of social skill development
Milestones
Social smiling
Attachment behaviours: secure base; distress on separation; seeking comfort
Stranger wariness
Joint attention
Functioning at age 4–5 years
Social approaches and responses: frequency and circumstances; quality
Reciprocity in social interaction: use of eye gaze and contact to regulate interaction
Social disinhibition/ inappropriateness
Recognition of facial and vocal expressions of emotions
Integration of facial and vocal expressions of emotion
Current functioning (following schema at 4–5 years)
Understanding of emotions
Understanding of social roles and relationships: empathy; insight
Box 4. Assessing the development of interests, activities and play
Milestones
Giving and showing
Symbolism and pretence
Parallel play
Joint interactive play
Age 4–5 years
Social aspects: interest; playfulness; reciprocity; enjoyment
Cognitive level: curiosity; grasp; complexity (rules; drawing; puzzles; inventiveness); imagination (spontaneity; pretence; creativity)
Content, type and quality: initiation; flexibility; rituals/routines; odd preoccupations; unusual attachments; resistance to change; repetitive stereotyped movements; unusual sensory interests
Current function
Adapt schema from age 4–5 years
Circumscribed interests (timetables, fixtures, results, scores, listings, classification, categorisation)
Collecting and hoarding
Box 5. Observational and cognitive assessment
Observational assessment
Settings: with family; psychiatric interview; cognitive testing; school/assessment unit
Special assessments: Autism Diagnostic Observation Schedule – Generic
Cognitive evaluation
Social maturity: self-help; skills; use of objects; test (Vineland Adaptive Behaviour Scales)
Play: history; test (the Symbolic Play Test)
Intelligence: history; tests (Mullen scales; Wechsler Preschool and Primary Scale of Intelligence – Revised; Wechsler Intelligence Scale for Children–111; Wechsler Adult Intelligence Scale–111; Wechsler Abbreviated Scale of Intelligence)
Language: history; tests (Reynell Developmental Language Scales, Clinical Evaluation of Language Fundamentals – revised; Wechsler Objective Language Dimensions)
Scholastic attainment: history; tests (Wechsler Objective Reading Dimensions; Wechsler Objective Numerical Dimensions)
Attention: history (e.g. Strengths and Difficulties Questionnaire); test (Every Day Attention for Children)
Motor coordination: history; physiotherapy assessment; examination; Motor Assessment Battery for Children
Box 6. Making a diagnosis
Determine age, intellectual and cognitive level
Make diagnoses, if appropriate, of: mental retardation (mild, moderate, severe, profound); specific developmental disorder (motor, language, literacy, numeracy)
Is the child's behaviour appropriate for: chronological age; mental age; language level
If not, make Axis I diagnosis according to: pattern of language development; pattern of social development; pattern of interests/activities; other behaviours
Identify relevant medical conditions
Identify relevant psychosocial factors
The framework for obtaining a developmental history described here focuses on three key phases. The interviewer asks the parents first for details about the child's early development, then for a description of the strengths and weaknesses of the child at age 4–5 years and finally for an account of the child's current abilities. This scheme clearly needs to be adapted according to the child's age. The decision to focus on the child's behaviour at the age of 4–5 years is based on the fact that the child will usually have developed quite a wide range of skills and behaviours by this age, so the overall pattern is fairly clear. In addition, however, the developmental profile at this age is quite predictive of future progress, so the details can be used to advise about prognosis. Moreover, this is the age at which children in the UK begin schooling, so it can act as a convenient anchor point for the parents' recall.
A relatively recent advance has been the development of specific interview schedules and observational measures for diagnosing pervasive developmental disorders. As yet, they have mainly been used in research investigations, but they are increasingly being used in clinical settings and further refined for clinical purposes. The most established instruments currently used are the Autism Diagnostic Interview – Revised (Reference Lord, Rutter and Le CouteurLord et al, 1994) and the accompanying observational schedule, the Autism Diagnostic Observational Schedule – Generic (Reference Lord, Pickles and McLennanLord et al, 1997). Each schedule contains a set of prespecified codings that are scored according to operationalised rules. The scores are then combined in diagnostic algorithms to produce ICD–10 diagnoses. Quite intensive training is required to use them properly.
Communication skills
The aim of assessment is to determine whether development of speech comprehension was impaired (signifying a potential receptive language disorder), production of speech was delayed (signifying an expressive language disorder), or pronunciation and articulation were abnormal (signifying an articulation disorder). Also, development of the child's pragmatic skills or socio-communicative use of speech is evaluated, as impairments in these abilities are suggestive of a pervasive developmental disorder.
Care needs to be taken when questioning about speech comprehension that the child is not using context and non-verbal cues as clues to the meaning of verbal instructions. Asking whether the child is able to follow instruction when in another room and unable to see the parent may help clarify this.
The child's speech should be evaluated in terms of vocabulary size, the syntactic and grammatical complexity displayed (e.g. past, present and future tenses, the use of prepositions) and the ability to articulate words and phrases (e.g. how understandable the child's speech is to others). As parents are able to follow very poorly articulated speech, it is important to determine how easily strangers understand what the child says.
Specific speech and language disorders are often characterised by a mix of problems in each aspect of speech (comprehension, production and articulation), so careful assessment of each facet is required. Enquiry about qualitative abnormalities in speech development is especially important in diagnosing pervasive developmental disorder. Examples include: persistent echolalia (repetition of phrases just heard or picked up from the television or radio); neologisms (creation of completely novel words that are used consistently to mean something, e.g. the word ‘willip’, referring to a night dress; this does not include use of accepted mishmash words like ‘brunch’, or creation of words similar to this, derived from the juxtaposition of two other words); pronoun confusion (e.g. saying you instead of I, or he instead of she); and idiosyncratic or metaphorical speech (an unusual way of describing things, e.g. hot rain to mean steam from the kettle or oval sizzlies to refer to fried eggs).
Pragmatic skills relate to the social aspects of communication: that is, the speaker's ability to take the listener's perspective into account during a conversation. For example, does the individual introduce the topic of conversation and pitch what he or she says at a level appropriate to the listener's knowledge base? Does he or she check that the listener is following what is said and signal, using intonation and linked non-verbal signals such as eye gaze, that he or she is about to give the listener space to say something in response? How well does the speaker mesh what he or she says with the comments of other people? How much does he or she modulate what is said according to the social context (e.g. being in church or within earshot of other people, or according to the age and status of the conversational partner)? When a conversation breaks down, what strategies does the speaker use to repair it? Does the speaker vary intonation to aid expressiveness and use gestures in a related demonstration of what he or she is talking about or to add emphasis to what is said?
Social skill development
A rich but subtle repertoire of social behaviours emerges in early infancy. Attachment behaviours (6–12 months) and stranger wariness (9–12 months) are among the clearest manifestations of early social development, and are soon augmented by a growing range of social skills and behaviours. Most people are familiar with the notion of social maturity and the extent to which people ‘act their age’, but far fewer appreciate that there may be qualitative and distinctive abnormalities in social development. Although these may be manifest in quite subtle ways, they are nevertheless associated with very severe impairments in the individual's ability to integrate socially and establish friendships and love relationships. Abnormalities of this kind constitute one of the key components of the pervasive developmental disorders, and autism is the prototypical form of this group of conditions. Recent genetic research has shown that the traditional diagnostic boundaries for autism were too narrowly defined: the genetic liability to the condition confers a risk for the development of a broader spectrum of impairments in social communication skills, coupled with unusual patterns of interests (Reference Bolton, Macdonald and PicklesBolton et al, 1994; Reference Bailey, Le Couteur and GottesmanBailey et al, 1995). This spectrum probably includes atypical forms of autism and Asperger's syndrome, as well as even more subtle deficits, but there remains uncertainty as to quite how far the boundaries should be extended. The findings highlight the need to evaluate social functioning carefully, particularly the reciprocity of social interactions. The view that individuals with autistic spectrum disorders are always socially aloof is common, but inaccurate. They may instead be rather passive or ‘active but odd’ in social interactions (Reference Wing and GouldWing & Gould, 1979). This means it is necessary to get detailed descriptions of the way in which the individual makes and responds to social approaches and engages in what has been called the ‘social dance’. People, especially parents, are extremely good at adapting their behaviour and integrating it with a child's. Moreover, children with autistic spectrum disorders are able to learn basic social rules and the way to greet or part from people. Great care needs to be exercised, therefore, in obtaining accurate descriptions of the child's behaviour across a range of situations, as otherwise it is possible to overlook some of these subtle abnormalities. In older children and adults the problems may principally be evident in social understanding, empathy and insight.
Interest patterns, activities and play
The task here is to assess whether the child's interests, activities and play are appropriate to their mental age and whether there is any evidence for rituals, routines, circumscribed interests, resistance to change in the environment or a lack of imagination or creativity in play. The unusual interests and activities seen in children with autistic spectrum disorders may not be very marked in early childhood, becoming more obvious only when the child reaches 4–5 years. When present at a young age, the special interests are often focused on videos and the child shows intense excitement at specific sequences and insists on watching them over and over again. During the early years, play is frequently very repetitive and lacking in imagination and creativity. Not uncommonly it entails re-enacting activities seen on television or video or taught activities (e.g. tea parties). There tends to be little if any pretend play, unless it is led by another child or it represents a literal re-enactment of a film character's part.
Difficulties can arise in deciding when a childhood interest or hobby is more than just a craze or fashion, as well as in differentiating obsessive–compulsive phenomena from the rituals and routines found in children with pervasive developmental disorders. As a general guide, autistic-like interests and hobbies are unusual in their content and are pursued intensively, excessively and repetitively, to the exclusion of other activities. In addition, the interest or activity is often followed in a solitary manner, without any desire to share experiences with others. Similarly, distinctions between obsessive–compulsive phenomena and autistic-like rituals and routines are made on the basis of their content and the manner in which the behaviours are manifest. Thus, isolated contamination fears with repeated hand-washing, evening-up phenomena or complex compulsions involving counting or touching things in special sequences would not usually typify an autistic-like ritual or routine. More often, the interests and rituals focus on specific objects, such as lamp-posts, fans, toilets, lights, washing machines, trains, routes, dates and lists, as well as on collecting and categorising things. Moreover, the interests are pursued willingly and without any attempt to resist doing them. Frequently, there will be a long history of these rituals and routines, although the focus of interest may change from time to time. Resistance to changes in the environment may be manifest in an insistence that objects or ornaments be placed in specific locations in the house.
Observation and cognitive evaluation
As outlined in Box 5, it is important to observe the child in a variety of contexts (e.g. with their family, on their own, in school and at the clinic), as well as to observe how they manage in situations that vary in the amount of structure provided (e.g. during cognitive and behavioural evaluation, play and mental state assessment). Cognitive assessments by a clinical psychologist and speech/language therapist may require several separate appointments. Test results should not be considered in isolation, but interpreted in the light of all available information. A variety of psychometric tests have been developed to evaluate cognitive functions, and in addition to the few outlined here there are numerous others available for identifying more specific neuropsychological deficits. Cognitive testing is usually possible if undertaken by a skilled psychologist using ingenuity and patience (Reference Berger, Rutter, Taylor and HersovBerger, 1994). It is important to start with items that are within the child's capability, so that he or she does not lose interest and heart; it is also important to ensure that rewards for participating in the tests are provided. Care must be exercised in selecting tests tailored to the child's age and abilities. When children with severe problems or autism are being evaluated, tests that entail complex verbal instructions are best avoided.
The results of tests aimed at evaluating specific cognitive skills, such as speech, language, literacy and numeracy, must be interpreted in the context of the individual's general level of intelligence. This is because the diagnosis of a specific developmental disorder is based on demonstrating that the child's abilities fall below those expected according to their age and intelligence. The recent editions of the Wechsler intelligence scales and the accompanying tests of language, literacy and numeracy are well suited for this purpose, as they have been specifically developed to be used together (Reference WechslerWechsler, 1989, Reference Wechsler1991, Reference Wechsler1993, Reference Wechsler1996a ,Reference Wechsler b , Reference Wechsler1997a ,Reference Wechsler b , Reference Wechsler1999). Other useful tests (see Box 5) include the Mullen Scales (Reference MullenMullen, 1995), the Clinical Evaluation of Language Fundamentals – Revised (Reference Semel, Wiig and SecordSemel et al, 1980), the Reynell Developmental Language Scales (Reference ReynellReynell, 1990), the Symbolic Play Test (Reference Lowe and CostelloLowe & Costello, 1976), and the Vineland Adaptive Behaviour Scales (Reference Sparrow and CicchettiSparrow & Cicchetti, 1985). Motor coordination can be assessed using the Movement Assessment Battery for Children (Reference Henderson and SugdenHenderson & Sugden, 1982).
Medical investigations
Developmental disorders are often the result of specific medical conditions, and the identification of an underlying cause can have important implications for management, prognosis and risk of recurrence. The choice of appropriate tests to identify these conditions has to be guided by the history and results of physical examination, as well as the expected yield and invasiveness of the procedure. This issue has been the subject of some debate in the investigation of autistic spectrum disorders, with some clinicians advocating that an extensive medical work-up (e.g. brain scans and lumbar punctures) should always be conducted (Reference Gillberg and ColemanGillberg & Coleman, 1996). By contrast, the majority favour a much more limited set of investigations (Reference Rutter, Bailey and BoltonRutter et al, 1994; Reference Barton and VolkmarBarton & Volkmar, 1998). The likelihood of identifying a medical condition is related to the severity of the developmental disorder and is greatest in people with severe and profound degrees of handicap.
Other assessments
Individuals with developmental disorders are at increased risk of a range of behavioural and emotional disturbances, as well as serious psychiatric disorders. Clearly, evaluations aimed at picking up symptoms and signs of these comorbid conditions also have to be conducted. The challenge often lies in the fact that the presence of developmental problems restricts the individual's ability to describe his or her mental experiences, so it is sometimes only possible to assess the nature of any behavioural change. A systematically gathered history from an informant who knows the individual well can go a long way in mapping out the nature of the accompanying psychopathology and narrowing down the options, especially when accompanied by careful observational assessments.
Making a diagnosis
The results of both the observational assessments and cognitive tests need to be considered in conjunction with the details obtained in the developmental history. Results from any one source of information should not be considered to provide a more accurate picture than those from any other. Inconsistencies between the sources of information in the pattern of impairments identified should lead to further investigation until the reason for the differences is explained.
The procedure for making a diagnosis is summarised in Box 6. In essence, it entails a stepwise approach. First, the individual's intellectual level is determined and classified according to the degree of learning disability, if present. The same is done for the language level. A diagnosis of a specific language disorder should be considered if the individual's performance on a test of language falls significantly below that expected for his or her chronological age and intellectual level. The specific subtype is determined according to the particular mix of impairments (Reference Bishop, Rutter, Taylor and HersovBishop, 1994).
Next, it is necessary to determine whether the child's social, communication and play development are consistent with his or her chronological, mental and language age. If not, then various Axis I psychiatric conditions should be considered. The principal diagnoses to consider are those falling under the general category of pervasive developmental disorders and several conditions that bear some resemblance to them (e.g. selective mutism, attachment disorders, childhood schizophrenia) (Reference Lord, Rutter, Rutter, Taylor and HersovLord & Rutter, 1994). Differentiation between the various conditions is based on age at onset, the nature, mix and severity of problems and the presence of accompanying deficits. Thus, the autistic spectrum disorders typically have an onset within the first 3 years of life. Usually, onset is insidious, with no clear beginning, but in about a third of cases a faltering or minor setback in development is reported at some point in the second year. By contrast, the disintegrative disorders of childhood have a rather later and more dramatic onset. Usually, development is reported to be normal for the first 2 years at least, and the child attains quite a range of language and social skills. This is followed by a marked regression in behaviour, accompanied by a loss of cognitive skills as well as bladder and bowel control. Neurological conditions are sometimes identified as the cause of the disintegrative disorders, so this pattern of onset should alert the clinician to the need for more detailed medical work-up (Reference Malhotra and GuptaMalhotra & Gupta, 1999). Another disorder that sometimes presents with similarities to autism, but has a distinctive onset, is the syndrome of acquired aphasia with epilepsy, or Landau–Kleffner syndrome (Reference Bishop, Rutter, Taylor and HersovBishop, 1994; Reference TuchmanTuchman, 1997). Typically, expressive and receptive language are lost over a period of weeks or months and following a normal period of early development. In most cases there are a few seizures and generalised electroencephalogram abnormalities at the time of onset, but neither tend to persist. Sometimes the language abilities fluctuate along with the seizures. More often, however, the child is left with a profound receptive language impairment, but comparatively normal social reciprocity and general intelligence. Yet another syndrome that has a pattern of onset different from that of classic autism is Rett's syndrome. This is probably exclusive to girls, and the X chromosome gene abnormality responsible for the condition has recently been identified (Reference Amir, Van den Veyver and WanAmir et al, 1999; Reference Hagberg, Berg and SteffenburgHagberg et al, 1999). Development is reported to be normal for the first 6 months, but then there is a behavioural and intellectual regression that is accompanied by a deceleration of head growth and the emergence of midline hand-wringing and hand-washing stereotypies. Sometimes the child begins to walk, but then temporarily loses this ability. A kyphoscoliosis can develop. The child is usually profoundly handicapped.
Cases that fail to meet full criteria for a diagnosis of autism, but nevertheless have quite a few features of the syndrome, are relatively common and outnumber the cases that meet full diagnostic criteria (Reference FombonneFombonne, 1999). Fairly frequently these individuals have severe or profound degrees of mental retardation or a mental age of less than 2 years, by virtue of their young age and general developmental delay. In such circumstances it is hard to determine the extent of deviance in development because the delays are so marked and there is such a limited repertoire of behaviours on which to base a judgement. If these individuals meet criteria in two of the three symptom domains (communication, social and play), they are classified as having atypical autism. If they fail to meet criteria in more than two areas, but nevertheless have impairments that are evident in all three symptom domains, then they can be considered to have a pervasive developmental disorder not otherwise specified. Much the same approach is adopted at the other end of the autistic spectrum, where cases are of normal intelligence but fail to meet all the criteria for a diagnosis of autism. However, in these circumstances the diagnosis of Asperger's syndrome also needs to be considered. This diagnosis is reserved for individuals of normal intelligence who meet the criteria for a diagnosis of autism in the social symptom domain and who also exhibit circumscribed interests. However, in contrast to individuals with autism, they do not show delays in early language development and in general have good language skills, apart from a rather deviant style of communication that is predominantly characterised by pragmatic impairments. Asperger's syndrome bears very close similarities to autism, and it is likely that it will eventually be shown to represent a mild variant of the syndrome. As this has not yet been firmly established, however, and as it is unclear how to demarcate Asperger's syndrome from normal variations in personality development, it is separately classified.
Four other disorders warrant brief consideration: selective mutism, reactive and disinhibited attachment disorders and childhood schizophrenia. Typically, children with selective mutism present at around the age of school entry. They apparently communicate well in some situations (usually the family home), but are mute in others (at school or when strangers visit). Social reciprocity and play are, however, normal.
Children who have been seriously neglected and abused or raised in poor-quality institutional homes exhibit abnormalities in their attachments and peer relationships. Abused children who develop a reactive attachment disorder may be hypervigilant and wary of people, but also aggressive towards peers. They exhibit very contradictory and ambivalent social responses to caregivers. Children with a disinhibited attachment disorder are rather indiscriminate in their social approaches and have difficulties in developing selective attachments. It is thought that this pattern of attachment may develop as a response to the frequent changes in caregivers that take place in children's homes. In both cases the children exhibit normal social reciprocity in some situations and none of the typical autistic-like abnormalities in language usage.
Very early-onset childhood schizophrenia has recently been described in this journal (Reference HollisHollis, 2000). The main features that differentiate this condition from the developmental disorders considered here are: the relatively good social relationships developed; the extent of reciprocity in social interactions (especially with regard to eye gaze); the presence of positive features of schizophrenia such as thought disorder; and the presence of a family history of schizophrenia.
Conclusions
Developmental disorders are common, often complex in form and not infrequently accompanied by comorbid psychiatric and behavioural disturbances. Assessment must be undertaken carefully and systematically by a multi-disciplinary group of professionals. A developmental history based on detailed descriptions of the child's behaviour at key stages in early and middle childhood is one of the cornerstones of evaluation, but it should be supplemented by observational and cognitive assessments. Particular attention should be given to the consistency of the picture obtained from different sources and the overall pattern of development. A stepwise approach to differential diagnosis helps prevent the confusion threatened by the plethora of possibilities.
Multiple choice questions
-
1. A high-quality developmental history:
-
a requires the interviewer to get descriptions of the child's behaviour
-
b is the best source of information for making a diagnosis
-
c is easier to obtain for details concerning whether, rather than when, something happened
-
d can be structured to focus on specific phases of development.
-
-
2. Psychometric testing of presenting children:
-
a may be impossible
-
b is useful for diagnosing specific cognitive disorders
-
c may be all that is required to make a diagnosis
-
d is not always necessary.
-
-
3. Observational assessments:
-
a help confirm details obtained by report
-
b can provide information about context specificity
-
c have been developed for the assessment of pervasive developmental disorders
-
d are best done in a very structured way.
-
-
4. Autistic spectrum disorders:
-
a have diagnostic criteria extending more widely than previously
-
b are always characterised by social aloofness
-
c can be difficult to differentiate from reactive attachment disorders
-
d warrant intensive medical investigation.
-
MCQ answers
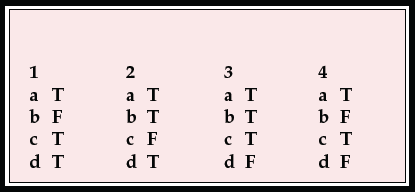
| 1 | 2 | 3 | 4 | ||||
|---|---|---|---|---|---|---|---|
| a | T | a | T | a | T | a | T |
| b | F | b | T | b | T | b | F |
| c | T | c | F | c | T | c | T |
| d | T | d | T | d | F | d | F |





eLetters
No eLetters have been published for this article.