Over recent years early intervention in psychosis has fired the imagination of clinicians and researchers, following the publication of several studies linking a long duration of psychosis prior to receiving treatment with a poor treatment outcome: a relationship that has been cogently argued to be independent of illness factors (e.g. Scully et al, 1997). Most influential was Wyatt's (1991) review of 22 studies, in which relatively similar groups of patients suffering from schizophrenia were, or were not, given antipsychotic medication early in the course of their illness. This pointed towards an improved long-term course in schizophrenia with early treatment.
At the same time, evidence was emerging that the early phase following the onset of a first psychotic illness could be conceived of as a critical period, influencing the long-term course of the illness. During this period individuals and their families may also develop adverse psychological reactions to psychosis and the circumstances of its management. It was therefore proposed that timely and effective intervention at this stage might alter the subsequent course of the illness (Reference Birchwood, Todd and JacksonBirchwood et al, 1998). The early intervention concept has even been extended, with some success, in an attempt to identify people experiencing the prodrome of a first episode of psychosis (Reference Yung, Phillips and McGorryYung et al, 1998).
These developments resulted in the establishment of specialised services for the management of first-episode psychosis, notably in Australia and Scandinavia. In the UK, the National Service Framework for Mental Health stresses the necessity of prompt assessment of young people at the first sign of a psychotic illness, in light of the “growing evidence that early assessment and treatment can reduce levels of morbidity” (Department of Health, 1999: p. 44). The Government's plan for the National Health Service (NHS) specifically targets the funding of 50 early intervention services by 2004.
The primary aims in the management of first-episode psychosis are detailed in Box 1. In this paper, we will describe best-practice principles for the management of first-episode psychosis, illustrating them with reference to their application in our service, the Birmingham Early Intervention Service. This is the UK's first dedicated service for young people with a first episode of psychosis, which has recently been granted NHS Beacon Service status.
Box 1. Aims in the management of first-episode psychosis
To reduce the time between onset of psychotic symptoms and effective treatment
To accelerate remission through effective biological and psychosocial interventions
To reduce the individual's adverse reactions to the experience of psychosis and to maximise social and work functioning
To prevent relapse and treatment resistance
The Birmingham Early Intervention Service
This service takes clients aged between 16 and 35 years, who are experiencing their first episode of psychosis and are also in their first year of treatment by mental health services. It is one of a number of functionalised teams within Northern Birmingham Mental Health Trust and it provides clients with comprehensive and streamed mental health care for a 3-year period, the initial ‘critical phase’ of psychosis. It serves an inner-city catchment area of high psychiatric morbidity with a multi-ethnic population (about 28% African-Caribbean and 30% Asian). Research in similar populations has shown that African-Caribbean patients in particular may be poorly engaged with traditional mental health services (Reference McGovern and CopeMcGovern & Cope, 1991).
At the core of the service is an assertive outreach team consisting mostly of community psychiatric nurses (CPNs). They act as keyworkers, with support from multi-disciplinary health professionals and ex-service users. The service, in conjunction with a youth housing agency, also operates a community-based respite unit. Within this context we deliver intervention programmes, including protocol-based pharmacotherapy, family work, social recovery, work and training schemes and cognitive therapy.
Best-practice management of first-episode psychosis
The principles detailed in Box 2 are drawn from the literature on early intervention in psychosis. These are further elaborated in a set of clinical and service guidelines for use in the West Midlands, prepared by the Initiative to Reduce the Impact of Schizophrenia (IRIS) team. An audit tool to assess the adherence of services to these guidelines has also been prepared (both are available from M.B. upon request).
Box 2. Principles for best-practice management of first-episode psychosis
A strategy for early detection and assessment of frank psychosis
A specific focus on therapeutic engagement
A comprehensive assessment
An embracing of diagnostic uncertainty
Treatment in the least restrictive setting using low-dose medication
Strategy for early detection and assessment of frank psychosis
The pathway to care in first-episode psychosis can be long and traumatic, and most people have active psychotic symptoms for 1–2 years before treatment (e.g. Larsen et al, 1996). Long duration of untreated psychosis is associated with ineffective and demoralising help-seeking and a variety of traumatic events, including high rates of involuntary hospital admission (Reference Johnstone, Crow and JohnsonJohnstone et al, 1986).
A strategy identifying pathways from the onset of psychosis to successful engagement with specialist treatment is vital: this may reveal circuitous and undesirable routes and opportunities for earlier intervention.
In the UK, most cases of first-episode psychosis pass through primary care, so the interface with secondary care is of particular interest. However, British data on the treatment of first-episode psychosis in general practice are sparce. Studies of schizophrenia in primary care describe problems with reviewing psychiatric status and difficulties of communication with secondary services (Reference Lang, Johnstone and MurrayLang et al, 1997). Overseas data suggest that general practitioners (GPs) have a low index of suspicion of the presence of psychosis and little confidence in making the diagnosis and that they see mental health services as slow to respond to referrals (Reference Lincoln and McGorryLincoln & McGorry, 1995).
A number of strategies have been used to strengthen the links between primary and secondary care for people with serious mental illness. One such strategy has been the introduction of standards for and audit of communication between the two services and the development of shared care. These could become part of contractual arrangements (Reference Bindman, Johnson and WrightBindman et al, 1997). Another has been to site a liaison CPN within primary care, taking care to ensure that the appropriate patient group is prioritised (Reference Lang, Johnstone and MurrayLang et al, 1997). The Early Psychosis Prevention and Intervention Centre (EPPIC) programme in Melbourne, Australia, has published on the internet guidelines for GPs on the early detection and management of psychosis (http://home.vicnet.net.au/~eppic/).
The Birmingham Early Intervention Service is developing a shared-care programme with local GPs that involves GP training, increased communication regarding client progress and treatment and shared care of selected clients after a period of intensive management by the early intervention service. The service also maintains good relationships with the local police and has conducted some training with them in the recognition of psychosis. Regular audits of pathways to care are conducted.
Focus on therapeutic engagement
Engagement, or the formation of a therapeutic alliance, is an independent predictor of treatment retention rates and a range of good of symptomatic and functional outcomes in psychosis. However, it is difficult to achieve (Reference Frank and GundersonFrank & Gunderson, 1990). In particular, young people doubt the usefulness of professional help, and their negative stereotypes of mental illness and fear of mental health services form barriers to self-referral (Reference Lincoln and McGorryLincoln & McGorry, 1995).
In the face of the failure of clients with first-episode psychosis to attend out-patient appointments or to take antipsychotic medication, the temptation to ‘wait and see’ is considerable. However, this approach often ends in a crisis and preventive opportunities are lost. For example, after a first episode of psychosis, clients who cease contact with mental health services are more likely to be readmitted under the Mental Health Act (Reference McGovern and CopeMcGovern & Cope, 1991).
There has been little systematic study of engagement of clients with first-episode psychosis. Opinion leaders in the field (e.g. Birchwood et al, 2000a), however, agree that it is fostered by a search for common ground with the client, an avoidance of a premature confrontation of their explanatory model of illness and the delivery of treatment in as flexible a manner as possible. If a client does not accept that he or she is ill, practical assistance and an initial focus on the resolution of a problem of importance to the individual, but unrelated to the psychotic disorder, may be helpful. Studies of substance misuse suggest that aspects of the service-delivery process, such as home visits, short waiting lists and frequent client contact with a single worker, can also maximise client engagement (e.g. Henggeler et al, 1996).
For the client to develop a positive, trusting relationship with a mental health worker, a single keyworker needs to be allocated as early as possible, regardless of whether the client is perceived as having ‘complex needs’. This worker should preferably be assigned for the entire ‘critical period’. Failure to take prescribed medication or attend appointments should not lead to reduced contact or discharge; in such cases contact should be increased. Staffing levels must take into consideration the fact that frequent contact is often needed to engage such clients.
Furthermore, since most people suffering from first-episode psychosis are young, best-practice services for early intervention must also be ‘youth attractive’. In their approach to the engagement of clients and in the interventions offered they should reflect youth culture and the legitimate aspirations of young people concerning work and autonomy.
The assertive outreach model provides a good structure for workers, and different aspects of the model encourage engagement. Low case-loads allow the time required for the development of a therapeutic relationship and for persistent follow-up of individuals in danger of being lost to services. The ‘team’ model, which demands that all the staff know all the clients, enables the best matching of staff skills to client needs as well as continuity of input when there are problems in particular relationships or breaks owing to holidays and so on. The use of extended hours and community outreach provides the flexibility to see patients at the most appropriate time and place. In our own service, keyworkers have an individual case-load of 15, somewhat higher than recommended in a strict assertive outreach model. All members of the team know all the clients. The service operates 7 days a week, with flexibility of hours if necessary. Workers attempt to engage the client on the basis of the latter's self-perceived needs, building on his or her strengths. Much of the work involves practical help with aspects of everyday life, including benefits and housing. Providing the majority of services within the team gives continuity, which enhances engagement. The team is involved with clients during admissions and the team psychiatrist is responsible for in-patient care. The service also employs former service users, to whom clients may better relate, as support workers. A vocational assistance programme led by an occupational therapist is available if needed. The client does not have to accept an illness model of psychosis for initial engagement, and cognitive-behavioural therapy (CBT) is available to address problems that the client perceives. The service also has a small social budget, which is very important in allowing keyworkers to engage with clients in low-stigma settings such as sporting events. This is also formalised in a weekly social recovery group. There is a staff v. clients football match most Friday afternoons, at which relatives and friends are welcomed as players or spectators.
Comprehensive assessment
The stress-vulnerability model conceptualises the development of psychosis as the action of social or psychological stressors acting on the vulnerable individual. This implies the need for a full assessment of mental state, risk and biological, psychological and social vulnerabilities and stressors.
People with first-episode psychosis often come to care after a prolonged symptomatic period that may have led to unstable living or financial circumstances. Furthermore, comorbidity with problems such as substance misuse, depression, suicidal thinking, social avoidance and phenomena similar to post-traumatic stress disorder (PTSD) are common, and need assessment and treatment both in their own right and because of their potential to act as stressors provoking relapse (Reference Birchwood, Todd and JacksonBirchwood et al, 1998).
In our service, initial assessment involves a traditional psychiatric history and mental status examination plus relevant physical investigations. However, assessment is not considered complete until information is obtained about the client's sense of stigma, his or her own explanatory model of the illness and view of the future. The individual's access to appropriate social resources, opportunities and social networks is also assessed, as are the current and ‘best ever’ levels of occupational functioning. Most clients will allow us to talk to their family, and the quality of family relationship is noted, as well as the family's attitude to, and understanding of, the client's illness. These data are summarised as the psychological and social needs and strengths of the client, the strengths and needs of the family and the client's own perception of his or her needs.
Embracing diagnostic uncertainty
The embracing of diagnostic uncertainty is crucial in work with first-episode psychosis, since many of the symptoms found in the prodromal or early stages of psychosis are sometimes found in normal teenagers (Reference McGorry, McFarlane and PattonMcGorry et al, 1995). For true early detection, referring agents must feel free to refer clients for expert assessment on the basis of a suspicion rather than a certainty of psychosis, and a low threshold for reassessment must be set.
The application of a diagnosis too early in the course of a functional psychosis not only has been found to be unreliable, but may also be harmful. The early course of psychosis is often characterised by changing symptoms, and premature diagnosis (e.g. of schizophrenia) tends to engender pessimism in clients, families and staff, which may exert a negative influence on the course of ensuing psychoses (Reference McGorryMcGorry, 1995).
Provided that organic causes of psychosis are excluded, a symptom-based approach to treatment has been advocated. This might include prescribing, for example, mood stabilisers in the presence of a full or partial affective syndrome. Decisions about diagnosis can then be deferred until some degree of symptom stability has emerged.
Our service, like most similar ones, has adopted the above practice. We have observed that clients generally find the term ‘psychosis’ more tolerable than ‘schizophrenia’ and we focus psychoeducation on risk and vulnerability factors for psychosis in general. A series of booklets have been developed for this purpose (available from M.B. upon request).
Treatment in the least restrictive setting using low-dose medication
McGorry et al (1991) found high levels of symptoms of PTSD following hospitalisation for an acute psychotic episode. It is therefore recognised that exposure of treatment-na¨ve patients to the adverse experiences associated with acute psychiatric wards must be minimised. While some services have tried to reduce the trauma for clients of an in-patient admission for first-episode psychosis by providing special nursing, single rooms and accommodation for family members, others have found treatment at home to be a viable alternative to hospitalisation.
For example, Fitzgerald & Kulkarni (1998) successfully treated 22 of 37 first-episode psychosis patients entirely at home, using home visiting as frequent as twice daily. The success of home-based treatment depended not on the degree of initial psychopathology, but on the degree of family support available to the client. In our service, we have used the 24-hour trust-wide home-treatment team to provide out-of-hours assistance to clients, with good results.
The aim of pharmacotherapy in first-episode psychosis should be to maximise the therapeutic benefit while minimising adverse effects. A number of guidelines for this can be drawn from the literature. These are listed in Box 3 and discussed in detail below.
Box 3. Recommendations for pharmacotherapy of first-episode psychosis
-
1 An antipsychotic-free observation period
-
2 A low threshold for the use of atypical antipsychotic medications
-
3 The use of low-dose antipsychotics plus benzodiazepines
-
4 The aim of remission
-
5 Early assessment of treatment resistance
-
6 Maintenance of medication for at least 1–2 years in non-affective psychosis (except in some cases with short duration of untreated psychosis)
-
1. If possible, have an antipsychotic-free observation period during which the diagnosis of psychosis can be confirmed and organic causes can be excluded. During this time benzodiazepines may be used for tranquillisation, as an alternative to antipsychotic medication.
-
2. At present, there is no methodologically sound evidence that novel antipsychotics (excluding clozapine) are more effective than conventional ones in treating the positive and negative symptoms of psychosis in unselected first-episode psychosis populations. However, they have been repeatedly found to cause fewer side-effects (e.g. Emsley, 1999), with resultant improved adherence to treatment. The escalating cost of atypical antipsychotics and their impact on service budgets have led to greater scepticism about their use, especially since trials have not compared their side-effects with those of very low-dose regimes of conventional antipsychotics. If conventional antipsychotics are chosen as a first-line treatment, a low threshold for change to atypical antipsychotics is needed in the face of extrapyramidal side-effects, poor response or non-compliance. Similarly, factors that may increase the likelihood of the early development of tardive dyskinesia (e.g. organic brain disease) should prompt the early use of atypical antipsychotics, which it is hoped will lead to a lower incidence of this side-effect (see Bebbington, 2000, for a review of the area).
-
3. The positive symptoms of most patients with first-episode psychosis will respond to 2–3 mg haloperidol equivalents daily, but they may take 2–4 weeks to do so. There appears to be no response advantage in exceeding doses of 6 mg haloperidol daily and doses above this are likely to cause unpleasant side-effects and potential non-compliance. Similarly, 2–4 mg risperidone daily should be adequate in most cases. There may be some advantage in prescribing higher doses of antipsychotics in the treatment of hostility, but benzodiazepines are to be preferred for this purpose owing to their absence of extrapyramidal side-effects (see Remington et al, 1998, for a review of the area).
-
4. With sufficiently assertive treatment involving changes in antipsychotics as necessary, symptoms in the vast majority (Lieberman et al, 1993, report 83% in their study) of patients with first-episode psychosis will remit. Therefore, remission of symptoms, not adjustment to them, should be the aim of treatment.
-
5. Studies have shown that, even with changes in antipsychotics (excluding clozapine), remission rates of positive and negative symptoms tend to plateau after 3–6 months of treatment following a first episode of psychosis (Reference Edwards, Maude and McGorryEdwards et al, 1998). Failure of symptoms to remit after 6 months of treatment with adequate doses of two antipsychotics (preferably including one atypical agent) and psychosocial input as appropriate should trigger prompt action. For example, review for unsuspected organic factors, mood disorder, substance misuse or non-compliance with medication: then consider using CBT and/or clozapine for persistent symptoms.
-
6. It is not clear for how long people with first-episode psychosis should continue maintenance antipsychotic medication. Current consensus guidelines suggest ceasing antipsychotics after 1–2 years of remission following a first episode of non-affective psychosis. Future guidelines may recommend a longer period of treatment, in light of Robinson et al's (1999) 5-year follow-up of people with first-episode schizophrenia, which showed that relapse rates rose quickly to 51% over the first 2 years after index admission, then plateaued to a certain extent, reaching 78% by 5 years. Some people with first-episode psychosis stay well with shorter periods of antipsychotic treatment (Reference Crow, MacMillan and JohnsonCrow et al, 1986). Identifying this group is a challenge for future research, but it is unlikely to include those who have had psychotic symptoms for more than 1 year prior to treatment (Reference Crow, MacMillan and JohnsonCrow et al, 1986).
Focus on pychological adjustment and maintenance of social roles
Adverse reactions to the experience of psychosis and its treatment, including depression, PTSD and suicide, are well established. While denial of illness may lead to non-compliance with medication and subsequent relapse, its acceptance can lead to pessimism, loss of self-efficacy and absorption of the pejorative stereotypes of mental illness (Reference Birchwood, Todd and JacksonBirchwood et al, 1998).
In our service, we use a theoretical framework focusing on individuals' appraisal of their illness in relation to ‘loss’, ‘humiliation’ and ‘entrapment’: this reveals their psychological adjustment to the illness (see Birchwood & Spencer, 1999, for a review of the area). We strive for a blame-free acceptance of illness, together with the encouragement of a sense of mastery over it. We aim to achieve this through client education in cognitive-behavioural strategies of symptom control, the management of early signs of relapse and highlighting and challenging cultural stereotypes of mental illness. Most of this is provided in the context of an ongoing therapeutic relationship with a keyworker and group psychoeducation.
Social roles and goals, particularly work, are highly prized by young people. They provide a source of self-esteem that can affect the psychosis itself (Reference WarnerWarner, 1994), and their loss has been linked to depression and suicidal thinking in psychosis (Reference Birchwood, Iqbal and ChadwickBirchwood et al, 2000b ). Since alleviating symptoms is no guarantee of a good social outcome (Reference Birchwood, Todd and JacksonBirchwood et al, 1998), clients must be given the opportunity to regain and develop life skills in a supportive milieu, particularly one in which a peer group is present. Preliminary results suggest positive effects from the EPPIC recovery programme, which is delivered in such a manner (Reference Albiston, Francey and HarriganAlbiston et al, 1998).
Our service has developed a structured approach to help clients enter paid employment. The service occupational therapist delivers an 8-week accredited pre-vocational training guidance programme, funded through a local college. A short, intensive work-preparation course has also been developed, which acts as the referral point to a specialised employment service for people with mental health problems. It is run by an agency linked to social services and the National Schizophrenia Fellowship. A less-structured approach is taken to social recovery, with social, cooking and mother and baby groups held weekly at our community base.
Focus on the entire family
Since most people with first-episode psychosis are young, many will be living with a family or partner. There is now little doubt that family interventions in schizophrenia are effective in postponing psychotic relapse over periods of up to 2 years. Furthermore, high levels of emotional distress are found among the relatives caring for a person with schizophrenia. Despite their obvious relevance, family interventions in first-episode psychosis remain underresearched (see Birchwood & Spencer, 1999, for a review of the area).
The traditional concepts, such as expressed emotion that form the rationale for family interventions, may be of less relevance in a family experiencing first-episode psychosis than are concepts involving trauma and loss. Indeed, the mitigation of loss and negative experiences of caregiving within such families in the early stages of psychosis may be crucial in order to prevent the development of a critical family atmosphere later.
In our service, we are in the process of training all keyworkers in skills-based family intervention, following Falloon's (1985) model. We also facilitate a monthly family and carer support group, as we found that families appreciate a forum in which to share their feelings of loss, guilt and confusion, drawing on support from similar families. Families seem to benefit more when this is driven by issues they themselves bring to the group, rather than by a structured ‘agenda’.
Prevention of relapse and resistance to treatment
It has been argued that the early course of psychosis is sharply predictive of its longer-term course, and that there may be a toxic effect of cumulative exposure to positive symptoms. Given this, the prevention of relapses and treatment resistance might alter the long-term outcome of psychosis, presumably by limiting the postulated neurotoxic effect of active psychosis (Reference WyattWyatt, 1991).
The basis of relapse prevention is the modification of stress and vulnerability factors by means of the best-practice interventions discussed above. Clients and their families should be informed about the risk factors, within the context of the stress-vulnerability framework. A shared and documented relapse prevention plan for each individual can then be developed and rehearsed with the client and his or her social network. An active relapse-monitoring procedure can also be instituted.
We have developed an approach to relapse prevention involving collaboration with the client and the family to identify the client's unique early warning signs of psychotic relapse and to prepare and rehearse a response to these. This response draws on cognitive therapy of emerging delusional themes and the use of coping mechanisms, drug interventions and resources within the family and treatment network (Reference Birchwood, Spencer and McGovernBirchwood et al, 2000c ).
A system for the early identification of treatment resistance is needed, so that a wait-and-see attitude is not encouraged beyond the appropriate period. This has been discussed above with respect to pharmacotherapy. Similarly, the early application of CBT should be encouraged, since controlled studies have found these to lead to a significant reduction in both the duration of an acute psychotic episode and persisting positive psychotic symptoms (see Birchwood & Spencer, 1999, for a review of the area).
On the basis of a study of time to recovery, the EPPIC programme has identified 3 months after initiation of treatment as the critical point at which the presence of persisting positive symptoms should motivate assertive action. Clients are screened for persisting positive symptoms at this time and, if they are present, they are referred to a specialised subservice (the Treatment Resistance Early Assessment Team; TREAT), which offers reassessment and a variety of interventions including CBT and assertive pharmacotherapy (Reference Edwards, Maude and McGorryEdwards et al, 1998).
Conclusion
Services dedicated to young people experiencing psychosis for the first time have not hitherto been afforded a high priority in routine psychiatric care. This is changing as it is recognised that the early phase is a stormy period in which disability and relapse flourish, and one often preceded by a long period without treatment. This, combined with the high risk of suicide, provides an ethical basis for improved practice. Accumulating evidence supporting the critical-period concept holds out the hope of improving early and long-term outcome by intensive early treatment. Early intervention does not simply involve ‘bringing forward’ best practice to this early phase; it requires special care in recognition of the biological, psychological and familial challenges and changes that are active in this period and that have informed these guidelines.
Multiple choice questions
-
1. The ‘critical period’ following a first psychotic illness is:
-
a the time during which individuals decide whether or not to stop treatment
-
b inversely related to the duration of untreated psychosis prior to admission
-
c a period during which relapse is common
-
d associated with increased risk of suicide
-
e a period when it is important to offer intervention.
-
-
2. In the pharmacotherapy of first-episode psychosis:
-
a it is often sufficient to treat with benzodiazepines
-
b novel antipsychotics are the first-choice treatment
-
c in most cases, remission of symptoms can be expected within 6 months
-
d symptoms often remit with low doses of an antipsychotic
-
e treatment can usually be safely stopped 6 months after remission of symptoms.
-
-
3. Best-practice management of first-episode psychosis includes:
-
a strategy for the early detection of psychosis
-
b the early establishment of a definite diagnosis
-
c early admission and assessment in hospital
-
d the maintenance of valued social roles
-
e a strategy for relapse prevention.
-
-
4. Psychological adjustment following a first-episode psychotic illness:
-
a is usually uncomplicated if psychotic symptoms resolve completely
-
b is helped by developing a sense of mastery
-
c can be problematic if the individual feels trapped by the illness
-
d is nearly always successful if the individual accepts the illness
-
e is helped by learning how to self-manage relapse.
-
-
5. Therapeutic engagement of young people with a psychotic illness:
-
a improves if staff insist that the young person accepts the diagnosis as soon as possible
-
b is helped if staff search for common ground to understand clients' experiences
-
c can be helped by an assertive outreach approach
-
d requires regular out-patient appointments
-
e is helped by persistent contact with a keyworker.
-
MCQ answers
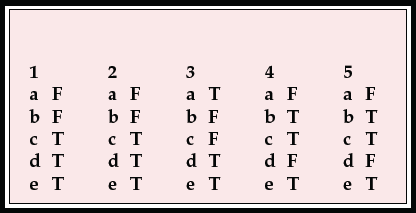
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | T | a | F | a | F |
| b | F | b | F | b | F | b | T | b | T |
| c | T | c | T | c | F | c | T | c | T |
| d | T | d | T | d | T | d | F | d | F |
| e | T | e | T | e | T | e | T | e | T |





eLetters
No eLetters have been published for this article.