Dependence on alcohol or other drugs is a depressing experience. The way of life of the individual who is dependent on alcohol is replete with incidents that are demoralising, waking daily with a hangover or with tremor and retching, coupled with amnesia for events of the night before, a sense of inability to face the day ahead and awareness of recriminations at work and at home. Little wonder that depressed mood is common in such circumstances. Similarly, the drug addict, when life is dominated by the daily problem of obtaining supplies of a substance that brings transient relief or pleasure but also experiences of an impoverished existence and low mood. Add to this the fact that the biological action of many commonly misused substances can induce depression then it is hardly surprising that depression is common in this population. There are also a smaller number who use alcohol or illicit drugs to cope with primary depression. Teasing out the interplay of affect and substance misuse is a challenge for the general psychiatrist and the addiction specialist.
As many as 80% of alcoholics complain of depressive symptoms, including 30% who fulfil criteria for a major depressive disorder (Reference Raimo and SchuckitRaimo & Schuckit, 1998). A lifetime history of depressive disorder has been found in 48% of opiate addicts (Reference Rounsaville, Weissman and Crits-CristophRounsaville et al2001). Thus, it is clear that substance misuse and depressive symptoms often occur together, but what is less clear is their true relationship. Box 1 shows three frequently asked questions concerning it.
Box 1. The relationship between substance misuse and depression
Three frequently asked questions
Are the depressive symptoms and disorders caused by the substance misuse?
Do depressive illnesses cause people to self-medicate with alcohol and drugs?
Are there common predisposing factors linking the two presentations that account for their frequent co-occurrence?
The combination of depressive symptoms and substance misuse presents important management issues, both at the level of the individual patient and regarding service provision. In individual patients it is often difficult to disentangle all threads of the presentation. An unusual mental state may be due to intoxication, and substance misuse may be hidden. A frequent management dilemma is the intoxicated patient in the middle of the night, who has self -harmed, or is threatening to do so.
Although depressive symptoms and substance misuse commonly occur together, services for their joint management do so less frequently; a recent editorial talks of the “medical model of psychiatric services […] contrasting sharply with the psychosocial orientation of substance misuse services” (Reference Weaver, Renton and StimsonWeaver et al1999). In the UK patients with depression are cared for by generic psychiatric services and substance misusing patients by drug and alcohol services, with few examples of dual diagnosis services evident. We should, however, remember that no similar distinction exists in primary health care and that the general practitioner has a key role in which route is taken by the patient. It is also known that the majority in both categories do not come to specialist services. None the less, having more than one psychiatric diagnosis leads to an increased likelihood of presentation to treatment services (Reference Wu, Kouzis and LeafWu et al1999), but there are rarely skilled appropriate services available, able to offer a multifaceted approach to care.
Epidemiology
The scale of the co-occurrence of the diagnoses of depression and drug and alcohol misuse has been examined by a number of large population-based studies.
The largest of these is the Epidemiologic Catchment Area (ECA) study (Reference Regier, Farmer and RaeRegier et al1990). This showed that of people with an alcohol disorder, 13% met criteria for an affective disorder. More strikingly, 32% of those with affective disorder met criteria for a substance misuse disorder. Other studies support these figures and suggest higher correlations (Reference Farrell, Howes and TaylorFarrell et al1998; ,Reference Kessler, McGonach and ZhoaKessler et al2001).
As would be expected, studies looking at groups of people in contact with treatment services give an even higher estimate of the co-occurrence of depression and substance misuse (Reference Rounsaville, Weissman and KleberRounsaville et al1982).
There is also a body of work looking at suicide in this group; in fact, the most common mental disorders preceding suicide have consistently been found to be depressive illness and alcohol misuse. Comorbidity is more common in alcoholics who commit suicide than in alcoholics who do not commit suicide, and has been found to predict suicide risk (Reference Driessen, Veltrup and WeberDriessen et al1998). Interestingly, severity of alcoholism seems not to be of importance (Reference Berglund and OjehagenBerglund & Ojehagen, 1998). The extent to which substance misuse increases the likelihood of a fatal outcome also needs to be taken into account: drug overdoses are frequently taken in association with large quantities of alcohol.
The likelihood of suicide in conservatively diagnosed alcoholics has variously been estimated at between 60 to 120 times that for those without psychiatric illness. A number of life stressors have also been implicated, including interpersonal loss and conflict, which have been found more often in the 6 weeks preceding death in those suicides associated with substance misuse. Other associations include an increased likelihood of parental alcoholism and a younger age at which problem drinking started (Reference Berglund and OjehagenBerglund & Ojehagen, 1998).
A strong predictor of completed suicide is previous self-harm. A consistent finding has been that suicide attempters who misuse alcohol have higher rates of substance misuse and depression, multiple psychiatric disorders and more encounters with law-enforcement agencies (Reference Berglund and OjehagenBerglund & Ojehagen, 1998). In drug misusers there is also a high excess mortality from suicide. Prevalence rates of attempted suicide have been reported ranging from 15 to 45% (Reference Rossow and LauritzenRossow & Lauritzen, 2001).
Substance misuse and depressive symptoms
Are depressive symptoms and disorders caused by substance misuse?
Alcohol intoxication can be accompanied by temporary but severe depressive symptoms. Long-term alcohol use is also associated with depressed mood, and almost all alcoholics report periods of intense sadness. A categorisation of the presentations of alcohol-associated mood disorders is given in Box 2. This suggests that substance-induced disorders are commonly phenomenologically indistinguishable from independent major depressive disorders. However, they will remit 2–4 weeks after alcohol drinking has ceased, without the need for antidepressants. At presentation to an alcohol treatment programme, 42% of alcoholic men had significant depressive symptoms, but only 6% were clinically depressed after 4 weeks of abstinence (Reference Brown and SchuckitBrown & Schuckit, 1998).
Box 2. Presentations of alcohol-associated mood disorders (Reference Raimo and SchuckitRaimo & Schuckit, 1998)
Patients with alcohol-related mood disorders may be categorised as
Those with a primary substance-induced disorder and secondary depressive symptoms
Those with underlying physical disorders, such as liver disease or medication effects (e.g. treatment with anti-hypertensives), who are remediable by treatment of the underlying disorder
Those with an independent major depressive disorder
In support of the validity of this distinct sub-category, Brown & Schuckit give the following evidence: both alcoholism and depression are highly familial disorders, but children of alcoholics, although showing increased problems with substance misuse, do not show an increased incidence of independent mood disorders, as would be expected if all depressive symptoms were attributable to independent mood disorder. Work looking at longitudinal follow-ups of adults who had had teenage depression demonstrated no increased incidence of alcohol dependence compared with controls. A longer-term follow up of alcoholic men also showed that with sobriety, the incidence of depression was similar to other men (Reference Raimo and SchuckitRaimo & Schuckit, 1998). It is from such work looking at the differences in presentations over time that the concept of substance-induced depressive disorder came to be formulated.
Although the majority of work done has related alcohol and mood, other substances also have important mood effects. Amphetamine and cocaine may have dramatic intoxication presentations, including mood disturbance, which have been well documented. Post-intoxication effects, particularly depression, should also be borne in mind with these drugs, as they can be more devastating than acute effects. Depressed mood following the use of ecstasy (3.4–methylenedioxymethamfetamine) is frequently described and sometimes severe.
Long-term studies have looked at depressive symptoms in opiate addicts. Overall, depressive symptoms were found to be common, particularly at presentation to services, but were generally in the mild to moderate category. The reasons prompting the contact, such as child custody or criminal justice involvement, may also lead to lowering of mood. During contact with drug treatment services substantial improvement occurred, with little difference between drug-free and methadone-maintained groups. Only 1% of this patient group required antidepressant treatment, showing that stabilisation of drug use and detoxification can have beneficial effects on the mood state, without formal treatment for depression (Reference Rounsaville, Weissman and Crits-CristophRounsaville et al2001).
Do depressive illnesses cause people to self-medicate with alcohol and drugs?
It is very difficult to design studies to answer this question. A search for plausible explanations is a universal human characteristic, and patients seeking treatment will inevitably be involved in a search for cause and explanation, thus biasing their recall. A key concept in this field is the ‘self-medication hypothesis’, the proposal that people with psychiatric symptoms are motivated to take alcohol or drugs to relieve their symptoms. Patients will often report that they drink or take drugs to alleviate stress or to help depressed feelings.
One review (Reference ChickChick, 1999) quotes a prospective population study (Reference Moscato, Russell and ZieleznyMoscato et al1998). This showed that in females, depressive symptoms predicted alcohol misuse at 3 and 4 years, but not at 7 years. There was no effect for men. This suggests that, for women, depression may predate alcohol misuse. Prospective studies have also found that a diagnosis of major depression at entry to in-patient treatment predicted a shorter time to first drink (Reference Greenfield, Weiss and MuenzGreenfield et al1998).
Stimulants such as cocaine or amphetamines produce a transitory lifting of mood but with rebound depression. Alcohol relieves anxiety and gives some blunting of concern about depressing circumstances, but these effects are short lived. There are, however, no indications for the positive effects of alcohol in psychiatric disorder, and any effect may be explained more by positive expectations from alcohol than by any true effect (Reference Berglund and OjehagenBerglund & Ojehagen, 1998). Indeed, the detrimental effect of alcohol and drug misuse on symptomatology is much more common.
Are there common predisposing factors linking the two presentations that account for their frequent co-occurrence?
An alternative way of viewing these disorders is that there are factors, either genetic or environmental, that independently cause both conditions. Several genes involved in serotonin metabolism have been implicated in both depression and alcohol dependence. Research using twin studies has also been initially supportive of this hypothesis, although further studies are needed (Reference ChickChick, 1999).
Recognition of comorbidity
As already stated, substance misuse has a key role in the genesis of symptoms and has also been shown to worsen prognosis in mood disorders (Reference Berglund and OjehagenBerglund & Ojehagen, 1998). It is therefore important to seek out its occurrence, especially in frequent users of psychiatric services, who have been found to be particularly at risk (Reference Scott, Gilvarry and FarrellScott et al1998).
Assessment
The assessment process should ensure that mental health service staff can reliably detect alcohol and drug misuse and that addiction services can detect depressed mood. Ideally, both services should use similar guidelines for identifying and recording this information.
Nearly half of 15- and 16-year-olds in the UK report illicit drug use (Reference Miller and PlantMiller & Plant, 1996). Because these drugs may be relevant to the patient's mood, a history of drug use is an essential part of the initial examination. This should be backed up by urine testing for drugs in cases where suspicion is aroused. Many commonly misused substances are eliminated from the body within 24–48 hours; therefore, if testing for toxicology is required, samples should be taken early after admission or at the time of first contact.
The close links between alcohol misuse and mood disturbance make it essential that a drinking history is taken in every case. It is still not uncommon to find psychiatric case records where there is no description of the patient's drinking pattern or it is given in a very cursory way, for example “drinks socially” or “moderate drinker”. What is required is a brief but clear picture of the patient's drinking habits. This can be achieved in a variety of ways; one of the simplest is to ask on how many days a week the patient normally has a drink of alcohol, and how much is typically drunk on those days. Calculate the answer in units and you have a rough estimate of that patient's weekly consumption. This information is augmented by asking whether alcohol has caused any problems.
There are a variety of screening tests for alcohol use, including the CAGE questionnaire (Reference Mayfield, McCleod and HallMayfield et al1974), which reliably identifies drinkers with problems but often misses ‘at-risk drinkers’. The latter are detected by the broader Alcohol Use Disorders Identification Test (AUDIT) questionnaire (Reference Babor, Hofman and DelbocaBabor et al1989). Both of these are slightly more time consuming than very brief tests such as the Paddington Alcohol Test (Reference Smith, Touquet and WrightSmith et al1996), developed for accident and emergency settings. These tests can be augmented by blood markers such as gamma-glutamyl transferase (GGT), mean corpuscular volume (MCV) and carbohydrate-deficient transferrin (CDT). These biological measures can also be used as a guide to progress. Feedback concerning abnormal blood results can be powerful objective evidence demonstrating to the patient that alcohol is causing damage, an appreciation that is reinforced by signs that these figures gradually improve once drinking ceases.
The assessment interview should provide a clear picture of the level of current substance misuse, the amount taken on a daily basis, the pattern of use and the route of administration. Evidence of self-harm, violence to others, disturbed thoughts or moods, and their relationship to substance use should be noted. Assessment of mood should enquire into biological symptoms of depression, the duration of the depression and its particular relation to substance misuse.
The screening instruments for alcohol and drug use and those concerned with affective disorder have not been tested in patients with dual diagnosis. The influence of one condition on the other may give rise to misleading results; for example, many of the features of biological depression are mimicked by the consequences of repetitive excessive drinking, such as feeling ill and depressed in the morning, being unable to face the day, weight loss, impaired concentration and memory and insomnia.
Depression is probably overdiagnosed in individuals with alcohol problems, as it often proves to be secondary to the drinking problem itself. A wrong diagnosis of depression may give rise to unnecessary prescribing of drugs or even electroconvulsive therapy. However, on some occasions, an underlying depressive disorder is missed. The lifetime risk of suicide is very much higher in problem drinkers than in the general population, and this risk is increased by the presence of a depressive illness.
Even at the stage of assessment it can be useful to include components of motivational interviewing (Reference Miller and RollnickMiller & Rollnick, 1991) and to forge links in the patients mind between increased substance misuse and worsening of symptoms. At assessment it is also important to create an open, non-judgemental attitude to try encourage frankness about substance misuse.
If the patient is intoxicated it may be very difficult to obtain any form of coherent history. In these circumstances the importance of a collateral history cannot be overstated. In an ideal world a safe environment would be available, in which the patient could remain until the effects of intoxication have resolved, leaving a clearer assessment of mental state. Unfortunately, this is not always possible owing to lack of resources. Even an assessment on the following day is not always straightforward, as withdrawal symptoms are not without their own powerful influences.
Management
Safety is of prime importance in the management of this group. In addition to the increased risks of self-harm, the disinhibiting effects of many substances, particularly alcohol, should be carefully considered. Within psychiatry, there prevails a culture of ignoring the threats of intoxicated patients, even though they are sometimes carried out. A risk assessment should be made of each individual patient's circumstances.
Pharmacological management
At initial presentation it will be very difficult to differentiate independent mood disorders from those due to continued substance misuse. A key message in all the literature in this area is the importance of treating the substance misuse, and the highly probable beneficial effects that this will have on the mood state.
Alcohol detoxification has been discussed in a previous paper in APT (Reference RaistrickRaistrick, 2000), which recommends a period free from psychoactive drugs prior to starting treatment for depression. A wait of 2–4 weeks post alcohol cessation is advised before commencing antidepressant treatment, to ensure that the mood effects of the alcohol have cleared the system (Reference Raimo and SchuckitRaimo & Schuckit, 1998).
With opiate misuse, a primary aim of treatment may be stabilisation and substitute prescribing, not detoxification. This in itself has been shown to have a beneficial effect on mood (Reference Rounsaville, Weissman and Crits-CristophRounsaville et al2001).
In the past, antidepressants were considered as treatments for alcohol misuse in people without depressive symptoms. Current opinion does not support this. However, in an in-patient sample, detoxified patients with depression randomly allocated to fluoxetine or placebo showed that the active drug helped to reduce depressive symptoms (Reference Cornelius, Salloum and EhlerCornelius et al1997). Other studies do not support this result, and work continues to clarify the benefits of antidepressants within alcoholic subtypes (Reference Pettinati, Volpicelli and KranzlerPettinati et al2000).
In one study, Mason et al (1996) found that desipramine reduced depressive symptoms and was associated with significantly longer abstinence from alcohol. However, they concluded that there was no support for desipramine in alcoholics without depression. In a review of this topic, Lynskey (1998) concludes that antidepressant treatment is not a standalone treatment for alcoholics with depression, but that pharmacological treatment of depression may help to optimise the outcome of treatment for alcohol dependence in this group. The same paper also raises the important question of drug safety in this group.
Darke & Ross (2001) studied the safety of the use of antidepressants among injecting drug users in Australia. They reported a strong association between antidepressants and non-fatal heroin overdose. The use of tricyclics was particularly hazardous. They recommended the use of selective serontonin reuptake inhibitors (SSRIs), but only where clearly indicated. They commented on the street value of antidepressants, noting that opiate misusers took them for a variety of reasons: to self-medicate depressive symptoms, to become intoxicated, to aid sleep and to manage heroin withdrawal. A further consideration is that methadone slows tricyclic metabolism, so tricyclic dosing must be carefully titrated.
There are few studies examining the positive effects of antidepressant use among drug misusers. Randomised controlled trials have been difficult to complete owing to high dropout rates. There are mixed reports of efficacy, with some positive results reported (Reference Scott, Gilvarry and FarrellScott et al1998). A study looking at fluoxetine concluded that it was not effective in treating depressive symptoms in methadone-maintained opiate addicts, but commented that there were significant overall reductions in depression while patients were in contact with drug treatment services (Reference Petrakis, Carroll and NichPetrakis et al2001).
A variety of pharmacotherapies are available in the treatment of alcohol problems. Disulfiram is a useful aid to abstinence of proven effectiveness when combined with supervision. In a small number of cases, psychotic episodes have been described as a side-effect of disulfiram, but in most respects it is safe to use. Unfortunately, it can have serious consequences if misused, and particular care should be taken in prescribing it to patients with depression who may be suicidal. Acamprosate and naltrexone have both produced improved outcomes in individuals who are alcohol dependent. We do not know about their efficacy in patients with dual diagnosis, but it seems reasonable to use one or the other when patients are particularly conscious of craving during the early months of abstinence. Either can be combined with antidepressants, if necessary.
Psychological therapies
Psychological therapies must be considered both in their own right and in combination with medication. There is a growing literature in this area, although most work has centred on motivational interviewing (Reference Miller and RollnickMiller & Rollnick, 1991), which can be a useful technique throughout assessment and treatment.
Trials of cognitive therapy have shown promising results that mirror antidepressant findings: an improvement in depressive symptoms can lead to an improvement in substance misuse (Reference LynskeyLynskey, 1998). There has also been promising work incorporating facets of cognitive therapy and early work on interpersonal therapy (IPT; Scott et al1998).
Miller et al (1998) reviewed the literature on the treatment of alcohol misuse, deriving a methodological quality score; they listed a number of positive and negative results for each and gave a clinical effectiveness score for those methods that had been adequately investigated. Motivational enhancement showed consistent benefits, as did community reinforcement, acamprosate, naltrexone and social skills training. Again, it is not clear how well these approaches combine with other treatments for depression. None the less, it seems reasonable to think that that these psychological therapies for alcohol problems should be added to traditional therapies for depression.
Treatment for substance misuse commonly relies heavily on the motivation or commitment of the patient. Bien et al (1993) outlined the key features of brief intervention as feedback about current misuse, the patient's own responsibility for change and advice about making and maintaining this change. Therapy for substance misuse, and particularly alcohol dependence, places much greater responsibility for change on the patient and there is less reliance on a medical model. Patients with severe depression may find it hard to engage in this kind of therapy until their mood has lifted.
Although group therapy now has a less salient place in the treatment of alcohol problems than formerly, it is still widely used. Patients with depression may find group processes very threatening and require careful introduction, after severe depression has lifted. Alcoholics Anonymous (AA) and Narcotics Anonymous are very effective self-help agencies but, again, individuals who are depressed may find it difficult to join them because they anticipate that the experience will be threatening. The first steps can often be made easier by introduction to an empathic member before attending the first meeting.
The risks of the interaction of antidepressant medication with alcohol and illicit drugs, and the associated special hazards of medication overdose and misuse, make psychological therapies an attractive proposition either as an alternative or additional treatment.
Prognosis
Comorbidity carries with it a worse prognosis, both for substance misuse and depressive symptoms (Reference Hall and FarrellHall & Farrell, 1997). A diagnosis of current major depression at entry into in-patient treatment for alcohol dependence predicted a shorter time to first drink and relapse in both men and women (Reference Greenfield, Weiss and MuenzGreenfield et al1998). Similarly, among patients addicted to opiates, a current major or minor depressive episode at entry to treatment was correlated with higher levels of illicit drug use during the subsequent 6-month period (Reference Rounsaville, Weissman and Crits-CristophRounsaville et al2001). The large increase in risk for attempted and completed self-harm implicit in a diagnosis of comorbidity has been described above.
Service provision
Often, patients with two diagnoses fall between services designed to treat either the depression or the substance misuse. The creation of ‘super-specialist’ services has been advocated, particularly in the USA, but UK services have suggested other strategies to try to improve practice. In a number of centres, combined psychosis and substance misuse teams have been created to treat patients with dual diagnosis and act as a consultancy and training resource for other agencies. These initiatives will be watched with interest.
There have been calls for improved staff training, both in mental health and addiction services, to try to improve recognition of comorbidity. Increased sharing of skills and support between the two services has also been recommended (Reference Hall and FarrellHall & Farrell, 1997). It is often helpful for staff in one agency to gain experience in the other, as this helps mutual understanding and knowledge of the issues involved. It has also been stated that services for drug misuse and mental health have tended to develop in ways determined more by public anxiety and political ideology than by research evidence. Training an appropriate workforce, research into the efficacy of services and the development and testing of new models of service provision are required (Reference Weaver, Renton and StimsonWeaver et al1999). Box 3 lists the attributes that should be present if both services are to achieve optimum efficacy.
Box 3. Requirements of services to ensure optimal treatment of depression in substance misuse
Psychiatric services
Individuals who misuse substances must have the same right to treatment as other patients
A substance-use history must be recorded in all cases
Clear protocols should be in place to ensure treatment and follow-up when misuse is identified
Regular liaison with addiction services and knowledge of services available are essential
Care plans should identify a strategy for dealing with substance misuse
The implications of drug interactions between prescribed medication and alcohol or illicit drugs must be considered
Addiction services
The attitude that mental illness excludes patients from effective therapy must not be allowed
Mood and suicidality must be assessed and monitored
If mood disorder persists after 2 weeks of abstinence or stabilisation, a diagnosis of depressive illness should be considered
Regular liaison with general psychiatric services is essential
Follow-up plans should include regular mental state assessments
Summary
Patients presenting with depression complicated by substance misuse pose particular challenges in their management. Their depressive symptoms are very likely to be caused or exacerbated by their substance misuse. In alcohol misuse, a 1-month period of abstinence and then further evaluation are recommended before the commencement of pharmacotherapy. Opiate users should be stabilised before pharmacotherapy. Prescription of antidepressants must be very carefully considered, as they have a street value and might therefore be widely disseminated; also, there is little evidence supporting their efficacy in treating depressive symptoms in this group. SSRIs would be the treatment of choice. Strong consideration should be given to psychological therapies such as motivational interviewing and cognitive–behavioural therapy, which are currently being further evaluated and hopefully should become more available to patients with comorbidity. Equally, treatment of depressive symptoms also yields benefit in managing substance misuse, with antidepressant treatment decreasing alcohol intake in alcoholics with depression.
Multiple choice questions
-
1. Regarding the epidemiology of substance misuse and depressive disorders:
-
a. in the ECA study, 32% of those with affective disorder met criteria for an alcohol disorder
-
b. the likelihood of suicide in alcoholics has been estimated at 120 times that of those without psychiatric illness
-
c. in the ECA study, 31% of those with an alcohol disorder met criteria for an affective disorderd.a long-term follow-up of alcoholic men showed that, with sobriety, their incidence of depression was equal to that of other men
-
d. teenagers with depression show an increased incidence of alcohol misuse in later life.
-
-
2. Regarding self-harm in substance-misusing populations:
-
a. comorbidity predicts suicide risk
-
b. interpersonal loss is unimportant
-
c. parental alcoholism has been found to be associated
-
d. alcoholics who have no diagnosis of depression do not self-harm
-
e. in drug misusers deaths attributed to accidental overdose may be suicides.
-
-
3. Antidepressants:
-
a. are unhelpful in the treatment of alcohol misuse
-
b. are contraindicated in methadone-maintained populations
-
c. have been implicated in opiate overdose
-
d. may decrease substance misuse
-
e. have a street value.
-
-
4. Regarding the treatment of depression in substance misusers:
-
a. assessment of an intoxicated patient is without value
-
b. IPT and CBT may prove beneficial to both depressive and substance-misuse symptoms
-
c. contact with treatment services may prove more beneficial to mood than antidepressants
-
d. depressive symptoms may be predictive of earlier relapse
-
e. abstinence will improve mood in the majority of cases.
-
-
5. True or false:
-
a. motivational interviewing is solely for use in substance misuse
-
b. comorbidity increases the chance of presentation to treatment services
-
c. comorbidity services are always evidence based
-
d. methadone has antidepressant properties
-
e. children of alcoholics have high rates of depressive disorders.
-
MCQ answers
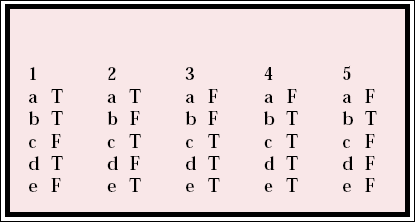
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | T | a | F | a | F | a | F |
| b | T | b | F | b | F | b | T | b | T |
| c | F | c | T | c | T | c | T | c | F |
| d | T | d | F | d | T | d | T | d | F |
| e | F | e | T | e | T | e | T | e | F |





eLetters
No eLetters have been published for this article.