The term ‘therapeutic community’ is usually used in the UK to describe small cohesive communities where patients (often referred to as residents) have a significant involvement in decision-making and the practicalities of running the unit. Based on ideas of collective responsibility, citizenship and empowerment, therapeutic communities are deliberately structured in a way that encourages personal responsibility and avoids unhelpful dependency on professionals. Patients are seen as bringing strengths and creative energy into the therapeutic setting, and the peer group is seen as all-important in establishing a strong therapeutic alliance. The flattened hierarchy and delegated decision-making are sometimes misunderstood as anarchy by outsiders. However, staff in modern therapeutic communities are deeply aware of the need for strong leadership and their responsibility to provide a safe ‘frame’ for therapeutic work (Association of Therapeutic Communities, 1999).
In the USA, the term ‘therapeutic community’ is more often used to describe user-run communities for substance misusers with: a hierarchical structure; a reward system; fierce encounter groups; and a simple explanatory model of addiction and its treatment. These are referred to as ‘concept’ or ‘behavioural’ therapeutic communities, as opposed to ‘democratic’ therapeutic communities, which are the main focus of this paper. Phoenix House and Daytop are two major concept therapeutic community programmes that grew from this movement in the USA and spread to many different countries (Reference KennardKennard, 1998). In the UK, this model is currently being developed within the prison service. In common with democratic therapeutic communities, the primary mechanism by which these units aim to alter behaviour is by encouraging residents to take responsibility for themselves and for others.
Democratic therapeutic community principles are applicable to a wide variety of client groups and settings, for example HMP Grendon Underwood (Reference Cullen, Jones and WoodwardCullen et al1997), which helps offenders within the prison system, and Peper Harow (Reference RoseRose, 1990), for children with severe behavioural problems. This paper, however, focuses on the importance of the therapeutic community movement within the National Health Service (NHS).
The living–learning experience, culture of enquiry and importance of community meetings
Some therapeutic communities work exclusively in a group forum, others incorporate individual psychotherapy. The day-to-day experience of living and working together is felt to be as important as formal therapy, and the structure is such that the two are closely integrated and inform each other – the living–learning experience. Understanding the institutional dynamics of the social setting is fundamental. This understanding is informed by systems theory and organisational management theory as well as psychoanalytical and group-analytical ideas. An important underlying principle is that all involved are encouraged to be curious about themselves, each other, the staff, the management structure, psychological processes, the group process, the institution and everything else pertinent to events and relationships within the community. This is known as the ‘culture of enquiry’ – an openness to questioning, so that understanding is owned by all and not seen solely to reside in professionals.
A typical day in a therapeutic community starts and finishes with a community meeting, usually chaired by a resident. The agenda is driven by the attempt to bring as much information into the large group as possible, so that it is accessible to all. Exclusive discussions in which a resident divulges significant material to another resident or staff member are usually discouraged in order to avoid ‘splitting’. This is a phenomenon often seen in patients with personality disorders: typically, one staff member is privy to the vulnerable side of the patient – made to feel special and drawn into a rescuing role – while the rest of the team feel irritated by the patient's destructive behaviour and are more in touch with the manipulative aspect of his or her personality. These splits often develop in teams, with both sides blaming the other for the patient's worsening state. An understanding that team members are holding different aspects of the patient's personality can potentially redeem the situation and inform psychological understanding. Therapeutic communities are therefore structured to discourage ‘secrets’ and ‘special relationships’ between individuals and subgroups. The community meetings play an important role in establishing a culture of open communication, in which individuals can check things out, paranoia is minimised and expression of feeling is encouraged. At Francis Dixon Lodge, for example, accounts of psychotherapy groups, activity groups, work groups, staff meetings, assessments, as well as the ongoing lives of community members, including incidents of self-harm or other forms of rule-breaking, are all brought into the community meeting for discussion. In addition, crisis meetings can be held at any time of the day or night – usually if someone feels like self-harming. The pressure to talk and therefore to think about feelings rather than act on them eventually leads to a less brittle superego and more effective impulse control.
Historical perspective
Therapeutic community ideas have their roots in various religious and political movements and most obviously develop some of the ideas espoused by Tuke and the ‘moral treatment’ movement in the early 19th century – for example the importance of work, a healthy environment and warm relations. Therapeutic communities, as we know them today, developed from two visionary experiments between 1942 and 1948, known as the Northfield experiments (Reference HarrisonHarrison, 2000). The first experiment was led by Bion and was unsuccessful, in the sense that it had to close after 6 weeks. The ideas were, however, taken up and developed by others such as Rickman, Bridger, Main and Foulkes. Army psychiatric services were faced with hundreds of psychologically traumatised soldiers and the expectation that they were to help as many as possible recover to a state where they could return to the front line. The psychiatrists at Northfield Hospital in Birmingham decided to focus on the unit as a whole rather than on individual problems; they structured the wards as communities, encouraging mutual support and cooperation in living (in some ways similar to life in the army), with non-directive group discussions to examine and understand the process. They saw the whole community as both the patient and the instrument of treatment, and the aim was the education and training of the community in the problems of neurotic defences and interpersonal relationships. This idea was later known as the living–learning experience. After the war, Main went on to become the Director of the Cassel Hospital in Surrey, which he reorganised on psychoanalytical lines to be a therapeutic community.
At the same time, Maxwell Jones was developing a unit along similar lines at Mill Hill in London, helping soldiers suffering from what was known as ‘effort syndrome’. Lectures about the physiological basis of their symptoms gradually led to more open discussions, the more experienced patients giving information to newer patients and a less rigid demarcation between doctors, nurses and patients. Maxwell Jones went on to become the director of a new unit set up to tackle the problems of ‘unemployed drifters’ at Belmont Hospital in Surrey. Belmont was renamed Henderson Hospital in 1958.
During the 1960s and 1970s, a number of democratic therapeutic communities were set up in different parts of the country, sharing some basic ideological principles but evolving in individual ways, according to local needs and resources. The 1980s and 1990s saw many of these units close. This was partly due to pressure from NHS reforms and the introduction of the purchaser–provider split and partly, perhaps, because they were antithetical to the prevailing philosophy within society –particularly the promotion of individualism at the expense of collectivism. It seems that the tide is changing again and the past few months have seen the opening of new therapeutic communities within the NHS: two of them residential, based on Henderson Hospital model and nationally commissioned; two others, day units, the result of a health authority response to local need. There are other units in the planning stage. A parallel expansion can also be found within the prison service and voluntary sector.
Defining a therapeutic community
Although therapeutic community practice overlaps with other services, the structured attempt to raise the status of patients and the all-embracing culture of enquiry mean that therapeutic communities, although differing in detail between themselves, have a cohesive philosophy and aspire to be more than a setting where severely disturbed patients can be contained while they undergo therapy.
By definition, therapeutic communities are continually evolving. This makes them difficult to categorise, define and study. One of the lessons learnt over the past 50 years is that, however benign the set-up, institutionalisation will occur unless the culture of enquiry is such that the status quo is continually questioned. Main (1967) eloquently described how ideas originating in the ego of one generation move to the superego of the next, losing their creative potential and becoming ritualised.
Rapoport and a team of sociologists were invited to study Henderson Hospital, and the book Community as Doctor (Reference RapoportRapoport, 1960) describes their findings. Four principles emerged, which are often quoted as defining the work of a therapeutic community: democracy, reality confrontation, permissiveness and communality. These should not be seen as absolutes but rather as principles in tension with each other. For example, the reality of professional accountability cannot be ignored: although it is vital that all community members have a significant voice in decisions that affect their lives, it is important to be realistic and clear about the limits of democratic decision-making and the responsibility of professionals to provide a safe frame for therapeutic work. Likewise, permissiveness would usually be limited to the verbal expression of feelings and would be strongly confronted if it led to other members of the community being emotionally hurt or damaged or feeling excluded. Racist comments, for example, would not be allowed to go unchallenged in modern therapeutic communities.
Another important observation from this study, replicated in other therapeutic communities, was the repeated cycle of oscillations: times of healthy functioning, when residents were well able to manage responsibility and a level of therapeutic permissiveness; other times when high levels of disturbed behaviour meant that staff had to take a more active role. The observation may be pertinent to other settings in psychiatry – the frequent observation that suicides occur in clusters, for example. My own experience of a series of suicides connected to a therapeutic community (Reference Campling, Campling and HaighCampling, 1999) is a sharp reminder that group dynamics can be powerfully destructive as well as therapeutic. An understanding of these oscillations in therapeutic communities is of importance when designing research programmes and interpreting the results.
The Rapoport study also highlighted the conflict between those whose main objective was preparing residents for the outside world and those whose main objective was helping residents to understand themselves better. This conflict between rehabilitation and psychotherapy continues in many of today's communities. A balance is important, as they potentiate each other – more psychotherapeutic work is possible if the resident is well grounded in a healthy structure of practical everyday living. Indeed, the structured programme and the need to roll sleeves up and get on with the washing-up when you are feeling suicidal, or dig the vegetable patch with someone whom you had been raging at earlier in the day, is one of the things that make a therapeutic community containing. It is interesting that the new therapies designed for a similar client group (e.g. cognitive–analytic therapy and dialectical–behavioural therapy) also have a component that is practically focused and skills-based.
Another tension is the need to focus on both the community as a whole and the parallel development and progress of individual residents. For example, a hand-over at Francis Dixon Lodge would usually start with a description of the general atmosphere and common themes, before going on to discuss individual residents. There is always the danger of one being subsumed within the other, with the consequent loss of information affecting the creative potential to understand and make meaningful connections. For this reason, most therapeutic communities would not have a keyworker system, where there is a danger that thinking both resides in and is focused on an individual, with the complexities of the group and institutional dynamics avoided. Truly working as a team means that there is always a richness of perspective to draw on, and differences are understood as reflecting the splits in the patients’ personalities, grist to the mill of psychotherapeutic work, rather than being personalised or even pathologised, as happens if this understanding is not harnessed. Putting the ‘ward atmosphere’ consciously on the agenda for discussion is something that all in-patient units would find helpful.
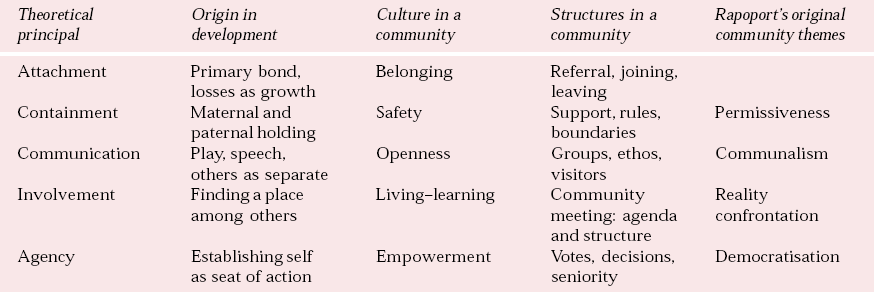
Forty years on from Rapoport, Haigh has attempted to define the quintessence of a therapeutic environment (Reference Haigh, Campling and HaighHaigh, 1999). He describes five essential qualities and presents them in a progressive sequence, linking the developmental stage, the qualities in the culture and the structures that establish and maintain them. Table 1 relates these to Rapaport's earlier themes. While ‘attachment’, ‘containment’ and ‘communication’ are qualities to be found within all psychotherapeutic settings, ‘involvement’ and ‘agency’ are specific to therapeutic communities and refer to the sense of mutual dependence, responsibility for each other and the growing awareness of the self as the seat of authority and power. The five can be seen as a simplified sequence of the normal development of the sense of self in relation to others. For many patients, the process of ‘primary emotional development’ has gone seriously wrong, with abuse, trauma, neglect, deprivation and loss disturbing the network of relationships. Therapeutic communities, by recreating these conditions, can facilitate ‘secondary emotional development’, where things that went wrong can be re-experienced and worked at, hopefully leaving members stronger and more insightful.
Clinical and political developments in therapeutic communities
Therapeutic communities within the NHS have increasingly defined their client group as those with severe emotionally unstable personality disorder. As a group, these patients seem to be presenting more often to psychiatrists and psychotherapists, and there is some evidence that there may be a real increase in numbers. We now recognise that many of these patients were severely sexually or physically abused as children. In therapeutic communities this has necessitated a heightened awareness of the need for strict professional boundaries: the affectionate rituals that were an accepted part of the scene in the 1960s and 1970s no longer feel appropriate.
An important influence has been that of attachment theory. Therapeutic community patients are helpfully understood as suffering from ‘attachment failure’ in an attempt to make their pattern of multi-service usage understandable. Early experience of chaotic, abusive attachments means that they lack ‘basic trust’ and find it difficult to express their distress or ask for help in a constructive manner. The task is to provide a safe frame within which they can explore intrapsychic and interpersonal problems and find more constructive ways of dealing with distress. Many of them lack the capacity to manage or think about their feelings and ‘act out’, usually in a self-destructive manner, in an attempt to rid themselves of such feelings. The structure of a therapeutic community, with its community meetings, diverse network of relationships, supportive peer group, strong sense of belonging, 24- hour support, structured day and clear rules and boundaries owned by the residents, means that a strong therapeutic attachment can be forged – an attachment that can withstand high levels of aggression and risk. The understanding that this client group needs a secure attachment if therapeutic work is to be beneficial and, conversely, that such patients find endings particularly problematic, indeed often catastrophic, has led a number of therapeutic communities to develop follow-up programmes.
Therapeutic community day units seem to be able to contain high levels of disturbance while maintaining a degree of independence. Research is needed to ascertain which patients do better in day units as opposed to residential units and vice versa. Winterbourne Therapeutic Community and, more recently, Francis Dixon Lodge have developed patient telephone and e-mail networks – a system of mutual support that seems to act in a holding capacity and is, incidentally, cost efficient (Reference HigginsHiggins, 1997). The idea of a telephone network is not simply that one vulnerable individual contact another, in a state of crisis; it is a tangible manifestation of a complex containing matrix of relationships, which can bring a sense of belonging and meaning to life.
There is also an understanding that patients do better in all types of psychotherapy if they are well prepared and know what to expect. Written information, and sometimes audio- or videotapes, are sent to potential residents. Assessments tend to be more comprehensive than they used to be. The experience of being in a therapeutic community can be difficult and painful, occasionally damaging. It is therefore important that assessments are thorough and patients are given as much information as possible about what to expect, if ‘consent’ is to be meaningful. For these reasons, Winterbourne run a pre-admission therapeutic community, where patients can have the experience of a therapeutic community for half a day each week before deciding to make a commitment to the full programme.
One of the fundamentals of life in a therapeutic community has been the flattened hierarchy: the idea that all have a voice that is heard and respected; that there is less demarcation between staff and patients and between professionals than in other settings; and that staff members are essentially themselves with the patients, engaging in dialogue that is authentic, meaningful and natural, rather than self-consciously playing the professional role. In the past, this had led some, driven by ideology, to reject the usefulness of expertise and training. It is now generally recognised that the work is difficult and demanding and that knowledge, experience and supervision are essential. Holland, Finland, Norway and Greece all have recognised therapeutic community training schemes, and the Association of Therapeutic Communities in the UK is currently planning a basic training programme. It is envisaged that the training will be consistent with therapeutic community philosophy, with the experiential therapeutic community workshop (already running) being an important component. In this way, it is hoped that therapeutic community staff will be able to establish a professional identity without losing touch with the important idea that patients are in many ways the experts; and that learning – and therefore training – is essentially about developing an open questioning attitude and respect for patients' experience.
The therapeutic community approach
Another strand in the developing practice of therapeutic community ideas has been the work in the old lunatic asylums with patients with psychosis. This has been described as the ‘therapeutic community approach’ as opposed to the ‘therapeutic community proper’, and from the 1950s until the 1970s it was what many psychiatrists meant by the phrase ‘social psychiatry’. A World Health Organization report (1953) describes the most important single factor in the efficacy of the treatment given in a mental hospital as “an intangible element which can only be described as its atmosphere”. It went on to say:
“too many psychiatric hospitals give the impression of being an uneasy compromise between a general hospital and a prison. Whereas in fact, the role they have to play is different from either; it is that of a therapeutic community” (pp. 17–18).
The basic premise was that for people spending a long time in hospital, the way that they lived, the work they did, their personal relationships, the regime, with its rewards and punishments, were more important for their rehabilitation than the medical treatment they might receive. This was revolutionary in the early 1950s, when mental hospitals were closed, prison-like institutions. David Clark first coined the term ‘therapeutic community approach’ for this movement and has written a detailed historical account of the reforming work at Fulbourn Hospital, Cambridge (Reference ClarkClark, 1996).
Although there have been many changes in the intervening years, most noticeably the improvement in psychopharmacological approaches and the move from hospital to community management of patients, the therapeutic community approach continues to raise fundamental questions about the nature and management of mental health problems (see Box 1).
Box 1. Questions relevant to modern practice raised by the therapeutic community approach
Do we nurture the healthy, creative part of our patients or does the system reward the sick, disturbed part?
Do we give enough attention to the importance of patients functioning meaningfully in society and the consequent importance of work and occupational therapy?
Does the prevailing reductionist attitude to risk management fail to acknowledge that a trusting relationship is a prerequisite for therapeutic change and that risk will ultimately be managed within therapeutic relationships?
How can we encourage patients to locate responsibility in themselves when policies such as the Care Programme Approach encourage patients and the public to see professionals as responsible?
With so many medical treatments available, how do we prevent patients becoming passive recipients of a prescription?
Does the keyworker system encourage an unhelpful focus on the individual at the expense of understanding the group or institutional dynamic?
How do we prevent malignant regression, where patients develop hostile–dependent relationships with staff and tend to deteriorate in an in-patient setting?
Therapeutic communities for severe mental illness
The Eric Burden Community in Oxford is a therapeutic community for people with severe schizophrenia. This community is modified, in the sense that many patients are treated against their will under the terms of the Mental Health Act, but in essential ways it is similar to other therapeutic communities (Reference Pullen, Campling and HaighPullen, 1999). The focus is on the community itself as the instrument of therapy, and the danger that the ‘therapists’ will project their own ‘sickness’ onto the patients, who in turn will project away their ‘health and sanity’ is emphasised. Following from this is the idea that staff have ‘therapeutic rights’; in other words, the living–learning environment is for all.
Tucker and her colleagues (Reference TuckerTucker, 2000) develop some of these themes in describing the work of Community Housing and Therapy, a charitable organisation (an offshoot of the Richmond Fellowship) providing community care for those with severe mental health problems. Their careful analysis of the concept of enabling care, the importance of dialogue in promoting education and active participation in the world is of interest to all who genuinely seek to empower their patients.
Another example where therapeutic community principles have been modified and adapted for those with severe mental illness is Davenport's work in Salford in a secure setting with patients with poor-response schizophrenia (Reference Davenport, Mace and MargisonDavenport, 1997 ,Reference Davenport2000). Particular attention is given to potentially harmful interactions between the dynamics of the psychosis itself, early experiences of abuse and the psychology of the institution. The dynamic processes that may interact to produce an anti-therapeutic outcome are examined in frequent meetings in an attempt to avoid re-enacting the dynamics of abuse or being caught up in the dynamics of the institution.
Evidence base
Therapeutic communities have a long history of involvement in research. Much of this has been from a social science perspective and qualitative in nature. Some of it is of importance to other areas of psychiatry, for example methodological approaches to develop, describe and measure the therapeutic milieu, of which the Ward Atmosphere Scale developed by Moos (1997) is the best example. In the past decade, therapeutic communities have started to scrutinise outcome in terms of both cost offset and psychological change. A systematic international literature review of therapeutic community effectiveness for people with personality disorders and mentally disordered offenders found 8160 papers on therapeutic community outcome research (Reference Lees, Manning and RawlingsLees et al1999). A meta-analysis of suitably controlled studies showed a substantial positive effect.
In addition to work being done by individual therapeutic communities, the Association of Therapeutic Communities Research Group is involved in coordinating collaborative initiatives. A randomised control trial (RCT) of therapeutic community day care is currently being planned, but there are a number of methodological difficulties setting up RCTs in therapeutic communities, in particular, the fact that therapeutic communities are multi-dimensional – consisting of a great many ‘molecular’ variables that interact in a complex way. Controlled trials are of more value when the treatments being compared can be regarded as ‘molar’ variables. Other methodological difficulties are listed in Box 2.
Box 2. Difficulties of applying randomised controlled trial methodology to therapeutic communities
The complex and volatile nature of the treatment being measured
The heterogeneity of the clinical population
The diversity of therapeutic community approaches
The relatively small numbers involved
The need for long-term follow-up
Finding appropriate outcome measures
Establishing a suitable control group
Ethical issues of not treating (especially the high risk of suicide in this group)
Finding an equipoise for randomisation (‘installation of hope’ is a therapeutic factor)
The non-independence of observations
One alternative to the experimental design is the exploitation of natural variations, by comparing large numbers of settings and using their natural differences to explore relationships. A cross-institutional project using this idea is being set up involving 24 therapeutic communities in the UK (www.pettarchiv.org.uk/atc-protocol.htm).
Perhaps the most influential studies recently have been those looking at cost effectiveness (Reference Davies, Campling and HaighDavies, 1999). For example, Dolan et al (1996) compared the service usage (psychiatric and prison) of Henderson Hospital residents for 1 year pre- and post-treatment. They found that service usage following treatment was reduced to such an extent that the cost of therapeutic community treatment would be recouped within 2 years. Davies et al (1999) compared patients' usage of psychiatric in-patient services 3 years pre- and post-treatment at Francis Dixon Lodge and showed a similar reduction. By comparing referrals from within and outside their own area, they also suggested that a local service may have a preventive cost-offset function: in other words, patients are referred at an earlier point in their career before utilising other resources inappropriately.
Conclusion
Therapeutic communities have a valuable role to play in the future of mental health services. Within the NHS, they have established a niche for those suffering from severe emotionally unstable personality disorder – a group of high-risk patients who become heavy users of services if they do not get the long-term intensive psychosocial therapy that they need.
There is a growing body of research suggesting that therapeutic community treatment has a positive effect. Cost-offset studies suggest that therapeutic communities pay for themselves in the medium term. Service provision, however, is currently patchy and poorly coordinated, resulting in ‘post-code prescribing’ based on the availability of a local therapeutic community. This suggests that many people with clinical need who could benefit are not referred for treatment. The National Service Framework promotes the view that all patients should have equal and equitable access to psychosocial assessment and treatment. This should include therapeutic communities for those who would benefit, with the added incentive that therapeutic communities are a valuable training resource for a wide range of mental health professionals.
The application of therapeutic community ideas has had a significant impact on the practice of psychiatry. The need for caring asylum has not gone away, and with many acute admissions wards in therapeutic crisis it is becoming a pressing problem. The task is to provide therapeutic social environments where people are able to “express feelings and views, engage in fulfilling activity and participate in decisions affecting their lives” (Byrt, 1999: p. 73). Therapeutic community ideas continue to raise fundamental questions and challenge mental health professionals to think more positively and creatively about the potential within their patients.
Multiple choice questions
-
1. The following people are associated with the development of therapeutic communties:
-
a Maxwell Jones
-
b Sigmund Freud
-
c Wilfred Bion
-
d Tom Main
-
e Donald Winnicott.
-
-
2. Concept or behavioural therapeutic communities:
-
a are appropriate for patients with schizophrenia
-
b are appropriate for patients with problems of drug addiction
-
c are being developed in the prison service
-
d treat patients with obsessive–compulsive disorder
-
e encourage confrontation.
-
-
3. The following are true of democratic therapeutic communities:
-
a primitive regression is encouraged
-
b residents are encouraged to do whatever they like
-
c a rigid hierarchy is enforced
-
d there is a structured programme
-
e a culture of enquiry in which everything can be questioned is encouraged.
-
-
4. Therapeutic community ideas have been applied to the following institutions:
-
a prisons
-
b schools
-
c community homes for those with mental illnesses
-
d surgical teams
-
e secure psychiatric units.
-
-
5. The following are fundamental qualities of a therapeutic environment:
-
a aromatherapy
-
b dialectical–behavioural therapy
-
c a culture of belonging
-
d a culture of empowerment
-
e open communication.
-
Therapeutic community principles
| Theoretical principal | Origin in development | Culture in a community | Structures in a community | Rapoport's original community themes |
|---|---|---|---|---|
| Attachment | Primary bond, losses as growth | Belonging | Referral, joining, leaving | |
| Containment | Maternal and paternal holding | Safety | Support, rules, boundaries | Permissiveness |
| Communication | Play, speech, others as separate | Openness | Groups, ethos, visitors | Communalism |
| Involvement | Finding a place among others | Living–learning | Community meeting: agenda and structure | Reality confrontation |
| Agency | Establishing self as seat of action | Empowerment | Votes, decisions, seniority | Democratisation |
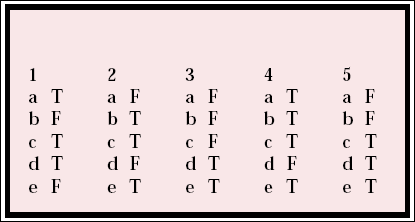
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | F | a | F | a | T | a | F |
| b | F | b | T | b | F | b | T | b | F |
| c | T | c | T | c | F | c | T | c | T |
| d | T | d | F | d | T | d | F | d | T |
| e | F | e | T | e | T | e | T | e | T |





eLetters
No eLetters have been published for this article.