The practice of brief psychotherapy is a distillate of the active ingredients in longer-term work but with the addition of two special elements: limited time and therapist activity in formulating a focus and focusing on it. Typically, patient and therapist work together over 10 to 25 sessions in weekly meetings. In very brief dynamic psychotherapy (VBDT), the time frame is shrunk to fewer than 10 sessions, sometimes just a single session; the constraint means that there is less room for corrective manoeuvre in order to achieve the therapeutic task of maximum benefit and minimum harm in the time available. To do this well requires knowledge, skill and sensitivity. In this paper, special attention is paid to a ‘three-plus-one’ intervention (brief intervention and follow-up (BRF)) that has been tested in a randomised controlled trial (RCT).
Historical overview
Psychoanalysis
Paradoxically, early psychoanalyses were brief in duration. Often, they were concluded in a few sessions. It was only as they became more ambitious in scope, seeking to exhaust the potential for neurosis and having to face up to the intractability of human nature, with its compulsion to repeat, that they expanded into the popular stereotype of five sessions per week for 5 years. When such therapy is depicted as being endless in time and endless in goal, it offers an irresistible target to its critics. In the uproar of one-sided attack, the enduring contributions of psychoanalysis tend to be forgotten. These include careful attention to meaning, the importance of complex motivation and psychological conflict in determining behaviour, the distortion through use of mental mechanisms of reality perception (self and others) and the crucial importance of childhood experience in development.
In classic psychoanalysis, there is an illusion of timelessness, which is given encouragement by the open-ended nature of the contract. This illusion has benefits for the patient that we need to bear in mind when considering VBDT. At its best, psychoanalysis offers the patient a unique experience of a free space; there for the person to use as he or she wills, with no preconditions, no prejudgements, a platform for exploration and self-observation, a world in which the deeper recesses of psychic reality can be discovered, a place in which progress can be made at a pace the patient can tolerate (Reference Aveline, Palmer-Barnes and MurdinAveline, 2001). In contrast, VBDT demands speed and compromise in the scope of what can be addressed.
Psychodynamic origins of VBDT
The father figure of brief therapy is Franz Alexander, a Hungarian émigré and founder of the Chicago Institute for Psycho-Analysis. His 1946 book caused outrage in orthodox analytic circles (Reference Alexander and FrenchAlexander & French, 1946). Alexander and his colleagues fine-tuned therapy to improve the chances of the patient having a ‘corrective emotional experience’:
“In all forms of etiological psychotherapy, the basic therapeutic principle is the same: to re-expose the patient, under more favourable circumstances, to emotional situations which he could not handle in the past. The patient, in order to be helped, must undergo a corrective emotional experience suitable to repair the traumatic influence of previous experiences. It is of secondary importance whether this corrective experience takes place during treatment in the transference relationship or parallel with the treatment in the daily life of the patient.” (Alexander & French, 1946: p. 66)
Note both the emphasis on lived experience, that is, on helping the patient
“to face again and again, under more favourable circumstances, those emotional situations which were formerly unbearable and to deal with them in a manner different from the old” (Alexander & French, 1946: p. 67),
and the commonsense valuing of experience and change in daily life as well as within the transference relationship in the consulting room. To understand what might be a corrective emotional experience for a particular patient, the therapist has to formulate the problems and plan the treatment. The conscious intentionality that this implies was anathema to some analysts but paved the way for Alexander to vary the frequency, focus and transferential style of the therapist in order to promote certain kinds of interaction, e.g. kindness for guilt, acceptance for benign dependence and reduced contact for more malignant regression.
Cognitive–behavioural therapy
Of particular relevance to VBDT is the cognitive–behavioural therapy (CBT) focus on teasing out the detail of how symptoms arise and what goes wrong in interactions (cognitively and behaviourally): the antecedents, the behaviour that results and its consequences (Reference Nemeroff, Karoly, Kanfer and GoldsteinNemeroff & Karoly, 1991;Reference EllisEllis, 1994). Homework is also very important. Completion is an indicator of involvement: success breeds success. The homework technique underlines the message that therapy is about change (Reference Blackburn and DavidsonBlackburn & Davidson, 1990).
Single sessions, Balint, EAPs, GP counselling, Yalom ward groups
There has been long-standing interest in what can be achieved in single sessions. Malan was surprised to find genuine improvement at follow-up among patients with neurosis who had been assessed but not taken on for therapy (Reference Malan, Heath and BacalMalan et al1975). For these patients, the assessment had been an important encounter, occurring at an auspicious time in their lives (‘kairos’) and presenting them with a formulation of their problems, which deepened understanding and helped them see a new way ahead. Balint saw great potential for psychological understanding and change in general practice consultations, with the doctor as the active drug reaching past the presenting problem to the real ones (Reference BalintBalint, 1968). There has been a major expansion of counselling in primary care and at work (Employee Assistance Programs (EAPs)), offering one, two or three sessions, rarely more than six. In group therapy on wards, Yalom, the doyen of interpersonal group therapy, advocates treating each meeting as if it were a complete group therapy in itself (Reference YalomYalom, 1983).
Common therapeutic factors
Frank (1973) has argued convincingly that in all effective therapies six influential factors are operative. Therapy provides (1) an exploratory rationale and facilitates (2) the exploration of traumas and conflictual issues in a state of emotional arousal. The effect is strengthened (3) when the therapist is sanctioned as a healer by the society. Responding to patients' requests for help (4) encourages them to be hopeful about themselves and counters the demoralisation that typifies most patients' states. Therapy provides or prompts (5) success experiences, which enhances a sense of mastery, thus countering demoralisation. Finally, psychotherapy provides (6) an intense confiding relationship with a helping person.
These factors have a much greater influence on outcome than the contribution made by approach-specific theory and technique; in Lambert's (1986) review of empirical studies, common therapeutic factors accounted for 30% of the therapeutic effect, technique 15%, expectancy (placebo-effect) 15% and spontaneous remission 40%.
Soul of change
Hubble et al (1999) have taken these ideas further. They see successful therapy as being that which assists the person's natural capacity for healing. Each person has his or her own theory of change, which is an emergent reality in the therapy, there to be prized and learnt from. The therapist has to be sufficiently flexible to work congruently and creatively with the patient's world-view. Technique acts, then, like a magnifying glass, focusing the forces for change and causing them to ignite into action.
Best of breed
Although this paper is about dynamic VBT, there is clearly convergence between CBT and dynamic principles. Given the brevity, there is inevitably a cognitive flavour to the work, an appeal to what the patient can readily bring to mind. The principles of focus on present-day real-life problems, formulation, flexibility and some form of corrective emotional experience are central to VBDT but inform much of current brief therapy practice.
Research foundations for brief therapy
Brief therapy
Over the past 30 years, there has been a considerable development of brief dynamic psychotherapy, grounded in empirical research (Reference MalanMalan, 1963;Reference Strupp and BinderStrupp & Binder, 1984; Reference Lambert and NorcrossLambert, 1986; , Reference Luborsky, Crits-Christoph and AuerbachLuborsky et al1988; Reference RyleRyle, 1990; Reference Messer and WarrenMesser & Warren, 1995). Central to these approaches is the formulation of an operational understanding of the patient's difficulties, based on the narrative of the history and clinical observation of the relationship patterns shown at assessment and in therapy sessions. Malan terms this the psychodynamic or explanatory hypothesis, Strupp & Binder the dynamic focus, Luborsky et al the core conflictual relationship theme (CCRT) and Ryle the procedural sequence model, which is expressed in a written reformulation. In these brief psychotherapies, the therapist identifies at an early stage a dynamic focus, which is of central importance in the genesis of the patient's difficulties and to which the closest attention is paid during the therapy. This selective focus, together with the urgency confirmed by the constraint of a time-limit, form the two principal ingredients in the demonstrated success of this approach. Successful outcome correlates with early positive therapeutic alliance (by session 3), therapist activity, the prompt addressing of negative transference and focused work with intrapsychic and interpersonal conflicts of central importance to the patient (Box 1).
Box 1. Enhancing effectiveness: research evidence
Early positive therapeutic alliance (by session 3)
Therapist activity
Prompt addressing of negative transference
Focused work with intra-psychic and interpersonal conflicts of central importance to the patient
Most forms of brief dynamic psychotherapy investigated have durations of between 12 and 25 sessions. The most detailed UK study was done in Sheffield. In the first Sheffield Psychotherapy Project (Reference Shapiro and FirthShapiro & Firth, 1987) prescriptive and explorative psychotherapy were compared in a 16-week cross-over design with businessmen with moderate depression. The subjects had work-related stress. Both therapies were effective, with a slight advantage in this treatment population for the directive therapy.
The Sheffield model: two-plus-one intervention
As an off-shoot of the Sheffield Psychotherapy Project, Barkham (1989) and Barkham & Hobson (1989) argued in favour of a two-plus-one model, in which patients are seen for two sessions 1 week apart followed by a third session 3 months later. In their model, an immediate or key issue is addressed and effort is made to enable the patients to experience themselves effecting change in their lives. Barkham et al (1999) have reported work using two forms of therapy (CBT and psychodynamic–interpersonal therapy) within this time model in an RCT on sub-syndromal depression.
The Nottingham model: three-plus-one (BRF)
Origins
In Nottingham, we have concluded an RCT, funded by the Mental Health Foundation, into the effect of brief intervention and follow-up (BRF) in comparison with the standard assessment procedure for dynamic psychotherapy (further details avaliable from the author upon request). We are a specialist psychotherapy department providing tertiary health care in the NHS, and referrals far outstrip our limited clinical resource. We were and are very concerned that the consequent waiting-list for psychotherapy may compound the patient's problem, either through further social breakdown or the ossifying force of chronicity. On the basis of the research literature, we devised a brief intervention as an experimental treatment at the time of referral. Our hope was that this might help in three ways: (1) as a sufficient therapy for some, (2) to identify those who need longer work and initiate it and (3) to conserve resources by excluding those who would not benefit from explorative psychotherapy.
In BRF, the patient is seen for four sessions in total: for an assessment interview, then for two therapy sessions during the second, third or fourth weeks and, finally, for a follow-up session at 3 months. The decision about entry into therapy is made collaboratively at the final session. This is a three-plus-one intervention. In standard assessment, the patient is seen for a single assessment interview.
Power analysis required a cohort of 68 BRF and 68 standard-assessment controls matched for age, gender, educational achievement and severity of problems. The sample was formed from referrals to the author for dynamic psychotherapy. Independent assessment of target problems, symptoms, self-esteem, problems in interpersonal relationships and other relevant aspects was made by a research psychologist at 0, 4, 15 and 36 months.
Results
In total, 267 referrals for assessment for specialist psychodynamic psychotherapy were entered into the trial. Complete data were achieved on 156 subjects at time 0 and at 4 months.
The three-plus-one intervention provided sufficient therapy for only 6% of subjects (standard assessment: 3%). More detailed and patient-informed assessment was done in the three-plus-one intervention and, as a consequence, more subjects were judged to be unsuitable for specialist psychotherapy (50%) in comparison with standard assessment (21%) (number needed to treat = 3.4; OR 3.70; 95% CI 2.08–6.66). Regardless of outcome, patients preferred the three-plus-one intervention. While the three-plus-one intervention was resource intensive, there was an overall cost saving of between 8.5 and 5.7 sessions per patient not put on the waiting list for subsequent therapy.
In our patient population, BRF was an insufficient therapy for most, but it does provide a therapy close to the time of referral, conserves resources, has face validity and is liked by patients. Consequently, we have adopted the three-plus-one intervention as our standard form of dynamic assessment.
Practice of the Nottingham three-plus-one intervention
Context and framing
Brief intervention and follow-up (BRF) developed in a particular context as part of assessment for specialist dynamic psychotherapy. While it is a therapy in its own right, the sessions link in both patient's and assessor's minds to the possibility of more therapy at a later date, entered into from the waiting-list. This is made explicit by saying to the patient at the very beginning:
“The way that we are going to do this assessment is to do some work with the issues that are important to you. This will help you know more about dynamic psychotherapy and, from your reaction, whether or not this form of therapy is likely to be helpful for you. After session three, there will be a 2-month gap which will be an opportunity for you to put into practice the things that we have talked about. At session four, we will decide together if more therapy is needed and what kind.”
Framing is important as it helps both parties know what they are engaged in. In another setting, the framing might be simply on doing what can be done in the time available.
Examples of recent central issues
The case vignettes below are examples of VBDTs that illustrate the BRF method. The first is about an agonising choice where loyalty and idealisation are in conflict and both may be destroyed. In the second, the patient is faced with a most uncomfortable alternative view of his motivation. In the third, the patient only wants the external problem to go away. Exploring and revealing are alien processes in her way of being and are respected.
Case 1: ‘speak or die’
Samantha has been in an agony of conflict for over a year. Her 40-year-old life was turned upside-down when her sister confided that she had been sexually abused by their father and swore her to silence. Up to that point, Samantha had admired her parents for bringing them up happily despite circumstances of poverty. She loved her father and was especially close to her mother. Now, she felt unable to speak to her mother, inwardly fearing that her mother must have known of the abuse, but constrained from asking because of her promise to her sister. The secret was tearing her apart; her mother could not understand Samantha's change in attitude. It was no exaggeration to say that her survival was on the line; suicide often seemed the only solution. The central issue in her VBDT was her life or her promise.
Outcome She chose to break her promise and spoke with her mother. There had been abuse but, despite that, she was reconciled with her mother. For the sister, it seems that conflicting feelings of hate for being abused and love for being the favoured one prompted her to spoil Samantha's view of their father and obstruct resolution. Destroying the idealisation through bringing history into the open made her sister hate Samantha even more. The VBDT was enough to move Samantha's life on.
Case 2: the man who hates women
“Why, when I am such a helpful person, do women always go off with other men?” Aged 32, John lends a supportive ear to the emotional problems of his female friends but, in the end, he is left alone. He has never had a relationship. It all seems so unfair to him. He lusts after women and is tormented by the sounds of sex coming from his lodger's bedroom. Even worse, the lodger is a woman and, he adds disparagingly, “fat and ugly”. The only area of his life that he can control is physical activity. He exercises obsessively, finding in that comfort for disappointment and distraction from crippling anxiety that interferes with work. His thinking is rigid. He is sure that the fault lies with women and their fickleness. Frustration turns women into hateful deniers. In the transference, he is scornful and attacking. The central issue in his VBDT was the hate for women that lies just beneath his surface appreciation and his willingness to face this and attempt to modify it.
Outcome The psychotherapy message of “look at yourself and accept responsibility for the contribution you make to your problems” was not welcome. He made a half-hearted acceptance and accepted an offer of group psychotherapy, knowing that that would be a place in which he could see himself in relation to others and experiment with change. He knows with his head but not yet with his heart that change will be uncomfortable and difficult. He will need at least 18 months in a group.
Case 3: the woman who wants to be left alone
“I came because my solicitor said I should.” Rachel is separated from the father of her 4-year-old son. If she could, she would have nothing to do with him at all. He sees their son on neutral ground, a reception centre, but is pressing for increased access. Rachel is outraged. Unusually for someone in this position, she will not give details of why she so passionately objects. Indeed, as we talk, her life is full of no-go areas. Urging her to be more explicit only brings out a more suspicious, almost paranoid, side to her nature. Without consciously linking the two, she reacts to our exploration in the session with stories of sexual perversity by neighbours. It is difficult to know where the boundary lies between fact and fantasy but the timing of her utterances points to bad past experience and deep disturbance, brought closer to the surface by inquiry. What is clearer is a long pattern of functioning better at a distance from others, not sharing a home and concentrating on her animals and her painting, at which she is talented. Faced with any challenge that would result in her coming more into the open, she goes yet further to ground. Currently, this pattern is working against her, as she is not giving her side of the story to the social worker appointed by the Court to decide on access. The central issue in her VBDT is her independence and the negative effect of her ostrich-like stance. “Psychotherapy is not compulsory”, I say. It is only if there are psychological issues that she identifies and wants to do something about that we would be in business. We talk about her discussing with her solicitor what to tell the social worker.
Outcome She does not attend her final appointment in the three-plus-one intervention. I hope this means that she argued her case to best advantage and that on some level, unlikely as it seems now, she knows that she could return if she ever wanted to work on her way of relating.
Key features
Time
Time is precious and finite. It has to be made the most of. This attitude of mind is helpful to patient and therapist alike, and underlines the fact that their time together is a window of opportunity for saying important things to each other. Working briefly, however, is not a mandate for the therapist to rush the patient unduly, swamping him or her with all the insights that might be faced in a considered way in a long therapy. It does mean being sensitive to what the patient can bear to face and being explicit about the time frame and the purpose of the encounter.
Structure
The structure of three-plus-one intervention expresses its logic. The first session, of 1–2 hours, facilitates entry into the patient's world, doing justice to the problems that have been brought. The conversation continues at weekly intervals (as near as can be arranged), amplifying the beginning, focusing on core conflicts and working towards taking stock and a temporary end in session 3. Recurrent questions are: What has been stirred up? How did it feel? What change, if any, has occurred? How did the change come about? The last taps into the patient's theory of change and, if positive, is praised. The 2-month break before the final session is long enough for problematic situations to occur and be tackled by the patient but not so long that the therapy is forgotten.
Box 2. Key features
Focus on present-day, real-life problems
Formulation (see Box 3)
Frame focus on what is of central importance
Flexibility: adapt to what is needed
Some form of corrective emotional experience
Crises are opportunities for change
Reinforce patient's natural capacity for healing and change
Box 3. Formulation
Move discussion from the symptomatic to the psychological
Work out the central interpersonal issues
Derive these from detailed examination of recent problematic interactions
Central issues are likely to be recurrent
Issues may pose choices for the patient, e.g. to explore or ignore, to change or accept
Termination
Ending has to be spoken of from the outset. Ending is set by the time frame of the VBDT; it may coincide with some resolution of problematic issues or with the point at which a new perspective on the patient's problems is emerging. Ending is where a new phase of work by the patient begins, consolidating and extending any gains made.
Focus
My focus is interpersonal. In order to cope with particular situations, prototypically difficult ones, people learn adaptive patterns. Later, these patterns become maladaptive as they are repeated in new contexts that, ideally, would be approached in fresh ways. Persons and contexts interact and mutually influence. What one person does evokes reciprocal or complementary reactions in the other – abuse and submission, kindness and trust – and, thereby, sets going the next stage of reaction and counterreaction. It is person and persons in overlapping systems of interaction, showing their history in what they feel and do, and creating their future in the collective authoring of the now. The stern demand of explorative psychotherapy is to see and accept one's own contribution to problems in living and to make changes. In this, brief interpersonally focused psychotherapy is no different from long-term work. It is just that the core of the problems has to be addressed quickly.
Central issues: establishing, translating, agreeing and truth-speaking
Brevity and depth can be companions, not antagonists. Getting to the heart of the matter quickly is all-important. The therapist has to be agile, moving back and forth from hearing and feeling what it is like to be the patient to observing and formulating the central issues. The therapist draws upon his or her own experience in the session, the transference and the countertransference. Emerging insights are fed back to the patient, sometimes as reflections, sometimes as interpretations, for correction and amplification. The aim is to reach agreement on the underlying issues. This may require the translation of symptoms into processes, an essential step in Case 1, an unwelcome one in Case 2 and an imprudent one in Case 3. In all cases, there is an attempt to speak the truth. How vehemently that goal is pursued depends on clinical judgement of the patient's resilience and readiness to go further. Cases 1 and 3 are at the opposite ends of a spectrum, the former illustrating a difficult but essential step, the latter a recognition of fragility and risk of decompensation.
There is a substantial descriptive and research literature on formulation models (see Eells, 1997, for an excellent overview). In Nottingham, we have drawn upon Luborsky's CCRT and Strupp's dynamic focus models to create our own Core Conflicts Form (available from the author upon request).
We use this form in consensus discussion in assessment supervision meetings. In another setting, practitioners could use it to summarise their assessment. The focus is on narrative about formative interactions during the patient's life, described or demonstrated by him or her in the assessment, in any questionnaire completed and in the referral material. The interactions of interest are those that have shaped that person's view of self and of the world. Recent problematic interactions are of special interest, particularly if they are recurrent. These are the hot areas, where the individual's contribution is critical. When problems are enacted in the session, there is a powerful opportunity for direct address. In the form, relationship elements are linked: formative acts and events feed into feelings about self and, in turn, into relationship responses to others. Characteristic favourable and malign sequences may form. Therapy aims to foster the preferential use of mature patterns over maladaptive ones. Risk factors is a self-evident category but restorative factors is there to remind the therapist that there is more to the patient than a psychopathology. People have strengths, abilities and natural ways of coping.
Responsibility and personal choice
Knowing what the underlying issues are is the foundation for dynamic psychotherapy. As that knowledge develops, patients can take more responsibility for the contribution (I emphasise contribution) that they make to recurrent difficulties and decide what, if anything, they want to do about it. In this, they have choice but no guarantee of success (an enraging disappointment for Case 2). A VBDT helps that choice to be an informed one. Useful questions in defining the nature of the task are: What would you do if you were more able in your life? What do you need to change in yourself in order to be different?
Activity
Both therapist and patient are active in VBDT. The therapist has to contain his or her anxiety about the magnitude of the task, the brevity of the therapy and the risk of leaving the patient in the lurch with the work half done and focus on what can be done safely and usefully in the time available. The objective is more than assessment; it is to be therapeutic. Careful attention has to be paid to the implications of what is said on the patient's life and to tempering confrontation with professional responsibility. But the acid test of psychotherapy is change in the patient's life. Hence, the message of VBDT is think and do, reflect and act, consider and change. Both within the sessions and in the patient's ordinary life, the therapist looks for opportunities for the patient to take ‘significant action’ (Reference Aveline and DrydenAveline, 1988 , Reference Aveline and Dryden1996). This is action of personal significance for the patient that, once succeeded in, will loosen the hold of self-limiting patterns of interaction. It will be a ‘corrective emotional experience’. Some dynamic therapists prefer to be less active in promoting significant action, but all use the opportunity of repeated meetings to check what impact the sessions are having, especially the effect on self-view and view of others. In Case 1, Samantha had protected herself from thinking critically about her mother and to a lesser extent her father by idealising them. The price was some limitation in perception of her family world. In thinking with the therapist about her sister's accusation, she had to face her ambivalence to her sister and mother. Initially, the process of taking significant action was uncomfortable and guilt-ridden. Later, she felt liberated.
Anticipation of problems, week to week and post therapy
When therapy works, it is a catalyst to change. Change occurs through encountering personally difficult situations and transcending old, self-limiting ways of interacting. Its beneficial effect continues as the patient engages with his or her life in a different way. Life does not change in abstract; it has to be lived. Looking forward to problematic situations and anticipating how they might be tackled in new ways heightens the urgency of the VBDT process. A man is about to go to a funeral, wanting to show his love and grief but fearing breaking down and fracturing a lifetime of safe reticence. A woman recoils from her mother-in-law's hug; she craves the hug but inwardly has never felt loved and now feels unlovable. Change is to do what is personally difficult: to cry, to hug in these two examples. As the VBDT ends, what the patient might work on in the next 6 months is explored and agreed.
Reviews
While the three-plus-one intervention is fine for many, the frame can be altered. Especially when there is good progress, a review after a further 3 or 6 months can help maintain momentum. That advantage has to be balanced against the risk of fostering unhelpful dependence.
Application and training
The Nottingham three-plus-one intervention developed in a particular context in which many patients have further therapy after BRF. In other settings, it could be a stand-alone therapy or a first offer in a psychotherapy service. It is certainly within the capability of most departments of psychotherapy. It is not suitable for those with vestigial ability to trust or needing to tell their story in depth, but it can begin a beneficial process that subsequent work may advance. The therapist needs to have a keen appreciation of what can and cannot be achieved through dynamic psychotherapy and at what emotional cost. Being flexible is vital. Therapy has to be adapted to what the patient wants and can cope with. This is skilful work in which a particular attitude of mind is helpful (see Box 4). Supervision is important. It helps the therapist to discern an appropriate focus, stay with it and temper therapeutic ambition with responsibility.
Box 4. The brief therapist: attitudes of mind
Prizes pragmatism and parsimony
Sees change as inevitable in life
Accepts that many changes will occur after therapy is concluded
Emphasises patient's strengths and resources
Does not accept timelessness of some models of therapy
Sees being in the world as more important than being in therapy
This three-plus-one intervention has not been tested in other settings. However, it brings together in a single package the elements that have been found to contribute to effectiveness. The method provides time for assessment, therapeutic work and review. It promotes change and faces patients with the challenge of choice and personal responsibility. It could therefore form the basis of an out-patient intervention in general psychiatry, either as a stand-alone brief therapy or as a preparatory text before referral to specialist psychiatry.
Multiple choice questions
-
1. The term ‘corrective emotional experience’ was coined by:
-
a Strupp & Binder
-
b Malan
-
c Alexander & French
-
d Luborsky
-
e Ryle.
-
-
2. Research associates good outcome with:
-
a an initial deterioration in therapeutic alliance
-
b not challenging negative transference
-
c therapist activity
-
d having an agreed focus
-
e open-ended therapy.
-
-
3. The Nottingham trial of VBDT:
-
a was a non-randomised matched pairs series
-
b was a test of a two-plus-one intervention
-
c was manualised
-
d had follow-up points at 4, 15 and 36 months
-
e was located in primary care.
-
-
4. Dynamic formulation:
-
a is jointly authored between patient and therapist
-
b focuses on central issues
-
c provides a map for future psychological work
-
d identifies reciprocal and complementary reactions
-
e authorises the therapist to set the agenda.
-
-
5. Very brief dynamic therapy:
-
a is a total solution for psychological problems
-
b poses choices for the patient
-
c requires responsible action by the therapist
-
d is symptom focused
-
e can enable the patient to take significant action.
-
MCQ answers
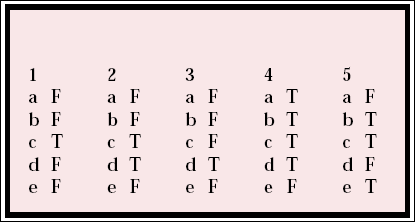
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | T | a | F |
| b | F | b | F | b | F | b | T | b | T |
| c | T | c | T | c | F | c | T | c | T |
| d | F | d | T | d | T | d | T | d | F |
| e | F | e | F | e | F | e | F | e | T |





eLetters
No eLetters have been published for this article.