At present, the elderly constitute 18% of our population but receive 45% of prescribed drugs (Royal College of Physicians, 1997). Many patients (78%) receive medication via a repeat prescription system and for approximately a quarter of prescriptions written for this age group, patients have not seen their doctor for over a year. A substantial proportion of the elderly live not in their own homes but in residential or nursing homes, and a small number live hospital. Prescribing and administering medicines poses different problems in each of these settings.
Prescribing medication for the elderly has long been recognised as requiring special expertise and knowledge. There are three main reasons for this. First, the pharmacokinetics and pharmacodynamics of drugs are different in an older person compared with a younger one and hence the elderly are more susceptible to adverse drug reactions and drug interactions. These topics have been well covered elsewhere (Reference Mayersohn, Evans, Schentag and JuskoMayersohn, 1986). Second, the prevalence of dementia among people aged over 65 years is 5% in the community and 80% or more in residential or nursing homes (Reference Macdonald, Davies and CraigMacdonald, 1998). Psychotropic medicines are prescribed to treat the behavioural disturbances and agitation associated with dementia, despite the limited evidence base for their use in such settings (Reference Kirchner, Kelly and HarveyKirchner et al, 2000). Third, there are the questions of capacity and consent and how we treat patients with dementia. Although concern usually centres on incapacitated patients who do not comply with medication, equally or perhaps more vulnerable are the group of incapacitated patients who do comply. It is essential that vulnerable patients who cannot choose receive good-quality care with the minimum of obstruction, but also with adequate safeguards to prevent abuse.
Evidence-based practice with elderly patients
Almost all treatments that are given to elderly patients have been rigorously studied only in younger adults with one or a few medical problems. The evidence base that guides the use of therapeutic agents in frail elderly patients with multiple pathology is very limited. Ethically, this presents a complex challenge. It is essential that we treat patients even where the evidence base is limited, but we must be aware of the danger of overtreatment and inappropriate treatment. An interesting example of this is the case of Re C (1994; see below), where the medical view that treatment was required to save life was proved wrong when the patient survived without the treatment. Doctors must therefore be both humble about the limitations of their diagnostic skills and treatments and to provide care even where the evidence base is weak.
This dilemma is well illustrated by the controversy surrounding the management of the behavioural complications of dementia (Reference Ballard and O'BrienBallard & O'Brien, 1999). Antipsychotics are commonly prescribed to treat agitation and behavioural disturbances, although there is a feeling among doctors and nurses that such medicines do not always help to control these behaviours, especially non-violent restiveness and sexual inappropriateness (Reference ThackerThacker, 1996). This feeling is supported by systematic reviews that have failed to demonstrate substantial evidence for the efficacy of these drugs, for example, thioridazine (Reference Kirchner, Kelly and HarveyKirchner et al, 2000). Recent studies have demonstrated some benefits with risperidone (Reference Katz, Jeste and MintzerKatz et al, 1999) and olanzapine (Reference Street, Scott Clark and GannonStreet et al, 2000) in controlling disturbed behaviour in patients with severe dementia, but the overall evidence base for the use of psychotropic medication remains poor. There is a strong clinical need to manage such behavioural problems and to alleviate torment in distressed individuals who cannot understand what is happening to them. As a result of this, the use of psychotropic drugs for this purpose seems likely to continue.
Elsewhere, we now have better evidence that antidepressants (Reference Evans, Hammond and WilsonEvans et al, 1997) are effective in treating depression in frail elderly people with multiple pathologies. There is also some evidence to suggest that aggressive behaviour is associated with untreated depression, thus indicating antidepressants in these circumstances (Reference Lyketsos, Steele and GalikLyketsos et al, 1999). Despite this, the access of patients to such treatments remains problematic. Antidepressants are underused, depression often being seen as understandable in elderly patients, and therapeutic nihilism may lead to the undermanagement of problems among such patients (National Institutes for Health, 1992).
Access to care: overtreatment and undertreatment
Patients are also concerned about side-effects and long-term harm. They will often prefer no medicine whenever possible. This is probably even more common for psychotropic medications. The belief that patients with dementia are administered psychotropics simply to quieten them down and reduce the demand on carers (the ‘liquid cosh’) remains prevalent. The Omnibus Budget Reconciliation Act (OBRA) guidelines (Reference Zaleon and GuthrieZaleon & Guthrie, 1994) (see Box 1) were introduced in the USA in 1987 following evidence to suggest that a high proportion of elderly patients in long-term care facilities were receiving antipsychotics for non-specific indications, with inadequate monitoring for either efficacy or adverse effects. These guidelines recommend that antipsychotic drugs should not be prescribed in the absence of a specific documented indication and that ongoing monitoring for efficacy and side-effects is essential. There is a trend towards using atypical antipsychotics, but the level of monitoring shows little sign of improvement (Reference Beck, Paton and EubaBeck et al, 2001). This trend will almost certainly increase following the recent withdrawal of the product license for using thioridazine to control behaviour among elderly patients with dementia in UK and the USA.
Box 1. Omnibus Budget Reconciliation Act (OBRA) guidelines (Reference Zaleon and GuthrieZaleon & Guthrie, 1994)
-
• An antipsychotic may be used only for a specific condition (see below) for which a supporting diagnosis has been documented and that any resident taking an antipsychotic should receive gradual dose reductions and behavioural interventions, unless clinically contraindicated, in an effort to discontinue these drugs
-
• Appropriate conditions include schizophrenia, acute psychotic episodes and certain documented psychotic or agitated behaviours associated with organic mental syndromes
-
• Inappropriate conditions include wandering, restlessness and agitated behaviours that do not represent a danger to the patient or others
-
• Antipsychotic medication should only be given on a prescription basis under certain circumstances, such as:
-
(a) when making dosage adjustments to regular antipsychotic medication;
-
(b) to manage unexpected harmful behaviours (this should occur no more than twice in 7 days without an assessment of the cause and development of an appropriate care plan)
-
-
(c) Two sets of guidelines, one for ‘psychoses' and one for 'organic mental syndromes’, give the maximum daily dosage of specific antipsychotics that should be given to older adults
Of equal or perhaps greater concern has been the poor availability of new treatments for elderly patients. It is well known (Anonymous, 2000) that the new anti-dementia drugs have been slow to receive support from funding organisations and (in the UK) still remain unfunded, with severe constraints on provision 3 years after the launch of donepezil. Response to the problem has been patchy. The Standing Medical Advisory Committee (SMAC) of the UK Government advised their use supervised by secondary care in 1998, but with an absence of funding for their use from several health authorities uptake remained low. The UK National Institute for Clinical Excellence (NICE; 2001) has recently come to the same conclusion as SMAC. With central government support in implementation, the NICE guidance should lead to treatment becoming more uniform across the UK.
There is also a perception that the elderly in general do not have as many health care options made available to them as they might expect. There was considerable discussion about quality of care issues for the elderly at the end of 1999 (Daily Telegraph, 6 December 1999). The UK Government's National Service Framework for the Elderly (Department of Health, 2001) requires clinicians and authorities to ensure that each patient gets the treatment he or she requires and to “root out ageism”.
Ethical issues of consent
The ethical principles surrounding consent to treatment in the elderly vary according to the patient's mental capacity and his or her reaction to the treatments offered. Table 1 shows the four levels of agreement to treatment that an individual can give.
Patients require a discussion of risk, benefit, likely side-effects and potential serious adverse reactions. Not all side-effects need to be discussed (British Medical Journal Legal Correspondent, 1985), but important ones such as tardive dyskinesia for neuroleptics and lithium toxicity, should be. It is also a good idea to discuss common side-effects such as nausea for selective serotonin reuptake inhibitors (SSRIs). For the anti-dementia drugs, it is important to point out that clinical benefit may be limited, and to emphasise that treatments are not a cure. Even though it may be problematic in a time-pressured clinical setting, a record should be made of such discussions; good documentation promotes better clinical care. Patient information leaflets are now provided in all treatment packs given to patients (Reference CollierCollier, 1998), but clinicians should not rely solely on these for the imparting of clinical information. Not all patients will receive such leaflets, especially in settings where original packs are not used. Leaflets vary in their readability, provide information only about licensed indications and cannot substitute for proper discussion with the prescribing clinician.
Assent (incapacitated patients who comply with treatment)
Compliant elderly patients without capacity are perhaps the most vulnerable group for whom we care. Most patients with dementia will take whatever treatment is offered to them, irrespective of its purpose or anticipated side-effects. With no proper method of consent, and little involvement of relatives or advocates, these patients are truly vulnerable. In his judgment on the Bournewood case ( R v. Bournewood Community and Mental Health NHS Trust, 1998), Lord Steyn emphasised his grave disquiet at the lack of safeguards for such patients. The ‘Bournewood Gap’ as it has been described, might be better named a chasm, as it contains many thousands of elderly patients who receive treatments with little discussion, no valid consent and no safeguards. Although the use of advocacy was recommended by the Department of Health in the wake of the Bournewood judgment, there have been no new resources made available for this and we do not believe that much has improved since the judgement. It is to this group of patients that the OBRA guidelines primarily apply. Those patients do at least have the advantage that they can receive treatments that will be of benefit to them and safeguard mechanisms must not be so cumbersome as to prevent access to care. Indeed, such an imperative was discussed by Lord Goff in the Bournewood judgment.
Dissent (incapacitated patients who do not comply)
When patients do not comply with treatment it is always appropriate to be sure that the treatment envisaged is necessary. One of the seminal cases of non-compliance (Re C, 1994) was based on a medical judgement that amputation was required to save a life. In fact the patient survived without amputation. It is therefore always right that treatments should be critically reviewed and, if they are still felt to be needed, then all attempts to give treatment in the usual way should be made. When this fails, however, a doctor's duty of care (Re F: Mental Patient: Sterilization, 1990) means that the patient must not simply be left untreated.
There is evidence (Reference Treloar, Beats and PhilpotTreloar et al, 2000) that most settings in which the elderly with dementia are cared for resort to the covert use of medication at times. The most common method of administration is to mix medication with drinks or foodstuffs. Although a last resort, ethical analysis (Reference Treloar, Philpot and BeatsTreloar et al, 2001) suggests that such actions are legitimate in exceptional circumstances. Where the Mental Health Act does not apply, then common law must be used. Again, it is important to balance ease of access to good clinical care against restrictions aimed at preventing abuse. In essence, it appears that if medication is given covertly, then it should be discussed between the doctor, nurse, pharmacist and relative or advocate, and recorded, so that legal redress is possible. The opportunity for legal redress is, of course, a key element of the UK Human Rights Act 1998.
Refusal (capacitated patients who do not comply)
Capacitated patients may not be treated without their consent. Refusal to consent may be for any reason or no reason and is not dependent on that refusal being a good idea (Sidaway v Board of Governors of the Bethlem Royal Hospital and the Maudsley Hospital, 1985). None the less, it is critically important that the clinician discusses treatment options with the patient and ensures that the patient's decision is properly informed and based on adequate knowledge and understanding. Patients who have made an advance directive that applies to the situation in question and that does not cause unintended harm can also guide decisions about their future care (for a review of the limitations of advance directives see Reference TreloarTreloar, 1999).
Detained patients who refuse treatments
The Mental Health Act 1983 for England and Wales states that detained patients may be capacitated to consent to treatment. Although it is suggested that all patients detained under the Mental Health Act must be incapacitated in some way, capacity is situation-specific (British Medical Association & Law Society, 1995) and so it may be possible to be detained for treatment and yet still consent to a core component of that treatment. The Mental Health Act exists to enable the provision of treatment to those who need it while providing safeguards against the inappropriate use of medication. Although the Bournewood judgment held that treatment should be given under common law where the Mental Health Act does not apply, it was conversely quite clear that where the Act applies, it must be used. It is thus clear that the use of Section 3 along with Sections 58 and 62 should be considered whenever a patient is detained under the Mental Health Act.
Practical issues
For a drug to have a therapeutic effect it must be ingested, absorbed, distributed, metabolised and excreted. In the elderly, there are a number of practical difficulties in achieving this. These include compliance, actual administration and polypharmacy.
Compliance
Most patients of all ages who decide to take a treatment will at times forget to take it. Such non-compliance is not refusal, merely an anomaly that can be reduced by various methods. The most effective way of facilitating compliance is to make drug regimes manageable. Once- or twice-daily administration with drugs that do not interact with food is preferred, especially where elderly people live independently and require daily supervision of their medication. The use of slow-release preparations may help, although these can lead to problems: if a repeat prescription omits the slow-release part of the order, then patients may suffer side-effects from excess peak blood levels of drug, and insufficient 24-hour cover.
The widespread use of compliance aids (see Box 2) seeks to improve uptake in this group, although objective evidence of benefit is sparse. Compliance aids can cause difficulties: patients can find them difficult to open or use them upside down and not all medicines are stable in such devices. It is important to choose a device appropriate to the patients needs, assess their ability to use it and make appropriate arrangements in advance for the device to be refilled. A compliance aid can be useful in helping a carer to manage medication. Home care workers or relatives who are able to visit once or more daily and prompt the taking of medication are invaluable. As well as ensuring compliance among those with cognitive impairment, such visits may hugely enhance the quality of daily life for individual patients. Given the problems caused by irregular compliance, any strategy that may help should be tried.
Box 2. Compliance strategies
-
• Simple medication regimens
-
• Appropriate presentation (e.g. syrups)
-
• Administration aids (e.g. spacer devices and dosette boxes)
-
• Medication reminder charts
-
• Supportive carers
-
• Appropriate information for patients and carers regarding the purpose and likely side-effects of all prescribed medication
Repeat prescription systems in general practice surgeries must incorporate recall systems so that all treatment can be reviewed on a regular basis (at least 6-monthly).
Actual administration
Tablet timing may be important, for example, the regimens used to treat Parkinson's disease and diabetes. There continues to be a real problem with the administration of medicines at mealtimes. Although many medicines do not interact with food, some do. The use of standard labels as defined in the British National Formulary (BNF; British Medical Association & Royal Pharmaceutical Society of Great Britain, 2001) helps to reduce this problem, but this advice does not account for some of the less usual administration routes employed by carers.
Crushing tablets can be a particular problem. Delayed release mechanisms may be critically affected (for example, aminophylline and nifedipine tablets), and dissolving a medicine in, for example, orange juice, may destroy the active ingredient if it is unstable in acid. All such techniques must therefore be discussed in advance with a pharmacist.
Polypharmacy
Polypharmacy, too, is a significant problem, requiring regular critical appraisal of the indications for treatment and of potential drug interactions. We have seen recent examples of the co-prescription of anti-dementia drugs with anticholinergic tricyclic antidepressants, as well as a devastating lowering of blood pressure produced by the co-prescription of a tricyclic, a beta-blocker and a alpha-blocking anti-prostate drug.
Administering medications in controversial circumstances
Attempts to provide good-quality care in unusual and difficult circumstances will inevitably result in some potentially controversial treatment decisions. While the need to provide good care to those who cannot choose is an inescapable duty, it is mandatory that doctors and nurses recognise the nature of what they are doing and discuss decisions thoroughly with colleagues and patients or advocates in an open and balanced way. Decisions and discussions should be recorded and open to criticism and inspection. The failure of the Mental Health Act 1983 to apply in so many situations means that treatment must be enforced under common law. This does not mean that it can be done in a haphazard and sloppy way. All professionals must ensure proper consultation and recording of their decisions and actions.
In time it may be that incapacity legislation will provide some answers, but if safeguards are too cumbersome, then access to care may be inadvertently denied. There is a fine balance between ensuring good access to high-quality treatment for patients who, by virtue of their illness, cannot choose and having in place safeguards to prevent the abuse of patients by overenthusiastic treatment. Perversely, the creation of Health Care Continuing Powers of Attorney (The Lord High Chancellor, 1999) may make it easier rather than harder to impose controversial treatments on those who resist care.
Conclusion
Medicines are useful in the elderly but should be used where specific indications for treatment exist and with appropriate monitoring. Polypharmacy should be avoided wherever possible and simple administration regimens used. Practical help with adhering to prescribed medication can be invaluable. Those patients who are unable to choose have a right to receive the good care that they cannot choose for themselves. Health systems must be able to respond to these needs and clinicians must strive to ensure that abusive forms of treatment are avoided, while patients do not miss out on good and appropriate care. Safeguards, while important, must not be so restrictive as to prevent access to such good care.
Multiple choice questions
-
1. In the elderly:
-
a reduced capacity to metabolise and excrete drug makes drug -induced toxicity more likely.
-
b antidepressants are effective in treating depression in the presence of chronic physical illness.
-
c aggression may be secondary to depressive illness and may respond to antidepressants.
-
d lithium is not effective in augmenting antidepressant response.
-
e the use of cholinesterase inhibitors is not supported by NICE owing to an insufficient evidence base.
-
-
2. Regarding antipsychotic medication for dementia in elderly people:
-
a the evidence base for its use has been rigorously tested
-
b physical frailty affects the ability to tolerate antipsychotic medication
-
c adherence to OBRA guidelines should increase the use of antipsychotics in nursing homes
-
d continued monitoring of response following initial prescription is advised.
-
e risperidone and olanzapine have been shown to have some benefit in controlling behavioural disturbance.
-
-
3. Regarding deciding whether or not patients may be treated:
-
a any treatment of patients who have not consented to medication constitutes assault
-
b doctors have a duty to give good-quality care to those who cannot consent to treatment by virtue of mental incapacity
-
c all possible side-effects must be explained to the patient before informed consent can be given
-
d patient information leaflets fulfil all the requirements for information on prescribed medication.
-
e Incapacitated patients who do not resist or question their treatment, require no special consideration or advocacy.
-
-
4. Regarding compliance:
-
a compliance may be facilitated by simplifying medication regimens
-
b a compliance aid is useful in all cases of poor compliance
-
c some medicines are not stable in compliance aids
-
d non-compliance is a common cause of treatment failure
-
e any tablets or capsules can be crushed and administered with a drink.
-
-
5. When incapacitated patients do not comply with medication:
-
a the Mental Health Act always applies
-
b treatment plans must be critically reviewed and all attempts to give medication in the usual way made
-
c if persuasion fails, patients must be left untreated, regardless of the consequences
-
d as a last resort, medication may be administered covertly
-
e covert administration does not require multi-disciplinary discussion or specific records to be made.
-
MCQ answers
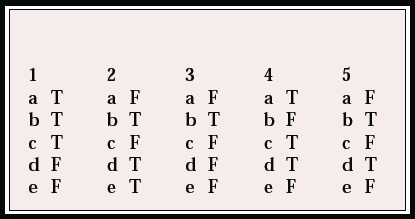
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | F | a | F | a | T | a | F |
| b | T | b | T | b | T | b | F | b | T |
| c | T | c | F | c | F | c | T | c | F |
| d | F | d | T | d | F | d | T | d | T |
| e | F | e | T | e | F | e | F | e | F |
Table 1 Levels of agreement to treatment

| Consent | Agreement to accept treatment based on full information and adequate mental capacity |
| Assent | Acceptance of treatment that is not based on mental capacity |
| Dissent | Rejection of treatment of someone who has insufficient mental capacity to make such a choice |
| Refusal | Refusal of treatment based on full information and mental capacity |






eLetters
No eLetters have been published for this article.