Comprehensive health care services respond effectively to the needs of their patients not just in terms of treatment of health problems but also by addressing overall well-being by understanding, informing, involving, counselling and respecting the individual. By contrast, the history of health care for people with learning disabilities has been characterised by a lack of communication and poor understanding of their ordinary and special needs. There have been many barriers to access to health services that most members of the population take for granted. In addition, people with learning disabilities have many special health care needs that also have to be addressed. Therefore, person-centred services must be aware of the wide range of needs to which they must be able to respond while treating each person as an individual (see Box 1).
Box 1 Requirements for meeting the health care needs of people with learning disabilities
Equal access to all health services
Sufficient support to enable access to these services
Disability awareness as an integral part of staff training
Access to specialist health services for those with more complex and special needs
Community learning disability teams delivering and/or coordinating these services by working closely with primary health care services (health facilitation role)
Systems for individualised health care planning (such as Health Action Plans)
Partnerships between agencies, service users and carers, so that social, educational and health care needs are addressed in a coordinated way
Health care needs of people with learning disabilities
Ordinary health care needs
People with learning disabilities have ordinary health care needs similar to those of the rest of the population and the same rights of access to health care services (Reference LindseyLindsey, 1998). In the UK this involves access to health promotion, primary health care services, community health services and specialist health services as required. However, barriers to access arise from two main sources: the learning and communication difficulties of people with learning disabilities and the knowledge, attitudes and beliefs of carers, clinicians and managers of services. This situation has five main consequences, which are described below and summarised in Table 1.
Table 1 Barriers to the access of people with learning disabilities to health care services

| Barrier | Addressed by |
|---|---|
| The learning and communication difficulties of people with learning disabilities | Providing opportunities for service users to learn about health issues and to self-advocate Sensitive and flexible services with good communication skills |
| Lack of carer and professional awareness of the health needs of people with learning disabilities | Provision of suitable training for carers and health professionals |
| Discriminatory attitudes of carers or professionals | Disability awareness training Explicit organisational policies and codes of conduct |
| Physical barriers and inflexible administrative and care procedures | Involvement of service users and carers in planning Implementation of adaptations and changes Awareness of consent issues |
| Poor awareness of the other factors that can create disadvantage | Sensitivity to social, ethnic, cultural and economic needs of individuals |
Learning and communication difficulties
The individual with a learning disability may not understand the significance of a healthy lifestyle and the importance of health screening or recognise symptoms or signs of ill health. This can lead to failure to cooperate with carers in following a healthy lifestyle or in participating in health screening activities. When the person has ill health he or she may not draw this to the attention of others in the usual ways because of failure to realise the significance of symptoms or because of communication difficulties.
There are several ways of addressing this. First, services should ensure that people with learning disabilities have opportunities to learn about their health and that information is provided in ways that take communication difficulties into account. Picture-based books are available aimed at people with learning difficulties and their carers (e.g. Reference Hollins and DownerHollins & Downer, 2000; Reference Hollins and PerezHollins & Perez, 2000). Some community learning disability teams have found that well-woman and well-man groups have been successful in raising awareness of health issues.
Second, people with severe learning and communication difficulties may not be able to express discomfort or pain in usual ways. Carers must be aware of this and sensitive to changes in behaviour or well-being that indicate pain, illness or unhappiness.
Third, regular health (including dental and sensory) checks are needed to detect problems by symptom screening and physical examination (Reference Martin, Roy and WellsMartin et al, 1996). It is important to screen for mental as well as physical health problems; the Psychiatric Assessment Schedule for Adults with Developmental Disabilities (PAS–ADD) can be used for this (Hester Adrian Research Centre, 1996).
Poor carer and professional awarenness
Carers may not be aware of the importance of a healthy lifestyle and may misinterpret changes that indicate health problems. Inexperienced carers and professionals may assume that unusual or changed behavioural patterns are a manifestation of the learning disability rather than caused by discomfort or a mental health problem. Many family and paid carers lack knowledge about health issues, and training opportunities should be available to them. All health professionals need ongoing training to recognise and respond appropriately to the ordinary and special needs of people with learning disabilities.
Discrimination
Carers and professionals may undervalue people with learning disabilities and may not consider their health needs to be important. In extreme cases this has led to neglect, ill treatment, euthanasia or discrimination in the UK and to the practice of eugenics to the point of homicide elsewhere, particularly in Nazi Germany (Reference WealeWeale, 2001). Most often, however, it leads to more subtle discrimination and neglect of health care needs. This can be addressed in various ways.
First, the training of carers and professionals should include examination of their own and society's attitudes and beliefs and the ways that these shape services and service responses. Positive changes in attitudes and beliefs can most readily be achieved by direct contact and discussion with self-advocates and with family carers.
Second, organisations should have explicit policies about disability discrimination based on discrimination legislation and also ‘whistle-blowing’ policies; involvement and consultation with service users and carers should be a priority. Professional organisations should make these explicit in their codes of conduct.
Physical and administrative barriers
Physical barriers to access may be present and these include not only unsuitable buildings but also unsuitable signs, support, information about appointments, timing of appointments and information about treatment. Sometimes people with learning disabilities need careful preparation for hospital appointments or admissions and opportunities to familiarise themselves with places and procedures. Again, books addressing such issues are available (e.g. Reference Hollins, Avis and ChevertonHollins et al, 1998a , Reference Hollins, Bernal and Gregory b ). Issues of consent also need to be understood and addressed in order to avoid this becoming another barrier to access.
Services should be aware of the potential needs of people with learning disabilities by listening to them and to specialist learning disability services and should then undertake the adaptations that are needed. Flexible services are necessary in order to accommodate the particular needs of people with learning disabilities.
Social factors
Finally, barriers to access will be greater if services are insensitive to the social, ethnic, cultural and economic backgrounds of individuals and their families: these should be both recognised and understood (Reference Baxter, Poonia and WardBaxter et al, 1990).
Special health care needs
In addition to ordinary health care needs, people with learning disabilities may have much greater special health care needs than the general population (Table 2). They have high rates of general health problems, mental health problems, epilepsy, sensory impairment, cerebral palsy and other physical disabilities. They need assistance with personal growth and development, and many syndromes and genetic and chromosomal causes of learning disabilities carry particular health risks.
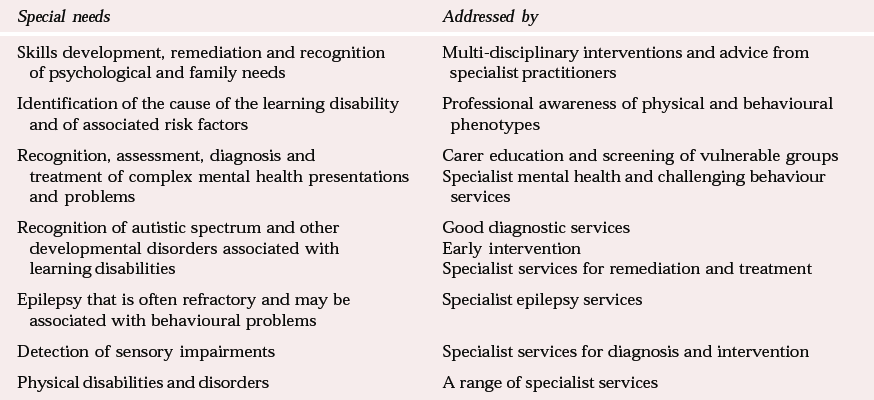
Table 2 Special health care needs that frequently arise for people with learning disabilities
| Special needs | Addressed by |
|---|---|
| Skills development, remediation and recognition of psychological and family needs | Multi-disciplinary interventions and advice from specialist practitioners |
| Identification of the cause of the learning disability and of associated risk factors | Professional awareness of physical and behavioural phenotypes |
| Recognition, assessment, diagnosis and treatment of complex mental health presentations and problems | Carer education and screening of vulnerable groups Specialist mental health and challenging behaviour services |
| Recognition of autistic spectrum and other developmental disorders associated with learning disabilities | Good diagnostic services Early intervention Specialist services for remediation and treatment |
| Epilepsy that is often refractory and may be associated with behavioural problems | Specialist epilepsy services |
| Detection of sensory impairments | Specialist services for diagnosis and intervention |
| Physical disabilities and disorders | A range of specialist services |
To address this, health professionals can work alongside colleagues in education and social services to advise on the development of skills and approaches to overcoming disabilities. Physiotherapists have an important role in assisting the development of gross motor skills, occupational therapists in the development of fine motor skills and coordination, and speech and language therapists in communication skills. Mental health professionals can advise on the promotion of good mental health through the development of emotional security, self-confidence and self-esteem and through bonding to primary caregivers.
Family members should not be overlooked: they are at risk of mental health problems as they come to terms with the child's disability, and they also have to cope with the practical aspects of care and skills development.
The cause of the disability
If possible, the cause of the learning disability should be found in order to identify the particular physical or mental health risks associated with that condition. For example people with Down's syndrome are at greater risk of congenital heart disease, visual and hearing impairments, thyroid disorders and pre-senile dementia, and those with tuberous sclerosis are at risk of epilepsy, rhabdomyomas, renal disorders, autistic spectrum disorders and cerebral tumours of low-grade malignancy. These physical and behavioural phenotypes are becoming increasingly recognised as a source of some health problems and professionals should be aware of their potential significance (Reference Dykens, Hodapp and BourasDykens & Hodapp, 1999).
Mental health needs
The assessment, diagnosis and treatment of mental health problems in people with learning disabilities requires a good understanding of the genetic, neurological and social predisposition to mental illness that is likely to account for the much higher rate reported in this population. In addition, it is necessary to know about the developmental disorders, including autistic spectrum and attention-deficit hyperactivity disorders, that frequently coexist with a learning disability. Mental disorders may present atypically and people with diagnosable mental illness tend to be more able, usually with only a mild learning disability. It is extremely difficult to diagnose a mental illness in a person with a severe learning disability because the diagnostic criteria require that the person has the ability to report subjective symptoms. It is very likely that mental health problems are underreported in people with learning disabilities (Reference Patel, Goldberg and MossPatel et al, 1993).
Targeted services
The justification for comprehensive and extensive mental health services geared to people with learning disabilities is broad-based. Estimates vary, but 10–39% of adults with learning disabilities have mental health needs arising from additionally diagnosed psychiatric and behavioural disorders (Reference Borthwick-DuffyBorthwick-Duffy, 1994; Reference Bernal and HollinsBernal & Hollins, 1995). The rate of specific disorders such as schizophrenia has also been shown to be greater than in the general population (Reference Doody, Johnstone and SandersonDoody et al, 1998; Reference Morgan, Ahmed and KerrMorgan et al, 2000). There is some evidence that in community settings the rate of psychiatric disorders such as anxiety and depression is higher than it was in the institutions (Reference JacobsenJacobsen, 1982; Reference DayDay, 1985). This may be a reflection of the stress of coping with day-to-day living, particularly if there is inadequate or unskilled support and insufficient attention to lifestyle issues.
Challenging behaviour is often accompanied by carer stress and carer reactions that reinforce the abnormal behaviour pattern over time (Reference McGill, Clare and MurphyMcGill et al, 1996). The uncertain status of challenging behaviour makes it difficult to achieve a consensus on the rate of mental health problems in people with learning disabilities. About 6% of people with learning disabilities show behaviours that can be regarded as seriously challenging (Reference Kiernan, Qureshi and KiernanKiernan & Qureshi 1993). These problems are often long-term behavioural patterns rather than time-limited illnesses. However, there have been suggestions that mental illness may underpin at least some of these behaviours (Reference Allen and KerrAllen & Kerr, 1994).
People with challenging behaviour in the absence of diagnosed mental illness are most likely to have communication difficulties, often as part of an autistic spectrum disorder, severe-to-moderate learning disabilities and an inappropriate care environment. Modern behavioural approaches can result in significant short- and medium-term reductions in the severity of the behaviour (Reference Allen, Felce and BourasAllen & Felce, 1999), and psychotropic medication may be effective when there is an underlying psychiatric or developmental disorder.
Mental health problems occur at all ages. Children and adolescents with learning disabilities have a much higher rate of mental health problems compared to other children. It has been estimated that 50% of them are likely to need special services at some point in their childhood (Royal College of Psychiatrists, 1998; Reference BernardBernard, 1999). Elderly people with learning disabilities have a higher rate of mental disorder compared to other elderly people and to younger adults with a learning disability (Reference CooperCooper, 1997). Some of this is due to the high prevalence of dementia (Reference Patel, Goldberg and MossPatel et al, 1993).
Offending behaviours are often included under the category of challenging behaviours and some are secondary to psychiatric disorder. People with learning disabilities are overrepresented in the criminal justice system and are most likely to commit crimes against other people (Reference HayesHayes, 1996).
Developmental disorders
Many people with learning disabilities have autistic spectrum (Reference Gillberg and BourasGillberg, 1999), hyperactivity (Reference Fox and WadeFox & Wade, 1998) and other developmental disorders, even if not formally recognised. Therefore it is important that all services for this population have the skills to recognise and make adequate local provision for them.
This involves many factors. First, there must be good diagnostic services, to detect in early childhood any developmental disorder additional to a learning disability. The diagnosis depends on a full and competent assessment by a child and adolescent psychiatric, paediatric or learning disability service that specialises in this area. This will include a detailed developmental history as well as direct observation of the child and family.
Second, treatment is important. There is some evidence that early intervention for children with autistic spectrum disorders may result in significant improvements in skills and behaviour (Reference Lovaas, Calouri, Jada and GillbergLovaas et al, 1989; Reference Schopler and GillbergSchopler, 1989; Reference SiegelSiegel, 1996). Attention-deficit and hyperactivity disorders may benefit from the use of psychostimulant medication, which requires specialist assessment and monitoring. Communication disorders are often associated with challenging behaviour. Speech and language disorders require access to skilled speech and language therapy and carers and teachers who can apply such specialist advice in day-to-day care. Coordination disorders (dyspraxia) require skilled occupational therapy input. Tic disorders may improve with the use of medication but are often undiagnosed.
Epilepsy
Access to specialist services for epilepsy is important because 13–24% of people with a learning disability are affected by the disorder (Reference Jenkins and BrownJenkins & Brown, 1992; Reference DebDeb, 2000). They are also at a much greater risk of more complex and refractory seizure disorders (Reference Deb and JoyceDeb & Joyce, 1999).
Modern diagnosis includes referral to a specialist with expertise in epilepsy for detailed examination and investigation, followed by effective monitoring of seizure control and medication. Expert knowledge is required of the many anti-epileptic drugs available and of the indications and risks associated with their use.
Sensory impairments
Sensory impairments must be detected and remedied to minimise the consequent disability, and a specialised and sensitive approach is usually needed. About 30% of people with learning disabilities have a significant sight impairment and 40% have significant hearing problems. Sometimes both are present, resulting in a complex disability. The prevalence of these problems increases with age, and professionals should be aware of this as a possible explanation for changes in behaviour and awareness. Sensory disabilities are often associated with challenging behaviour. There is a very high rate of underdetection of sensory impairments, most of which can be treated.
Physical disabilities
Up to 30% of people with learning disabilities also have physical disabilities, most often owing to cerebral palsy, and they need input from a range of specialist services. A large number of serious health problems are secondary to these physical disabilities (e.g. gastro-oesophageal reflux, aspiration pneumonias, risk of choking, joint pains and muscle spasms). The chronic discomfort caused by such problems may present as a behavioural problem and this can lead to misdiagnosis. Pain management is particularly important for people who cannot easily communicate their discomfort.
Some people with learning disabilities have very complex health needs because of multiple disabilities and some are totally dependent on others for their care throughout their lives. They may need a wide range of equipment and adaptations.
Children with profound disabilities are living longer, often with life-maintaining technologies that require a high level of skilled care. Some serious conditions are life-threatening and palliative care is required.
Changes in health care services
Previous patterns of service delivery
It is evident from the range of needs that no single service can effectively meet them all. People with learning disabilities are a heterogeneous group in terms of their age, degree of disability and associated health problems.
In the past, large hospitals were established mainly for care and segregation rather than with a therapeutic purpose, and the staff attempted to address all the physical and mental health needs of their long-stay patients. As these hospitals became overcrowded, care standards became poor and the problems of institutionalisation were increasingly recognised. As a result, a policy of resettlement from hospital to the community has been in operation in the UK for over 30 years but is not yet complete. Pilot projects in the 1980s showed that even people with high health care needs could be cared for by community services if the various agencies worked together effectively.
As the hospitals closed, the professional staff shifted their specialist work to community settings and specialist community learning disability teams have become the norm in most areas. The knowledge and skill base has steadily improved so that more effective interventions are now available to help people with learning disabilities and their families and carers (Reference Emerson, Forrest and CambridgeEmerson et al, 1996).
However, the majority of those with learning disabilities have always lived in the community and have had to compete with the general population for health care. There is evidence that the health needs of these people have for many years gone underrecognised or undertreated in the ordinary primary, community and hospital health services. This is less likely to happen if specialist services are involved in drawing attention to the barriers to access and in meeting the special needs outlined above.
Present and future trends
Patterns of health service provision for people with learning disabilities are shifting (Box 2). The residual hospital provision is mainly for specialist psychiatric assessment and treatment and also for some continuing care of people with severe and complex health problems. ‘Social care’ is no longer the responsibility of health services and the emphasis is much less on the disability and much more on support to the individual to build on strengths and respond to needs. There is a risk that this change of emphasis could lead to neglect of health care needs, and there has been a recent resurgence of interest and concern in this area (Reference LindseyLindsey, 1998). The difficulty in separating health from social care, particularly for people with long-term and complex needs, has led to an increasing emphasis on partnerships between organisations. Also, there has been an increasing awareness that the problems of institutionalisation and poor-quality care can arise in any care setting and that organisations that commission, provide and monitor services must work together to ensure that service delivery is optimal in terms of quality and effectiveness.
Box 2 Trends in the pattern of health service provision for people with learning disabilities
Shift from institutional to personalised community care, leading to greater use of community health services and reduction of the barriers to access
Increasing service-user and carer consultation and involvement in improving services
Changes in health needs as more children with complex disabilities live into adulthood and most people with learning disabilities reach old age
Identification of physical and behavioural phenotypes
Development of specialist out-patient and in-patient mental health services for people with learning disabilities with complex needs
Improved understanding of developmental disorders and specialist interventions for these
Increasing awareness of the need to develop mental health services for children and adolescents with learning disabilities and emphasis on early intervention
Increasing awareness of the needs of older people with learning disabilities
Improved understanding of seizure disorders and new treatment approaches, leading to higher expectations of services
As a result of international and national changes in services for people with learning disabilities and changes in the attitudes of society towards them, there have been major policy reviews at government level (Scottish Executive, 2000; Department of Health, 2001a ), with considerable implications for future provision of health care services.
Elements of comprehensive health care services
The two main elements of service provision for people with learning disabilities are the enhancement of access to mainstream health services and the provision of specialist services only when the needs of individuals cannot be met by ordinary services. In view of the complex and long-term needs of many individuals, services must also ensure that care is effectively coordinated and planned.
Access to mainstream services
Health promotion services should work with service users, carers and the agencies involved to ensure that health promotion is accessible to people of all ages with learning disabilities and geared to their needs. They also have a role in educating carers and professionals, who can then promote the health of this population. It is important to promote mental as well as physical health, but this is often neglected.
Screening services should understand the importance of including people with learning disabilities and helping them to cooperate with screening. Guidance on accessing breast and cervical screening services has been produced by the National Cancer Screening Programmes (National Health Service, 2001a,b).
Primary health care services not only provide care and treatment but also act as a gateway to specialist services. They therefore play a key role and need to be well-informed about the needs of people with learning disabilities (Reference Lindsey and RussellLindsey & Russell, 1999). A Government White Paper for England (Department of Health, 2001a ) states that by June 2004 all people with learning disabilities should be registered with a general practitioner (GP) and that all general practices will have identified all people with a learning disability registered with the practice. Staff from community learning disability teams will take on the role of health facilitators to support people with learning disabilities in gaining access to the help that they need from primary care and other NHS services. The role of health facilitators should embrace mental as well as physical needs. Each individual with a learning disability will also be offered a Health Action Plan, and responsibility for completion and subsequent updating of this will rest with the health facilitator in partnership with primary care nurses and GPs. The effectiveness of this novel approach to improving the health of people with learning disabilities has yet to be evaluated.
There are many other community health services to which people with learning disabilities will need help to gain access; these include dental, optician, continence promotion, nutrition, audiology, pharmaceutical, sexual health and chiropody services.
Access to general hospital services continues to cause concern for many families because these services often lack the sensitivity and flexibility required to respond to special needs. People with learning disabilities and their carers often complain that the attitudes of staff are discriminatory. Nevertheless, they also report a steady improvement over the years, with greater equity of access and treatment. The same standards of care available to the general population, for example those described in the recent National Service Frameworks for England (Department of Health, 1999, 2001b ) apply equally to people with learning disabilities.
Access to specialist health services
Children
Specialist health care for children with learning disabilities are provided by child health services, which are now developing a greater community focus. Community paediatricians frequently have a long-term involvement with children with learning disabilities and their families; for children with life-threatening illnesses community nurses and children's hospices also play an important role. The holistic approach and the continuity of care provided by such services are highly valued by most families. Some services also employ psychologists and address the mental health needs of children and their families; others work closely with child and adolescent psychiatric services or with specialist learning disability services that cater for children.
There is now widespread recognition of the importance of sensitive communication and counselling for families from the time of diagnosis of a disability. Unfortunately in many areas there are inadequate or no services for children and adolescents with more complex and severe mental health problems. The probable importance of early, skilled intervention to reduce challenging behaviour and other mental health problems has been recognised relatively recently and the lack of services is such that the potential long-term impact of such an approach has not yet been evaluated (Reference EmersonEmerson, 1996).
Adults
In contrast to the situtation for children, most, but not all, areas of the UK have specialist mental health services for adults with learning disability (Royal College of Psychiatrists, 1996/7). However, there are no specialist physical health services equivalent to those for children that can address the more complex needs associated with chronic physical disabilities and health problems. This service deficit is becoming even more evident now that many children with severe health problems requiring interventions (such as gastrostomy) are surviving into adult life. This is a historical anomaly that arose because the medical staff in the large learning disability hospitals aligned themselves with the speciality of psychiatry in the 1960s and 1970s.
Community learning disability teams often employ physiotherapists to work with adults, and learning disability nurses have a more holistic approach. However, medical support is often lacking unless the learning disability psychiatrist has an interest in this area. In other countries, notably The Netherlands, there are very good specialist health services for adults with learning disabilities who have physical health problems, but there is a lack of specialist psychiatric services.
Epilepsy
Access to epilepsy services is also very variable, and providers of these services may be paediatricians, neurologists or learning disability psychiatrists. Most psychiatrists and other health professionals working in specialist learning disability services have a good understanding of the issues related to epilepsy and of seizure and medication monitoring and management. Many learning disability and neurology services now have epilepsy nurse specialists, who have an important role in patient education, support and monitoring. There are also tertiary neuropsychiatric services.
Old age services
As people with learning disabilities living in the community are increasingly surviving into old age, the need for specialist services for the elderly is emerging. Learning disability services and old age services must work together to address this problem.
Mainstream v. specialist care
In the UK, the existence of specialist mental health services for people with learning disabilities is the envy of psychiatrists in many other countries. It has resulted in the development of very effective services that can respond to the complex mental health needs outlined above (Reference LindseyLindsey, 2000). However, it has also been criticised because it is seen as discriminatory and leading to the exclusion of people with learning disabilities from mainstream mental health services. It is clearly unacceptable for people with learning disabilities to be excluded from mental health services from which they could benefit. On the other hand, many mental health professionals report that inclusion without addressing special needs may disadvantage the individual (Reference Gravestock and BourasGravestock & Bouras, 1996). In reality, overstretched mental health workers in mainstream care have neither the time nor the willingness to expand their skills and knowledge base; furthermore, they are not motivated to do so when they are aware that specialist services do exist that are generally better equipped with skills, although often even more poorly resourced.
For some patients with very special needs, such as those with forensic problems, the situtation is even more acute, as there is a national shortage of suitable in-patient and out-patient services. In each area, local in-patient services offering specialist psychiatric assessment and treatment are essential but the number of beds required depends on the resources and effectiveness of the community services (Reference LindseyLindsey, 1998). The Scottish Executive's (2000) strategic review of services estimates that four treatment and assessment beds are required for every 100 000 head of population, in addition to appropriate community services to avoid in-patient admissions. Specialist mental health services should be able to address the needs of patients of all ages with a wide range of mental health problems, and this requires an extensive knowledge and skills base. It should also be possible for those services to help people with learning disabilities to gain access to mainstream mental health services if these can better meet their needs.
Equal access to health care
It is essential that sufficient high-quality multi-disciplinary specialist services are available, and the locally based community learning disability team is a key component of these. However, the goals of such teams are being changed to give greater emphasis to their role in providing specialist expertise to enhance the competence of local services. This includes direct support, facilitation, teaching and service development. It also requires other services to work collaboratively in partnerships with specialist services. In addition, the teams must have access to the necessary range of in-patient, assertive outreach and other very specialised services.
The training of health professionals to work with people with learning disabilities and to understand their needs is crucial to the success of a policy of equity of access and this must be an ongoing process.
The planning and coordination of health care is increasingly the responsibility of primary health care services, with the support of specialist learning disability services. The introduction of Health Action Plans as part of the personal planning process should help in the provision of the necessary health services and the development of those that are not currently available. The health facilitator role will be critical in this.
Organisations involved in the commissioning and provision of health and social care must support these changes at every level if they are to be successful.
Multiple choice questions
-
1. People with learning disabilities:
-
a need separate health care services
-
b often can learn to advocate for their own health
-
c are less aware of pain than other people
-
d often experience discrimination
-
e need regular health checks.
-
-
2. As regards the health of people with learning disabilities:
-
a they have a much higher rate of mental health problems than the general population
-
b about 50% show seriously challenging behaviour
-
c about 40% have a significant hearing loss
-
d they have the same rate of autistic disorders as the general population
-
e about 60% have epilepsy.
-
-
3. Large hospitals for people with learning disabilities in the UK:
-
a were all closed by 1999
-
b at one time cared for more people with learning disabilities than were left in the community
-
c provided better health care than was available in the community
-
d had professional staff who relocated to community teams
-
e provided an institutional model of care.
-
-
4. UK policy for health care services for people with learning disabilities includes:
-
a specialist mental health assessment and treatment beds
-
b placing all offenders in medium secure units
-
c access to child and adolescent mental health services
-
d exclusion from mainstream health services
-
e provision of special health promotion information and programmes.
-
-
5. In the future, community services for people with learning disabilities in the UK are likely to:
-
a ensure availability of a health professional who will facilitate access to health care services
-
b make training in disability awareness a fundamental part of professional training
-
c make special provision for health care for all
-
d provide Health Care Plans for all
-
e stop providing specialist learning disability health care services.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | F | a | T | a | T |
| b | T | b | F | b | F | b | F | b | T |
| c | F | c | T | c | F | c | T | c | F |
| d | T | d | F | d | T | d | F | d | T |
| e | T | e | F | e | T | e | T | e | F |







eLetters
No eLetters have been published for this article.