A classification system can benefit disturbed children enormously by bringing to bear a wealth of knowledge and experience. This can make all the difference between an inadequate consultation and a precise formulation of the nature and extent of a child's difficulties, their cause, the likely outcome and a realistic treatment plan. However, inappropriate application of a diagnostic label that has little validity could do more harm than good, and classification systems can be misused. This paper discusses, with examples, issues particular to childhood and adolescence that diagnostic systems need to address if they are to be useful. It considers different solutions applied by the two most widely used schemes, the International Classification of Diseases (ICD–10; World Heath Organization, 1992) and the Diagnostic and Statistical Manual of Mental Disorders (DSM–IV; American Psychiatric Association, 1994). Finally, the types of criteria used to validate categories are discussed.
Benefits of diagnosis
Making a correct diagnosis enables a body of knowledge to be applied. Take, for example, a boy who is persistently disobedient and aggressive. If no diagnosis is given, a counsellor might describe him as a child who gets into trouble a lot and look at the circumstances preceding his behaviour and its consequences. The treatment could be very variable, from changing the external circumstances that led to his outbursts to extended sessions with him to find out what makes him angry and help him to find new coping strategies.
Alternatively, a diagnosis of conduct disorder might be made if the behaviour had been fairly severe and lasted for over 6 months. It should be pointed out that the basis for applying the diagnostic label is only the child's behaviour, which must fit a certain pattern. In modern schemes, the defining criteria for nearly all psychiatric diagnoses are purely descriptive and phenomenological (Reference Dilling, Gelder, Lopez-Ibor and AndreasenDilling, 2000). No causal mechanisms are necessarily implied – that is for research to determine. This is a great step forward from old classification schemes that attributed untestable causes, for example saying a worried boy has ‘castration anxiety’. Those who believe that the phenomenological approach taken in psychiatric classification is inferior or less scientific than that found in physical medicine are mistaken – after all, epilepsy, hypertension and asthma are all diagnosed on the basis of observable phenomena with no assumptions of causality required.
To return to the boy described above, if a diagnosis of conduct disorder is applicable considerable knowledge accrues based on extensive research. Thus, we know that his long-term outlook without treatment is relatively poor: 40% of children with conduct disorder go on to be convicted of three offences by age 17 (Reference FarringtonFarrington, 1995), so saying that he will ‘grow out of it’ would be untrue. The prognosis is worse if onset was before he reached 4 years old, if the antisocial behaviour is frequent and widespread, if his IQ or reading age is low, if hyperactivity is present and if the parenting is hostile (Reference RobinsRobins, 1978). Further assessment should be made for the presence of specific reading retardation (dyslexia) and for hyperactivity, as each is present in about one-third of cases (Reference Rutter, Giller and HagellRutter et al, 1998). Although the cause of conduct disorder is multi-factorial and varies from case to case, it does include genetically determined temperamental predisposition and harsh parenting (Reference Rutter, Giller and HagellRutter et al, 1998). As regards evidence-based treatment, parent-training is known to be successful (Reference Scott, Spender and DoolanScott et al, 2001), stimulants are effective for coexistent hyperactivity (Reference Taylor, Rutter, Taylor and HersovTaylor, 1994) and remedial education can improve reading skills. Hence, the diagnostic label may help steer this individual's life course away from crime and social exclusion towards a fruitful existence with satisfying relationships (Reference Rutter, Giller and HagellRutter et al, 1998). Conversely, failure to apply a diagnosis could lead to several aspects of the boy's condition being missed and ineffective treatment being given, with a subsequent decline in the quality of his life.
Growth and development: a moving target
The restrictive specification of particular behaviours to fit them into a diagnostic category is often inappropriate, as a child is continually changing and growing. Therefore, sound knowledge is required of normal development and its limits. For example, repeated lining-up of toy cars may be normal in a 3-year-old, but abnormal in an 8-year-old. Once identified, it is helpful to decide if abnormalities are due to delay or to deviance from the usual pattern of development. The implications of each differ. For example, a child may exhibit a speech problem. If she produces only a handful of words, but in the appropriate context, she may suffer from expressive speech delay, which could be part of generally delayed development. If, on the other hand, the words are neologisms and pronouns are reversed, she may have autism, and the assessment would need to cover this: the diagnosis and outlook would be very different.
Because manifestations of behavioural tendencies change as a child develops, it is not always clear whether the same diagnosis should be applied across the age range. Thus, a highly aggressive toddler may throw himself screaming onto the floor in daily tantrums, whereas a highly aggressive teenager may assault old ladies and rob them. Do they suffer from the same disorder? ICD–10 holds that they do – both meet criteria for conduct disorder, which is defined in terms of antisocial behaviour that is excessive for the individual's age and that violates societal norms and the rights of others. DSM–IV, on the other hand, offers two separate diagnoses: oppositional–defiant disorder for the younger case and conduct disorder for the older. However, as both diagnoses have similar correlates and there is strong continuity from one to the other, the validity of the division is questionable (Reference Lahey, Applegate, Barkley, Widiger, Frances and PincusLahey et al, 1999). To complicate the picture further, neither scheme has a diagnosis to apply to adult antisocial behaviour, unless it is part of a personality disorder. This example illustrates how the two main diagnostic schemes can handle the issue of developmental change differently and how, in adults, both fail to include a group of people, thereby denying them potential benefits of treatment.
Should the same criteria be used for adults and children?
The extent to which adult criteria should be applied to children should be decided on the basis of good empirical data about the phenomenology and continuity of disorders. In the case of obsessive–compulsive disorder, the phenomenology is remarkably similar in both childhood and adulthood, so there is not a problem. However, for depression the picture is different. Currently, ICD–10 and DSM–IV have few emotional disorder categories specific to childhood, and they are mostly subtypes of anxiety. Mood disorders are diagnosed according to adult criteria, with the consequence that most surveys of depression find prevalence rates of zero under 8 years of age. Yet there are miserable children who cry frequently, say that they are unhappy, look sad and are withdrawn. However, they usually sleep and eat reasonably well and their mood fluctuates during the day, with spells when they sometimes appear more cheerful. Should they not be allowed a diagnosis? ICD–9 had a category for ‘disturbance of emotions specific to childhood and adolescence, with misery and unhappiness’, and Puura et al (1997) have shown that such children suffer social impairment. Follow-up studies of prepubertal children referred with this presentation showed a moderately increased risk of adult-type depression later on, whereas adolescents with depressive symptoms had a higher risk of adult depression (Reference Harrington, Fudge and RutterHarrington et al, 1990). Genetic studies show that symptoms of depression in prepubertal children are predominantly due to environmental influences, whereas after puberty genetic influences become more important (Reference Thapar and McGuffinThapar & McGuffin, 1994). This example shows that misery in younger children has some phenomenological features and external correlates in common with adult depression, but also some differences: this makes a comprehensive yet parsimonious classification system hard to achieve.
Dimensions or categories?
Using single words to denote categories is a widespread human practice. Where there is little overlap along a dimension, this is easy – we speak of brown or blue eyes, of men and women, of cats and dogs. Sometimes, even when traits are dimensional, we use categorical terms to describe one end of the dimension, as in ‘he's short and fat’. The majority of childhood problems arise from an excess of behaviours exhibited by many young people, such as aggression or anxiety. They are seldom due to qualitatively distinct phenomena of the kind more often seen in adult conditions, such as hearing voices or hanging oneself. Consequently, choosing a cut-off point to make a categorical entity from a dimensional construct is inevitably an arbitrary process, albeit informed by empirical criteria. This may be criticised as labelling the child unnecessarily. Psychiatrists in particular may be accused of ‘medicalising’ a child's difficulties by talking about disorders or diagnoses, whereas other professionals and parents may see them as understandable variations in child development and prefer to call them ‘emotional and behavioural difficulties’. However, the fact that the criteria for determining the dividing line between presence and absence of a category are arbitrary and do not correspond to a natural division does not invalidate the usefulness and validity of the category. As shown below, differences in mental ability are continuously distributed, yet categorising learning disability according to whether IQ is above or below 50 carries information about a whole host of characteristics, from brain pathology to life expectancy.
In practice, there is often not a huge difference between dimensions and categories, since the one can be converted to the other. Thus, the DSM–IV criteria for several disorders require counting up the number of symptoms to meet a cut-off. Even once a category is assigned, different degrees of severity may be named along a dimension: both DSM–IV and ICD–10 recognise mild, moderate or severe depression.
The social context
Nearly all children live within families. Often some or all of a child's problem may appear to lie in the structure or functioning of the family, rather than in the individual child, who may merely be reacting to the situation. For example, a child with poor weight gain and feeding difficulties may be being tantalised at mealtimes and having food withheld by his mother, who herself has anorexia nervosa. The question then arises whether the child has a diagnosis, or whether in fact the problem is the way he is being treated. Some professionals are concerned that to use a diagnostic label in this context is to locate the problem in the child and thus fail to recognise the causal role of the parent and treat the predicament accordingly. Although the blind application of a diagnosis could lead to this situation, it is important that the diagnosis be recognised as purely a description of a child's difficulties at the time, with no assumptions being made about causality. A diagnosis is no substitute for a full formulation, where cause should be addressed.
The formulation may reveal that the direction of effect runs the other way, from child to parent, with for example a boy's extreme hyperactivity leading his parents, in exasperation, to be critical and punitive. In support of this process, Schachar et al (1987) showed that giving methylphenidate to hyperactive children halved the criticism expressed towards them by their parents. Because of the central importance of the family in childhood in shaping a child's life and responses, it is helpful to categorise psychosocial stressors. They are addressed in the multi-axial ICD–10 system as described below.
Different sources of information can lead to different diagnoses
Traditionally, information is obtained from the parents and the child, and is then combined by the clinician on a case-by-case basis; rigid rules may lead to errors. Thus, if a parent says that a child has symptoms of conduct disorder but the child denies it, the parent is more likely to be right and the child may be covering up. However, if the parent says that the child is not depressed but a mental state examination of the child reveals otherwise, the parent may be ignorant of the child's true state. Such difficulties reduce the validity of interviews that use invariant combination rules. Further, the scientific attribution of cause can vary by informant. For example, in the Virginia Twin Study, conduct disorder was 69% heritable according to the information derived from interview with the mother, 36% using information from the child and only 27% using information from the father (Reference Eaves, Silberg and MeyerEaves et al, 1997). Furthermore, child behaviour differs markedly according to context. Thus, Rutter et al (1970) found that the correlation between questionnaire scores filled in by teachers and by parents was only 0.2–0.3. Direct observation, although expensive (it may involve a home or school visit), often provides the most reliable and valid information for assessment of disruptive disorders (Reference ScottScott, 1996).
To conclude, in child psychiatry information should be gathered from several informants using several methods (e.g. interview and observation) and combined in a clinically sensitive way.
Social impairment as a requirement of diagnosis
In general, ICD–10 and DSM–IV do not require impairment of social functioning to be present in order to make a diagnosis. But there are exceptions: in DSM–IV, for example, oppositional–defiant disorder does require social impairment. With many qualitatively distinct adult disorders, it makes sense to have no impairment criterion: a person experiencing the delusions and hallucinations characteristic of schizophrenia but able to go to work and form relationships while on neuroleptics still has schizophrenia. But should a child who says he is afraid of dogs and crosses to the other side of the street on seeing one, but otherwise functions well, be deemed to suffer from a specific phobia? If impairment criteria are not applied, very high rates of disorder are obtained in epidemiological surveys. This lacks credibility with the general public, who may then dismiss all psychiatric problems in children, and is unrealistic for clinicians and health planners, who would not see most of the identified individuals as cases needing treatment. For example, Bird et al (1990) in a large epidemiological survey found that using DSM–III criteria, 50% of children and adolescents had a diagnosis. However, when an impairment criterion was added, the figure came down to 18%. The recent Office of National Statistics survey of mental health in British children and adolescents used an impairment criterion and found an overall rate of disorder of 10% (Reference Meltzer, Gatward and GoodmanMeltzer et al, 2000). This would appear to be a much more realistic figure. However, it could be argued that social impairment is too constraining, as it would exclude, for example, an adolescent who is fairly depressed but able to function. The term ‘impact’ can be used to include subjective distress as well as social impairment, and it is gaining in popularity among many child psychiatrists (Reference Goodman and ScottGoodman & Scott, 1997).
Undiagnosed but impaired
Diagnostic systems must, above all, be practically useful. If they are over-inclusive, the risk is that there are too many categories with poor reliability and high overlap. If, on the other hand, they are too exclusive, the risk is that there will be many individuals suffering from problems not encompassed by the scheme. In the Bird et al (1990) survey, 6.2% of the population had moderate impairment but no DSM–III diagnosis. In a different survey, using DSM–III–R criteria, Angold et al (1999) found that 9.4% had no diagnosis but significant impairment. Across a variety of caseness measures, these individuals were as disturbed as those with a diagnosis. Many of the difficulties were around relationships with parents and siblings, and Angold et al argue that children who have symptoms associated with psychosocial impairment should be regarded as suffering from a psychiatric disorder.
Differences between classification systems
DSM–IV and ICD–10 are the only two widely used systems. The committees designing each worked closely together and strove to use names and criteria that are as similar as possible (Reference ShafferShaffer, 1996). However, there are some important general differences.
Pattern recognition v. symptom checklists
First, for children as for adults, ICD–10 has one set of ‘clinical descriptions and diagnostic guidelines' and a separate set of ‘diagnostic criteria for research’. The former comprises general descriptions of disorders that require a qualitative matching of case characteristics with the scheme – a pattern recognition approach. The latter comprises lists of symptoms with explicit criteria detailing the number and permutation required for diagnosis – a symptom checklist approach. DSM–IV has only the latter, the symptom checklist approach. It has advantages in increased reliability, but is relatively cumbersome so that many clinicians do not bother to apply the criteria rigorously. Even for the simpler DSM–III criteria, Prendergast et al (1988) found that although trained researchers achieved κ values of 0.83, 0.80 and 0.74 for attention-deficit disorder, conduct disorder and emotional disorder respectively, US clinicians in regular practice obtained values of only 0.30, 0.27 and 0.27.
A further disadvantage of the symptom checklist approach arises when the clinician believes that a diagnosis is present because of the severity of symptoms, but their number is insufficient to meet criteria. For example, consider the following youth: he repeatedly mugs old ladies, sets fires frequently, often argues, is often spiteful or vindictive, has unusually severe tantrums and has no friends or job because of his behaviour. According to ICD–10 Research Diagnostic Criteria (or DSM–IV criteria) he has no diagnosis, as he has two but not three symptoms of conduct disorder, and three but not four symptoms of oppositional–defiant disorder. However, according to ICD–10 Clinical Descriptions and Diagnostic Guidelines, he easily meets the requirements for conduct disorder since ‘any category, if marked, is sufficient’.
Comorbidity
A second difference between ICD–10 and DSM–IV is the way in which multiple diagnoses are handled. ICD–10 encourages the selection of one diagnosis that closest fits the picture, assuming that differences are due to a variation on the typical theme. DSM–IV and the closely similar ICD–10 Research Diagnostic Criteria encourage selection of as many diagnoses as criteria are met. Problems arise with this approach when symptoms are common to two disorders, for example, irritability contributes to affective disorders and to conduct disorders, so double coding is more likely. Since comorbidity is very common in clinical practice, multiple coding is frequent using a symptom checklist approach so that it begins to approach a dimensional system and to lose the advantages of categorisation (Reference Caron and RutterCaron & Rutter, 1991).
The pros and cons of each approach vary according to whether extra information is conveyed by the second diagnosis. Where there is good evidence of the validity of common comorbid conditions, ICD–10 has combined categories. Thus, the external validating characteristics of ‘depressive conduct disorder’ are similar to those of pure ‘conduct disorder’, with no increase of affective disorders in individuals followed up to adulthood, nor in their relatives. Double coding would convey erroneous information about the depressive aspect. ‘Hyperkinetic conduct disorder’ is characterised by more severe neuropsychological deficits than occur in either condition alone and by worse psychosocial outcome in adulthood. Double coding would not convey the poor prognosis (Reference RutterRutter, 1997).
Multi-axial framework
A third difference is that ICD–10 has a multi-axial framework for psychiatric disorders in childhood and adolescence (World Health Organization, 1996), as described below. DSM–IV uses a somewhat different multi-axial framework for all ages (this is outlined only briefly here).
Axis I: Clinical psychiatric syndromes
Here, criteria for particular diagnoses are applied, as described in the relevant manuals for DSM–IV and ICD–10.
Axis II: Specific disorders of development
These include speech and language, reading, spelling and motor development. In DSM–IV they are included in Axis I. Standardised tests are almost essential in order to characterise specific disorders of development. The lack of such tests for motor development is reflected in the lower reliability of the category (Reference Rispens and van YperenRispens & van Yperen, 1997).
Axis III: Intellectual level
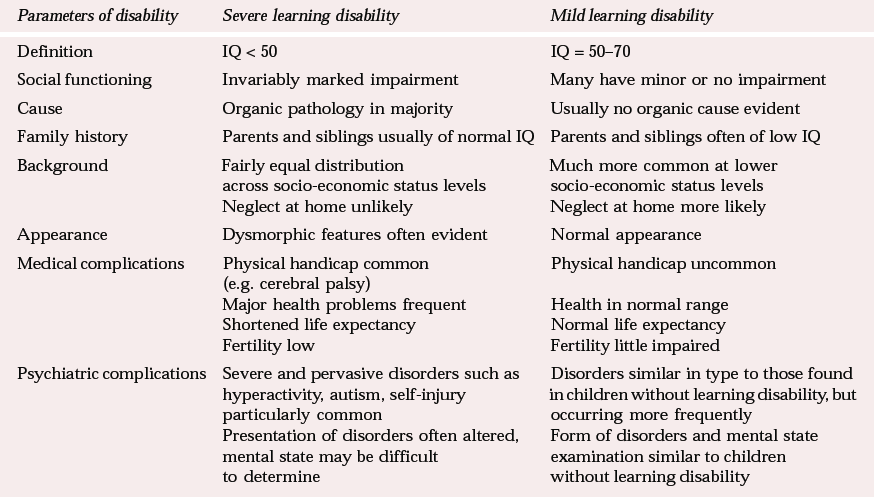
Subtyping generalised learning disability gives a good example of the substantial differences that arise when categories are imposed on top of a dimensional construct. If all children with an IQ below 50 (‘severe’ learning disability) are taken together and compared with those with an IQ between 50 and 70 (‘mild’ learning disability), major differences emerge on independent validating criteria, as shown in Table 1.
Table 1 Characteristics of children with severe and mild generalised learning disability
| Parameters of disability | Severe learning disability | Mild learning disability |
|---|---|---|
| Definition | IQ < 50 | IQ = 50–70 |
| Social functioning | Invariably marked impairment | Many have minor or no impairment |
| Cause | Organic pathology in majority | Usually no organic cause evident |
| Family history | Parents and siblings usually of normal IQ | Parents and siblings often of low IQ |
| Background | Fairly equal distribution across socio-economic status levels | Much more common at lower socio-economic status levels |
| Neglect at home unlikely | Neglect at home more likely | |
| Appearance | Dysmorphic features often evident | Normal appearance |
| Medical complications | Physical handicap common (e.g. cerebral palsy) | Physical handicap uncommon |
| Major health problems frequent | Health in normal range | |
| Shortened life expectancy | Normal life expectancy | |
| Fertility low | Fertility little impaired | |
| Psychiatric complications | Severe and pervasive disorders such as hyperactivity, autism, self-injury particularly common | Disorders similar in type to those found in children without learning disability, but occurring more frequently |
| Presentation of disorders often altered, mental state may be difficult to determine | Form of disorders and mental state examination similar to children without learning disability |
No particular psychiatric pattern arises in children with generalised learning disability; rather, the incidence of all disorders is raised, so that in those with IQ < 50, half have a psychiatric disorder (Reference Scott, Rutter, Taylor and HersovScott, 1994). In this group, precise characterisation of mental state is difficult and validity less certain (Reference Einfeld and AmanEinfeld & Aman, 1995). In DSM–IV, personality disorders are also included on Axis III.
Axis IV: Associated medical conditions
All medical conditions should be coded. A few have specific associations with psychiatric disorders, for example, tuberous sclerosis predisposes to autism and Cornelia de Lange syndrome to self-injury; Down's syndrome, on the other hand, protects against autism. Even where there is no specific disorder, congenital syndromes are often characterised by a particular pattern of behaviour. The study of these behavioural phenotypes is emerging as a discipline in its own right (Reference Flint, Yule, Rutter, Taylor and HersovFlint & Yule, 1994).
Axis V: Associated abnormal psychosocial conditions
These include a range of psychosocial hazards, from abnormal intrafamilial relationships, such as physical or sexual abuse, to mental disorders in other family members, distorted intrafamilial communication patterns, abnormal upbringing (e.g. in an institution), acute life events and chronic interpersonal stress arising from difficulties at school. As the number of psychosocial adversities goes up, so the rate of psychiatric disorders increases (Reference Garmezy, Masten, Rutter, Taylor and HersovGarmezy & Masten, 1994). Rutter (1987) found that no single psychosocial adversity was associated with particular disorders; rather, the total number was important. Those with only one adversity had no increase in disorders over those without adversity, whereas those with two had a fourfold increase in disorders. There were further exponential rises in disorder rates as the number of adversities increased. Conduct disorder is particularly associated with a poor immediate psychosocial environment (Reference Steinhausen and ErdinSteinhausen & Erdin, 1992), whereas emotional disorders are more associated with acute life events and school-related chronic stressors (Reference Moselhy, Vostanis and WinkleyMoselhy et al, 1997).
As on the other axes, abnormalities are coded irrespective of apparent cause. This is particularly relevant in light of continually developing understanding of causal mechanisms: 20 years ago the mechanism was thought to be directly environmental, but in the past 10 years good evidence has been collected to show that some environmental characteristics of the home are genetically mediated (Reference Braungart, Fulker and PlominBraungart et al, 1992). For example, the association between lack of books in the home and a child's poor reading skills is partly mediated through parents with lower IQ buying fewer books.
Axis VI: Global social functioning
Here a judgement is made on a nine-point dimensional scale, ranging from superior social functioning to profound and pervasive social disability. Unlike on other axes, ratings of disability are not independent, but have to be judged as arising from the psychiatric or developmental disorder identified on Axes I–III. Thus, impairment arising from adverse circumstances cannot be coded, but impairment due to intra-individual factors can. This rule therefore excludes recognition of psychosocial interventions that aid functioning, from reduction of parental expressed emotion to changing schools. DSM–IV studies often use the Children's Global Assessment Scale (CGAS; Reference Shaffer, Gould and BrasicShaffer et al, 1983), an adaptation of the Global Assessment of Functioning (GAF) used in adults. An advantage of the CGAS is that the impairment rated need not be caused by psychiatric disorder. A disadvantage is that psychiatric symptoms, rather than impairment alone, contribute to the rating. Reliability is reasonable (Reference Rey, Starling and WeverRey et al, 1995).
Conveying useful information: the need for validity
Categories need to be distinct not only in terms of the phenomena used to define them but, crucially, also in terms of external criteria. Even if categories can be reliably distinguished, when external criteria are the same, one is likely to be dealing with two variants of the same condition. An analogy would be the difference between black cats and white cats. Calling them different animals would not convey any extra information. Conversely, a tendency to lump too many categories together loses information. Calling a donkey a short horse would fail to convey that it lives longer, is prone to different diseases, cannot breed with a horse and can carry greater loads.
Reliability is a prerequisite for validity, and most categories have reasonable interrater and test–retest values when used by trained investigators. Where there are many overlapping categories, as in the present ICD–10 anxiety disorders, interrater reliability falls (Reference Thomsen, Jorgensen and NedergaardThomsen et al, 1992).
Typical validating criteria considered in child psychiatry
Distinctive current phenomenology
Although there may be partial overlap of accompanying symptoms, most defining criteria are almost always mutually exclusive between main categories. They describe current functioning and do not usually define causes or course. Exceptions are post-traumatic stress disorder, where the trauma must be defined, and autism and the hyperkinetic syndrome, where onset has to be before 3 years of age.
Epidemiology
Age at onset and gender ratio are frequently helpful. Forty years ago ‘childhood psychosis' was a unitary classification, but work showing the clear difference in age at onset helped to validate the distinction between autism and schizophrenia. Disruptive disorders occur four times more commonly in boys, whereas emotional disorders are more common in girls.
Long-term course
Most childhood disorders show reasonable homotypic continuity, that is they stay the same. Some show heterotypic continuity, so that, for example, some individuals with childhood hyperactivity end up as antisocial adults. This does not necessarily invalidate the category, but requires explanation.
Genetic and family findings
If individuals with distinct categorical diagnoses have relatives with different disorders, this helps to validate the distinction. This has confirmed the validity of several diagnostic categories, but not all. For example, it has not held for the many specific subtypes of anxiety disorder in ICD–10, whose validity is questionable. Genetic studies can also clarify the scope of symptom clusters. For example, family studies of autism have revealed a broader phenotype in relatives of probands (Reference Bolton, Macdonald and PicklesBolton et al, 1994). Therefore, new disorders may need to be considered that encompass only one of the original three constituent domains of classical autism (social relatedness, communication problems, and repetitive and stereotyped behaviours).
Psychosocial risk factors
The association between institutional upbringing with many changes of carer and reactive attachment disorder is so strong that it has been made a requirement for diagnosis in ICD–10. Harsh parenting is far more common in conduct disorders than in emotional and psychosomatic disorders.
Neuropsychological functioning
The hyperkinetic syndrome is clearly distinguishable from conduct disorder on tests of attention such as the continuous performance task. There has recently been considerable progress in showing that one of the core deficits in autism is failure on ‘theory of mind’ tests of ability to see another person's point of view, which children with comparable levels of learning disability but without autism can do.
Organic conditions
As noted above, these differentiate severe from mild generalised learning disabilities. However, there have been many failed attempts to show organic conditions in other diagnoses, including endocrine markers of aggression. However, the advent of functional neuroimaging is allowing pictures of children's brains to be built up relatively non-invasively, and reliable findings are beginning to emerge, for example in the hyperkinetic syndrome.
Response to treatment
This has proved a disappointing and unreliable distinguishing characteristic. For example, methylphenidate improves concentration in both normal children and those with hyperactivity; specific serotonin reuptake inhibitors (SSRIs) improve enuresis as well as depression; and parent-training improves both hyperkinetic syndrome and conduct disorder in the child.
Conclusions
Classification of child psychiatric conditions has advanced enormously in the past 20 years. There is a much stronger empirical basis to support current schemes, which are based on the many scientific disciplines that contribute to developmental psychopathology. Correctly applied, they are a powerful tool to use for the good of children and adolescents. The diagnostic castles have been built on firm sand, but need to be further reinforced against the waves of misunderstanding that sometimes threaten their usefulness.
Multiple choice questions
-
1. In ICD–10:
-
a the application of diagnostic criteria of most disorders requires an understanding of their cause
-
b the multi-axial classification system for childhood disorders has six axes
-
c keeping to one psychiatric diagnosis where at all possible is encouraged
-
d the multi-axial classification system for childhood disorders includes an axis for family history of psychiatric disorder
-
e subtypes of anxiety can be distinguished with a high degree of reliability.
-
-
2. The following are useful validating criteria for child psychiatric disorders:
-
a phenomenology of symptoms
-
b results of neuropsychological tests
-
c response to drug treatment
-
d gender ratio of prevalence
-
e age of onset.
-
-
3. Social impairment:
-
a is always a requirement if a psychiatric diagnosis is to be given
-
b can be assessed using the Children's Global Assessment Scale
-
c is of little consequence for the child, provided that no psychiatric disorder is present
-
d is present to a substantial degree in over one-third of children with no psychiatric diagnosis e leads to a reduction in prevalence rates of psychiatric disorders when applied to cases meeting DSM–IV criteria.
-
-
4. Childen with conduct disorder:
-
a have a good prognosis
-
b have a worse prognosis if onset is late
-
c have hyperactivity in about one-third of cases
-
d have specific reading retardation in about one-third of cases
-
e become less antisocial with parent training treatment.
-
-
5. Children with severe learning disability:
-
a live longer than those with a mild disability
-
b usually have parents with learning disability
-
c have often been neglected at home
-
d often have dysmorphic features
-
e have an IQ < 50.
-
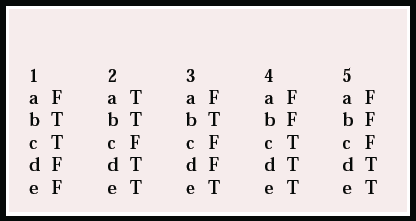
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | F | a | F | a | F |
| b | T | b | T | b | T | b | F | b | F |
| c | T | c | F | c | F | c | T | c | F |
| d | F | d | T | d | F | d | T | d | T |
| e | F | e | T | e | T | e | T | e | T |






eLetters
No eLetters have been published for this article.