There is widespread support for a positive and lasting relationship between participation in regular exercise and various indices of mental health, and several consensus documents and reviews (e.g. Reference Biddle, Fox, Boutcher, Biddle, Fox and BoutcherBiddle et al, 2000; Reference Craft and LandersCraft & Landers, 1998) have been published in this field. The evidence for psychological benefits, although impressive for mentally healthy individuals, is even stronger for psychiatric populations (Reference Martinsen, Stephens and DishmanMartinsen & Stephens, 1994). For example, a number of studies have demonstrated a positive relationship between exercise and mental health in people with alcohol misuse problems (Reference Donaghy, Ralston and MutrieDonaghy et al, 1991), people with schizophrenia (Reference ChamoveChamove, 1986; Reference Faulkner and SparkesFaulkner & Sparkes, 1999) and those with clinical depression (Reference MutrieMutrie, 1988; Reference MartinsenMartinsen, 1993; Reference Martinsen1994; Reference Martinsen, Hoffart and SolbergMartinsen et al, 1989a ,Reference Martinsen, Hoffart and Solberg b ).
Despite the growing body of evidence supporting the relationship between exercise and mental health, organisations have been reluctant to endorse the use of exercise in treating mental illness. Furthermore, exercise has not been widely adopted by clinical psychologists and psychiatrists as a viable adjunctive intervention strategy for improving the mental health of patients. For instance, a recent overview of depression and its treatment in the UK made no mention the value of exercise (Reference HaleHale, 1997). Similarly, Faulkner & Biddle (2001) reported that exercise as an intervention was not considered appropriately specific by clinical psychologists, and therefore, of incidental value. It appears much work has to be done to convince those who deliver mental health services to focus on the links between mind and body and to look more positively on the role of exercise as a treatment in mental health issues (Reference Mutrie, Biddle, Fox and BoutcherMutrie, 2000). This paper explores the potential value of exercise therapy as an adjunctive treatment in alleviating mental health disorders in clinical populations. The evidence supporting a positive relationship between exercise and mental illnesses is summarised and a rationale for the usefulness of exercise therapy along with more conventional treatments is provided. Some attention is also given to the role of exercise and lifestyle counselling in the exercise therapy process. The potential problems that might be associated with exercise therapy are explored and recommendations for good practice in the delivery of exercise therapy are suggested.
Exercise therapy in clinical populations
Pelham & Campagna (1991) investigated the physiological, psychological and social effects of exercise in out-patients with schizophrenia, using a single-subject design that emphasised interviews and questionnaires. A typical exercise programme consisted of cycling on a ergometer, 4 days per week for 30 minutes per session. Their results indicated a general trend of reduced depression, increased general well-being and improved aerobic fitness. More recently, Faulkner & Sparkes (1999) conducted an ethnographic study that examined the influence of exercise as a therapy for schizophrenia and reported that a 10-week exercise programme of twice-weekly sessions appeared to help reduce participants' perceptions of auditory hallucinations, raise self-esteem and improve sleep patterns and general behaviour.
Craft & Landers (1998) conducted a meta-analytical review of studies that had investigated the effects of exercise on clinical depression and depression resulting from mental illness. A Master's thesis and unpublished Doctoral dissertations and were also included in the analyses. To meet the inclusion criteria for this study, participants had to be suffering from depression as either the primary disorder or as a secondary disorder as the result of mental illness. Results from 30 studies showed an overall mean effect of –0.72, indicating that individuals who exercised were less depressed than their non-active counterparts. This study also concluded that those individuals who were initially more depressed benefited the most from exercise. Several other well-considered reviews (Reference MartinsenMartinsen, 1993; Reference Martinsen1994; Reference Mutrie, Biddle, Fox and BoutcherMutrie, 2000; Reference North, McCullagh and TranNorth et al, 1990) have indicated a positive relationship between exercise and clinical depression scores. An example of exercise therapy being used as an adjunctive treatment for depression is described below.
Martinsen et al (1989c) investigated hospitalised patients with various DSM–III (American Psychiatric Association, 1980) anxiety disorders; somatoform disorders; conversion, somatoform pain and somatization disorder; and hypochondriasis. Patients participated in an 8-week specialised aerobic exercise programme (main treatment) and three sessions of group psychotherapy. Anxiety was assessed using the Symptoms Rating Test (Reference Kellner and SheffieldKellner & Sheffield, 1973). No control group was included. During the study, anxiety scores fell significantly in most diagnostic groups. However, 1 year after treatment, those patients who experienced panic disorder with agoraphobia had lost their gains, while those with generalised anxiety disorder and agoraphobia without panic attacks remained well. Patients with social phobia were unchanged at discharge as well as 1 year after treatment. According to Martinsen (1995) these mixed findings may be due to normal variations in the course of different disorders, but they could also highlight that various anxiety disorders respond differently to exercise. Orwin (1974) has also reported positive results with a combination of exercise and exposure to the anxiety-provoking stimuli, although sample size was small.
Several studies have reported a positive association between participation in exercise and enhanced mental health in people who misuse alcohol, with some studies reporting significant changes after relatively short exercise programmes. Gary & Guthrie (1972) found that self-esteem improved along with fitness in a 4-week jogging programme. Other studies using quasi-experimental designs (e.g. Reference Palmer, Vacc and EpsteinPalmer et al, 1988; Reference Preedy and PetersPreedy & Peters, 1990) reported significant reductions in trait anxiety and depression during exercise. They also found that people with alcohol misuse problems who undertook aerobic exercise were better able to cope with life-stresses after discharge from the alcohol treatment programme. Research has also reported that participation in exercise appears to help reduce levels of alcohol consumption in misusers, although published research in this area remains limited and somewhat contradictory. Using self-report, Sinyor et al (1982) indicated that exercise can be linked to sustained abstinence up to 3 months after discharge from an alcohol treatment programme. Using a multi-site random control study, Donaghy (1997) investigated the relationship between exercise participation and levels of drinking by using serum carbohydrate deficient transferrin (CDT) as a marker of chronic alcohol consumption. No evidence to support a positive relationship between participation in exercise and maintained abstinence or controlled drinking was reported, highlighting a need for further research to clarify this relationship.
Patient views on exercise therapy
An important issue that warrants attention is patients' thoughts and perceptions about the usefulness of treatments that they receive in comparison with exercise therapy (Box 1). Pelham & Campagna (1991) reported that psychiatric out-patients who participated in a 12-week exercise therapy programme expressed positive views of exercise. Moreover, antidepressant, mood-elevation, moderate anxiety-reduction, increased self-esteem and improved concentration were some of the effects described by participants. Anstiss (1988) examined the relationship between exercise and well-being in alcohol-dependent patients who exercised for 4 weeks. On discharge, 60% of clients reported that exercise was of great value, and 29% said it was of considerable value. Likewise, Martinsen & Medhus (1989) asked patients to evaluate the usefulness of physical fitness training as compared with other more traditional forms of therapy (i.e. contact with nurses, psychotherapy and medication). Patients in the training group ranked physical fitness training as the therapeutic element that had helped them most. Patients in the control group ranked individual psychotherapy as most important. This raises the issue of patient choice and, collectively, these studies indicate that patients perceive exercise as a useful strategy in their rehabilitation.
Box 1 Case study
This case study is based on a referral that was made to me. Lucy is a 38-year-old female who was diagnosed with clinical depression. Prior to this, Lucy had experienced a period of hospitalisation, having threatened to commit suicide. She also had a long-term history of emotional abuse and neglect and had been receiving weekly out-patient services from a clinical psychologist for 12 months prior to the start of the exercise therapy treatment. Lucy is married and has an 11-year-old son.
During psychological therapy sessions with the clinical psychologist, Lucy had continually referred to her weight as being a major contributory factor to her depressive feelings and she blamed her medications as the cause for her excess body weight gain in recent years. Given this, Lucy was keen to explore ways in which she might reduce her body fat and become more active, both physically and mentally. Lucy's participation in exercise in the past had been sporadic and while she had been physically active as a child, she had not been able to maintain regular physical exercise in recent years and had become very inactive over the past five. As Lucy's son has become older, she wants to become more actively involved in his life by improving her physical fitness and health so that she can ‘keep up with him’.
Prior to commencing the exercise therapy, it was considered important for Lucy and the exercise therapist to discuss the therapy in conjunction with the clinical psychologist. Consequently, sessions were organised in successive weeks so they could get to know each other. Each exercise therapy session lasted 60 minutes and local amenities and facilities (e.g. leisure centres and parks) were used to try and ‘normalise’ the exercise sessions. Lucy was encouraged to participate in a range of physical activities (e.g. swimming and brisk walking) and to exercise at moderate intensity for 30–40 minutes, twice per week for 10 weeks. An important feature of each session was exercise and lifestyle counselling, which was based on the underlying principles of Carl Rogers' theory of person-centred therapy (Reference RogersRogers, 1957). During the counselling component, the exercise therapist introduced a variety of cognitive–behavioural techniques (e.g. consciousness raising, finding social support and goal setting) with the aim of moving Lucy towards sustained, independent and regular exercise behaviour as well as improved general health (e.g. improved diet and hydration).
At baseline, Lucy recorded a Beck Depression Inventory (BDI; Beck, 1987) score of 39 and by week 5 this had reduced to 34. Lucy reported a BDI score of 33 post-intervention, indicating a 15.3% reduction in her BDI score from pre- to post-exercise therapy. Lucy's adherence rate was excellent as she only missed two (out of 20) exercise therapy sessions over the 10-week intervention period. This study highlights a successful case where a clinician and researcher/practitioner were able to work together to understand how an alternative intervention treatment might be beneficial in reducing clinical depression. Such findings indicate that exercise therapy might be a worthwhile adjunctive intervention strategy that clinicians might want to promote with their patients.
Exercise therapy and convention interventions
The high prevalence of mental health disorders is costly to the National Health Service (NHS) and the local authority personal and social sevices net expenditure for mental illness in 1994–1995 totalled £311 million in England (Department of Health, 1996). For 1996–1997, the NHS Executive estimated the cost of mental health problems as over £32 billion (NHS Management Executive, 1996). There is, therefore, a need for simple, innovative, cost-effective strategies to be offered to clinical populations as part of their rehabilitation process, which could also contribute to a reduction in health care costs. Given that many common treatments (e.g. medication and cognitive–behavioural therapy) can be expensive and often in short supply, there is much to commend other strategies (Reference Fox, Boutcher, Faulkner, Biddle, Fox and BoutcherFox et al, 2000).
In support of the use of exercise therapy with clinical populations, meta-analyses have concluded that exercise may be as effective as psychotherapy and more effective than other behavioural interventions (e.g. Reference Craft and LandersCraft & Landers, 1998; Reference North, McCullagh and TranNorth et al, 1990) for treating depression. Specifically, Craft & Landers (1998) found that, compared with more conventional interventions, exercise is as beneficial as group or individual psychotherapy and behavioural interventions. That exercise is as effective as more conventional therapies is encouraging, especially if consideration is given to the time and costs involved with treatments such as psychotherapy (Reference Craft and LandersCraft & Landers, 1998).
The high demands on health services in recent times have led to time limits being set for some therapeutic treatments/services. Exercise therapy could be a positive adjunctive alternative to this problem since participants can use it whenever they choose and it is less reliant upon external factors associated with more traditional treatments (e.g. availability of a therapist). Martinsen (1993) has argued that exercise can be self-sustaining in that it can be maintained by individuals once the basic skills have been learnt. This may well help to make patients feel more empowered about their health and in control of their well-being. Exercise can be used as a recreational activity as a means to reintroduce individuals into the wider community. This is often an important element of treatment plans for people who have less severe mental health problems. Exercise has the potential to reach a broad audience who might not be able to access other types of psychological interventions or prefer not to use drug-based treatments. Often there is uncertainty about the best treatment plan for an individual and the form of treatment to which the individual will most likely adhere. This diversity should be matched by offering patients a range of appropriate treatments.
In the UK, medication remains the most frequently used treatment for depression (Reference HaleHale, 1997), yet patients often report that they do not want drugs (Reference ScottScott, 1996). Many drugs also have unpleasant side-effects such as fatigue, cardiovascular complications and even addiction (Reference MartinsenMartinsen, 1990). Exercise therapy, unlike drugs, requires individuals to become involved in an active rather than a passive rehabilitation process. In other words, drug interventions do no require any physical effort, are externally regulated and participants are passive recipients in the process. In contrast to this, exercise is more internally based and requires participants to experience physical commitment and effort.
Models explaining the benefits of exercise
There are many hypothesised mechanisms by which exercise is thought to influence mental health. Several biological, psychosocial and psychological models and theories have been suggested that may help us to understand these proposed relationships. It is difficult to pinpoint any single mechanism that is likely to account adequately for the exercise and mental health relationship until further research specifically addresses each proposed explanation. Although there have been a number of suggested hypotheses for this relationship, research supporting physiological explanations has been weak, with many studies being poorly designed. Moreover, while evidence supporting psychologically based explanations are not conclusive they do seem intuitively appealing. Specifically, the mastery explanations have had consistent empirical support.
Hyperthermic model
A common explanation of affective change is a neuro-physiological model known as the hyperthermic model. This suggests that the primary stimulus for promoting affective change is the elevation in body temperature from exercise, and this alteration in physiological state is manifested in a number of responses that are orchestrated by the hypothalamus. The belief that elevating body temperature can be therapeutic is longstanding (e.g. saunas and steam room). Indeed, research has revealed that total body warming (e.g. warm showers) reduces muscle tension (Reference deVries, Beckman and HubnerdeVries et al, 1968). Specifically, in relation to exercise, Horne & Staff (1983) concluded from their counterbalanced design that high intensity exercise and passive heating produced similar increases in slow wave sleep (relaxation effect) and that exercise may be a vehicle for these effects. Support for the hyperthermic explanation has been mixed and, in fact, there are many studies that have failed to demonstrate a positive relationship between exercise, increases in temperature and improved psychological states. It is now thought that there are more comprehensive models that explain the relationship between physical activity and psychological well-being more accurately.
Endorphin hypothesis
The endorphin hypothesis proposes that the effects of acute exercise on psychological well-being, in particular ‘euphoria’, is caused by the release and subsequent binding of endogenous opiods, these being -endorphins to receptor sites in the brain (Reference Steinberg and SykesSteinberg & Sykes, 1985). The endorphin hypothesis originated from early research on rat brain tissue that revealed significant increases in opiate receptor occupancy after the rats had been forced to exercise (Reference Pert, Bowie, Usdin, Bunney and KlinePert & Bowie, 1979; Reference Wardlaw and FrantzWardlaw & Frantz, 1980). Christie & Chesher (1982) have also demonstrated that mice can become ‘swimming junkies' if they exercise regularly. Unfortunately, because of the inherent problems of examining -endorphin receptor site occupancy in humans, research has attempted to examine peripheral -endorphin levels (blood outside the blood–brain barrier) after exercise (see Reference SynderSynder, 1977). Furthermore, DeMeirlier et al (1986) reported a positive relationship between -endorphins and exercise, which they contended leads to more positive affective states.
Research by Farrell (1989) suggested that exercise does not alter the blood–brain barrier in a way that allows peripheral endorphins to act directly upon the barrier. In other words, endorphins have been measured in the circulation and not directly in the brain, and because the blood–brain barrier blocks the passages by which ‘opiate’ substances move from the blood to the brain it is difficult to test the endorphin hypothesis. Interestingly, despite very limited support, the endorphin hypothesis remains one of the most popular explanations of the psychological benefits of exercise.
Self-esteem and mastery explanations
There are a number of theoretical models that have attempted to consider the possible relationship between participation in physical activity and self-esteem. One such model is Sonstroem's (1978) psychological model for physical activity. This model assumes that involvement in physical activity increases physical ability, which positively influences one's self-estimation and consequently leads to higher levels of self-esteem. Specifically, as individuals with high self-esteem take pride in their bodies, they continue to exercise, thereby maintaining and/or increasing fitness. Additional physical activity leads to increased perceptions of physical ability and self-esteem, which results in even greater attraction to physical activity. The cycle continues in this way. The model has been reasonably successful in presenting correlational evidence associating physical activity and psychological health, although some researchers have indicated inconsistencies in the application of this model.
Related to the concept of mastery is the idea that exercise can provide proprioceptive feedback of improvements in the overall functional ability of individuals' bodies. This in turn might be effective in changing body perceptions. Related to this, the positive relationship between exercise and mental health could be explained in terms of the physical signs associated with exercise (e.g. muscle tone and weight loss) and these physical signs could be viewed as positive cues towards a sense of achievement in one's physical self. This is important for clinical patients who often have negative feelings about themselves and their bodies.
Distraction hypothesis
A popular explanation for the positive relationship between exercise and mental health is the distraction hypothesis. This was originally conceptualised by Bahrke & Morgan (1978) in a study that compared the effects on state anxiety of walking on a treadmill, meditating or resting in a comfortable chair. Their findings demonstrated that all three groups showed decreased levels of state anxiety after treatment. It was concluded that exercise can serve as a useful distraction or ‘time-out’ from stressful stimuli and feelings and that this can lead to improved psychological wellness. In this respect, patients may find exercise a useful strategy to help them focus on events other than their particular life circumstances.
Exercise and lifestyle counselling
Although psychological outcomes associated with participation in exercise are important, consideration also needs to be given to patients' wider needs. Exercise therapy is much more than simply a way of providing facilities for patients to take part in exercise; like other therapies, it is an active psychological process. When promoting exercise with patients it is also crucial to consider the long-term consequences of this type of therapy. Many clinical patients will previously have been mostly sedentary or they will not possess the psychological skills or knowledge to adhere to a regular exercise programme and therefore they will need more than exercise alone. Ideally, exercise should be offered in conjunction with exercise counselling that is aimed at equipping individuals with skills, knowledge and confidence so they feel able to participate in physical exercise on a regular basis throughout the rest of their lives. Therefore, it is important that exercise therapy incorporates practical strategies that give patients the physical and psychological tools to sustain their exercise behaviour and experience positive psychological gains from exercise once the therapy comes to an end. In accordance with the principles of the transtheoretical model (Reference Prochaska and DiClementeProchaska & DiClemente, 1983) exercise therapy sessions should use a variety of cognitive–behavioural techniques (such as cognitive reappraisal and consciousness raising, goal setting, self-monitoring and finding social support) for promoting positive exercise attitudes, experiences and behaviour.
Exercise and lifestyle counselling should be offered within a counselling framework and, ideally, exercise therapists will have some experience of counselling psychology. Perhaps one of the most well-known and used approaches in mainstream counselling psychology is Carl Rogers's theory of person-centred therapy (1957) and it would be important for exercise therapists to demonstrate the core conditions of unconditional positive regard, empathy and congruence in their relationships with patients.
Physical health and mental illness
A range of psychological interventions (e.g. psychotherapy and medication) is available to assist clinical patients to improve their mental health. Furthermore, while other types of therapies and interventions might be useful in changing mental states, they are less likely to address adequately the physical and functional problems that individuals with depression might experience. Moreover, exercise has the potential to influence patients' physical and psychological health simultaneously and this could have cost implications for the NHS. Faulkner & Biddle (2001) have commented that, regardless of any mental health benefits, exercise should be promoted, since the physical needs of psychiatric clients are often underserved.
A number of studies have highlighted that clinical populations tend to suffer from poor physical health. For example, Chamove (1986) has indicated that patients with schizophrenia score well below the normal population on physical fitness. People with schizophrenia are commonly overweight, have excess body fat and are unfit. The physical health of substance misusers could benefit from exercise therapy. Specifically, people who misuse alcohol have been reported to have poor physical fitness (Reference Palmer, Vacc and EpsteinPalmer et al, 1988), loss of bone mass (Reference Peris, Pares and GuanabensPeris, et al, 1992) and a reduction of type II muscle tissue (Reference Preedy and PetersPreedy & Peters, 1990). Given this wide range of physical ailments typically experienced by clinical patients, the physical benefits of exercise therapy alone present a sufficient reason for inclusion in any form of psychiatric rehabilitation (Reference Faulkner and SparkesFaulkner & Sparkes, 1999).
Implications and possible problems
Drop-out from exercise has been identified as a major health issue in healthy individuals and there is no reason to assume that this will not be the case with clinical populations. With this in mind, it is important that exercise therapy should be offered to appropriate patients by psychologists and psychiatrists in the first instance, and thereafter coordinated by accredited health professionals who have the experience and expertise to deliver and prescribe exercise in the appropriate way. The British Association of Sport and Exercise Sciences (BASES) provides a 3-year supervised experience accreditation scheme and it is suggested that any individual employed to deliver exercise therapy in clinical settings should have undergone this process. Furthermore, as is the case with other types of mental health professionals, good practice would dictate that exercise therapists should receive some form of ‘supervision’ from a mental health worker. Indeed, it would be unwise for exercise therapists to believe that they can operate without this support. Some guidelines concerning the delivery of exercise therapy are presented in Box 2.
Box 2 Exercise therapy guidelines
Exercise programmes need to be flexible, enabling individuals to progress at their own rate
The exercise professional needs to have good planning and management skills as well as a wide range of physical activity options
Exercise interventions should promote mastery and personal accomplishments
The exercise intervention should develop key skills that are transferable to the community setting and between activities
Many mental health professionals do not appear to view exercise as a worthwhile strategy. McEntee & Halgin (1996) reported that, even though many psychotherapists believe in the therapeutic value of exercise, only approximately 10% recommended exercise to their clients. Perhaps future developments in this field should focus on attempts to forge greater links and partnerships between exercise/health professionals and those who deliver mental health services so that a greater range of appropriate intervention therapies might be offered to patients. In the short-term, this could involve the establishment of closer links between clinicians and staff at local leisure centres to facilitate the process of engagement with exercise for their patients.
Exercise therapy might not be suitable or useful for all patients (e.g. those with pre-existing physical ailments) and it would be unrealistic and unwise at this stage to suggest otherwise. There may also be some element of ‘psychological resistance’ from some patients who may have had poor exercise experiences in the past or who are not convinced of its possible benefits. Exercise therapy might not be appropriate with patients who have, or who are experiencing, severe eating disorders because it could hinder their recovery.
There is still some uncertainty about optimal levels of exercise for therapeutic effects. At present, several organisations (e.g. American College of Sports Medicine, 2000) recommend that adults should exercise 3–5 times per week at moderate intensity, but these guidelines were developed with physiological adaptations in mind rather than the therapeutic benefits of exercise. Exact guidelines have yet to be developed for each specific mental disorder, although the available evidence indicates that moderate intensity exercise would be best. The ‘Physical Activity and Mental Health National Consensus Statements and Guidelines for Practice’ document (Reference Biddle, Fox, Boutcher, Biddle, Fox and BoutcherBiddle et al, 2000) has made a number of suggestions for good practice and these are summarised in Box 3.
Box 3 Exercise prescription guidelines
Exercise therapy programmes should be no less than 4 weeks in duration
Patients should strive to participate in moderate intensity exercise for 20–30 minutes per session, 2–3 times per week
Patients should be encouraged to use a wide range of exercise and recreational activities
When possible, patients should be introduced to local amenities and facilities (e.g. local swimming pools, parks and leisure centres)
Ideally each session should last approximately 45–60 minutes and include exercise per se and exercise counselling
Conclusions
Given the prevalence and considerable financial costs associated with poor mental health, exercise as a therapeutic possibility deserves attention. Few clinical psychologists and psychiatrists currently consider exercise therapy as a worthwhile intervention strategy that could be useful in reducing mental illness. Whether exercise can be offered to patients as a stand-alone therapy remains to be seen, but the existing evidence suggests that this might be worthwhile adjunctive treatment. Of course, the physiological implications of exercise should not be ignored or underestimated either.
Perhaps an important step forward would be the inclusion of information about the exercise and mental health relationship in the training of clinical psychologists and psychiatrists who are key stakeholders in the therapeutic process, and who are often involved in the implementation of treatment plans. In the future, health authorities might wish to pursue the possibility of employing exercise therapists to work alongside clinical psychologists and psychiatrists. Some mental health communities around the UK have exercise scientists within their multi-disciplinary team, although these are limited in numbers.
It is not the aim of this paper to suggest that conventional treatments should be abandoned. Rather, it is hoped that this review will encourage psychologists and psychiatrists to be more open to less conventional alternatives so that patients are offered a range of interventions that might include exercise therapy. It is hoped that exercise therapy will become a mechanism by which the body and mind are viewed as dependent, rather than as separate entities, and that over time mental health professionals will begin to accept more readily the benefits of exercise as a therapy.
Multiple choice questions
-
1. Studies have demonstrated a positive relationship between exercise and mental health in the following patient groups:
-
a alcohol misusers
-
b those with schizophrenia
-
c those with clinical depression
-
d those with clinical anxiety
-
e those with psychoses.
-
-
2. Evidence supporting a positive relationship between exercise and levels of drinking in problem drinkers has been:
-
a positive
-
b contradictory
-
c negative
-
d equivocal
-
e very convincing.
-
-
3. Martinsen & Medhus (1989) indicated that patients in their study who experienced physical fitness training reported it to be:
-
a less useful than individual psychotherapy
-
b less useful than contact with nurses
-
c more useful than the traditional forms of therapy
-
d more useful than drug treatments
-
e less useful than group therapy.
-
-
4. The hyperthermic model suggests that the primary mechanism for the exercise and mental health relationship is:
-
a heat
-
b mastery
-
c endorphins
-
d biofeedback
-
e distraction.
-
-
5. The optimal level of exercise intensity for therapeutic benefits is:
-
a low
-
b moderate
-
c very low
-
d high
-
e very high.
-
MCQ answers
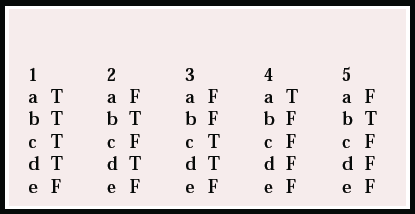
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | F | a | F | a | T | a | F |
| b | T | b | T | b | F | b | F | b | T |
| c | T | c | F | c | T | c | F | c | F |
| d | T | d | T | d | T | d | F | d | F |
| e | F | e | F | e | F | e | F | e | F |





eLetters
No eLetters have been published for this article.