Enormous cultural complexity is found in modern-day families. Spouses may belong to different racial, religious or ethnic groups, and two or more cultures may be represented among the parents and children (Reference FalicovFalicov, 1995). Relying on potentially stereotyped and ethnically focused information can be very misleading. Individuals vary considerably in the extent to which they choose to observe religious or cultural customs and conventions; the degree of acculturation may also vary between generations and between men and women. However, there is no doubt that the stigma of learning disability (‘mental retardation’) can be shattering and it transcends race, beliefs and culture. It creates profound emotional, practical and psychological experiences for all parents (Reference ShahShah, 1992).
The ‘minority experience’
Ethnicity is a complex concept which includes religious and cultural background, shared histories and common descent. Ultimately, it is the individual's psychological sense of belonging. Although not unique to families from ethnic minorities, there are distinguishing life events that differentiate the ‘minority experience’ from that of White middle-class families (Reference Sue and SueSue & Sue, 1999; Box 1).
Box 1 The minority experience (adapted from Reference Sue and SueSue & Sue, 1999)
Ethnic minority reality – often racism and poverty dominate lives.
Conflicting value systems – almost all ethnic minority groups place greater value on families, historical lineage and the submergence of self for the good of the family.
Biculturalism – many families inherit two cultural traditions. It is important to understand how biculturalism influences family structure, communication and dynamics. There is a need to understand the acculturation process.
Minority status – memories of colonialism, imperialism, slavery and the Holocaust, refugee and immigration status, skin colour and obvious physical differences are important factors that may determine the treatment of individuals and their families.
Migration – whether forced or voluntary
Language – many minority families may not possess vocabulary equivalent to standard English and may appear ‘flat’, ‘non-verbal’, ‘uncommunicative’ or ‘lacking in insight’.
Social class – aspects of wealth, name, occupation and status.
The notion of ‘White supremacy’ has dominated the social and political landscape in much of the world since the 19th century and it has fuelled exploitation and racism. At the same time, its ‘scientific’ justification in terms of skin colour, skull size and level of intelligence began to emerge.
Reference FernandoFernando (1989) describes racism as much more than just prejudice with social consequences. Once racism is embedded within the structures of society, the prejudice of individuals is no longer the main problem: more damaging is the issue of ‘institutionally generated inequality’. Direct racial attack is less common than are perceived discrimination in interpersonal communication and inequity in the receipt of services and justice (Reference Chakraborty and McKenzieChakraborty & McKenzie, 2002). Studies of Asian families that include someone with a learning disability reveal a deprived, isolated group who suffer racial abuse, encounter language barriers and experience significant levels of stress but have little knowledge or understanding of learning disability (Reference Nadirshaw, O'Hara and SperlingerNadirshaw, 1997). Although there is little information on the needs of other minority ethnic groups, the literature suggests that, despite formal health policy statements, families from minority ethnic communities with a member who has learning disabilities are doubly disadvantaged as a result of racial discrimination and culturally inappropriate forms of care and service provision. Ethnic identity per se does not affect health; what does affect it is the daily experience of racism, perceived racism and a discriminatory society (Reference Karlsen and NazrooKarlsen & Nazroo, 2002).
Another significant minority experience is that of migration. Whether voluntary or forced, it is a traumatic life event. It is the uprooting of meaning, with disruption of life-long attachments and external stability (Reference FalicovFalicov, 1995). Family disruption continues through separations and reunions, and parents who raise their children in a culture that differs from their own often feel disempowered.
Anthropological perspectives
Learning disability is a complex label involving interactions between biogenetic and sociocultural factors. The diagnostic criteria are the significant and enduring impairment in social and intellectual functioning evident before adulthood. Deciding on the presence or absence of learning disability requires an arbitrary line to be drawn across a continuum of ability. One measure is the IQ test, yet this was once used to prove the innate inferiority of immigrant populations. Eminent psychologists such as Arthur Jensen and Hans Eysenck supported claims that differences in IQ ratings between ‘White people’ and ‘coloured, primitive people’ were due to race, although this view is now strongly opposed by many (Reference FernandoFernando, 1989).
The cultural bias of IQ testing is well recognised but it is still administered in a culture-blind fashion. Cultural bias in verbal tests is obvious, but there is no guarantee that non-verbal tests are free from bias (Reference FernandoFernando, 1989). How well children with mild learning disabilities do in school or in adult life and, indeed, how they come to be diagnosed in the first place, largely depends on social and cultural conditions. This type of learning disability has been called ‘sociocultural’ or ‘reversible’ to emphasise the importance of social and cultural factors. Reference Ramey, Stedman and Borders-PettersonRamey et al(1978) showed in the USA that it was possible to identify children who would need special education before or during their school years, solely on information given on their birth certificates. The children most at risk were male, Black and had been born illegitimately to mothers with little formal education.
Society's views
‘In our country, we would not be allowed to treat cattle like that. Perhaps you cannot treat cattle this way in your country either – cattle, after all, are useful, while the retarded are not’ (N.E. Bank-Mikkelson, on visiting a state hospital in the USA; quoted in Reference EdgertonEdgerton, 1984: p. 28).
The neglect and ill-treatment of people with learning disabilities probably exhibits one of the worst histories for any group in society (Reference Sperlinger, O'Hara and SperlingerSperlinger, 1997). Western reactions have often been brutal. Those with learning disabilities have been killed, kept to entertain guests (a Roman practice that subsequently became common in the courts of European royalty), exhibited as freaks for profit, threatened with eradication and put at risk for the good of others, as in early trials of the measles vaccine. More compassionate views, tempered with pity, horror and contempt, prevailed through the 19th century, with Western attempts to provide institutional treatment and training.
There is little in the literature on the views of non-Western societies of the past. It was assumed that life in such societies was so simple that people with mild learning disabilities would be unexceptional members of their community, whereas the more severely disabled would be killed early in life. However, cross-cultural evidence indicates that even those with very mild learning disabilities were recognised throughout the world. There was a great variation in the treatment they received (Reference EdgertonEdgerton, 1984): although some societies inflicted casual cruelties others, including many in Central Asia, India and the Middle East, offered such persons protected and favoured roles.
Cultural and religious attitudes
Cultural and religious attitudes, understanding and beliefs all play their part in how care is ultimately sought, planned, accepted and delivered. Early research interest focused on the attitude of White middle-class parents within a Judaeo–Christian faith. The birth of a child with learning disabilities either stimulated a greater faith or resulted in a complete loss of faith. Some believed that they were being punished for their sins. Reference Fatimilehin and NadirshawFatimilehin & Nadirshaw (1994) found the variations in attitude between Asian and White British families to be related to cultural and religious differences rather than to any descriptive characteristics of the parent or their child (Box 2). Some would argue that South Asian cultures are more accommodating of people with disabilities (Reference McGrother, Bhaumik and ThorpeMcGrother et al, 2002)
Box 2 Differences in attitudes and beliefs of Asian and White British families
Reference Fatimilehin and NadirshawFatimilehin & Nadirshaw (1994) reported the following differences in a cross-cultural study of Asian and White British families
Asian British families
Had more contact with a ‘holy’ person (P<0.05)
Were less aware of what their child's problem is called (P<0.01)
Believed in a spiritual explanation/cause for their child's learning disability (P<0.05)
Fifty per cent said that they did not know the cause of their child's learning disability
Believed that religion had something particular to say about learning disability (P<0.005)
Their faith helped them to cope but offered little social or practical support
Wanted care to be provided by a relative when they were no longer able to provide it themselves (P<0.01)
White British families
Most received a medical explanation for their child's disability
None offered a spiritual explanation for their child's disability
Only one felt that it did not know the cause of the child's learning disability
Religion/faith offered social support
Most wanted their child to be cared for in a community home provided by statutory/voluntary services (P<0.05)
Many non-Western medical systems do not differentiate between physical and mental states, and the spiritual and supernatural elements are intertwined. The Hindu belief in the concept of karma – the cycle of reward and punishment for all deeds and thoughts as the immortal spirit is reborn into another body – may provide an understanding for what has happened and lead to a sense of resignation or acceptance. Middle Eastern cultures regard disability as a punishment from heaven, emanating from the spirits or caused by an evil eye (Reference Aminidav and WellerAminidav & Weller, 1995). Many Chinese people believe in fate and use a coping strategy of forbearance, seeking supernatural power and praying to ancestors (Reference Cheng and TangCheng & Tang, 1995). Clinicians have often cited fatalism and the search for a cure as reasons why families from some ethnic minority communities are not interested in educational or habilitative programmes for learning disability. It is frequently assumed that Asian parents do not have a positive or encouraging attitude towards disability, precisely because of their religious or superstitious beliefs (Reference ShahShah, 1992).
An important misconception about learning disability held by Asian parents is the notion of curability and that the marriage of the person with a learning disability may alleviate the condition. Reference Channabasavanna, Bhatti and PrabhuChannabasavanna et al(1985) found that neither the severity of disability nor the socio-economic status of the parents had any effect on this attitude. Rather, it was knowledge of the concept of learning disability, gained through counselling, that was most influential. An example of good practice in this area is provided by Reference Davis and RushtonDavis & Rushton (1991).
Gender and social roles
‘A woman's Heaven is at her husband's feet’ (traditional Asian saying).
Social and gender roles and, in particular, traditional female roles, are interpreted differently, in different communities, across generations and within individual families. In 19th-century English literature, men with learning disabilities were portrayed as lacking an essential component of masculine identity, usually because of their inability to handle money (Reference McDonaghMcDonagh, 2000). Women with learning disabilities embodied a paradox, being seen as threatening because of their ‘undisciplined sexuality’, yet also sexually innocent and in need of protection. This view resulted in mandatory sterilisation and prohibition from marriage. Both practices were still in force in 24 states in the USA as recently as 1971.
Bengali parents’ desire to see their children with learning disabilities married is at the heart of their parental responsibility, and services struggle with the ethical issues this situation may pose (Reference O'Hara and MartinO'Hara & Martin, 2003). However, securing a marriage partner also serves to reassure and provide comfort to parents that their child will be cared for after their own deaths.
Marriage between close biological relatives is generally regarded with suspicion and distaste within Western society (Reference BittlesBittles, 2001). By comparison, other populations perceive marriage outside the family as a risky and disruptive option. In some communities, consanguineous (first-cousin) marriages continue to account for 33%–53% of the total (Reference Jaber, Halpem and ShohatJaber et al, 2000). Professionals often relate disability explicitly to consanguineous marriage and they may be unsympathetic because they consider the condition to be self-inflicted. An Asian mother of a child with a learning disability said:
‘the first thing he [the general practitioner] asks is, “Is it a first-cousin marriage? You've had one disabled child, then another.” He's a good doctor, but, because of his attitude, I only go when I really have to’ (Reference Katbamna, Bhakta and AhmadKatbamna et al, 2002).
Asian women are seen as isolated because of their traditional customs; the failure by Asians to take up services provided by statutory bodies is attributed to their lack of skills relating to Western lifestyles (Reference FernandoFernando, 1989). Women with learning disabilities face ‘triple jeopardy’ in relation to race, disability/impairment and gender (Reference Mir, Nocon and AhmadMir et al, 2001). They may experience simultaneous discrimination and disadvantage and have additional support needs in terms of their sexuality and motherhood. However, there is a growing interest in the health and welfare of women with learning disabilities, as evidenced in Reference Walsh and HellerWalsh & Heller (2002).
Learning disability in ethnic minority communities
The prevalence of learning disabilities among South Asians is three times that in majority communities. Of these families, 19% have more than one member with a learning disability (Reference Mir, Nocon and AhmadMir et al, 2001). Unfortunately, prevalence within other minority ethnic communities, and even for different subgroups within the South Asian community, is not well documented. This higher prevalence has been linked to high levels of maternal and social deprivation combined with factors such as inequality in health care (Reference EmersonEmerson, 1997). The health care that is offered may be culturally inappropriate, unwelcoming and discriminatory, with a culture-blaming attitude. It may also have poor standards of communication and offer poor quality of care (Reference Mir, Nocon and AhmadMir et al, 2001). For example, prenatal diagnosis is sometimes withheld from Muslim families on the assumption that they will not consider a termination of pregnancy. This denies them information and choice.
There are reports of ethnic differences in the rate of detection of trisomy-21 using biochemical markers (e.g. Reference Gilbert, Nicholl and AlexGilbert et al, 1996), with more false-positives in ethnic minorities, which lead to unnecessary anxiety and invasive investigations.
The method used to break news of impairment/disability to a family from a minority ethnic community may be particularly poor, with the use of a non-professional interpreter adding to the stress and initiating or perpetuating a cycle of bad health experiences and expectations (e.g. Reference Butt and MirzaButt & Mirza, 1996). An information vacuum exists, in terms of culturally appropriate leaflets or audio-visual material, and the type of information that historically has been made available, for example about hygiene and fertility control, may be translated in a way that implies inferior cultural practices (Reference Mir, Nocon and AhmadMir et al, 2001).
Carers in ethnic minority communities
In the UK, the burden of care, both socially and financially, is greater for carers from minority ethnic communities compared with their White peers (Reference Butt and MirzaButt & Mirza, 1996). This is due to a number of contributory factors including poverty, poor housing, racism, higher levels of unemployment, low pay, minimum pension rights, reduced benefits because of residence status and inadequate education. For example, spouses of adults with learning disabilities from ethnic minority communities are allowed into the UK on the proviso that they do not claim on the welfare state for the first 5 years. There is evidence that general practitioner (GP) consultation rates in minority ethnic communities are significantly higher than in the majority community, but that these patients are less aware of the existence of specialist services (e.g. Reference Katbamna, Bhakta and AhmadKatbamna et al, 2002; Reference McGrother, Bhaumik and ThorpeMcGrother et al, 2002). Psychological and emotional distress may not be recognised, as patients from ethnic minorities tend to present to their GP with somatic symptoms (Reference Nadirshaw, O'Hara and SperlingerNadirshaw, 1997). A discriminatory view is that this is an unsophisticated form of communication (Reference FernandoFernando, 1989). There is also a danger of emphasising people's needs in terms of religion, customs and traditions and overlooking their basic needs for decent housing, access to health care and assistance to claim benefits. Factors such as immigration and the quality of housing available, particularly in inner-city areas, often militate against the supportive network traditionally offered by extended families.
A family's failure to spend time with a member with disabilities might be due to insufficient financial and practical support, but it can be perceived by professionals as a lack of interest or engagement with services.
It is a commonly held view that the hierarchical family structure in many non-Western cultures produces ‘stress-ridden relationships’, and the very strengths of this organisation are seen as a source of actual and potential weakness (Reference FernandoFernando, 1989). Research often pays little attention to the strengths of such a support network. Understanding of and respect for different family organisations are vital to service delivery. Parents may not have sole primary responsibility for looking after their children, as care is shared by a number of adults within the extended family. Extended families may involve grandparents, uncles and aunts, cousins and second cousins and even non-blood ‘relatives’. It is important to understand how decisions are made and who has the ultimate authority for making them. In some cultures, out-patient appointments may be seen as a social responsibility, with a large group of family members attending. Likewise, a consultation in the home can often involve the presence of a number of family members. The level of individuals’ contacts outside their own ethnic group varies, and this can have profound effects on the perceptions and lifestyles of different generations. Second and third generations may have very different attitudes from their predecessors and this can lead to tension and cultural conflicts within a family. When providing services to families that have a range of different structures and priorities, skills are needed to avoid giving primacy to a particular cultural or ethnic approach (Reference Mir, Nocon and AhmadMir et al, 2001).
Ethnic and racial identity
Racism and stigma are pervasive in the lives of people with learning disabilities who are from the South Asian community. Reference Azmi, Hatton and EmersonAzmi et al(1997) found this double discrimination to be a painful reality. However, in their study of such a population, all participants had a strong sense of their ethnic and racial identities and viewed these identities positively. There was a wide variation in the extent to which the ‘younger’ generation, mostly born in the UK, maintained traditional practices such as arranged marriages, gender roles, family obligations and religious observances. Almost all participants named a religious affiliation matching that of their families, and over 50% reported active observance of their religion. Sixty-three per cent felt that they were treated badly because of their ethnic group (27% did not respond clearly on this issue) and 57% also felt that they were treated badly because of their disability (33% did not respond clearly). Frequently, participants reported abusive behaviour from other people which combined racism and stigma.
An essential part of personal identity is personal appearance, and for some communities it is particularly important to pay attention to cultural factors associated with dress, hair and skin care and personal hygiene. Food is another aspect of basic care where cultural and religious needs might be ignored or inadequately catered for. Behavioural programmes and skills training might be based on White culture, for example teaching someone to use a knife, fork and spoon. Provision of physiotherapy activities such as massage, limb manipulation, dancing and swimming needs to be sensitive to the wishes of the family, especially with regard to modesty and appropriate behaviour. Unless such issues are addressed, people from ethnic minority communities are unlikely to use services that they perceive to be discriminatory.
Knowledge about religious beliefs and cultural practices can enable services to ensure that people with learning disabilities from ethnic minority communities experience a range of relevant cultural events and influences. Recurrent themes reported by carers include the need to meet dietary requirements; provide culturally appropriate activities and same-gender centres; increase the number of staff from minority cultures and the number of bilingual workers throughout mainstream services; and adapt materials in a culturally sensitive way. However, the assumption that a family wants support only from someone of their own culture is often misplaced, as workers from other cultures may be perceived as less intrusive (Reference Mir, Nocon and AhmadMir et al, 2001). The preference for same-gender staff to carry out intimate personal care and support is curiously portrayed as a requirement specific only to certain religions and cultures, when, in fact, it exists to a large extent in all communities. This belief is unhelpful as it suggests that the preference is ‘different’ or ‘special’ and it gives the impression of an additional burden on resources (Reference BaxterBaxter, 1996).
Importance of language
‘Ethnicity patterns our way of thinking, feeling and behaving. Language is one factor in the elaboration of ethnicity’ (Reference de Zuluetade Zulueta, 1990).
Communicating with people in a language other than their first language can affect our sensitivity to their attitudes and values (Reference ShahShah, 1992). Language structures the meaning of communication and contributes to a sense of belonging (Reference Sue and SueSue & Sue, 1999). We think and feel in our first language, and using a second language can block thoughts and emotions (Reference BhugraBhugra, 2002). Bilingual patients can appear less psychotic when interviewed in their second language rather than their first language, as well as remaining protected from anxiety and hidden meanings and feelings (Reference de Zuluetade Zulueta, 1990). In some cases, health practitioners are themselves using a second language in clinical practice and not enough attention has been paid to the resulting implications, especially in the context of psychotherapeutic approaches. The choice of language used in the delivery of health services to bilingual families may not appear neutral to them. It can be perceived as collusion between the clinician and the most fluent family member; it may allow the child to speak freely from the parent; and it may be used to track transgenerational alliances. Complexity increases with family size and the degree of bilingualism in each family member (Reference RavalRaval, 1996).
Interpreters: help or hindrance?
It is unethical and unprofessional to use children to interpret. Interpreting by family members should be avoided because of the possible biases and power relationships within the family (Reference ShahShah, 1992; Reference Farooq and FearFarooq & Fear, 2003). A very high level of interpreting skills is required, with the interpreter at the apex of a triad:
‘the interpreter is the person who makes the link between two different languages and cultures… [who] makes sense of unusual questioning, helps contain feelings’ (Reference RavalRaval, 1996).
However, interpreters do not have a professional status and their role within services may be ambiguous. They can be seen solely as interpreters of language or as community workers, link workers, advocates, cultural brokers or cultural consultants. Working effectively with interpreters requires training and is a necessary component of providing a high-quality service (Box 3). It is not a luxury. For clinicians who use interpereters, there is the risk of feeling disempowered and culturally ignorant in front of patients and their families, leading to a sense of therapeutic detachment and a mechanical or stilted interview. They may begin to feel de-skilled, excluded or resentful and hold a lower opinion of the efficacy of their involvement. They may become dependent on the interpreter in order to carry out their role. Patients or carers, however, can feel more reassured about their ability to communicate freely through a trained interpreter when describing religious beliefs (such as ghost possessions), unsatisfactory environmental conditions, mental illness and even abuse, without fear of being ridiculed (Reference RavalRaval, 1996). The interpreter, however, may feel it culturally inappropriate to translate particular language (e.g. verbal abuse or that related to sexual behaviour). Discussion of sexuality is surrounded by taboos, more so in some communities than others. Sometimes questions cannot be translated directly and have to be rephrased to make sense in another language. This can result in a translation that is semantically very different from the question originally asked. It is important, therefore, that a method of joint working with the interpreter is agreed prior to the interview.
Box 3 Working with interpreters (adapted from Reference ShahShah, 1992; Reference Nadirshaw, O'Hara and SperlingerNadirshaw, 1997)
Skills of a good interpreter
Fluent communication
Ability to engage with the patient while speaking as directed by someone else
Sensitivity and interpersonal skills
Calm and non-threatening personality
Capacity to offer comfort in discussing personal and emotional issues
Negotiating the interpreter–clinician relationship
Insist on mutual briefing and debriefing
Ensure interpreter is well versed in the information needed and in any specific concepts that may be used
Agree a model of joint working, e.g. literal translation or translation reflecting cultural context
Ensure interpreter understands the importance of confidentiality
Check for compatibility, e.g. in linguistic and religious backgrounds
Respect the professionalism of the interpreter – do not be suspicious of the relationship between patient/carer and interpreter
Be patient and open-minded. Ask questions without being intentionally offensive
Observe gender issues, religious and cultural events
Be sensitive to the discrimination that patients/families experience in their everyday lives
Developing cultural competence
Services must develop a sense of belonging in people from a variety of cultures, so that they feel comfortable about them. Reference FalicovFalicov (1995) urges applying a cultural lens to everything we do and taking culture into mainstream thinking, teaching and learning. Cultural knowledge is important, but care must be taken not to apply it in a stereotyped manner (Box 4).
Box 4 The continuum of cultural competence
Reference Cross, Bazron and DennisCross et al(1989) identified the following culturally appropriate or inappropriate behaviour in a health care organisation:
Cultural destructiveness – cultural/racial oppression, forced assimilation
Cultural incapacity – discriminatory practices, unchallenged stereotypical beliefs
Cultural blindness – ‘We treat everyone the same’: this approach ignores cultural strengths. The belief that methods used by the dominant culture are universally applicable can lead to implicit or explicit exclusion of ethnic minority communities
Cultural pre-competence – a false sense of accomplishment; inconsistent policies and practices; practitioners are sensitive to minority issues but these are not an organisational priority
Cultural competence – a vision that reflects multi-culturalism, values diversity and views it as an asset: evidence of continuing attempts to accommodate cultural change; careful attention to the dynamics of difference, realising that equal access is not equal treatment
Cultural proficiency – adding to knowledge-base by conducting research; developing new therapeutic approaches based on cultural considerations; follow-through social responsibility to fight social discrimination and advocate for social diversity
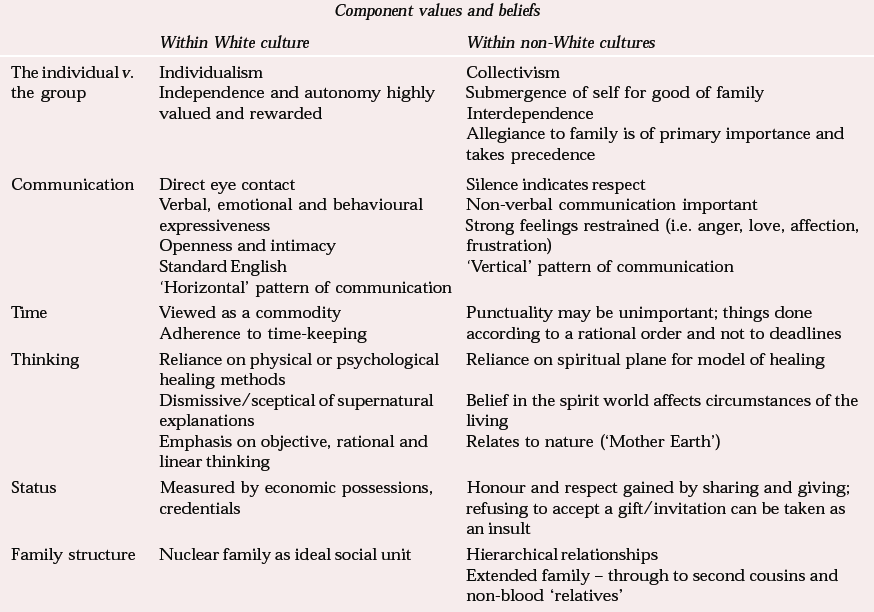
Ethnic matching of the clinician/doctor and patient is neither necessary nor always desirable, but it is essential that clinicians are aware of the interactions between the parties (Reference BhugraBhugra, 2002). These are often influenced by training, experience, social class, world views and knowledge of one another's culture and ethnicity (Table 1). For example, there may be an assumption that the absence of toys scattered around the living room floor during a home visit indicates that parents do not think that toys are important or, more worrying, it may be taken as a sign of neglect or environmental deprivation. The sharing of a parental bed is another culture-bound practice, which may lead to judgemental reactions from practitioners concerned with issues of child protection or adult vulnerability. Criticism, especially in front of others, may be a culture-bound expression of parental concern and the encouragement to better oneself. There is a risk, however, that it may be misconstrued as dysfunctional family dynamics. The diagnosis therefore of ‘family conflict’ may be no more than a racist assumption about family life (Reference FernandoFernando, 1989).
Table 1 Value and belief models of worldviews (adapted from Reference Sue and SueSue & Sue, 1999)
| Component values and beliefs | ||
|---|---|---|
| Within White culture | Within non-White cultures | |
| The individual v. the group | Individualism Independence and autonomy highly valued and rewarded |
Collectivism Submergence of self for good of family Interdependence Allegiance to family is of primary importance and takes precedence |
| Communication | Direct eye contact Verbal, emotional and behavioural expressiveness Openness and intimacy Standard English ‘Horizontal’ pattern of communication |
Silence indicates respect Non-verbal communication important Strong feelings restrained (i.e. anger, love, affection, frustration) ‘Vertical’ pattern of communication |
| Time | Viewed as a commodity Adherence to time-keeping |
Punctuality may be unimportant; things done according to a rational order and not to deadlines |
| Thinking | Reliance on physical or psychological healing methods Dismissive/sceptical of supernatural explanations Emphasis on objective, rational and linear thinking |
Reliance on spiritual plane for model of healing Belief in the spirit world affects circumstances of the living Relates to nature (‘Mother Earth’) |
| Status | Measured by economic possessions, credentials | Honour and respect gained by sharing and giving; refusing to accept a gift/invitation can be taken as an insult |
| Family structure | Nuclear family as ideal social unit | Hierarchical relationships Extended family – through to second cousins and non-blood ‘relatives’ |
A strategic approach is required to ensure that the needs of people from ethnic minority communities are not forgotten. These needs are complicated by issues of power, race and gender politics but they must not be overlooked just because they affect only ‘small numbers’ within a given population (Reference ColeCole, 2002; Box 5).
Box 5 Service principles and action plan for service development (adapted from Reference Mir, Nocon and AhmadMir et al, 2001 and Reference ColeCole, 2002)
The requirements of service development include:
A strategic approach
Meaningful consultation with families, carers and community workers
Going beyond consultation to real empowerment
Developing advocacy and self-advocacy, recognising family structures that differ from those of the majority ethnic community
Appropriate publicity for and full access to all service provision
Recruitment of ethnic minority and bilingual staff at all levels and ensuring their adequate support and training
Training for all staff, to increase competence in cultural awareness, sensitivity and flexibility
Person-centered planning, acknowledging discrimination and racism and its impact on the person; drawing up support plans to empower people from ethnic communities
Accurate information about need – effective monitoring processes, patterns of use, identifying unmet need
Targeting housing and placement opportunities within ethnic communities
Commissioning single-culture treatment options, including in-patient and residential facilities, self-help groups, social and psychological therapies
Working with provider agencies that specify ‘cultural competence’
Integrated services: the ideal is quality mainstream services sensitive to the needs of all users
‘Special-needs’ initiatives can provide a much needed focus on the issues to be addressed, but they are often structurally disadvantaged, with inadequate funding. They may appear to meet a need but in fact act as a surrogate form of racism while absolving mainstream services of responsibility. Specialist services do not eliminate the need to remove discriminatory practices and attitudes from mainstream services. This situation is reflected in the wider debates and philosophies underpinning the provision of health care in general, and mental health care in particular, for people with learning disabilities. Cultural sensitivity is only one element of quality in service provision. The notion of ‘cultural diversity’ is intended to move us away from a focus on ‘difference’ and the consequent perception of additional burden. Managing diversity means offering a level of respect to all. It also leads to recognition that the ‘majority’ is not a homogeneous population but comprises a number of cultural and social communities with their own needs and aspirations.
Multiple choice questions
-
1 Learning disability is:
-
a easily diagnosed when IQ testing is administered in a culturally blind way
-
b more prevalent in South Asian communities
-
c not recognised in developing countries
-
d easier to accept for parents from ethnic minority communities
-
e often the product of consanguineous marriages.
-
-
2 People with learning disabilities from ethnic minority communities:
-
a do not have a strong ethnic identity
-
b fail to observe their own cultural and religiou practices
-
c experience discrimination due to racism and disability
-
d often come from dysfunctional extended families
-
e seldom marry and have children.
-
-
3 Carers from ethnic minority communities:
-
a are more likely to be receiving specialist services
-
b are just as disadvantaged as their White peers
-
c often receive practical and social support from their religious faith
-
d prefer to have their child with learning disabilities looked after in a local residential community home
-
e often believe in a spiritual explanation for their child's condition.
-
-
4 Working with interpreters:
-
a is not necessary if someone in the family speaks English
-
b may lead the clinician to feel disempowered
-
c is a luxury that the NHS cannot afford
-
d requires training
-
e allows easier access to the patient's mental state.
-
-
5 Delivering culturally sensitive health care means:
-
a matching the patient to a clinician of the same ethnic/cultural background
-
b treating ethnic minority communities the same as everyone else
-
c developing specialist services
-
d using a ‘cultural lens’ in developing mainstream services
-
e realising that equal access is not the same as equal treatment.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | F | a | F |
| b | T | b | F | b | F | b | T | b | F |
| c | F | c | T | c | F | c | F | c | F |
| d | F | d | F | d | F | d | T | d | T |
| e | F | e | F | e | T | e | T | e | T |






eLetters
No eLetters have been published for this article.